T/NK-cell lymphoma of nasal-type was described in 1933 as a malignant medio-facial granuloma. The diagnosis of this rare condition is clinical and immunohistopathological. We report an original case of cutaneous T/NK lymphoma of the nasal type revealed by cutaneous ulcerations.
Cutaneous ulcerations, T/NK Lymphoma, Nasal-type
The cutaneous lymphoma T/NK nasal type is malignant proliferation of cytotoxic T lymphocytes (CTL). This is a particular entity associated with Epstein-Barr virus (EBV) infection, which explains, by its high prevalence in Asia, South and Central America. The development is usually aggressive with a poor prognosis.
A 31-years-old male patient, from southern Morocco, without any notable pathological history consulted for papulonodular skin lesions evolving for 6 months to ulcerations of upper limbs, lower limbs and the trunk. Context includes apyrexia and loss of weight not measured. The mucocutaneous review showed ulcerated skin lesions of the anterior aspect of the right forearm, thighs and legs without mucosal involvement (Figure 1).
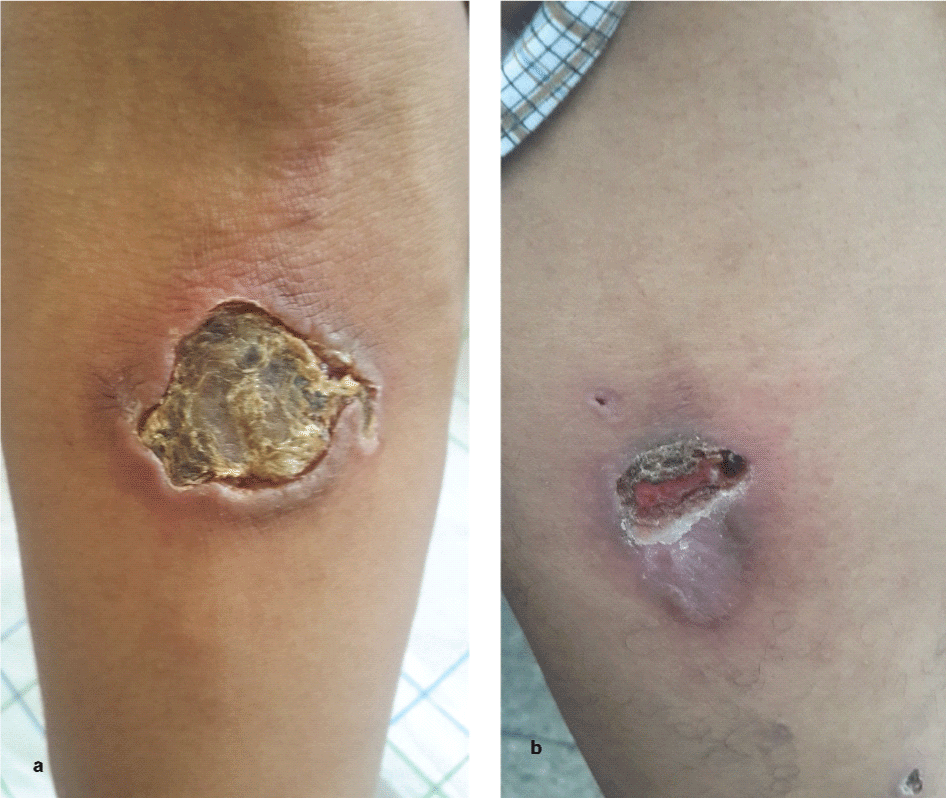 Figure 1: Skin ulcers located on the forward right arm and right thigh.
View Figure 1
Figure 1: Skin ulcers located on the forward right arm and right thigh.
View Figure 1
The review of the ear, nose and larynx was without any anomaly. The examination of the ganglionic areas showed numerous large, firm, painless adenopathies in the cervical, axillary and inguinal areas. The rest of the somatic examination was unusual.
Cutaneous histology was leaning towards cutaneous lymphoma T/NK nasal type of high grade objectifying an atypical lymphocytic infiltrate with angiocentric disposition (Figure 2). The immunohistochemistry (IHC) determines tumor cells strongly expressing CD3 and CD56 (Figure 3).
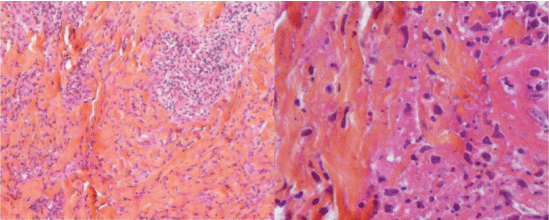 Figure 2: Histology: Lymphocytic infiltrate very atypical for a cutaneous lymphoma.
View Figure 2
Figure 2: Histology: Lymphocytic infiltrate very atypical for a cutaneous lymphoma.
View Figure 2
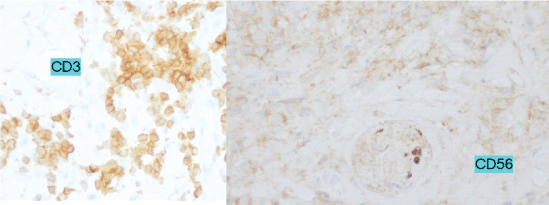 Figure 3: Immunohistochemistry: CD3+ and CD56+ markers for T/NK lymphoma nasal type.
View Figure 3
Figure 3: Immunohistochemistry: CD3+ and CD56+ markers for T/NK lymphoma nasal type.
View Figure 3
The Polymerase chain reaction (PCR) testing for EBV was positive. A CT scan of facial bones showed thickening of the right nostril. Nasal and lymph node biopsy were in favor of T/NK Lymphoma. The bone marrow biopsy was normal. The remaining tests were normal; however they identified an inflammatory syndrome with a slight increase in markers of the tumor mass.
An T/NK Lymphoma nasal type was diagnosed. A poly-chemotherapy was started. A bone marrow transplant was also considered. The disease evolved rapidly; the patient died after his first chemotherapy session (CHOP Protocols).
We report an original case of a cutaneous T/NK Lymphoma Nasal type revealed by skin ulcerations stressing how important to refer to this diagnosis in presence of chronic cutaneous ulcerations resistant to usual treatments. In view of this clinical case, several diagnoses have been mentioned, in particular, ecthyma, pyoderma gangrenosum, leishmaniasis or cutaneous tuberculosis. Cutaneous histology associated with immunohistochemistry license to the diagnosis by objectifying an atypical lymphocytic infiltrate at angiocentric disposition, with cells strongly expressing CD3 and CD56 markers.
T/NK-cell lymphoma nasal type accounts for 5 to 18% of non-Hodgkin's lymphoma [1,2]. Primarily affecting the populations of Southeast Asia, Central and South America, it is rare in Europe and the United States [2,3]. A male predominance is observed [4].
The extra-nasal forms of T/NK Lymphoma account for 20% of cases [5]. Primary skin involvement is reported from 10 to 26% of T/NK Lymphoma nasal type. A longer delay in proper diagnosing this disease and a different visceral involvement explain why prognosis of these extra-nasal forms is worse [4]. The cutaneous involvement is mainly in the form of infiltrated erythematous plaques capable of mimicking a panniculitis or a dermo-hypodermitis, with a tendency to necrosis and ulcerates. Sub-cutaneous nodules may also be the mode of dissemination of the disease [3].
Histologically, T/NK Lymphoma nasal types are characterized by an atypical lymphocytic infiltrate at angiocentric disposition with angioinvasion phenomena. Nevertheless, this presentation would be less frequent in T/NK Lymphoma nasal-type with primary cutaneous localization [6]. In immunohistochemistry, tumor cells usually express phenotypic markers of NK cells, including CD2 and CD56, and show intracytoplasmic CD3 expression indicating the presence of the CD3 epsilon chain, detectable only with polyclonal antibodies. There is an expression of cytotoxicity markers such as perforin, granzyme B and TIA-1 (T-cell Intracellular Antigen-1). In our case, tumor cells are strongly correlated to CD56 and CD3 markers.
. EBV is always detected when searched by hybridization of tumor cells or Polymerase chain reaction (PCR) in the patients' peripheral blood classifying lymphoma T/NK extra-nasal among lymphomas EBV-induced. PCR detects generally very high rates of the ADN of EBV in the blood of patients. These EBV-DNA levels reflect tumor volume, constituting a marker of prognosis and therapeutic response [7].
The treatment of extra-nasal T/NK Lymphomas is difficult. Indeed, the expression of the glycoprotein P by tumor cells gives them resistance to multiple chemotherapies, by exporting these drugs to the extracellular medium: This is notably the case with vincristine and with anthracyclines such as doxorubicin, and chemotherapies conventionally used in the CHOP protocols [5,8,9]. Radiation therapy is effective, but unable to prevent tumor recurrences away from the irradiated area. It is a lymphoma of high grade malignancy and poor prognosis: recurrence-free survival and overall survival are respectively 6 and 9% in 5 years [2].
Extra-ganglionic T or T/NK lymphoma Nasal type is a rare form of non-Hodgkin's lymphoma. The skin represents the second body part affected by this type of lymphoma. This observation highlights the interest of seeking nasal involvement in the case of T-cell lymphoma nasal type that has started on the skin.
The authors declare having no conflicts interest related to this article.