A case of large bilateral cystic ovarian masses is reported. Initial imaging, including ultrasound (US) and computed tomography (CT), showed a large right ovarian cystic tumor, a smaller multicystic left ovarian tumor and multiple solid peritoneal implants suspicious for metastases. Due to a history of remote post-traumatic splenectomy, the presence of bilateral benign ovarian cystic tumors in combination with peritoneal splenosis was considered. Magnetic resonance imaging (MRI) followed by total abdominal hysterectomy, bilateral salpingo-oophorectomy and omentectomy were performed. The final histological diagnosis of the peritoneal implants was splenic tissue consistent with splenosis and the ovarian tumors were ovarian serous cystadenofibromas.
Ovarian adenoma, Ovarian adenocarcinoma, Cystadenofibroma, Borderline malignancy, Splenosis, Peritoneal implants, Magnetic resonance imaging
The management of patients with benign versus malignant ovarian lesions differs significantly. An accurate preoperative working diagnosis, based in part on imaging studies, is mandatory to allow for proper surgical planning. Subsequently, unnecessary procedures may be prevented and patient morbidity decreased. A malignant ovarian lesion is radiologically suspected based on certain characteristics, including: large size, presence of thick walls and septae, solid components and signs of internal hemorrhage or necrosis [1]. Furthermore, identification of ascites and secondary peritoneal spread strongly support malignancy.
We describe a case of bilateral large ovarian masses accompanied by peritoneal soft tissue implants. Imaging studies revealed predominantly cystic lesions in the ovaries with minimal solid components, lack of ascites and hypervascular enhancement of multiple small peritoneal masses. Given the prior history of splenectomy, suspicion for metastatic ovarian cancer was low, and the suggestion of peritoneal splenosis and bilateral benign ovarian cystic tumors was raised. Intraoperative findings supported this diagnosis and consequently a less radical surgery was performed.
A 58-year-old woman was referred to our institution for pelvic pain and abdominal distention.
Her past medical history was remarkable for splenectomy performed following abdominal trauma in her youth, as well as an explorative laparotomy for chronic pelvic pain and infertility about 30-years-ago. Ovarian cyst aspiration performed at that time contained hemosiderin and erythrocytes but no tumor cells.
She was a smoker but otherwise healthy. The patient complained of worsening pelvic pain and abdominal distension. Laboratory results were normal apart of elevated CA-125 to a level of 331 U/ml.
Abdominal US (Figure 1) identified a 23 cm cystic mass in the central abdomen, most probably of right ovarian origin. The lesion contained cystic material with internal echoes; no solid component was identified (Figure 1a). In addition, a multicystic 9 cm mass was demonstrated posterior to the bladder, most probably of left ovarian origin. This second mass had thick septations and various fluid echogenicities (Figure 1b).
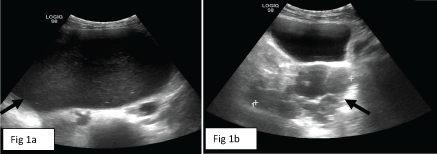 Figure 1: Large abdominal cyst with internal echoes at level of mid abdomen (arrow in a) and multicystic left ovarian lesion in the pelvis (arrow in b) on abdominal US examination. View Figure 1
Figure 1: Large abdominal cyst with internal echoes at level of mid abdomen (arrow in a) and multicystic left ovarian lesion in the pelvis (arrow in b) on abdominal US examination. View Figure 1
A contrast-enhanced abdominal CT was performed for further investigation of the bilateral ovarian masses. The CT exam demonstrated thin septations and a focal mural thickness in the larger, right ovarian mass. The left multicystic lesion showed minimal mural enhancement with no nodular component. The masses were free of calcifications, and no ascites or lymphadenopathy were seen. Multiple round and oval solid lesions were identified in the left abdomen and pelvis, the largest with a diameter of 3 cm, showing intense homogenous enhancement (Figure 2). No spleen was found in the left upper quadrant, and there were surgical clips in the splenic bed consistent with prior splenectomy.
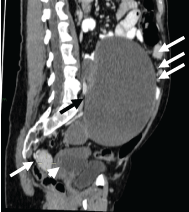 Figure 2: Contrast-enhanced CT image (sagittal reconstruction) demonstrates multiple, small homogeneously and strongly enhancing solid peritoneal masses (white arrows) of different size in addition to the large right abdominal cyst (black arrow) and smaller multicystic left pelvic mass (arrowhead). View Figure 2
Figure 2: Contrast-enhanced CT image (sagittal reconstruction) demonstrates multiple, small homogeneously and strongly enhancing solid peritoneal masses (white arrows) of different size in addition to the large right abdominal cyst (black arrow) and smaller multicystic left pelvic mass (arrowhead). View Figure 2
Based on prior splenectomy and the hypervascularity of the multiple peritoneal lesions, splenosis was suggested. MR imaging was obtained to further investigate the multiple peritoneal deposits as well as characterize the ovarian masses.
On MRI, the bilateral ovarian cystic masses had thick walls which were hypointense on T2 (Figure 3) and demonstrated minimal enhancement after gadolinium injection, consistent with a fibrous component, being more prominent in the right-sided lesion. The solid peritoneal lesions demonstrated rapid hypervascular enhancement, similar to normal splenic tissue (Figure 4).
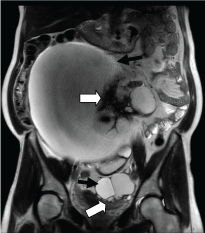 Figure 3: T2 coronal MRI image showed predominantly cystic, bilateral ovarian masses (black arrows). There were hypointense solid components (thick white arrows) consistent with papillary projections or fibrous tissue, more prominent in the larger right mass. View Figure 3
Figure 3: T2 coronal MRI image showed predominantly cystic, bilateral ovarian masses (black arrows). There were hypointense solid components (thick white arrows) consistent with papillary projections or fibrous tissue, more prominent in the larger right mass. View Figure 3
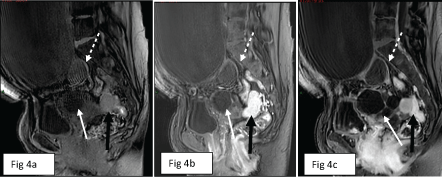 Figure 4: a,b,c) Sagittal T1 images of MRI performed before (a) and after gadolinium injection in arterial phase (b) and after several minutes (c) showed that the solid peritoneal lesions were initially slightly hypointense compared to the soft tissue, underwent rapid intense contrast enhancement and retained homogeneous enhancement in the late phase (black arrow in a, b and c). Of note, minimal mural enhancement of right (dashed white arrow in a, b and c) and left (white arrow in a, b and c) ovarian cystic masses. View Figure 4
Figure 4: a,b,c) Sagittal T1 images of MRI performed before (a) and after gadolinium injection in arterial phase (b) and after several minutes (c) showed that the solid peritoneal lesions were initially slightly hypointense compared to the soft tissue, underwent rapid intense contrast enhancement and retained homogeneous enhancement in the late phase (black arrow in a, b and c). Of note, minimal mural enhancement of right (dashed white arrow in a, b and c) and left (white arrow in a, b and c) ovarian cystic masses. View Figure 4
Based on the MR imaging, the bilateral ovarian lesions were considered to be non-malignant, such as cystadenomas or cystadenofibromas, possibly with some borderline characteristics. Peritoneal splenosis was strongly suggested.
An explorative laparotomy, with total abdominal hysterectomy, bilateral salpingo-oophorectomy and omental biopsy were performed. Intraoperative histology reported the peritoneal implants as splenic tissue consistent with splenosis (Figure 5) and the ovarian cysts as ovarian serous cystadenofibroma with small foci suspicious for borderline tumor. Hence, omentectomy was completed. The final pathology report confirmed ovarian serous cystadenofibromas, most compatible with benign features. The patient was discharged uneventfully on the 3rd postoperative day.
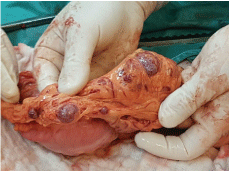 Figure 5: The surgical specimen of multiple omental lesions, which resembled splenic tissue on macroscopic examination. View Figure 5
Figure 5: The surgical specimen of multiple omental lesions, which resembled splenic tissue on macroscopic examination. View Figure 5
The management of patients with ovarian tumors differs significantly depending on whether the disease is benign or malignant. An accurate preoperative working diagnosis, based on the patient's history, clinical and laboratory findings, and imaging studies, is mandatory to allow proper surgical planning. Amongst imaging modalities US is usually the first, and commonly the only, diagnostic tool used for treatment planning and follow up of ovarian masses. In recent years however, the use of additional imaging modalities such as CT and MRI has become increasingly popular.
In this case, after identification of large cystic masses on ultrasound, a contrast-enhanced CT was obtained in order to determine whether the cystic masses were ovarian in origin and whether the lesions were likely benign or malignant. This was followed by MRI of the pelvis for further characterization of the ovarian lesions and peritoneal disease.
Cystadenomas are common and account for approximately 25% of benign ovarian neoplasm, being bilateral in up to 25% of cases. Features suspicious for malignancy in ovarian cysts include wall irregularity, thick septations (> 3 mm), papillary projections or solid components and size greater than 9 cm [2]. Similar to our case, the presence of only some of these features may suggest borderline lesions [3].
Ovarian cystadenofibromas contain various amounts of fibrous stroma. The typical lesion has been described as a multilocular cystic mass with a hypointense T2-weighted mural or septal component. The hypointensity on T2-weighted images most likely represents dense fibrous tissue within the wall or septae [4].
Regarding our patient's ovarian lesions, the findings were consistent with bilateral cystic masses, with a differential diagnosis between cystadenomas, cystadenofibromas or ovarian carcinoma of borderline malignancy. The possibility of borderline tumor was based on the thick mural component in the larger right sided ovarian lesion.
Intraperitoneal dissemination is the most common route of spread of ovarian cancer and it is one of the major factors influencing prognosis in ovarian cancer [5]. Peritoneal metastases are usually ill-defined, hazy or cloud-like masses of varying size, without marked enhancement. Ascites is common, and the fluid may outline small implants, facilitating their detection [6].
The initial differential diagnosis of the peritoneal deposits in our case included metastases and endometriosis plaques. Features which were against metastases included absence of ascites and intense enhancement of the peritoneal deposits after contrast injection. The patient's advanced age and lack of supportive findings on prior laparotomy were against endometriosis plaques. The other important differential diagnosis to consider was splenosis.
Splenosis, first described by Buchbinder and Lipkoff [7] refers to heterotopic implantation of viable splenic tissue after spillage or intravascular migration of cells from splenic pulp, secondary to splenic trauma with rupture, accidental damage to the spleen during splenectomy or other surgery. The spleen fragments or splenules may develop anywhere in the abdominal cavity, the peritoneal cavity being the most common location. However, cases of hematogenous spread have been observed, resulting in intracranial sites of implantation [8], and thoracic splenosis was reported in cases of rupture of the spleen combined with diaphragmic perforation [9]. Splenosis may be found incidentally in an asymptomatic patient or could complicate a diagnosis by mimicking malignant conditions such as peritoneal carcinomatosis. Based on the author's literature search, cases have previously been published where splenosis mimicked peritoneal metastases from non-ovarian primary abdominal tumors [10-14]. To best of our knowledge, this is the first case to describe splenosis mimicking malignant spread in complex ovarian masses.
In the presence of ovarian lesions, solid peritoneal masses become even more suspicious. Regardless, the possibility of splenosis should be ruled out in appropriate cases. Investigation of such lesions may require high level of suspicion and proper investigation. Imaging studies can support this diagnosis and assist the surgeon in planning the operation of an ovarian mass suspicious for malignancy. Typical imaging features of splenosis include being iso- or hypodense relative to the liver on CT, with early prominent enhancement similar to the spleen. Scintigraphy with 99Tc-labelled red blood cells is considered the most sensitive and specific imaging modality to confirm the diagnosis of splenosis [15]. Nowadays, MRI provides one-stop imaging for characterizing both primary abdominal lesions, in our case ovarian masses, and the presence of metastatic spread. Likewise, MR supports the diagnosis of splenosis, showing nodules that are hypointense in T1 and T2-weighted images with enhancement characteristics similar to normal splenic tissue [16]. A few case reports have suggested ferumoxides-enhanced MRI as a novel technique for diagnosing splenosis. Ferumoxides are superparamagnetic iron oxides that are removed from circulation by the reticuloendothelial system [17]. However, this imaging modality has not been incorporated in to every day practice.
As in our case, the preoperative consideration of non-malignant disease permits avoidance of unnecessary extensive procedures and medical treatment thereby improving disease management and decreasing patient morbidity.
It is important to emphasize that imaging studies alone provide nonspecific characteristics of splenosis with a wide differential diagnosis including metastatic disease, abdominal lymphoma, hemangiomatosis, peritoneal mesothelioma, multifocal endometriosis, primary renal or hepatic malignancy, gliomatosis peritonei, granulomatous peritonitis as the consequence of disseminated infection such as tuberculosis or histioplasmosis, rupture of the tumor or a hollow viscus, or, simply, reactive adenopathy [18]. Based on the imaging findings described above and history of prior splenectomy, the diagnosis of splenosis should be strongly suspected. However, in cases of suspicious or known malignancy, the tissue diagnosis is required through percutaneous biopsy or intraoperative sampling, as in our patient.
A history of post-traumatic splenectomy should bring to mind splenosis when faced with multiple intraperitoneal nodules. This is especially important in cases with suspected ovarian neoplasia. Furthermore, imaging-based characterization of the primary ovarian tumor may aid in the differential diagnosis of benign and malignant lesions. MRI may provide a one-stop imaging solution for advanced evaluation of ovarian masses and suspicion of splenosis nodules, followed by intraoperative histological confirmation.
Informed consent was obtained from the patient for submission of this manuscript for publication.