Background: The COVID-19 pandemic has profoundly and adversely impacted various aspects of our societies from health systems, tourism, education, economic growth, social interactions and even individual life. In addition to the various non-pharmacological interventions put in place globally, a safe and efficacious vaccine was one of the most promising strategies to curtail the virus, save lives and quickly end the public health crisis. This study assessed the willingness to accept COVID-19 vaccine among undergraduate students in Southern Nigeria.
Methods: A descriptive cross-sectional study was conducted among five hundred and forty undergraduate students in Benin City, Edo state in Nigeria. Data was collected using self-administered structured questionnaires. Five hundred and forty respondents were selected using a multistage sampling technique with statistical significance set at p ˂ 0.050 and 95% Confidence Interval. Data was collected and analyzed using IBM SPSS version 25.0. Quantitative variables were expressed as frequencies, percentages, mean and standard deviation and the main outcome variable in relation to willingness to accept COVID-19 Vaccine was classified as willing and not willing respectively.
Results: A total of 540 undergraduate students participated in the study with a mean age ± SD (21.34 ± 2.73) years. More than half 276 (51.1%) of the respondents were not willing to take the COVID-19 vaccine. Faculty (OR = 2.359 CI = 1.131-4.918, p = 0.022.) and attitude towards COVID-19 Prevention (OR = 10.178; CI = 6.432-16.101. p = 0.001) of accept COVID-19 vaccine.
Conclusions: Less than half of the respondents were willing to take the COVID-19 vaccine. Health education interventions targeting undergraduate students should be intensified to help improve their knowledge and positive behavioural change towards acceptance of the COVID-19 vaccine.
COVID-19, COVID-19 vaccine, Hesitancy, Students, Undergraduate, Vaccine acceptance, Vaccine willingness, Benin city
COVID-19: Corona Virus Disease of 2019; SAGE: Strategic Advisory Group of Experts on Immunization; SPSS: Statistical Package for Social Sciences; WHO: World Health Organization
Vaccination is considered one of the most successful public health measures of the twentieth century in combating infectious diseases [1]. According to the World Health Organization, two to three million lives are saved each year through vaccination1. However, for a few decades, vaccination has been perceived as unsafe and unnecessary by a growing number of individuals in the world, especially in most western countries [1]. This concept referred to as vaccine hesitancy is defined by the World Health Organization's Strategic Advisory Group of Experts on Immunization (SAGE) Working Group as the individual's unwillingness to take the vaccine even when the vaccines are available [2].
The coronavirus disease of 2019 (COVID-19) pandemic caused by SARS-CoV-2 has spread across the world with millions infected and hundreds of thousands dead [3]. The pandemic has profoundly and adversely impacted various aspects of our societies from health systems, tourism, education, economic growth, social interactions and even individual life. In addition to public prevention efforts, developing a safe and efficacious vaccine could be one of most promising strategies to curtail the virus, save lives and end the public health crisis [4].
The success of COVID-19 vaccination program will largely depend on people's acceptance of the vaccine. Vaccination is an important preventative measure against the COVID-19 pandemic. The youths including the undergraduates make up a significant part of the world's population and they are often asymptomatic when infected thus serving as asymptomatic carriers, a veritable and significant means of transmission of the virus to the vulnerable groups (patients with immune-deficiency states, persons with co-morbidities such as Diabetes Mellitus, Hypertension, elderly persons, amongst others). The need to assess COVID-19 vaccination acceptance and uptake by youths is strategic in ensuring successful uptake among the target population in Nigeria. During the COVID-19 pandemic, people used multiple information resources to gain knowledge and health information about the disease, including television, radio, newspapers, social media, friends, co-workers, healthcare providers, scientists and governments [5]. Such information sources can shape peoples' acceptance or refusal of COVID-19 vaccines as some of these information sources could disseminate false and inaccurate information about vaccines' safety and efficacy which leads to lack of trust of the population especially the already hesitant and skeptical ones [6]. Intention to be vaccinated against an infectious disease is recognized as a significant challenge affecting the success of vaccination programs, this is influenced by vaccine scandals and series of reports about side effects of vaccination. This perception of the benefits and risks of vaccines plays a role in the development of vaccine hesitancy. Indeed, several studies show that individuals who perceive vaccines as less necessary and safe, more often reject scheduled vaccinations for their children and for themselves [7]. To implement vaccination and immunization programs effectively, it is essential to study the willingness to accept COVID-19 vaccines among undergraduates in order to identify factors that could result in vaccine hesitancy and proffer solutions. This study determined the willingness to accept COVID-19 vaccine among undergraduate Students in Southern Nigeria.
This study was carried out among undergraduate students attending two higher institutions of learning in Benin City, Edo State. Edo State is located in the South-South geopolitical zone of Nigeria, bounded by Kogi State to the north-east, Anambra State to the east, Delta State to the south-east and Ondo State to the west and the north-west. The state is inhabited largely by the Edo (Benin) people, who are linked to the historic kingdom of Benin [8].
A descriptive cross sectional study design was conducted involving a sample size of 540 undergraduate students, calculated using Cochran formula taking into consideration a prevalence of 80% from an earlier study, a 10% non-response rate and a design effect of 2 [9-11]. Self-administered questionnaire which was developed and standardized by the researchers was used in collecting data for the study. Pre-test was conducted among a comparable group of undergraduates at the Igbinedion University, Okada, Edo State. Data collected was assessed for completeness, coded, subsequently entered and analyzed using IBM SPSS version 21.0 statistical software.
Willingness to accept the vaccine was assessed with 7 questions using the Likert scale "Agree", "Disagree" and "Undecided". The questions used in scoring attitude were internally consistent with a Cronbach's alpha of 0.695. Respondents were expected to select one of three preferred options. A score of 1 given for each appropriate response. The minimum and maximum score attainable was 0 and 7 respectively. Respondents’ scores were computed into percentages. Respondents scoring at least 50% were willing to take the COVID-19 vaccine while the vaccine.
Ethical clearance and approval were applied for and obtained from the Ethical Committee of the University of Benin Teaching Hospital, with ethical protocol number of ADM/E 22/A/VOL. VIII/14831055. Institutional approval at the various educational Institution was also applied for and obtained before questionnaire administration. Anonymity of respondents was assured in the study, while health education was administered to respondents following questionnaire.
The mean age of the respondents studied was 21.34 ± 2.73 years while all respondents studied had heard of the term COVID-19. Among the respondents, the predominant ethnic group was Benin 133 (24.6%) and (Esan 123 (22.7%). Five hundred and twenty one (96.5%) and 533 (98.7%) were christians and single respectively. Four hundred and and fifty (83.3%) and 90 (16.7%) were from non-medical and medical faculty respectively. One hundred and ninety nine (36.9%) and 136 (25.6) (9.8%) and 16 (3%) were in 100 L, 400 L, 500 L and 600 L respectively. All respondents 540 (100%) studied have heard of the term COVID-19.
Table 1: Willingness to accept COVID-19 vaccine among respondents. View Table 1
Majority 394 (73.0%) of respondents indicated interest to take COVID-19 vaccine if given adequate information about the vaccine while less than half 168 (31.1%) were willing to take the vaccine if the vaccine is taken by many in the public. Furthermore, less than half 175 (32.4%) stated that their religious beliefs encourage them to take the vaccine, also 410 (75.9%) reported that their cultural beliefs does not discourage them from taking the vaccine. Almost half 227 (42.0%) of the respondent reported that support from family and friends will encourage them to get vaccinated. Finally, less than half 174 (32.2%) of the respondents indicated they would take the vaccine if they knew where to get it while more than a third 195 (36.1) of respondents are willing to take the vaccine if vaccine is available (Table 1).
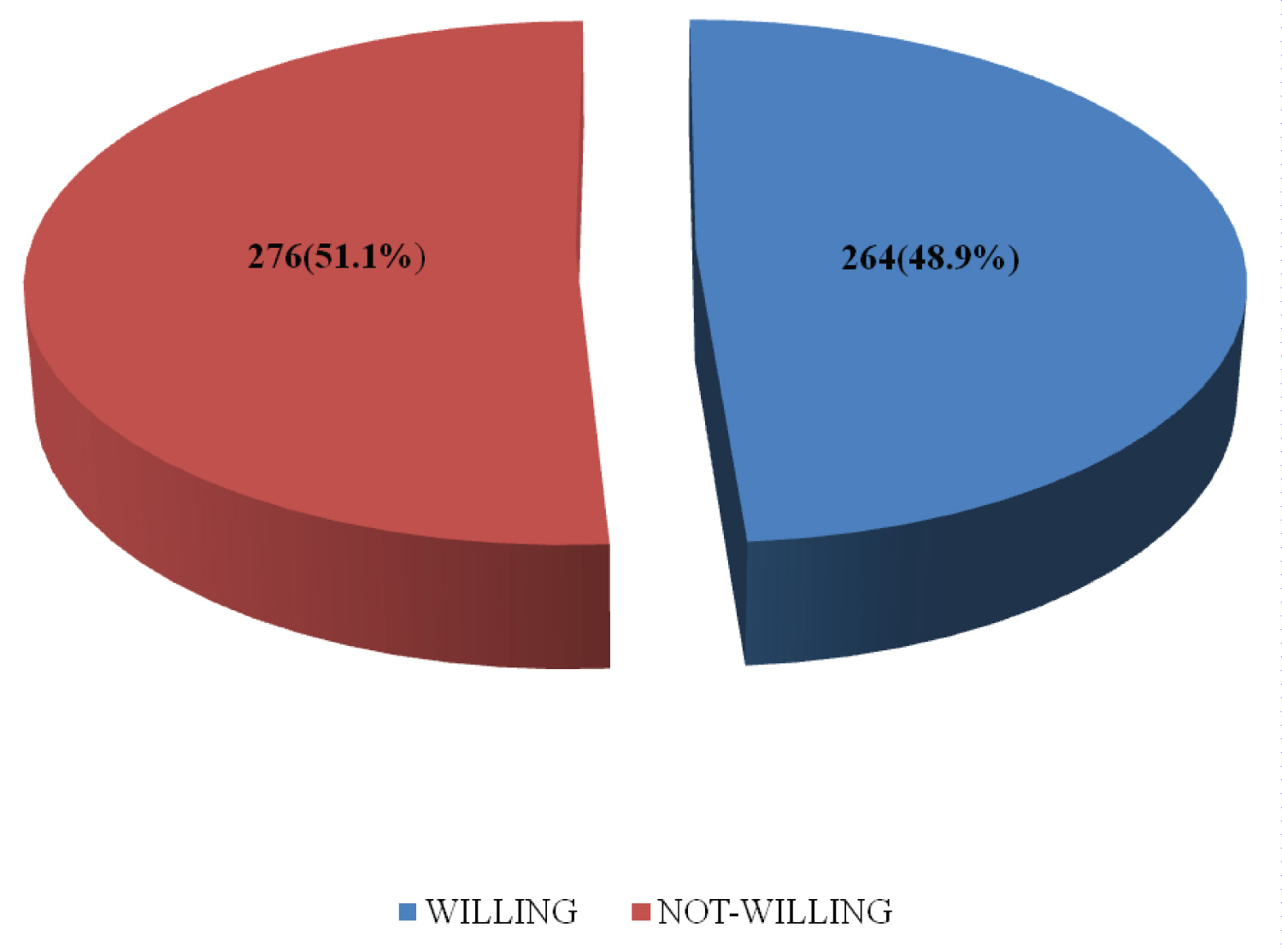 Figure 1: Overall willingness to accept COVID-19 vaccine among respondents.
View Figure 1
Figure 1: Overall willingness to accept COVID-19 vaccine among respondents.
View Figure 1
Less than half 264 (48.9%) of the respondents studied were willing to take the COVID-19 vaccine (Figure 1).
Table 2: Factors associated with willingness to take COVID-19 vaccine among respondents. View Table 2
Increasing age group of respondents was significantly associated with willingness to accept the COVID-19 vaccine (χ2 = 25.3931, p < 0.001). Gender of respondents was not a significant factor associated with willingness to take COVID-19 vaccine (χ2 = 0.4888, p = 0.541).
Willingness to take the vaccine was associated with respondents from medical faculties when compared with those from non-medical faculties and this association was statistically significant (χ2 = 15.421, p < 0.001). Increasing grade level of respondents was significantly associated with increasing willingness to take COVID-19 vaccine (χ2 = 19.442, p = 0.002).
Religion of respondents was not significantly associated with increasing willingness to take COVID-19 vaccine (χ2 = 5.487, p = 0.064). Respondents with positive attitude 178 (75.7%) towards COVID-19 prevention were significantly associated with willingness to accept COVID-19 vaccine (χ2 = 12.091, p < 0.001) (Table 2).
Table 3: Logistic regression model for determinants of willingness to accept COVID-19 vaccine among respondents. View Table 3
Respondents in the medical sciences were 2.359 (95% CI = 1.131-4.918, p = 0.022.) times more likely to be willing to be vaccinated compared with respondents in the (95% CI = 6.432-16.107; p = 0.001) more likely to be willing to get vaccinated compared to those with negative attitude towards COVID-19 prevention (Table 3).
Five hundred and forty undergraduate students participated in this study, of these, more than half were aged 20 - 24 years with a mean age (S.D) of 21.34 (2.73) years and more than half of the respondents were males. This is similar to a study done in Uganda among medical students in 2019 which showed a higher proportion of males [12] while a study carried out in Nigeria to assess the knowledge, COVID-19 vaccine among undergraduates [13] showed more than half of the respondents were between 18-25 years. About a quarter of the respondents belonged to the Benin and Esan ethnic groups which are the major ethnic groups in Edo State. Majority of the respondents were unmarried; this is similar to a study carried out in Northern Nigeria where majority of the undergraduates were unmarried [14]. This may be due to the fact that the respondents were all undergraduates and young persons. Majority of the respondents practiced Christianity; this is because Christianity is the major religion in Edo State. About one-tenth of the respondents were from the medical sciences while a majority were from the social sciences. Less than half of the participants of this study were willing to be vaccinated against COVID-19 while greater than 50% of study respondents were vaccine hesitant. Contrasting findings was reported in a study done in the United States where close to three-quarters of young adults (aged 18-24 years) were likely to be vaccinated [15]. Factors that may have influenced willingness to take the COVID-19 vaccine include the rapid pace of vaccine development, its fast-tracked approval, lack of trust in the health system and politicization of pandemic response efforts which may have influenced some public skepticism towards the safety of the vaccines [16-18]. Furthermore, misconceptions about COVID-19 such as; the vaccine being a mark of the beast, beliefs that the pandemic will not recur, or is a disease of the rich and that the chance of infection is small among young population, may have led students to have concerns about taking the vaccine [19,20]. A particular challenge for health authorities in managing the public's response to the pandemic is countering COVID-19 related misinformation and conspiracy beliefs common during public health crises which may influence people not to take preventive actions [21]. Majority of the respondents in this study indicated willingness to be vaccinated if adequate information was provided about the vaccine. This provides a huge opportunity for health information management and risk communication engagement to address key information gaps especially among the study population who are well exposed to information especially from social media with contents that may be verifiable and non-verifiable. Male respondents in this study were more willing than female respondents to take the vaccines, although not statistically significant, similar finding was reported in a survey done to assess receptivity towards COVID-19 vaccines [15]. This finding is in line with other studies that found high rates of women expressing concerns about the safety of vaccines and expressing a lack of trust in the quality and impartiality of information provided by healthcare professionals [22,23]. This gender variation concerning willingness to accept COVID-19 vaccines could be due to the myth that the vaccine can affect women's fertility [24]. Older respondents were more willingly to receive vaccine; this has been reported in several studies where receptiveness towards COVID-19 vaccine was associated with increasing age 15, [25,26]. The level of awareness among respondents were very high and can go a long way to show the importance and effectiveness of health education and awareness campaigns of health related events to enable individuals make the right decision on health promotion. Students in medical sciences could have a higher degree of understanding of the necessity, effectiveness, and safety of the COVID-19 vaccine compared to their non-medical counterparts. The reason for this is not far-fetched; students in medical sciences are more exposed to teaching and learning on vaccines etc to their counterparts in other courses and fields of study. What cannot be ignored is that students still have hesitations about vaccine safety and effectiveness hence there is need for proper health education which should not only target the general population but also specifically focus on special groups such as students, aged.
Less than have of respondents were willingness to accept COVID-19 vaccine designed to address anti-vaccination misconceptions and improve better acceptance of this cost-effective health intervention.
Authors declare that this manuscript is free of any form of competing interest whether financial or otherwise.
Authors sincerely acknowledge and appreciate all respondents that participated in this study and also appreciate the Management of Benson Idahosa University and University of Benin for permission to conduct this study.
University of Benin, Benin City, Edo State, Nigeria
Benson Idahosa University, Benin City, Edo State, Nigeria
Funding was by Authors.
We the authors certify that this work has not been published anywhere else and that all authors contributed significantly to this work.