Marburg virus disease (MVD) is a type of hemorrhagic fever caused by a genetically unique animal-borne RNA virus of the filovirus family-like Ebola virus. The African fruit bat is the known reservoir of this virus, and due to its animal-to-animal, animal-to-human, and human-to-human transmission patterns, it is capable of rapid spread. The history of previous MVD outbreaks shows that this can be highly fatal, and the fatality rate can reach up to 90%. Most MVD outbreaks have been in Africa and could trigger a disaster in an already crippled healthcare system, if not prevented properly. In this article, we aimed to discuss the origin and transmission of the Marburg virus along with the history of MVD, related challenges and efforts during the COVID-19 pandemic, and recommendations to prevent future epidemics considering the most recent outbreak in West Africa. Hopefully, through this manuscript, MVD can gain appropriate focus so that any unwanted epidemic due to this deadly virus can be avoided.
Public health, Guinea, West Africa, COVID-19, Ebola, Marburg virus
Marburg Virus (MARV), an RNA virus of the Filoviridae family, causes Marburg Virus Disease (MVD) [1]. Most of the viruses of this family are known to be notorious in humans and nonhuman primates for causing hemorrhagic diseases, especially the Marburg Virus or Ebola Virus genera [2]. Several species of bats act as host reservoirs for the filovirus family, and previous research studies indicate strong evidence of the Egyptian fruit bat "Rousettus aegyptiacus" being a reservoir for the MARV [3,4]. Marburg virus transmission occurs in several ways as illustrated in Figure 1.
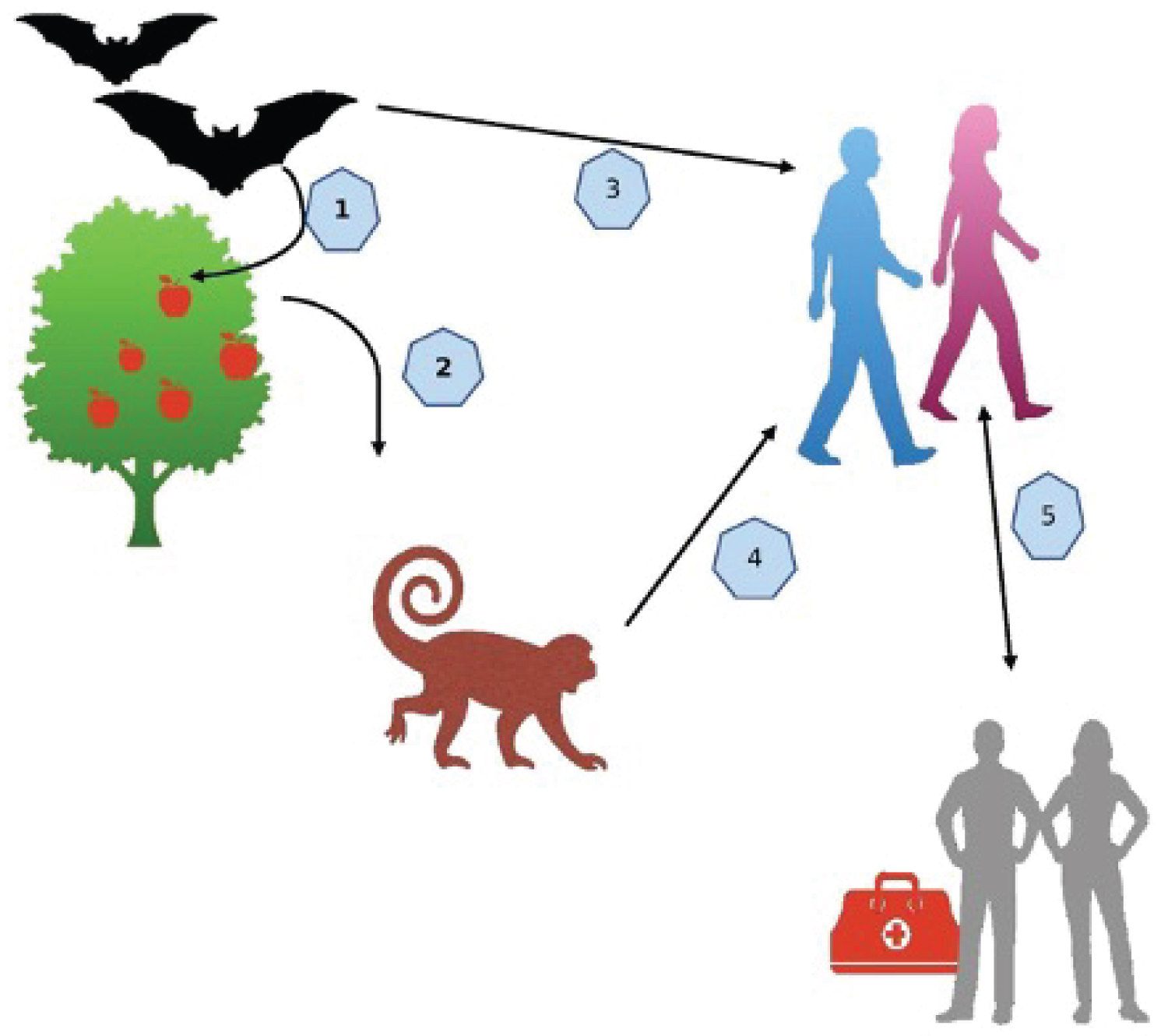 Figure 1: Transmission of the Marburg virus.
Figure 1: Transmission of the Marburg virus.
(1) & (2) Transmission of the virus to Cercopithecidae and Hominidae (monkeys) through the bite or partial chewing of fruits infected by bats' saliva; (3) Direct transmission to humans from the bats' shedding containing Marburg virus after encroachment into the caves and bat's habitat; (4) Transmission to humans through encounters with monkeys; (5) Human to Human transmission through direct contact.
View Figure 1
Direct transmission of the virus can occur either from bats to humans when humans encounter infected bat shedding after encroachment into caves and other habitats, from monkeys to humans by direct handling of infected monkey tissue, or from humans to humans by direct contact [5,6]. Direct human to human transmission is possible by contact through broken skin or mucous membranes in many ways:
a) Transmission via blood or body fluids including stool, urine, sweat, breast milk, amniotic fluids, etc.
b) Through sexual contact (oral, vaginal, anal sex) with a man (contaminated semen) who recently got recovered from a Marburg virus infection and has no active symptoms.
c) Transmission while handling objects like medical instruments, needles, syringes, and patient personal items that are soiled with bodily fluids from the infected patients or dead bodies before burial [7].
The pathogenesis of MVD illustrated in Figure 2 is similar to that of the Ebola virus and its clinical presentation is similar to tropical diseases like typhoid fever, malaria, or hemorrhagic fever of viral origin. The incubation period of MVD ranges from two to twenty-one days with typical symptoms including hyperthermia, shivering, headache, and muscle aches. Within a week of the onset of these features, a maculopapular rash can appear, more visibly on the torso. Pain in the abdomen, chest, and throat with giddiness, emesis, and loose stools may also be present. Disease severity increases suddenly from a rapidly progressing febrile illness, which later develops into multiorgan failure, exhaustion, and shock can increase causing signs of multiple organ damage [6,7].
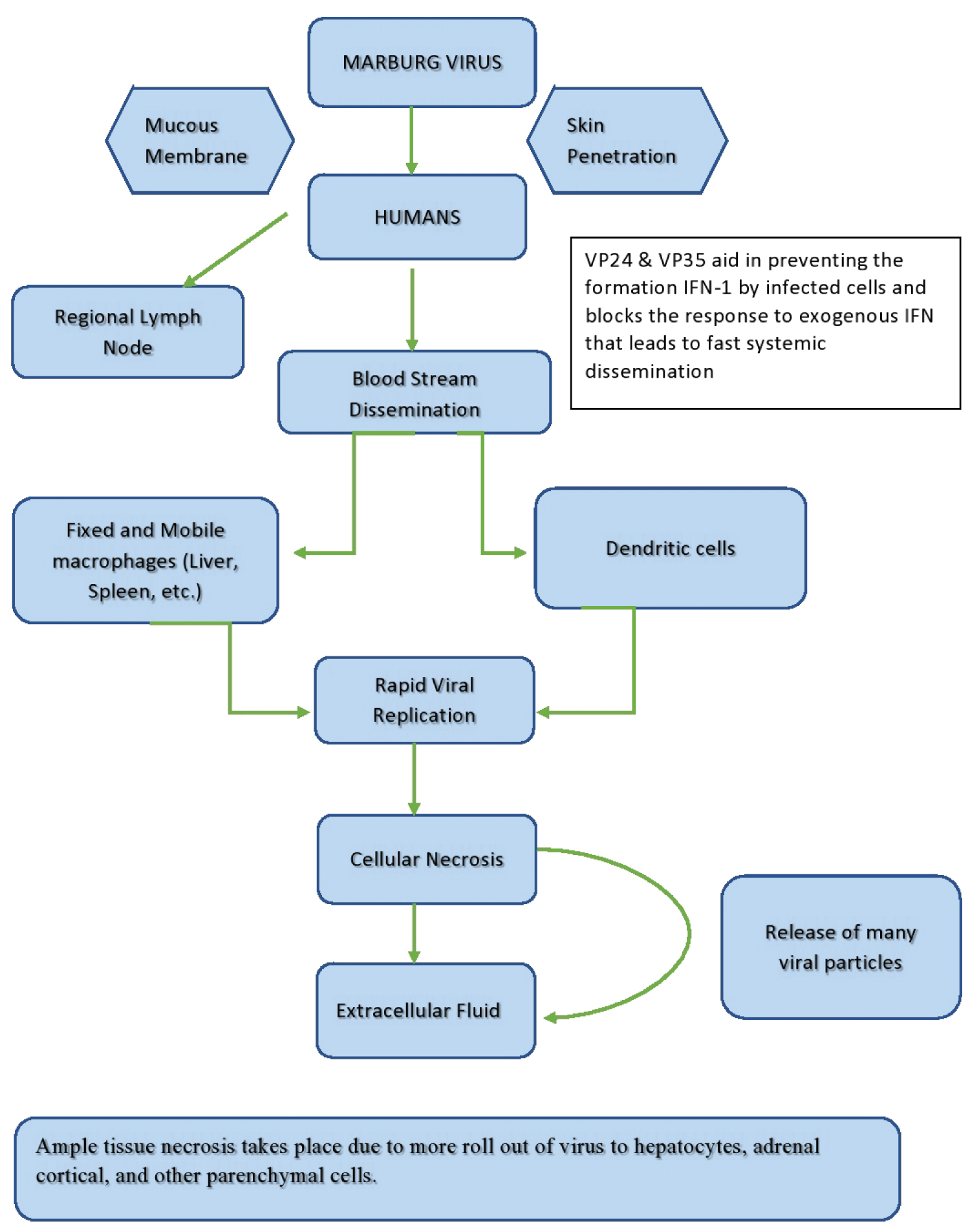 Figure 2: MVD outbreak cases and deaths since 1967.
View Figure 2
Figure 2: MVD outbreak cases and deaths since 1967.
View Figure 2
The diagnosis of MVD is detected through multiple modalities. The most favorable methods are Reverse-transcription polymerase chain reaction (RT-PCR) or detection of viral antigens by enzyme-linked immunosorbent assay (ELISA) in blood samples [7]. This differs from the Ebola virus, which had researchers undergoing field testing, whereas Marburg testing is confined within laboratory settings. Diagnosis can also be made at autopsy using blood, tissue, and other body fluids [7].
Currently, supportive measures are the only treatment for MVD. These supportive measures help to prevent disease progression to shock while the body upregulates its immune response. Although there is no approved treatment for this virus, monoclonal antibodies have been developed for Ebola, and scientists believe there is a possibility for their use in Marburg viral infections in extreme cases [7]. Five main proteins contribute to the infectivity of the Marburg virus. One protein, in particular, is called the VP40 which is a structural protein that has been the main source of the virus' virulence. This protein has evidence to support that it normally inhibits IFN signaling. The VP40 inhibition of signaling is a possible target for therapeutic techniques [8].
The World Health Organization (WHO) African region has the highest infectious illness burden and the most underdeveloped public health system [9]. As a result, a better knowledge of the factors that drive disease onset, prevention, and eradication is required in addition to establishing adequate surveillance programs, speedy diagnostic techniques, and major research efforts. This review aims to discuss the outbreaks of MVD with a focus on the most recent outbreak in West Africa, public health lessons that were learned from the most recent Ebola outbreak, and the ongoing COVID-19 pandemic in that region that can be applied to the management of future infectious disease outbreaks and how the Ebola virus outbreak in West Africa impacted efforts to eradicate the Marburg Virus. Additionally, the paper will highlight current efforts and public health responses relating to the MVD outbreak and recommendations that will help manage subsequent outbreaks and prevent future epidemics.
We performed a literature search on the databases PubMed, Google Scholar, Embase, and search engine Google from October 01, 2021, to November 30, 2021. The search strategy involved using relevant keywords in combination with the Boolean "AND". Relevant keywords used were "Marburg Virus", "Marburg Virus Disease", "West Africa AND Marburg Virus Disease", "COVID-19 AND West Africa" and "Ebola AND West Africa". Articles and news reports that highlighted the present and past outbreaks of the Marburg Virus, preventative and control measures against the Marburg Virus, the Ebola Virus, and COVID-19 were included.
Since the discovery of the Marburg virus in 1967 there have been 13 outbreaks with 10 occurring in Africa, including the recent 2021 Outbreak, outlined in Table 1 and Figure 3 [10].
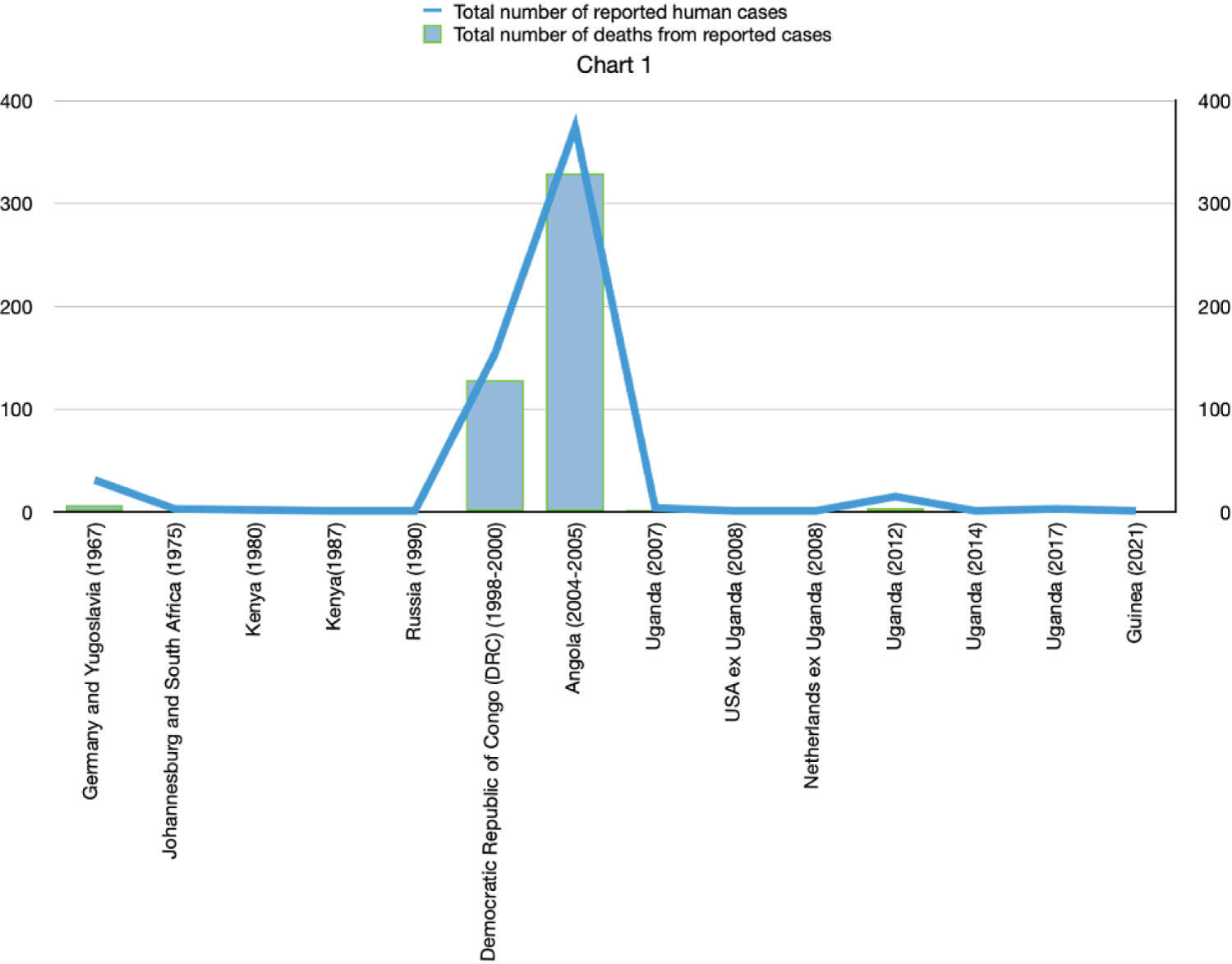 Figure 3: Supreselective angiography showing AVM node and embolized fistulous part of the AVM.
View Figure 3
Figure 3: Supreselective angiography showing AVM node and embolized fistulous part of the AVM.
View Figure 3
Table 1: MVD Outbreaks. View Table 1
The risk of exposure to the virus is increased in endemic areas, such as Sub-Saharan Africa, Germany, and Yugoslavia. These endemic areas have caves with Rousettus aegyptiacus, the suspected reservoir for the Marburg virus [11]. The largest outbreak in history occurred in 2004 in Angola, a nation in Southern Africa [12]. However, not enough effort was placed on determining the origin due to a lack of contact tracing and proper surveillance of the cases [13].
The second outbreak of MVD and the first ever recorded in the African region originated in 1975 in Rhodesia (now Zimbabwe) when visitors to the Sinoia Caves developed symptoms after 8-9 days. The cave was reported to have insectivorous bats; therefore, direct contact with bats or their discharge was a suspected source of infection [14-16].
On August 6, 2021, the WHO reported the first-ever known index case of MVD in Guinea [17]. Although MVD outbreaks have previously been reported in other parts of Africa such as Central Africa (Congo and Angola) and East Africa (Uganda), this is the first occurrence in Western Africa [16-19]. The patient began developing symptoms on July 25, 2021, and presented to the local health facility on August 01, 2021, with symptoms of fever, fatigue, headache, abdominal pain, and gingival hemorrhage. Malaria was suspected and the Malaria rapid diagnostic test turned out to be negative. After being given supportive therapy in the form of rehydration therapy, antibiotics, and symptomatic treatment the patient was discharged. The next day the patient died due to the severity of the symptoms. Further investigations were done by National health authorities and the WHO experts where multiple real-time polymerase chain reaction (PCR) tests were performed and showed the virus to be positive for the Marburg virus and negative for the Ebola virus. Contract tracing was adopted and about 172 out of 173 individuals were identified and followed up for 21 days along with 14 high-risk contacts. One high-risk individual was lost to follow up. After 21 days, no disease symptoms were found to develop in any of the individuals [17]. On September 16, 2021, the Ministry of Health of Guinea declared the end of the MVD outbreak which according to WHO recommendations was made after 42 days of safe burial of only confirmed MVD cases [19].
Two strains of the Marburg virus genus, MARV and Ravn, and the Ebola virus belong to the Filovirus family of RNA viruses [20]. Being the predominant class of viruses causing viral hemorrhagic fever, with case-specific mortality ranging from 24%-88% [21], the WHO has rated MARV as a Risk Factor 4 Pathogen, requiring Level 4 equivalent biosafety to curtail contamination [22].
The Egyptian Fruit bat (Rousettus aegyptiacus) is one of the most significant reservoirs for the virus in the African region, especially for miners and tourists exploring caves who are at increased risk of contracting the disease. The surge in clinical cases correlates to the breeding cycle of the bats in the region [10]. As with other hemorrhagic fever viruses, the Marburg virus has the capacity for human-to-human transmission via contact with bodily secretions to lacerated or broken skin [23]. Different body secretions have variable vector tendencies. One case is a woman becoming infected with the Marburg virus through her husband's semen after three months of infection. The WHO confirmed the finding since fluorescent antibodies test showed sperms were carrying the infected material [24]. Digital mapping of the African regions infected with zoonotic infection through computerized simulation models showed that 22 million were at risk from Ebola infection. In contrast, the Marburg virus is a potential threat to 105 million people [25]. It depicts the potential of another global pandemic, if not curtailed in a timely fashion.
Between 1967 to date, the Marburg virus has caused 13 outbreaks of variable scale, especially in sub-Saharan and eastern Africa, the area endemic to Ebola outbreaks, with a small number of cases in other regions [26]. A systemic analysis of the MVD outbreaks predicted that the major transmission of the Marburg virus was among close contacts in a later phase of infections, those caring for sick people, and those performing burial services for newly diseased patients, whereas superficial household contacts carry minimal risk of 1% [27]. There are also concerns regarding the potential to aerosolize and use this virus as a biological weapon [28].
As with the other hemorrhagic fever diseases, the initial presentation of MVD, is like malaria, typhoid, and the Ebola virus disease, making clinical differentiation difficult in the early phase of the disease, where only one-third of patients develop hemorrhagic symptoms, in the peak clinical course [20]. MARV tends to infect organs that are high in reticuloendothelial cells, especially the liver, spleen, brain, and kidney, followed by endothelial cells of lymph nodes and spleen [13]. Hemorrhagic symptoms are speculated to be either due to direct activation of the extrinsic coagulation pathway due to exposure to tissue factors or by an imbalance between the anticoagulant proteins due to liver necrosis [29]. Cerebral manifestations such as clouding of consciousness, aggression, and glial nodule encephalitis are also common symptoms of MVD [30].
The ongoing extended COVID-19 pandemic proved detrimental to African countries' already stressed healthcare system [31]. However, various African countries including Uganda, Rwanda, Nigeria, and South Africa, were the first countries to implement nationwide lockdowns to curb the COVID-19 pandemic [32]. Contrary to popular beliefs, African countries had recorded comparatively fewer COVID-19 cases than the western countries [33]. Among the various explanations for this are the early and strong political commitments to the robust implementation of public health measures, including lockdowns, contact tracing, and travel restrictions. Another hypothesis, yet unproven, is cross-immunity from various other endemic parasitic diseases and other circulating coronaviruses, the young age of the African population, and other environmental and genetic factors [34].
The extended COVID-19 pandemic raised concerns about the global availability of health resources, the resultant practice of social distancing, and struggles to ensure the safety of healthcare staff further declined the quality of health care [35]. Due to the pandemic, the focus of healthcare providers shifted to COVID-19, which left the other health needs less attended to and inclined local populations towards herbal remedies and self-medication, posing a significant threat to health standards. Neglect of needy patients by health care facilities was also observed, where chronic disease screening and management were suspended [36]. The COVID-19 pandemic provided a significant boost to the practice of telemedicine. African populations lagged in the development of telemedicine facilities due to a lack of infrastructure, electricity issues, scarce access to the internet, and ignorance of the method of operation of telemedicine [37,38].
The African countries developed effective contact tracing methods based on the statistics and the experience gained with the previous epidemics, to effectively control the COVID-19 spread [39]. Rwanda's strategy of using cellphone tower data and South Africa's use of the mobile application to augment contact tracing efforts could provide a long-term method of contact tracing in hemorrhagic fever diseases. However, past experiences can never compensate for the underdeveloped health system and scarce resources [40,41]. Unlike the Ebola epidemic in 2014, African countries rapidly reacted to ramp up COVID-19 diagnostic capacity from two to 43 countries in the earlier quarter of 2020 [42]. The use of GeneXpert platforms and HIV Molecular testing with COVID-19 cartridges helped decentralize testing facilities to reach remote populations [43,44]. The increasing use of biomechanical sensors in smart devices has been reviewed as a prospective method of performing mass screening in endemic areas [45].
Despite the disease being detected for more than 50 years, there is paucity in the development of treatment for MVD. To date, no FDA-approved vaccine or treatment exists [46]. Treatment is variably supportive, whereas antivirals and vaccines have shown mixed responses. Ribavirin, Galidesivir, Remdesivir, Favipiravir, Human convalescent serum, Interferon Beta, Pooled IgG from Equine antiserum, and desferal are some of the treatments which have shown promising results in preclinical and non-human primate trials. It has been seen that combining more than one treatment to extend the therapeutic window provides a better survival chance in MRV-infected patients [14,47]. Phosphorodiamidate Morpholino Oligomers (PMOs) with a positive charge, small interfering RNAs (siRNAs), and small viral-like proteins are being considered for advanced diseases, as they have been found to improve disease survival in animal models. A recombinant vesicular stomatitis virus-based vaccine that expresses MARV Glycoproteins (rVSV) has shown promising results if given within 48 hours of exposure, but there are concerns about the vaccine being an attenuated live virus [13].
To date, only three human trials have been conducted for MARV, whereas multiple non-human primate (NHP) trials are in different clinical phases. Marburg vaccines in phase 1 trials are cAd3, MVA-Bn-Filo, and MARV DNA, whereas only the MVA-BN-Filo has been listed for phase 2 trials [48]. Thirty-one percent of the subjects injected with attenuated MARV showed a positive antibody response, whereas 23% had positive antibodies response when injected with Ebola and Marburg virus combination. However, the trial was discontinued prematurely due to unexpected severe adverse effects. Another trial conducted with vaccines based upon wild-type Ebola and Marburg virus glycoproteins showed an 80% positive response at 12 weeks when the third dose was given during week eight. However, the response declines rapidly to 11% at 24 weeks, without any adverse effects [49].
More recently, structural proteins of the Marburg virus have been identified as potential therapeutic targets. The MVD genome contains five structural proteins, the most significant of which are viral proteins V35 and V40, which are crucial for the virus's infectivity [50]. V35 suppresses the immunological response to MVD and enhances the replication, synthesis, and assembly of viral RNA [51]. Meanwhile, V40 suppresses IFN signaling, impairing Janus kinase 1 activity (JAK1) [52].
While many antivirals have been tested, natural medicinal herbs can neutralize the effects of viral proteins with minimal side effects [53,54]. Because of the antiviral bioactive compounds that have been found, the usefulness of mushrooms in treating MVD has lately been investigated. Hasan, et al. [8] discovered Semicochliodinol B, a mushroom-derived inhibitor, to be one of the most efficient inhibitors of V35 and V40. While the drug's real effects may still require additional investigation, plant-based derivatives may have substantial potential in the management of MVD in the near future.
The world is plagued with emerging and re-emerging viral diseases, as elucidated by the COVID-19 pandemic. Public health personnel and clinicians should ensure that primary prevention and control measures are taken to contain the Marburg virus, which includes:
• Personal Protective Equipment such as gowns, gloves, masks, face shields, or goggles should be used to prevent contact with blood or body fluids, and adequate hand hygiene and sanitation measures are taken.
• Patients should be placed in a single room with a dedicated bathroom or commode.
• Physical contact should be avoided with infected individuals.
• The management and transfer of infected patients to a dedicated health facility should be conducted safely.
• Dead bodies infected with the virus should be safely disposed of.
• Wildlife should be handled safely with gloves and protective clothing.
• Aerosol-generating procedures should be undertaken with extreme caution, preferably in an airborne infection isolation room, with providers wearing appropriate PPE, including respiratory protection.
• Good food practices should be followed including adequate cooking of chicken and other animal products before eating [11,12].
Antiviral drugs and disease modifiers have shown positive results. Still, while efforts are taken to develop vaccines, efforts must be taken to identify the viral transmission cycles and educate the primary care workers to contain the disease [13]. While convalescent plasma therapy has been tested for the Marburg virus, management results have not been very optimistic besides the limited source of plasma available. Monoclonal antibodies have shown more promise [12].
Despite current treatment modalities and rapid advancements, community engagement, and participation it is imperative to create awareness and take measures to reduce the risk factors and motivate the community for self-prevention because no strategy fits all, and case-based real-time adjustments must be made to ensure further outbreaks. Technological advancements offer leverage in managing the disease outbreaks by real-time cases and datasets to not just guide the management but also complement the inadequate health workforce, especially in developing countries.
The emergence of the Marburg virus seems to be an overlapping challenge amidst COVID-19 and Ebola in endemic areas. Hemorrhagic fever such as MVD proved to be a lethal infection as seen in high case fatality rates in previous epidemics. Since MVD and Ebola can emerge in the same geographical regions, it could cripple African countries' already frail health systems. This can interrupt previously dedicated interventions for other diseases. Because of its highly contagious ability, it can heighten the current public health crisis. Prevailing travel restrictions and standard operating procedures of the ongoing pandemic can restrain its re-emergence. But, still, it possibly can escalate due to animal to animal and animal to human transmission. Management of the MVD is difficult due lack of a vaccine and the availability of only symptomatic treatment. Although few human trials are undergoing, further trials should be augmented. Even worse, vague symptoms and their resemblance with other infectious diseases can delay the diagnosis, thus increasing the chances of mortality. The lesson learned from COVID-19 should be enforced by an early anticipation of the possibility of a catastrophe. A clear-cut history of Marburg virus outbreaks in other countries and African nations shows there is a high risk of re-emergence in the future. The sudden emergence of calamitous outbreaks is difficult to manage due to a lack of prior preparedness. In addition, deficiency of specific treatment and similarity of symptoms with other diseases has confronted the current health systems. Unlike the common diseases, such outbreaks are less researched and studied, leading to the collapse of health systems. Moreover, such epidemics expose the healthcare status of the countries. Despite the better health systems of developed countries, they are still struggling with epidemics and lack prior surveillance systems.
For prevention and dealing with future MVD outbreaks, comprehensive research to combat looming threats must be conducted along with establishing complete surveillance systems. Emphasis on primary prevention at the community level would be the foremost way to control the upsurge.
All authors declare no conflicts of interest.
None Received.
JAL conceptualized the main idea and format for the study. JAL, MH, CP, SC, AS, SS, AM, PK and MS wrote the original manuscript. JAL and MS edited and improved the manuscript.
All authors revised and approved the final draft for submission.