The origin of ovarian epithelial tumors is still indistinct. Müllerian and coelomic hypothesis are controversial. Recently, there is also a small number of reports that tubo-peritoneal junction may play an important role in the development of tubo-ovarian tumors. Therefore, we aimed to investigate the relationship between tumors originating from Mullerian epithelium and peritoneal mesothelium, in other words primary and secondary Müllerian systems.
Seventy malignant tumors originating from the Müllerian epithelium and peritoneal mesothelium were included in the study. Tumors were analysed immunohistochemically for PAX8, WT1, CD56, Ber-EP4, ER and desmin expression. We evaluated the study based on three phases. Firstly, we investigated immunohistochemical stainings of different tumor types in different locations. Secondly, we assessed immunohistochemical characteristics according to their histologicals subtypes, and finally their relationship with primary or secondary Müllerian systems.
As a result different immunohistochemical features were detected between both localization and histological types of these tumor groups.
Absence of immunoreactivity of PAX8, WT1 and CD56 in endometrial serous carcinomas and, the presence of high immunoreactivity in ovarian and tubal serous carcinomas was considered to be an indicator of different origins of these tumors as primary and secondary Müllerian systems. It also seems possible that tubo-peritoneal junction could be the junction between primary and secondary Müllerian systems and, may play an important role in the development of tubo-ovarian tumors.
Müllerian system, Coelomic epithelium, Mesothelium, Ovarian surface epithelium, Malignant tumors, Immunohistochemistry
One of the most curious features of ovarian epithelial neoplasms is their histogenesis. The true source of origin of these normal cell types giving rise to these tumors is unclear. In some of these epithelial ovarian tumors, the cell morphology is indistinguishable from neoplasms arising from those organs of the female genital tract that are embryologically derived from Müllerian ducts just as the serous, the mucinous and the endometrioid types resemble the neoplasms of fallopian tubes, endocervix and endometrium, respectively. Besides, in most cases, primary peritoneal serous carcinomas (PSC), peritoneal malignant mesotheliomas (PMM) and also metastatic ovarian tumors showing similarity with ovarian serous carcinomas (OSC) have difficulties in discriminating. Since the treatment approaches are different in these tumor types, it is very important to achieve the definite diagnosis [1-3]. Lauchlan used the term secondary Müllerian system (SMS) to designate the structures lined by Müllerian epithelium found outside the fallopian tubes, uterus, and cervix while fallopian tubes, uterus, cervix and upper part of vagina derived from Müllerian ducts are called as primary Müllerian system (PMS) [4]. So, SMS is seemed to be the source of paraovarian and paratubal cysts, rete ovarii, endosalpigiosis, endometriosis and endocervicosis. Although ovary is not originated from PMS, it can contain SMS structures such as Müllerian duct remnants, rete ovarii, endosalpingiosis, endometriosis, and endocervicosis [4]. The coelomic epithelium ultimatelly links to the extraovarian mesothelium that is the region of tubo-peritoneal junction (TPJ) [5]. Since the junctions between different types of epithelia are designated as hot spots for carcinogenesis, the junction of the peritoneal mesothelium with the fallopian tubal epithelium may play a role in the development of these tumors [5]. The role of epithelial junctions, notably the cervical squamocolumnar, gastroesophageal, and anorectal junctions in neoplasia was well recognized but the junction of the columnar tubal epithelium with the mesothelial serosa on the fimbriae has rarely been mentioned in the literature. If regional junctions is important in carcinogenesis then the TPJ should be of particular interest [5]. On the other hand, ovarian surface epithelium is considered as modified pelvic mesothelium, originates from coelomic mesoderm, and is reported to have in both mesenchymal and epithelial properties unlike the tubal and the endometrial epithelium developing from PMS. These spesific features of ovarian surface epithelium may partly explain the different characteristics of the tumors with similar morphology originated from PMS and SMS [3,6-11]. In this study our aim is to investigate the relationship between tumors originating from Müllerian epithelium and peritoneal mesothelium, and also to contribute in differential diagnosis of these tumors by using six immunohistochemical (IHC) markers.
Cases that were diagnosed between 2005 and 2011 and diagnosed as OSC and tubal serous carcinomas (TSC) from the ovary and tuba; endometrioid carcinoma (EEC) and serous carcinoma (ESC) from the endometrium; PSC and PMM from the peritoneum were obtained from the archival records in the Department of Pathology at Cumhuriyet University Hospital, Sivas, Turkey. Patients age and tumor localizations were retrieved from the medical records. The histologic diagnosis of each tumor was confirmed on the hematoxylin and eosin stained sections. Twenty cases of OSC, 31 cases of EEC, 4 cases of ESC, 8 cases of TSC, 4 cases of PMM and 3 cases of PSC composed of totally 70 cases were included in this study. Cases in the study were divided into three groups as serous carcinoma (SC), endometrioid carcinoma (EC), and malign mesothelioma (MM) according to their histologic types. Moreover, cases were also divided into two groups as PMS tumors which were located distal to the TPJ and assumed to be derived from Müllerian ductus, and SMS tumors which were located proximal to the TPJ and assumed to be derived from modified mesothelium. Thus, EEC and ESC cases were evaluated as PMS tumors; OSC, TSC, PSC and PMM cases were considered as SMS tumors. H&E stained sections of the cases re-evaluated and the slides were selected from parafin blocks containing representative tumor without necrosis. Sections of 3 μm thickness were taken from these parafin blocks to Poly-L-Lysine covered slides. All of the cases were analysed IHC with PAX8 (a sensitive and spesific marker for Müllerian originated tumors), WT1 (a marker for both Müllerian and mesothelial origin), CD56 (a newly defined and very sensitive marker for ovarian sex cord stromal tumors), Ber-EP4 (an epithelial marker), ER (a marker having an important role in development and treatment of gynecological tumors), and desmin (a mesenchymal marker). Avidin-biotin peroxidase IHC method was applied to selected sections using a panel of antibodies to PAX8 (Cell Marque rabbit policlonal antibody, Clone 112970.2A, 1:50 dilution ratio), WT1 (Dako, Mouse Monoclonal Antibody, Clone 6f-H2, 7.0 ml ready to use form), CD56 (Thermo Scientific, Mouse Monoclonal Antibody, Clone 123C3.D5, 7.0 ml ready to use form), Ber-EP4 (Biocare Medikal, Mouse Monoclonal Antibody, Clone Ber-EP4, 7.0 ml ready to use form), ER (Dako, Rabbit monoclanal antibody, clone EP1, 7.0 ml ready to use form) ve desmin (Scytek, Mouse Monoclonal Antibody, Clone D33, 7.0 ml ready to use form).
Nuclear staining for PAX8, WT1 and ER; membranous staining for Ber-EP4 and CD56; cytoplasmic staining for desmin were accepted as positive. Furthermore, positive control slides were prepared for each IHC stain. Immunoreactivity was scored semiquantitively based on intensity of staining and percentage of immunoreactive area [12]. The intensity of stained cells was scored as 0 ( no staining), 1+ (weak staining), 2+ (moderate staining), 3+ (strong staining). The percentage of immunoreactive area was scored as 1 (less than 10%), 2 (10% to 50%), 3 (52% to 80%), and 4 (more than 80%). For each case, the values of the two parameters (predominant intensity and percentage of the positive cells) were multiplied, resulting in scores from 0 to 12. Final score was classified as negative or low reactive (score 0-1), moderate (scores 2-6), and high (scores 8-12). For the values obtained for each antibody, cases were again scored by giving numerical values as negative or low (1), moderate (2), and high (3) for statistical data.
 Figure 1: Immunohistochemical staining for PAX8. A) score 3, in OSC (X 100); B) score 3, in TSC (X 200); C) score 1, in ESC (X 100); D) score 3, in EEC (X 100); E) score 3, in PSC (X 200) and F) score 2, in PMM (X 200).
View Figure 1
Figure 1: Immunohistochemical staining for PAX8. A) score 3, in OSC (X 100); B) score 3, in TSC (X 200); C) score 1, in ESC (X 100); D) score 3, in EEC (X 100); E) score 3, in PSC (X 200) and F) score 2, in PMM (X 200).
View Figure 1
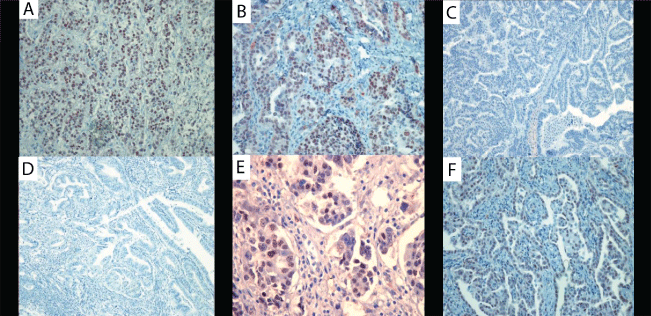 Figure 2: Immunohistochemical staining for WT1.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 200); C) score 1, in ESC (X 100); D) score 1, in EEC (X 100); E) score 2, in PSC (X 400) and F) score 3, in PMM (X 200).
View Figure 2
Figure 2: Immunohistochemical staining for WT1.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 200); C) score 1, in ESC (X 100); D) score 1, in EEC (X 100); E) score 2, in PSC (X 400) and F) score 3, in PMM (X 200).
View Figure 2
Data were installed to SPSS 14.0 (SPSS Inc, Chicago, III, USA) program. Kruskal-Wallis, Mon-Whitney U and Chi-square tests were used to evaluate the data analysis. Values with p < 0.05 were accepted as statistically significant.
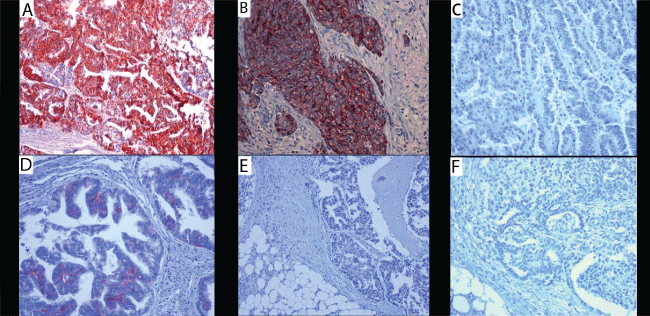 Figure 3: Immunohistochemical staining for CD56.
A) score 3, in OSC (X 200); B) score 2, in TSC (X 400); C) score 1, in ESC (X 200); D) score 2, in EEC (X 400); E) score 1, in PSC (X 100) and F) score 1, in PMM (X 200).
View Figure 3
Figure 3: Immunohistochemical staining for CD56.
A) score 3, in OSC (X 200); B) score 2, in TSC (X 400); C) score 1, in ESC (X 200); D) score 2, in EEC (X 400); E) score 1, in PSC (X 100) and F) score 1, in PMM (X 200).
View Figure 3
 Figure 4: Immunohistochemical staining for Ber-EP4.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 200); C) score 2, in ESC (X 400); D) score 3, in EEC (X 200); E) score 3, in PSC (X 200) and F) score 1, in PMM (X 100).
View Figure 4
Figure 4: Immunohistochemical staining for Ber-EP4.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 200); C) score 2, in ESC (X 400); D) score 3, in EEC (X 200); E) score 3, in PSC (X 200) and F) score 1, in PMM (X 100).
View Figure 4
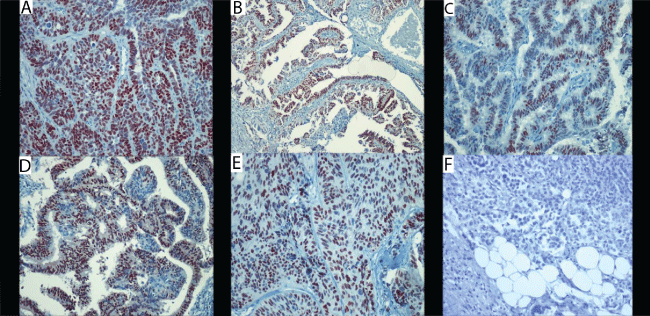 Figure 5: Immunohistochemical staining for ER.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 100); C) score 2, in ESC (X 200); D) score 3, in EEC (X 200); E) score 3, in PSC (X 200) and F) score 1, in PMM (X 400).
View Figure 5
Figure 5: Immunohistochemical staining for ER.
A) score 3, in OSC (X 200); B) score 3, in TSC (X 100); C) score 2, in ESC (X 200); D) score 3, in EEC (X 200); E) score 3, in PSC (X 200) and F) score 1, in PMM (X 400).
View Figure 5
Of the 70 cases included in the study, 20 (29%) cases were OSC, 8 (11%) cases were TSC, 4 (6%) cases were ESC, 31 (44%) cases were EEC, 3 (4%) cases were PSC, and 4 (6%) cases were PMM. The age of the youngest in the overall evaluation of patients was 34 and the oldest was 85-years-old and the average age was 60.5 ± 19.9. The mean age, the standard deviation, and the ages of the youngest and the oldest of the tumor groups were shown in Table 1. Statistical analysis of the IHC results of all tumors belonging to groups PAX8, WT1, CD56, Ber-EP4, ER, and desmin expressions was shown in Table 2. According to the histological types we divided the tumors into three groups as SC, EC and MM, tumors of the 70 cases were categorized as 35 cases of (50%) SC, 31 cases of (44.3%) EC, and 4 cases of (5.7%) MM. Of the SCs, 20 tumors were localized at the ovary, 8 at the fallopian tube, 4 at the endometrium, and 3 in the peritoneal cavity. Immunoreactive histological types stained with markers were shown on Table 3, Figure 1, Figure 2, Figure 3, Figure 4 and Figure 5. Tumors which were divided into two groups as PMS and SMS according to origin and their IHC staining characteristics were shown in Table 4. Each group was consisted of 35 patients (50%). In tumors of the PMS group, 31 (88.6%) were EEC, 4 (11.4%) were ESC; and in tumors of the SMS group, 8 (22.9%) were TSC, 20 (57.1%) were OSC, 3 (8.6%) were PSC, and 4 (11.4%) were PMM. As a result values of six different markers in different six tumor groups were found significant (p < 0.05) except desmin. Epithelial marker was all reactive in tumors except peritoneal malignant mesotheliomas whereas no expression was detected with mesenchymal marker in tumor groups. PAX8, ER and Ber-EP4 were found to be useful in differential diagnosis between serous carcinomas and peritoneal malignant mesothelioma. WT1 was found to be useful in differential diagnosis between serous carcinomas originated from primary and secondary Müllerian system and CD56 was found to be useful in differential diagnosis of ovarian and tubal serous carcinomas from peritoneal malignant mesotheliomas.
Table 1: The age distribution of cases. View Table 1
Table 2: Statistical analysis of the immunohistochemical results for all groups. View Table 2
Nowadays, Müllerian and coelomic hypothesis about the origin of ovarian epithelial tumors are still controversial [6,8]. Although it is widely accepted that ovarian epithelial tumours arise in the coelomic epithelium that covers the ovarian surface, researches conducted recently regarding the origin of ovarian cancer has begun to alter the classical information and in view of these findings are that the origin of serous carcinomas is tubal fimbrial epithelium in most cases [7,8,13]. The idea that different types of epithelial junctions is considered as hot spots in carcinogenesis, TPJ could be a source of serous carcinomas. But this site cannot account for all of these tumours, some of which are most likely derived from components of the SMS [6-8,10,13-19]. In the light of these findings it is assumed that serous carcinomas usually have fimbriated origin, endometrioid and clear cell carcinomas have endometrial origin, whereas Brenner and mucinous tumors may arise from fimbrias by transitional metaplasia [5,11].
Table 3: The distribution of cases according to tumor type and their immunoreactive features**. View Table 3
Table 4: Distribution of cases according to PMS and SMS and their immunoreactive features**. View Table 4
OSC, TSC, ESC, PSC, and tubulopapillary pattern of PMM are histologically similar tumors to each other. Panels including a large number of IHC markers such as p53, WT1, calretinin, D2-40, mesothelin, trombomodulin, CA125, HBME-1, LeuM1, CEA, CK20, CK7, Ber-EP4, CK5/6, EMA, ER, and PR are used in differential diagnosis.
In this study, exclusively tumors arising from the Müllerian system and peritoneal mesothelium were considered. Possible relationships of the tumors were investigated according to the expressions of the six IHC markers. In the selection of markers we have taken into account for; the high sensitivity and specificity of PAX8 which is recently identified as a Müllerian determinant; WT1 which is included mesothelioma panel but only recently identified as a determinant of Mullerian; CD56 which is a sensitive marker for neuroendocrine tumors but recently stated to be of diagnostic value for ovarian sex cord stromal tumors, and it has not been studied enough yet in gynecological malignancies. Determinants were also taken into account in the selection of Ber-EP4 as an epithelial, and desmin as a mesenchymal marker to assist the origin of these tumors whether they were epithelial or mesenchymal. Ultimately, ER, especially recently, which plays an important role in the differential diagnosis of PMM and OSC were also included in the study.
Statistical analysis of the expression values of PAX8, WT1, CD56, Ber-EP4, and ER in different tumor groups were found to be significant except desmin (p < 0.05). In the literature, there are studies that show the ovarian surface epithelium has both mesenchymal and epithelial features that makes it different than both endometrial or fallopian tube epithelium. Accordingly, the surface epithelium stains with vimentin, N-cadherin, calretinin, HBME1, CK7, and Ber-EP4 but it does not usually stain with CK20, and CA125 [1,3,9]. Besides, combinations of calretinin with Ber-EP4 as a marker of epithelial determinant which shows high expression in SC, and with ER that has an important role in the development of genital tract have been reported to be quite useful in the differential diagnosis of OSC with PMM [20-23]. In the study of Mozes, et al. it has been reported that ER reactivity was demonstrated in 64.3% (36/56 cases) of OSC, 10.7% (4/37 cases) of ESC and 16.7% (1/6 cases) of TSC, whereas all PSC cases (5 cases) were negative [24]. In particular, since Ber-EP4 is expressed in SCs in high levels, it is an important marker used in the differentiation of SC and PMM [20-22,25]. High rate of ER positivity is observed in OSC. Especially recently, it has an important role in the differential diagnosis of PMM and OSC. In addition, it is often used routinely in the differential diagnosis, due to negative expression in the SCs of female genital tract [11,26]. In contrast, EECs are usually positive for ER. Calretinin, Ber-EP4, ER combination is very useful in the differentiation of PMM and a primary or metastatic SC [20-22,24-26].
Concerning the Ber-EP4 expression in our study groups when analyzed according to the results; OSC, TSC, PSC, ESC and EEC have been found to be reactive with epithelial markers but PMM has not. In addition, in the evaluation of IHC staining characteristics of the tumor types defined as SC, EC, MM, epithelial marker Ber-EP4 was determined in 85.7% of SCs and in 90.4% of ECs, likewise high reactivity of ER was identified in 80% of SCs and 83.9% of ECs. In contrast, all MMs were negative with both of markers. These results can be explained by different epithelial features and estrogen sensitivity of the tumors. In fact, when this difference was evaluated statitically the differences of SC vs MM and of EC vs MM were significant (p < 0.05) in terms of Ber-EP4 and ER expressions. On the other hand, IHC staining patterns of tumors that were divided into two groups as PMS and SMS, showed no significant difference for Ber-EP4 and ER (p > 0.05). As a result, the data in this study revealed that Ber-EP4 and ER are useful markers to identify the epithelial origin as well as in the differential diagnosis of PMM and SC similar to the literature data. However, unlike the study of Mozes, et al. [24], in this study ER showed expression rate as high as 75% of ESC patients, 62.5% of TSC patients and 100% of PSC patients. The differences between two studies were thought to be due to the different antibody clones and the small number of ESC, TSC, and PSC cases. In addition, while staining ratio of ER in EEC cases (83.9%) consistent with the literature, higher staining ratio found than expected in ESC cases (75%) can be due to the small number of cases in the study.
Desmin is often used in the differential diagnosis of MM with mesothelial hyperplasia because it shows positive staining in reactive mesothelial cells and a very low rate of expression in MM [3,9,27-30]. We couldn’t find studies regarding desmin expression in relation to the ovarian surface epithelial tumors. In our study, although PMS and SMS tumors were generally positive with both Müllerian (PAX8 and WT1) and epithelial (Ber-EP4) markers, none of them react with desmin. This feature may be an indication of a loss of mesenchymal features in tumor cells. In this study, desmin were used just as a mesenchymal marker. Undoubtedly, to determine the mesenchymal properties of epithelial-stromal tumors of the ovary alone with desmin is not satisfactory alone but evaluation of desmin is thought to be guiding. In this study, all cases of PMM negatively stained with desmin was found consistent with the literature.
Recently, PAX8 has been shown to be a sensitive and specific marker for Müllerian system tumors [31-35]. Furthermore, tubal ciliated cells are negative and the secretory cells are stained positive with PAX8 and secretory cells has been suggested as the origin of OSC [31,34,36]. In addition, studies noted that PAX8 expression is quite specific in differentiating OSC than MM [31,37]. In this study, the highest rate of PAX8 expression was determined in OSC tumor group (90%). In addition, PAX8 expression was also determined in TSC, EEC, PSC and even in PMM to a lesser extent but no expression was found in ESC. In pairwise comparisons of tumor groups in terms of PAX8 expresion, differences between OSC with ESC, EEC, and PMM were found to be significant (p < 0.005).
WT1, helps the distinction of ESC from SC originating outside the uterus because it is usually negative in ESC but positive in TSC, OSC, and PSC. This difference is linked to genetic differences between tumors [38-44]. In our study we noted that although WT1 was generally positive in SC of fallopian tube, ovarian and peritoneal origin, it didn’t show positivity in EEC and ESC. This results showed us that WT1 expression may assist to differentiate ESC from SCs which is originating outside the uterus, in other words from PMS and SMS, but not useful in the differential diagnosis of OSC, PSC, TSC and PMM. In this study, WT1 expression was found as high as PAX8 in OSC (90%), and found to a lesser extent in TSC, PSC and PMM, but it was not determined in ESC and EEC. When the tumors were divided into three groups as SC, EC and MM according to histological types, and staining characteristics of PAX8 and WT1 were examined statistically, PAX8 expressions were significant in terms of the comparison of SC vs EC and SC vs MM, and WT1 expressions were significant in terms of the comparison of SC vs EC and EC vs MM (p < 0.05). In tumors divided into two groups including PMS and SMS, PAX8 expression was observed in 37.1% of PMSs and in 74.3% of SMSs, and in case of WT1, no expression was seen in PMS, while 80% of SMS tumors showed positivity. When PAX8 and WT1 values of the two groups were statistically evaluated in terms of the value of the PAX8 and WT1 difference was significant (p < 0.005).
Studies associated with CD56 and gynecological malignant tumors has not been observed, except a few publications that may be helpful in differentiating ovarian endometriosis from endometrioid tumors and in diagnostic value in endometrial stromal tumors [25,45-51]. Working with CD56 in our tumor groups positive staining was detected in OSC (40%), in TSC (37.5%), and in EEC (6.5%), but staining was not detected in ESC, PSC and PMM cases. When the values of CD56 expressions belonging to tumor groups were compared in pairs, the differences of OSC vs EEC and TSC vs EEC were significant (p < 0.05). However, divided into three groups according to histological type in terms of CD56 expression, differences between SC vs EC and SC vs MM were significant (p < 0.05), while no significant difference was detected between EC and MM (p > 0.05). In statistical analysis of the tumors divided into two groups including PMS and SMS in respect to CD56 expression, the difference between PMS and SMS were found as significant (p < 0.005). With these results, it can be concluded that CD56 may be a useful marker in the differential diagnosis of OSC with TSC and PMM.
Undoubtedly, molecular and genetic studies is necessary in determining the origin of the tumor. In this study, although IHC analysis lack sufficient sensitivity and specificity to determine the mutations, we searched the properties of malignant tumors that develop from peritoneal mesothelium and so far accepted to arise from different localization of Müllerian epithelium by using mesothelial, Müllerian, epithelial and mesenchymal markers as well as their relations with PMS and SMS. It seems possible that TPJ can take place around the fimbriated end of the fallopian tube or ovary, at the same time it seems possible that TPJ could be the junction between PMS and SMS. This junctional area, may have prepared the ground for Müllerian metaplasia as a result of injury occuring in each ovulation due to epithelial degeneration and regeneration processes that has developed by the ovarian and the surrounding area which is similar to formation of cervical squamous metaplasia. It seems that the occurrence of different tumors with the introduction of the different oncogenic pathways which is triggered by different genetic mechanisms might be possible. In our study, we found that IHC features in PMM were different than OSC, TSC and IHC features in ESC were different than OSC and TSC and we also found that epithelial markers were found to be dominant in the tumors except PMM. In particular, although PAX8, WT1 and CD56 were not immunoreactive in ESC, high immunoreactivity in OSC and TSC was considered as an indication which have different origins of the tumors as SMS with PMS. In conclusion TPJ may play an important role in the development of tuboovarian tumors as a junctional place of PMS and SMS. As the tumors of PMS and SMS the tumors arising from peritoneal mesothelium and Müllerian epithelium have different expression immunohistochemically but the finding in the study should be supported by molecular and genetic studies.
The present study was supported by Cumhuriyet University Scientific Research Projects (CUBAP) Project no T-501. We are grateful to Ersin Tuncer MD, Serkan Celikgün and Ziynet Cinar for providing us technical supports.
This study was presented as oral report at the 23rd National Pathology Congress Çeşme/İzmir, Turkey.
Fundamental ethical approval for the study was taken from Cumhuriyet University School of Medicine Scientific Research Evaluation Committee, with decision number of 2011/018 on the 13th of December, 2011.
The present study was supported by Cumhuriyet University Scientific Research Projects (CUBAP) Project no T-501. The authors declare no conflict of interest.