Sarcoma Kaposi is rare and most commonly affects the skin. Herein, we present a patient with ulcerative colitis, who developed intestinal Kaposi's sarcoma only six months after being diagnosed with ulcerative colitis. Therefore, we may conclude that sarcoma Kaposi was not due to immunosuppressive treatment, as its cutaneous form appeared only twenty days after having started azathioprine, mesalazine and corticosteroids enema. If there is any plausible link between ulcerative colitis and sarcoma Kaposi remains to be elucidated in further large-scale studies.
Sarcoma Kaposi, Visceral, Cutaneous, Ulcerative colitis
Sarcoma Kaposi is rare and most commonly affects the skin [1]. It has been divided into the following four forms: (i) Classical, (ii) AIDS-associated, (iii) Iatrogenic, and (iv) Endemic [2]. All forms have been documented to be related to HHV-8 infection [3-7]. Herein, we present a patient with ulcerative colitis, who developed intestinal Kaposi's sarcoma only six months after being diagnosed with ulcerative colitis.
A 72-year-old male patient presented to the hospital due to bloody diarrheas of two weeks duration. From his past medical history, he had been diagnosed with ulcerative colitis six months before now. Besides, he had diabetes mellitus that had been diagnosed two years before and had been a heavy smoker.
Six months before, the patient started to complain about diarrheas that eventually became bloody, were more than six per day and were accompanied by abdominal cramps. At that time, he underwent a colonoscopy, which revealed the presence of diffuse edema, intense redness, spontaneous hemorrhages and pseudo-polyps, which gave a cobblestone appearance, macroscopically. On histopathology, ulcerative colitis was present and as from his clinical and laboratory findings (≥ six bloody diarrheas, abdominal cramps, and elevated erythrocyte sedimentation rate > 30 mm/h), he was administered mesalazine 2 × 3 daily and corticosteroids enema as well as azathioprine 50 mg daily as maintenance therapy, according to treatment guidelines of severe forms of ulcerative colitis [8]. Notably, systemic corticosteroids were not administered to the patient due to the presence of diabetes mellitus. In addition, Clostridium difficile infection was ruled out on accounts of the absence of a positive assay for toxin A or B and on the absence of its presentation macroscopically and on histopathology, too. Twenty days after having started treatment for ulcerative colitis, a red to purple rash appeared on the right foot of the patient. A biopsy was performed, and the diagnosis of cutaneous sarcoma Kaposi was made. Azathioprine and mesalazine were discontinued and the patient received radiotherapy for the cutaneous sarcoma Kaposi. Six months later, the patient complained again of bloody diarrhea and a new colonoscopy was performed, which revealed the presence of tumor-like masses in the sigmoid and the rectum. Histopathology of these lesions was compatible with intestinal sarcoma Kaposi (Figure 1 and Figure 2). The patient was operated upon and afterwards he received liposomal doxorubicin for three cycles. Afterwards, he received interferon alpha-2b for three months. Another colonoscopy that was performed six months later was negative for sarcoma Kaposi, but showed the presence of ulcers of the intestinal mucosa again (Figure 3).
 Figure 1: H&E ×400: Sarcoma Kaposi-spindle cells with mild to moderate atypia arranged in vague fascicles and separated by slit-like vessels. View Figure 1
Figure 1: H&E ×400: Sarcoma Kaposi-spindle cells with mild to moderate atypia arranged in vague fascicles and separated by slit-like vessels. View Figure 1
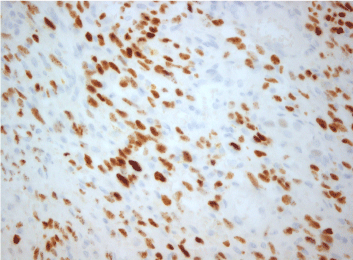 Figure 2: H&E ×400: Positive expression of HHV-8. View Figure 2
Figure 2: H&E ×400: Positive expression of HHV-8. View Figure 2
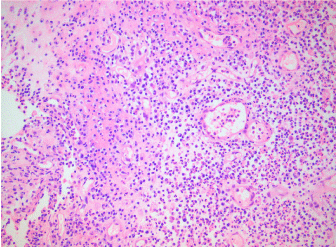 Figure 3: H&E ×20: Inflammatory full of vessels tissue from un ulcer of the intestinal mucosa. No findings of HHV-8 infection. View Figure 3
Figure 3: H&E ×20: Inflammatory full of vessels tissue from un ulcer of the intestinal mucosa. No findings of HHV-8 infection. View Figure 3
Ulcerative colitis together with Crohn's disease comprises chronic inflammatory bowel diseases, which cause inflammation and ulcers in the gastrointestinal system. Few case reports have reported an association between sarcoma Kaposi and ulcerative colitis [9-12]. The clinical manifestations of sarcoma Kaposi among patients with ulcerative colitis is quite variable. Most presented with bloody or watery diarrhea, abdominal pain and weight loss [6,13-16]. Complications like severe bleeding or toxic megacolon have rarely been reported. Most of these patients had refractory ulcerative colitis requiring long-term immunosuppressive therapy [6,14-16]. The majority of these patients developed cutaneous lesions before or after a diagnosis of sarcoma Kaposi was made [14].
To our knowledge, this is the first case of both intestinal and cutaneous sarcoma Kaposi in a patient with ulcerative colitis of only six months duration. Sarcoma Kaposi has been associated with ulcerative colitis in patients on long-term corticosteroids or azathioprine treatment [14-17]. Colorectal Kaposi's sarcoma, is exceedingly rare in human immunodeficiency virus-negative subjects and almost always reported in association with severe, refractory, inflammatory bowel disease on immunosuppression therapy [17]. On the contrary, our patient had ulcerative colitis and had been administered only azathioprine for a few months. Therefore, we may conclude that sarcoma Kaposi was not due to immunosuppressive treatment, as its cutaneous form appeared only twenty days after having started azathioprine, mesalazine and corticosteroids enema. If there is any plausible link between ulcerative colitis and sarcoma Kaposi remains to be elucidated in further large-scale studies.