Internal jugular vein (IJV) stenosis is being increasingly associated with certain neurological conditions, including benign intracranial hypertension, cerebrospinal fluid (CSF) disorders, multiple sclerosis and Alzheimer's disease. The role of surgery in IJV stenosis have typically been to manage the associated CSF disorders, or with IJV stents. We describe a case of a patient incidentally found to have bilateral possible IJV stenosis with dilated paraspinal collateral venous channels during pre-operative CT angiogram for a symptomatic craniocervical junction meningioma, and the associated operative considerations. We also review the literature on causes and clinical phenomena associated with IJV stenosis.
We report a 61-year-old right handed lady presented to her local Accident and Emergency Department with several week history of gradual heaviness affecting her left arm, on a background of four months of left-sided paraesthesia. She had no right-sided symptoms.
On further questioning, she also described more frequent coughing, with difficulty clearing her throat, a few weeks of dysphagia, and more difficulty in reaching high pitched sounds with singing. Her past medical history only included acute idiopathic thrombocytopenic purpura, complicated by pneumonia ten years previously. She is a keen horse-rider. On examination, she had a normal gait, with negative Romberg and Unterberger's tests. There was reduced sensation to light touch in her left hand. Her tongue was symmetrical, with mild fasciculations in the neutral position, and she had a slight uvular deviation to the right. Examination of lower cranial never function by flexible naso-endoscopy did not reveal any abnormality.
Computed tomography (CT) scan demonstrated a left sided mass at the level of the foramen magnum, measuring 23 × 16 × 22 mm, with a suggestion of brainstem compression. Magnetic resonance imaging (MRI) demonstrates a homogenously contrast enhancing intradural, extramedullary lesion, causing compression of the medulla and upper cervical spinal cord (Figure 1). Initial differential diagnoses included meningioma or nerve sheath tumour.
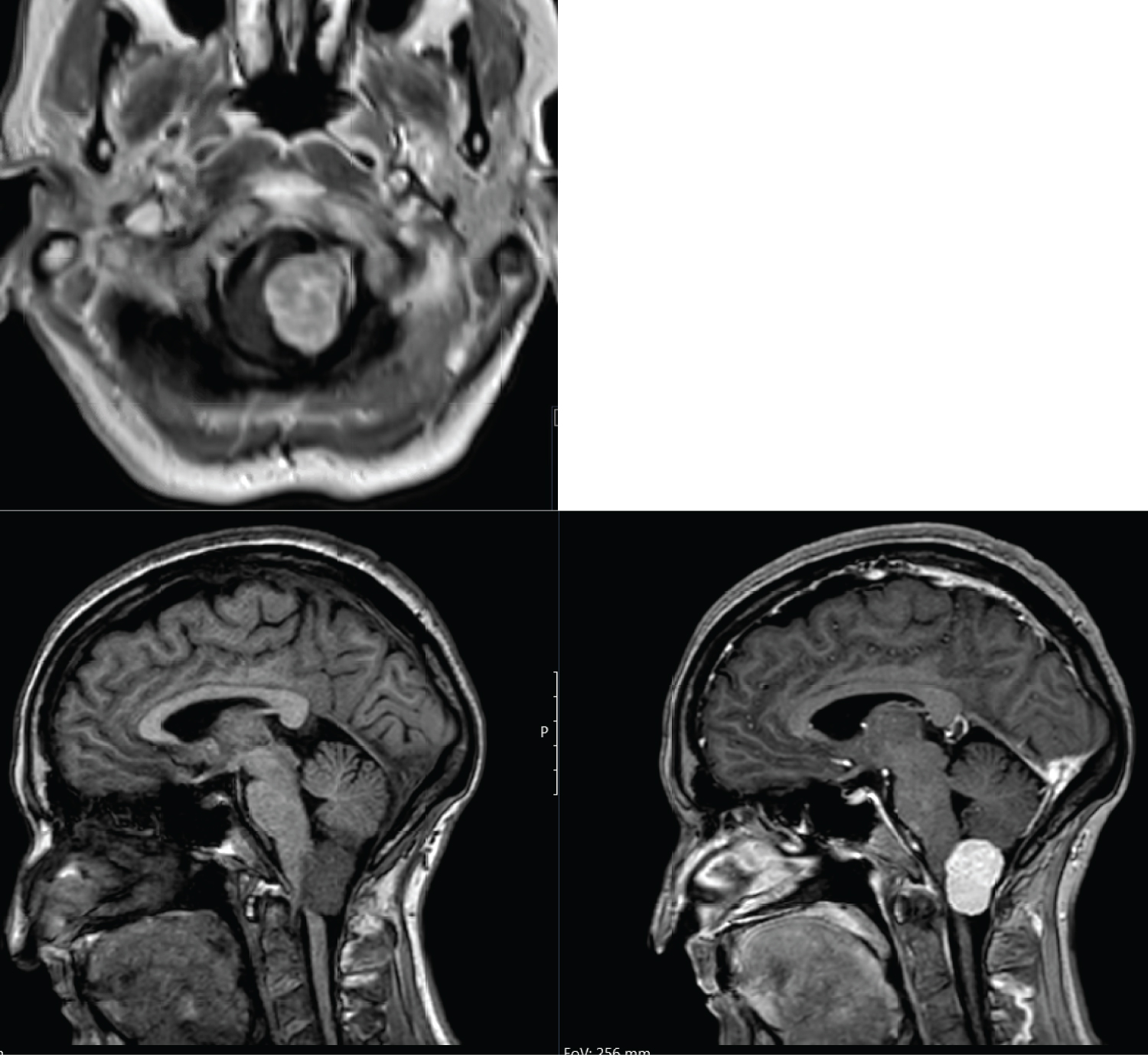 Figure 1: T1 MRI (non contrast scan left, contrasted right) demonstrating the contrasted, intradural, extramedullary lesion with medullary and upper cervical cord compression.
View Figure 1
Figure 1: T1 MRI (non contrast scan left, contrasted right) demonstrating the contrasted, intradural, extramedullary lesion with medullary and upper cervical cord compression.
View Figure 1
A brain and cervical spine CT angiogram (CTA) was performed as a part of our routine pre-operative planning. Review of this scan in our skull base MDT raised a possibility of bilateral jugular vein obstruction just below the skull base (Figure 2A) with enlarged venous system in the cervical paraspinal muscles (Figure 2B). There was also finding of bilateral elongated styloid processes of 4 cm, with associated bilateral internal jugular vein (IJV) stenosis. The narrowed calibre internal jugular veins continued throughout the neck. The stenosis of the IJVs resulted in a large substantial flow from the sigmoid sinuses into the deep and dilated venous channels in the paraspinal muscle. The concern at this stage was that the paraspinal venous channels were the primary intracranial venous outflow, with potential risks of venous hypertension with brain swelling, and venous infarction in event of any damage during surgical exposure for craniotomy for foramen magnum meningioma. A possible change in surgical approach was considered based on above findings, pending more information. Following discussion with vascular surgery service a doppler ultrasound of neck was performed, which reassuringly demonstrated patency and a reasonable blood flow through both IJVs. There was no evidence of underlying thrombosis (Figure 3). Although this was reassuring, the patient was counselled in detail about small risks of potential venous infarction, surgical access difficulties and incomplete resection.
 Figure 2: A) Internal jugular veins narrowing bilaterally at the junction between the styloid process and C1 lateral mass; B) Large, tortuous, engorged anastomotic venous plexus and collaterals to the posterior jugular vein and bilateral vertebral veins.
View Figure 2
Figure 2: A) Internal jugular veins narrowing bilaterally at the junction between the styloid process and C1 lateral mass; B) Large, tortuous, engorged anastomotic venous plexus and collaterals to the posterior jugular vein and bilateral vertebral veins.
View Figure 2
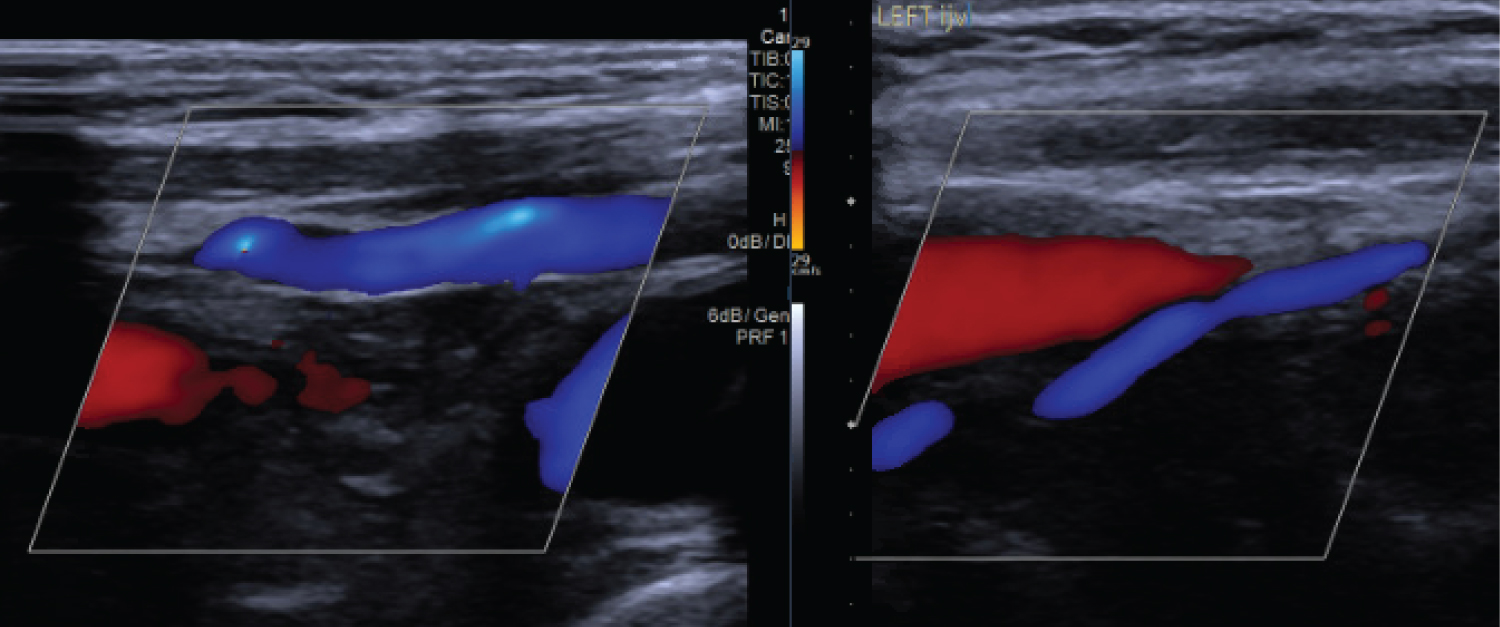 Figure 3: Right and Left Internal jugular vein Doppler ultrasound showing normal venous flow.
View Figure 3
Figure 3: Right and Left Internal jugular vein Doppler ultrasound showing normal venous flow.
View Figure 3
A midline hockey-stick incision curving to the left was used, with careful dissection in the midline raphe. There was no breach of the deep cervical dilated veins on the surgical exposure. A left suboccipital craniectomy was performed, with C1 hemi-laminectomy, and a part of left occipital condyle was drilled down to facilitate surgical access. After applying the retractors flow through deep veins were confirmed with intra-op ultrasonography. A hockey-stick dural incision was made. The tumour was firm, extra-axial, with a good arachnoid plane, and was debulked internally to minimise retraction on adjacent structure. The dural entry point of the left vertebral artery was identified, and seen to be separate from the dural base of the tumour. The tumour was then completely removed, and dural base coagulated, giving a Simpson grade 2 resection. Dura was closed with dural substitute reinforcement and sealant glue. Cervical fascia was closed in layers. Intra-operative neuromonitoring was used throughout the procedure, which showed no changes in MEPs, SSEPs, coMEPs of lower cranial nerves, brainstem auditory evoked potentials (BAEPs), laryngeal adductor reflex (LAR). Spinal accessory and hypoglossal nerves were visualised and protected throughout surgery.
The patient was discharged home on post-operative day 5 with no neurological deficits. Immediate post-operative MRI showed no residual tumour (Figure 4), and histology was that of a WHO Grade 1 meningothelial meningioma. Post-operative vascular imaging showed no change in the venous structures in paraspinal muscles. At six month follow-up, her left upper limb symptoms had resolved, and she has made a very good neurological recovery. She had problems with a right-thigh pseudoaneurysm from the central venous catheter during surgery, which had also resolved with conservative management. She still had no symptoms concerning for IJV stenosis.
 Figure 4: Post operative MRI showing no residual tumour.
View Figure 4
Figure 4: Post operative MRI showing no residual tumour.
View Figure 4
Internal jugular veins are the main intracerebral venous outflow channels, and have valves to prevent jugular reflux and raised intracranial pressure. Collateral vessels exist between both of the internal jugular veins to regulate venous outflow, and anastomosing vessels also exist with extracranial veins including the anterior condylar confluence. Causes of internal jugular venous stenosis include intraluminal anomalies, aetiologies of which include membranes, webs, and focal thrombi. Extraluminal causes include anatomical variations causing direct compression of the IJV along its course, typically from elongated styloid processes, enlarged C1 transverse process, thyroid goitres, mediastinal masses, or adjacent enlarged arteries. The most commonly stenosed region is at the upper jugular J3 segment [1]. Little is published in the literature on the true incidence of IJV stenosis, however they have recently been implicated in a number of neurological conditions. They are well known to be associated with idiopathic intracranial hypertension, and disrupt CSF dynamics. A recent review article also suggests a possible association between IJV stenosis and conditions such as multiple stenosis and Alzheimer's disease. Typical associated symptoms include headache, tinnitus, visual disturbances, and also intracranial hypertension or cerebral haemorrhage.
One study attempted to quantify the radiological incidence of IJV stenosis in 108 patients who had CT neck angiograms as investigations for traumatic brain injury, atherosclerotic disease or neck dissections [2]. In this study of 108 patients, incidence of IJV stenosis from direct external compression was up to 33%. 16.7% had severe dominant IJV stenosis (ie. > 80%), of which approximately 55% were associated with extracranial condylar collateral vessels. The most common causes of IJV stenosis was elongated styloid process, and enlarged digastric muscles.
The patient described in our case report did have bilaterally elongated styloid processes of 4 cm and there was a significant narrowing of the IJV calibre bilaterally in between the styloid process and C1 lateral masses. The reduced calibre of the IJVs in the neck is likely to be due to the stenosis seen more cranially in the neck. Elongated styloid processes exist in approximately 4% of the population, and can have a myriad of clinical manifestations. The most commonly known eponym for symptomatic elongated styloid process is "Eagle Syndrome", which describes pain and dysphagia, typically following a tonsillectomy due to local scar tissue around the elongated styloid process. Other symptoms can manifest through compression of the internal carotid artery, causing TIA symptoms. A more recent description of "Eagle Jugular Syndrome" has been described by Zamboni, et al. [3], whereby the internal jugular vein is compressed by an elongated styloid process against the C1 transverse process. Symptoms for Eagle Jugular syndrome in this paper also included classical pain and dysphagia, however additional clinical manifestations described include intracranial hypertension from venous congestion, and cerebral haemorrhage. There was no description of whether the patients in Zamboni's case series had engorged extracranial venous collaterals. On further retrospective questioning, the patient in our case report does not have any clinical symptoms of Eagle Syndrome and most importantly the doppler scan confirmed no major obstruction of IJVs on both sides [4].
The surgical relevance of IJV stenosis pertinent to this case report is the presence of enlarged venous collaterals within the cervical paraspinal muscles, which were at risk of compromise in a posterior cervical approach. This was only picked up incidentally during a pre-operative CT neck angiogram. The true incidence of intracerebral venous outflow obstruction is still unknown, and is most likely underdiagnosed due to the associated non-specific clinical symptoms. Based upon Jayaraman's paper, incidence of incidental dilated paraspinal venous collaterals secondary to IJV stenosis can be up to 8%. Whilst doppler ultrasound excluded any intraluminal thrombi as the cause for our patient's IJV stenosis, and confirmed presence of blood flow, it does not qualify the percentage of intracerebral venous outflow through the IJV, and therefore how dependent the patient is on the collateral venous drainage. The exact pathophysiology at present is still unclear, and there may be a complex underlying process in this patient's IJV stenosis. Sceratti's review looking at symptomatic stylogenic-cervical IJV stenosis, found that only 1/3 of patients had elongated styloid processes, and stenosis is most likely a combination of both extraluminal and intraluminal factors.
Given the relatively high incidence of IJV stenosis and collateral vessels, and the increasing number of pathologies associated with IJV stenosis, damaging collateral venous drainage in a posterior cervical operative approach and potentially precipitating other associated neurological conditions should be considered during operative planning in patients with anatomical variants or risk factors.