Vaginal leiomyomas are rare benign solid tumors of the vagina with only about 300 reported cases. Here we describe a 24-year-old sexually inactive patient presented with a vaginal bleeding. On ultrasonography, a 5-centimeter vaginal mass was diagnosis in the anterior vaginal wall under urethra. Preoperative MRI showed a well-circumscribed vaginal mass. After transvaginal surgical enucleation, histological examination confirms diagnosis of the vaginal leiomyoma. The peculiarities of the case we report are manifold. Indeed, vaginal leiomyoma is rare. Our patient was only 21-years-old. The vaginal surgery of this form of leiomyoma causes hymeneal damage and compromises the patient's virginity, which is not always accepted in our conservative society.
Benign or malignant neoplasms of the vagina are rare including papilloma, hemangioma, mucus polyp, and rarely leiomyoma. Vaginal leiomyoma is usually located in the anterior wall and rarely the lateral wall or vulvar region. Most vaginal leiomyoma are asymptomatic until a significant size is reached. Symptoms and signs may include a vaginal discharge or bleeding, dyspareunia, or urinary retention. Most of these lesions can be detected during routine examination of an asymptomatic patient, but the challenge is to diagnose case of vaginal leiomyoma in virgin girl by sonography or MRI. Only between, 250 and 300 cases have been reported in the world literature [1,2]. These lesions are benign smooth muscle neoplasms, usually solitary and in many cases asymptomatic. Histologically, it seems to look like leiomyoma of other origins.
A 24-year-old unmarried sexually inactive girl presented with unexplains vaginal bleeding for past 18 months. In her past medical history, she had undergone an abdominal myomectomy 2 years previously.
Pelvic sonography showed 5 × 5 cm a tissue mass under urethra (Figure 1). In view of these findings, we have discussed the following diagnoses; a vaginal fibroma, a leiomyoma delivered by the cervix, a polyp delivered by the cervix and a tumor of urethral localization.
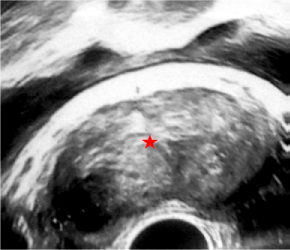 Figure 1: Percutaneous pelvic sonography: Suburethral tumor of 5 cm with homogeneous hypoechoic aspect (star). View Figure 1
Figure 1: Percutaneous pelvic sonography: Suburethral tumor of 5 cm with homogeneous hypoechoic aspect (star). View Figure 1
Magnetic resonance imaging revealed a tissue vaginal mass obstruent all vaginal cavities. The mass was in the anterior wall of the vagina and measured 5.1 × 4 × 50 cm with ovoid shape. The signal was iso-intense to muscle on T1- with intermediate signal intensity in the anterior vaginal wall distorting the vaginal canal on T2-weighted images, and enhancement is weak and delayed compared to the myometrium (Figure 2). Both urethroscopy and cystoscopy were normal. A vaginoscopy showed a large tumor in the anterior vaginal at the level between 10 o'clock and 2 o'clock position.
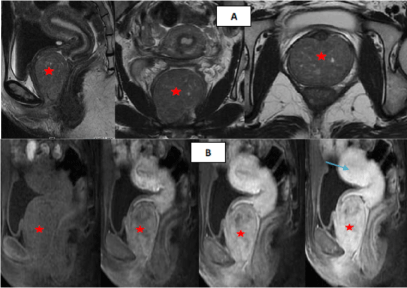 Figure 2: MRI appearance of vagial leiomyoma. A) Sagittal, coronal and axial T2-weighted MR Images: A well-defined solid mass with intermediate signal intensity in the anterior vaginal wall distorting the vaginal canal; Urinary bladder and urethra are displaced; B) Sagittal dynamic post-contrast T1-weighted MR images: The mass arises from the anterior vaginal wall (star) (note the bright enhancement of vaginal mucosa beyond the mass), the enhancement is weak and delayed compared to the myometrium (arrow). View Figure 2
Figure 2: MRI appearance of vagial leiomyoma. A) Sagittal, coronal and axial T2-weighted MR Images: A well-defined solid mass with intermediate signal intensity in the anterior vaginal wall distorting the vaginal canal; Urinary bladder and urethra are displaced; B) Sagittal dynamic post-contrast T1-weighted MR images: The mass arises from the anterior vaginal wall (star) (note the bright enhancement of vaginal mucosa beyond the mass), the enhancement is weak and delayed compared to the myometrium (arrow). View Figure 2
We opted for transvaginal route, but before surgery, we have clearly explained to patient the possible hymen lesion and we had consent from both patient and her parents.
The tumor was surgical removed by vaginal route with longitudinal incision and it was easily clivated. Postoperatively, the patient presented no complications in particular there was no hemorrhage or urine's retention or urinary tract infection.
Histopathological examination confirmed diagnosis. Gross examination revealed 2 masses weighing 50 grammes (Figure 3). After a two-year follow-up there was no recurrence of the leiomyoma.
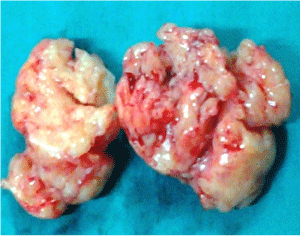 Figure 3: Macroscopic view of vaginal leiomyoma; whitish solid tumor. View Figure 3
Figure 3: Macroscopic view of vaginal leiomyoma; whitish solid tumor. View Figure 3
Leiomyoma in female genital tract are common in uterus followed by the round ligament, utero-sacral ligament, ovary, inguinal canal and very rarely in vagina. Vaginal leiomyoma is a rare benign tumor and they are only 300 reported cases [1,2].
They are commonly seen between 35 to 50 years [1-3]. However, in our case the patient was younger. Most of these lesions are small and they grow slowly, so they are generally asymptomatic. They can also regress spontaneously after menopause. However, Nidahnee reported a vaginal leiomyoma in postmenopausal hysterectomised women due, probably to hormone replacement therapy [3]. When leiomyomas are upper 5 cm in diameter, compressive symptoms appear. Larger tumors may cause pain and dyspareunia. There may be urinary tract symptoms including urinary bladder outlet obstruction, frequency, urgency, dysuria, post-voiding residue and urinary retention [2,4]. Indeed, vaginal leiomyoma has been termed "the female prostate" [5].
The tumors may be found in any location within the vagina, but they are most commonly located in the anterior wall and they are least commonly found in the lateral vaginal walls. In 2002, Shimada, et al. reported the first case of leiomyoma originating on the posterior vaginal wall which was associated with lumbar pain due to compression of the pelvic ligaments and lumbar venous plexus [6].
A pelvic examination can demonstrate a non-tender vaginal mass of a cystic, semi cystic, or solid consistency. But in unmarried patient as is the case of our patient with lack of physical exam, MRI, urethroscopy and cystoscopy can be helpful for diagnosis [4,7]. Paraurethral and vaginal wall leiomyomas can be identified before surgery based on their clinical and MRI characteristics. Indeed, leiomyomas are typically rounded, well-circumscribed masses of low T1-signal intensity with homogeneous enhancement after gadolinium administration [6-8]. T2-weighted images typically show masses with low to intermediate signal intensity, which is typical of smooth muscle tumors located elsewhere in the body. The diagnosis of vaginal leiomyoma can be made preoperatively but the best way to confirm diagnosis is by performing a histological examination.
Generally, the tumor is covered by intact and normal vaginal mucosa. However, ulceration of the overlying mucosa has been noted in a number of cases, and there is subsequent necrosis or purulent discharge and bleeding. Malignant degenerescence must be suspected if lesion reaches 10 cm in size [8].
Vaginal leiomyomas are estrogen-dependent tumors, and their growth is mediated by ovarian steroid hormones. Prolonged hypoestrogenism during post-menopause induce reduction of the leiomyomas size. However, some vaginal leiomyoma can be symptomatic in post-menopausal patient [3]. Similarly, leiomyomas can grow rapidly during pregnancy and lactation period [9,10].
Surgical enucleation is the treatment of choice, via a vaginal approach [8,9]. But, sometimes the size of the tumor necessitates an abdominoperineal approach and hysterectomy for better surgical access [10].