Definitive diagnosis of oral lichen planus (OLP) is important for planning treatment. The problems and difficulties of diagnosing OLP based on histopathological features were showing inter- and intra-observer variability. In terms of pathological diagnosis on OLP, microvascular appearance was not highly valued. Comparative histomorphometric analysis of intraepithelial papillary capillary loops (IPCLs) of OLP was performed to investigate the potential for use as diagnostic criteria.
Immunohistochemical and histopathological evaluations of microvascular morphology were performed in 42 cases diagnosed as OLP clinico-histopathologically. Average areas and capillary loop angles at the sites adjacent to the lesion and most prominent and erosive areas of OLP were measured using image analysis software under microscopic observation.
Area of IPCLs in sites adjacent to the lesion was larger than those in prominent areas of OLP (p < 0.001). Capillary loop angles were 26.6 ± 19.3°, 84.5 ± 17.8°, 30.2 ± 2.4° and 34.4 ± 19.3° for normal mucosa, sites adjacent to the lesion, prominent areas of OLP, and erosive areas, respectively. Significant differences were observed between the prominent areas and adjacent sites to the lesion (p < 0.001).
Characteristic IPCL patterns were identified in the present study despite reticular/erosive type. This research thus suggested the utility of these patterns in pathological diagnostic criteria.
Lichen planus is a chronic inflammatory disease in the skin and mucous membranes of unknown etiology. Oral lichen planus (OLP) was first described by Wilson in 1869 [1], and appears more peculiar (that is, more persistent and resistant to treatment) than cutaneous lichen planus [2]. In addition, OLP was included as an oral potentially malignant disorders (OPMDS), defined as clinical presentation carrying a risk of cancer development in the oral cavity in the new World Health Organization classification of head and neck tumors [3], but the frequency of malignant transformation is controversial [4]. Therefore, definitive diagnosis in OLP is very important to decide treatment planning [5].
The diagnosis of OLP is based on both clinical and histopathological features. OLP clinically shows six classical clinical presentations, as described in the literature [6]: Reticular, erosive, atrophic, plaque-like, papular and bullous.
In contrast, results of biopsy should be described, particularly when white striae are ill defined, plaques are present, or regions appear in any other way unusual [7]. Even though clinical and histopathological unified criteria for OLP have been unified [8], the potential for disagreement between clinical and histopathological diagnosis has been discussed for various other disorders clinically resemble OLP [9].
Histopathological features of OLP changes by the various conditions, such as the stage of disease activity at the time of biopsy, any recent treatment of the condition, clinical type, and/or anatomic site [4]. In addition, OLP shares several histopathological features with other muco-cutaneous lesions, thus may often be misdiagnosed [4]. The problems and difficulties in diagnosing OLP based on histopathological features alone have been shown in studies showing inter- and intra-observer variability [10,11].
As an autoimmune disease with an inflammatory origin and chronic progression, OLP satisfies all the prerequisites for creating hypoxia, which is essential for angiogenesis [12]. Previous investigations have shown a close relationship between angiogenesis and the activity of OLP, and angiogenesis remains one of the main factors contributing to the progression of OLP [13,14]. Superficial blood vessels in the lamina propria mucosae are branching vessels that immediately extend horizontally; forming single loops referred to as intraepithelial papillary capillary loops (IPCLs) [15]. Clinically, Giuseppe noted that capillary loop diameter in OLP patients was significantly increased compared to normal mucosa on video-capillaroscopy and concluded that capillaroscopy can be a very important method for evaluating the microcirculation in patients suffering from OLP [16]. However, the microvascular appearance has not been regarded as highly relevant to the pathological diagnosis of OLP, and the histomorphological characteristics of IPCL have yet to be clarified. The present study therefore undertook a comparative histomorphometric analysis of IPCLs in OLP to investigate the potential for use as diagnostic criteria.
Histopathological, immunohistochemical and histomorphological evaluations of microvascular morphology were performed in 42 cases diagnosed with OLP. Forty-two patients with OLP (9 males, 33 females) were selected from the pathology files of the Department of Oral Pathology, Nihon University School of Dentistry at Matsudo. Mean age was 64.6 ± 9.1 years (male: 60.2 ± 12.0 years; female: 65.8 ± 8.0 years). The characteristics of subjects in this study are summarized in Table 1. The patients with clinical and histopathoalogically proven OLP cases according to diagnostic criteria [3,17], and the materials does not lack all macroscopic view record, digital pictures of oral cavity and biopsy specimen which comprised an area at the boundary part of the most prominent lesion and an adjacent area of normal mucosa, were included in the study. Patients with history of exposure to dental materials, drugs, etc. [18], any treatment for lichen planus or drugs associated with lichenoid reaction before biopsy, any malignant or viral involvement in mouth and pregnant women were excluded from the study sample.
Table 1: Clinico-pathological details of all cases. View Table 1
Dental examination was performed by the same oral surgeon for 42 patients, and a total of 96 sites were enrolled in the study, because patients with OLP at multiple sites were included. OLP was clinically diagnosed by the oral surgeon with well-defined looping and intersecting white lines/striae/patches with or without erosions and ulcerations [3,5,7,9]. Clinical inspection classifications for the most prominent site were made by 2 oral surgeons and 3 oral pathologists based on Andreasen's 6 types and Brant's 2 types [19] independently. Three oral pathologists were judged by digital pictures of patients. In cases of disagreement classifications were discussed in a joint session until consensuses was reached.
Biopsy specimens were obtained for all 42 patients by the same oral surgeon, sampling an area at the boundary part of the most prominent lesion and an adjacent area of normal mucosa. Histologic specimens included in the study were selected according to definite histopathological criteria according to the American Academy of Oral and Maxillofacial pathology: 1) Presence of a well-defined band-like zone of cellular infiltration consisting mainly of lymphocytes in the superficial part of the connective tissue; and 2) Signs of "liquefaction degeneration" in the basal layer; and 3) Absence of epithelial dysplasia [17]. Patients with lesions that did not reflect the above strict histological criteria were not included in the study. Cases accompanied by secondary inflammation with ulcer/erosion and evidence of malignancy were also excluded.
The normal oral mucosae were obtained through polypectomy from the perilesional areas of fibrous polyps without epithelial dysplasia to constitute the control group (5 males, 5 females, 7 buccal mucosae, 2 tongues, 1 gingiva). Four oral pathologists blinded to the biopsy material made the histopathological diagnosis of OLP, and the assessments of immunohistochemical staining. Histopathological and immunohistochemical evaluations were identical among 4 oral pathologists.
One set of sections was stained with hematoxylin and eosin (HE) under standard methods and reviewed by two oral pathologists to confirm the diagnosis and identify histological characteristics. Immunohistochemical studies were conducted using 10% neutral formalin solution-fixed, paraffin-embedded tissues from all cases. Six serial sections (each 4 µm thick) were prepared and deparaffinized in xylene and hydrated in graded ethanol solution for further immunohistochemical analysis to calculate microvascular irregularities. The EnVision + Polymer System (Dako, Glostrup, Denmark), which also carries secondary antibody molecules, was used for antigen detection. To measure angiogenic activity in this study, a Pan-endothelial marker CD34 (QBEnd 10, 1:100; Dako) and smooth muscle actin (SMA) (1A4, 1:100; Dako) were used to stain microvessels. Sections were developed in a solution of 3,3'-dianibobenzidine tetrahydrochloride. Finally, all sections were counterstained with Mayer's hematoxylin. Muscle tissue and granulation tissue were used as positive controls for SMA and CD34, respectively. For evaluation of the immunohistochemical staining technique, mouse and rabbit universal g-negative controls (Dako) were used as negative controls during the staining procedure instead of primary antibodies. Slides were examined with light microscopy and projected on a color monitor.
Sections with SMA and CD34 immunoreactivities (1 section each) were used to decide fields for microvascular morphological observation. Regarding the run of blood vessels, the most prominent areas of OLP, sites adjacent to the lesion and normal mucosae were compared histologically. After immunohistochemical observation, entire sections with SMA reactivity were scanned microscopically at low power (×40) to identify hot spots, as the areas with the highest number of microvessels. Individual regional microvessels were then counted under high power (×200) and calculated as the average value ± standard deviation of 3 fields to evaluate microvascular morphology. Decisions on hot spots and microvascular measurements were performed manually by two independent investigators without any previous knowledge of the patient's pertinent clinical data. To evaluate micro vessel morphology, the SMA-positive vessel area was converted into a binary format image and changes in microvessel area and the angle of the course of the capillary in the submucosa were estimated. Angle of the course of the capillaries to the virtual basal membrane, i.e., the virtual basal membrane was parallel to the superficial layer, were used to define capillary loop angles (Figure 1). Average areas and capillary loop angles were measured using Win Roof version 3.4 image analysis software (Image J, NIH, USA) under microscopic observation.
 Figure 1: Histopathological evaluations of microvascular morphology were compared between prominent area of oral lichen planus and the site adjacent to the lesion. The angle of the course of the capillary in the submucosa to the basal membrane is defined as the capillary loop angle. View Figure 1
Figure 1: Histopathological evaluations of microvascular morphology were compared between prominent area of oral lichen planus and the site adjacent to the lesion. The angle of the course of the capillary in the submucosa to the basal membrane is defined as the capillary loop angle. View Figure 1
All statistical analyses were performed using SPSS for Windows version 14. OJ (IBM, Tokyo, Japan). Statistical analyses were performed using the Kruskal-Wallis test and Steel-Dwass test. Values of P < 0.05 were considered significant.
Informed consent was obtained from all individuals included in the study. All procedures performed in studies involving human participants were in accordance with the ethical standards of the Committee on Studies Involving Human Beings of Nihon University School of Dentistry at Matsudo (EC-15-14-033-1) and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
The distribution of clinico-pathological findings is shown in Table 1. The symptomatic region of the 96 sites in the 42 patients were the buccal mucosa in 72 (75.0%), gingiva in 13 (13.5%), tongue in 7 (7.3%), lip in 3 (3.1%), and palate in 1 (1.0%). Details of the most prominent areas at 73 sites were the buccal mucosa in 70 (95.9%), lip in 2 (2.7%) and tongue in 1 (1.4%). Brant's classification was white in 43 (58.9%) and red in 30 (41.1%). Andreasen's classification was reticular in 60 (82.2%), erosive in 6 (8.2%), erosive + reticular in 5 (6.8%), atrophic in 1 (1.4%) and reticular and white patch in 1 (1.4%).
Histopathological findings are provided in Table 2. Representative images of characteristic findings focused on IPCLs are shown in Figure 2 and Figure 3 (a1-d1, a1-d2), respectively. Concerning clinically white/reticular regions (Figure 2a and Figure 2b), the surface was covered by hyper- and/or parakeratotic stratified squamous cells with frequent saw-toothed rete ridges (Figure 2a). Separation of the epithelia-mesenchymal junction (Max Joseph spaces) was occasionally observed (Figure 2b). Compact, band-like lymphocytic infiltrating cells hugging the epithelia-mesenchymal junction were identified (Figure 2a, Figure 2b and Figure 2c). Regarding clinically red/erosive regions, the surface was covered by thinning and flattening of the epithelium (Figure 2c) or dropped out (Figure 3d1). A compact band-like, subepithelial inflammatory infiltrate hugging the epithelia-mesenchymal junction was also observed. Erosions merely showed destruction of the epithelium and lifting fibrin and granulating connective tissue in the floor of the region (Figure 2d, Figure 3d1 and Figure 3d2). Liquefaction degeneration was always seen in both types. Regardless of the color of the most prominent region, colloid/Civatte bodies, degenerating keratinocytes (Figure 2e; arrow), melanin deposition (arrows) and melanophores (arrowheads) (Figure 2c; in the square) and micro-hemorrhages (Figure 2f) were often seen in the epithelium and/or at the connective tissue. Figure 4 shows appearance rates of histopathological findings in all cases. Appearance rates of histopathological characteristics except for the 3 criteria, 1) Presence of a well-defined band-like cellular infiltration, 2) "Liquefaction degeneration" in the basal layer and 3) Absence of epithelial dysplasia [17], in all cases were: acceleration of keratinization, 100.0%; frequent saw-toothed profile of rete ridges, 69.0%; melanin deposition, 35.7%; micro-hemorrhages, 30.2%; appearance of Civatte bodies, 25.6%; Max Joseph spaces, 16.7%; and dyskeratosis, 11.9%.
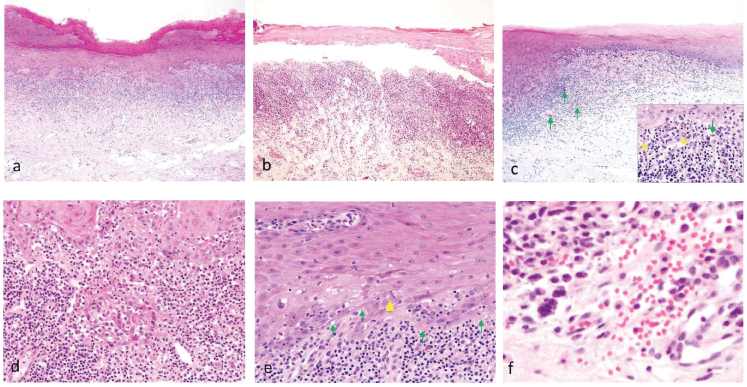 Figure 2: Characteristic histopathological findings of oral lichen planus (HE). a) Surface is covered by hyperkeratotic stratified squamous cells with saw-toothed rete ridges, and band-like lymphoplasmacytic cells are seen infiltrating at the epithelio-mesenchymal junction (×10); b) Max Joseph spaces are observed (×10); c) Surface is covered by thinning and flattening of the epithelium with band-like lymphocytic infiltration (×10). Arrows, melanin deposition; arrowheads, melanophores (×60, in the square); d) Fibrin and granulating connective tissue exist in the floor of the erosive lesion (×60); e) Liquefaction degeneration in basal cells at the epithelio-mesenchymal junction is evident (arrows), and Civatte bodies exist at the bottom of the epithelial layer (arrowhead) (×60); f) Micro-hemorrhages around IPCLs (×100). View Figure 2
Figure 2: Characteristic histopathological findings of oral lichen planus (HE). a) Surface is covered by hyperkeratotic stratified squamous cells with saw-toothed rete ridges, and band-like lymphoplasmacytic cells are seen infiltrating at the epithelio-mesenchymal junction (×10); b) Max Joseph spaces are observed (×10); c) Surface is covered by thinning and flattening of the epithelium with band-like lymphocytic infiltration (×10). Arrows, melanin deposition; arrowheads, melanophores (×60, in the square); d) Fibrin and granulating connective tissue exist in the floor of the erosive lesion (×60); e) Liquefaction degeneration in basal cells at the epithelio-mesenchymal junction is evident (arrows), and Civatte bodies exist at the bottom of the epithelial layer (arrowhead) (×60); f) Micro-hemorrhages around IPCLs (×100). View Figure 2
Table 2: Histopathological details of all cases. View Table 2
In normal mucosa, small, round IPCLs were present in the submucosa (Figure 3a1 and Figure 3a2). Elongated IPCLs were prominent and ran vertically to the basal membrane in the most prominent areas of white and red types of OLP (Figure 3c1, Figure 3c2, Figure 3d1 and Figure 3d2). Regardless of the classification from clinical inspection, IPCLs ran obliquely to the basal membrane at the sites adjacent to the lesion (Figure 3b1 and Figure 3b2).
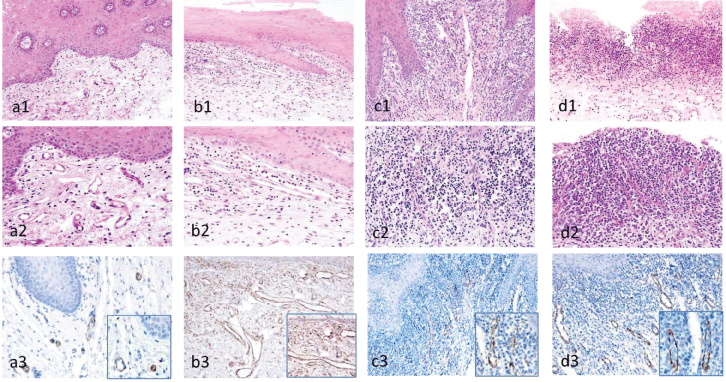 Figure 3: Images focused on IPCLs.
Figure 3: Images focused on IPCLs.
a) Normal mucosa: 1) Small IPCLs in the submucosa (HE, ×20); 2) Slight infiltration of lymphocytes and round IPCL (HE, ×40); 3) Small IPCLs with positive staining for SMA (SMA, ×40), and high-power magnification in the square (SMA, ×60).
b) Sites adjacent to the lesion: 1) Elongated/slightly expanded IPCLs run at an angle to the basal membrane in the sites adjacent to the lesion (HE, ×20); 2) IPCL area is bigger than normal and prominent areas (HE, ×40); 3) Elongated/slightly expanded IPCLs staining positive for SMA (SMA, ×40), with high-power field shown in the square (SMA, ×60).
c) Main lesion with keratotic epithelium: 1) Elongated IPCLs are prominent, and run vertically to the basal membrane (HE, ×20); 2) Strong infiltration of lymphocytes and swelling of endothelial cells of IPCLs (HE, ×40); 3) Elongated IPCLs run vertically with positive for SMA (SMA, ×40), and high-power field in the square (SMA, ×60).
d) Erosive main lesion: 1) Elongated IPCLs are prominent, and run vertical to the basal membrane (HE, ×20); 2) Strong infiltration of lymphocytes and swelling of endothelial cells of IPCLs (HE, ×40); 3) Expanded IPCLs are prominent, and run vertical to the basal membrane (SMA, ×40), with high-power field shown in the square (SMA, ×60). View Figure 3
Microscopic images with immunohistochemical staining using SMA antibody are shown in Figure 3 (Figure 3a3, Figure 3b3, Figure 3c3 and Figure 3d3). In normal mucosa, small round capillaries were observed just below the basal membrane (Figure 3a3). Elongated/slightly expanded IPCLs ran obliquely to the basal membrane at the sites adjacent to the lesion (Figure 3b3), and elongated IPCLs ran vertically in the most prominent areas of white and red types of OLP (Figure 3c3 and Figure 3d3).
Average areas (Figure 4a) and capillary loop angles (Figure 4b) of normal mucosa, the most prominent areas of OLP, sites adjacent to the lesion and erosive areas are shown in Figure 4.
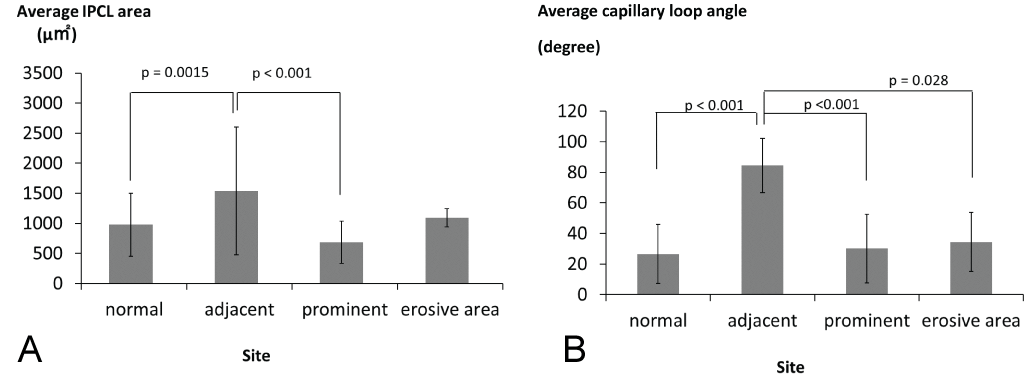 Figure 4: Results of IPCL histomorphometrical evaluation of oral lichen planus (normal: Normal mucosa, adjacent: Sites adjacent to the lesion, prominent: The most prominent areas, erosive: Erosibe areas). a) Average IPCL area of normal mucosa and lichen planus. A significant difference is apparent between the sites adjacent to the lesion and the most prominent areas of lichen planus (p < 0.001); b) Average capillary loop angles of IPCLs in normal mucosa and lichen planus. A significant difference is seen between the sites adjacent to the lesion and the most prominent areas of lichen planus (p < 0.001) and normal mucosa of lichen planus (p < 0.001). View Figure 4
Figure 4: Results of IPCL histomorphometrical evaluation of oral lichen planus (normal: Normal mucosa, adjacent: Sites adjacent to the lesion, prominent: The most prominent areas, erosive: Erosibe areas). a) Average IPCL area of normal mucosa and lichen planus. A significant difference is apparent between the sites adjacent to the lesion and the most prominent areas of lichen planus (p < 0.001); b) Average capillary loop angles of IPCLs in normal mucosa and lichen planus. A significant difference is seen between the sites adjacent to the lesion and the most prominent areas of lichen planus (p < 0.001) and normal mucosa of lichen planus (p < 0.001). View Figure 4
Mean IPCL areas were 978.0 ± 523.7 µm2, 1537.1 ± 1061.4 µm2, 689.0 ± 351.9 µm2 and 1092.1 ± 153.3 µm2 for normal mucosa, site adjacent to the lesion, prominent areas of OLP and erosive areas, respectively. Significant differences were observed between prominent areas of OLP and site adjacent to the lesion (p < 0.001). Area of IPCLs tended to be larger in sites adjacent to the lesion than in normal mucosa.
Capillary loop angles were 26.6 ± 19.3°, 84.5 ± 17.8°, 30.2 ± 22.4° and 34.4 ± 19.3° for normal mucosa, site adjacent to the lesion, prominent areas of OLP and erosive areas, respectively. Significant differences were observed between normal mucosa/prominent areas of OLP and site adjacent to the lesion (p < 0.001). IPCL angle tended to be larger at site adjacent to the lesion than at the erosive areas.
OLP is a chronic inflammatory disease without a clear pathogenesis [9] and was included in OPMDS in WHO 2017 [3]. Various oral manifestations have been described, with the reticular type according to Andreasen's classification representing the most frequent, comprising almost 80% of all cases in this study. Because of the complicated nature of Andreasen's classification, OLP is often classified clinically as reticular or erosive [18]. The reticular type according to Brant's classification was higher in this study, and it was concordance with previous study [18]. The incidence of OLP is greater among women between 30 and 60-years-old [20,21]. The most frequent site is the buccal mucosa, followed by the tongue and gingivae [6]. Characteristics of OLP cases in this study were similar to previous published reports.
As a clinicopathologic correlation is required for the diagnosis of OLP, all patients in whom a diagnosis of OLP is being considered require histopathological evaluation. The clinical condition of OLP changes according to disease progression and its site. Patients presenting with mucosal alterations and a region distribution fully consistent with OLP may thus only require a single tissue sample for histopathological evaluation. Conversely, the number of tissue samples to be obtained is guided by several considerations. Histopathological cases of "suspected OLP" lack the characteristic features of "liquefaction degeneration in the basal cell layer" and "Civatte body formation". In addition, in terms of chronic inflammatory changes, a dense subepithelial lympho-histiocytic infiltrate and increased numbers of intra-epithelial lymphocytes are also characteristic. This pattern of inflammatory change has been termed "interface mucositis", which is also encountered in oral regions of lupus erythematosus and in additional oral lichenoid conditions [22,23]. Pathologically, a "lichenoid region" exhibits a similar histologic pattern to OLP with definite causes. In addition, pathological diagnosis of OLP is difficult, particularly clinically diagnosed erosive OLP [24]. The differential diagnosis of erosive OLP includes squamous cell carcinoma, discoid lupus erythematosus and chronic candidiasis. In addition, the plaque form of reticular OLP can resemble oral leukoplakia [25]. Nevertheless, indirect immunofluorescence yields negative results and is not a useful technique for diagnosing OLP [9].
The precision of diagnosis is therefore regarded for these reasons as a problem in OLP biopsy, and supplementary examination methods are needed. As for direct oral microscopy, a pilot study described an unclear subepithelial capillary pattern of lichenoid region [26]. Scardina actively performed in vivo observation of angiogenesis in OLP by video-capillaroscopy [16]. Angiogenesis was interpreted as an increase in capillary density, diameter and tortuosity, total vascular caliber, and branched loops, indicating the angiogenic phenomenon of OLP in vivo, was significantly increased compared to normal mucosa [16,27]. However, in recent years, Drogoszewska used direct oral microscopy for OLP to observe surface pattern, color tone, borders of the lesion and subepithelial mucosal vessels [28]. Twenty percent erosive OLP showed visible numerous thin, elongated subepithelial hairpin capillaries under green filter [26]. Other differential diagnoses should be observed with a focus on IPCLs. OLP, like any analogous chronic inflammatory disease, shows significant secondary angiogenesis in response to the hypoxic effect on the inflamed stromal area. Angiogenesis represents a cycle of vital processes that leads to the formation of new blood vessels starting from pre-existing vascular structures [29], and regions represent a fundamental process in the pathogenesis of chronic inflammatory pathologies and contemporarily represent the base of OLP activity [14].
Concerning the histopathological evaluation of microvessels, some studies have evaluated microcirculation characteristics in the presence of OLP [30-35]. Microvessel density in OLP regions was observed to be significantly higher than in control specimens in previous studies [34,35]. However, López de Blanc, et al. reported the number of blood vessels was not increased, but the increased vessels area indicated that OLP is a more congestive region [33]. Furthermore, a significant increase in number of capillaries is seen in oral lichenoid mucositis compared to OLP, and this could be used as an adjunct histologic criterion in the diagnosis of OLP [36].
Concerning the relationship between IPCL and clinical condition of OLP, angiogenesis and expression of vascular endothelial growth factor correlated closely with the different clinical forms of OLP regions [13,37,38]. Mittal, et al. suggested that angiogenesis was significantly increased in OLP as compared to normal oral mucosa, and also in erosive OLP as compared to reticular OLP; this suggests angiogenesis as a main contributing factor in the progression of OLP [13]. However, no histopathological studies appear to have examined the morphology and course of IPCLs in OLP. In the present study, average capillary angle and area is much higher between normal and sites adjacent to the lesion and not between normal and prominent/erosive areas in this study. In prominent/erosive areas, epithelial regeneration starts from basal cells located near the erosion/ulcer caused by chronic inflammation, and granulation tissue is formed in the mesenchymal tissue. Therefore, small new vessels and elongated IPCLs by congestion were intermingled for tissue repair. Meanwhile, IPCLs around those pathological changes were expanded and ran obliquely in both reticular and erosive types of prominent areas. IPCLs in neighboring normal areas might extend and supply the prominent areas with oxygen. In addition, the presence of microhemorrhages was observed. Thirteen cases in this study showed microhemorrhages on histological examination. Erythrocytes were conjectured to have leaked due to dilation and hyperpermeability of IPCLs.
OLP shows histopathologically non-specific inflammatory changes under clinical conditions, and the pathological diagnostic criteria need to be discussed. By contrast, IPCLs are expanded and run obliquely to the basal membrane at the sites adjacent to the lesion. OLP shares several histopathological features with other muco-cutaneous lesions, thus may often be misdiagnosed. Consequently, characteristic IPCL patterns were identified in the present study irrespective of the reticular/erosive type, indicating the utility of IPCL patterns as the pathological diagnostic criteria.
This work was supported by JSPS KAKENHI Grant Number 18K07000.
Conflict of interest: The authors declare that they have no conflicts of interest.