The prevalence history for intestinal protozoal and helminthic infections among Iraqi people is reviewed from 2000-2020. The distribution of the intestinal parasites is mentioned in different communities including hospital patients, primary school children, food handlers, general population, immunocompromised patients, malnourished patients, sicklers and day-care centers attendance in both rural and urban regions. The prevalence rates are also illustrated in relation to age and sex parameters. Protozoal infections are the most common infections in Iraq. Other parasitic infections are of a local public health problem. Even parasitic infections could cause malabsorption, malnutrition and blood loss but also might cause physical and mental growth retardation specially among children. Therefore, Implantation of a national control program is essential to apply.
Intestinal parasites, Iraq, Prevalence
Intestinal parasites are prevalent throughout the world particularly in tropical and subtropical countries where deficiency in water and sanitation [1]. The high prevalence recorded in some regions possibly by introduction of infections through refugee camps and migration due to war and insecurity [2]. Many investigations have shown various prevalence rates of infections. The distribution of the parasites depends on the presence of suitable hosts, habits and favorable environmental conditions. Intestinal protozoa require only slight carelessness in habits leading to cosmopolitan distribution all over the world. They have a major public health importance due to their relation to socioeconomic, environmental factors, sanitation level and education in the community. Intestinal helminthiases contribute to poor nutritional status in infected children due to their adverse effects on food intake, normal nutrient absorption and immunity [3-5].
Nutritional impairment is often associated with chronic helminthiasis, as with those suffering from protein-energy malnutrition, iron-deficiency anemia and vitamin A deficiency [6,7]. The pathogenic protozoa are a common cause of diarrhea and have a worldwide distribution [6-8]. This remain an important cause of deaths among children less than 5 years old [9]. This is due to poorly developed immune systems. Therefore, severity of infection depends on virulence of the strain, host susceptibility and immune status as well as mixed infections [10].
Estimation of the global prevalence of the soil-transmitted helminths; 1000 million cases for Ascaris lumbricoides, 900 million for hookworms and 500 million for Trichuris trichiura. It has been reported that, probably 480 million people carried Entamoeba histolytica and 36 million develop invasive forms of amoebiasis. In addition, 200 million occur per year in Africa, Asia and Latin America [7,11].
In Iraq, studies on intestinal parasites started as early as 1939 [12]. Then, surveys were conducted recently and involved rural areas, school children in both sexes but mainly in and around the capital Baghdad. The prevalence diseases in Iraq differ from one region to another.
The present work illustrates the prevalence of intestinal parasites in relation to age, sex and socioeconomic factors.
The prevalence rates of intestinal protozoa and helminths parasites are reviewed according to the types of communities including general and selected populations in different Iraqi provinces (Figure 1).
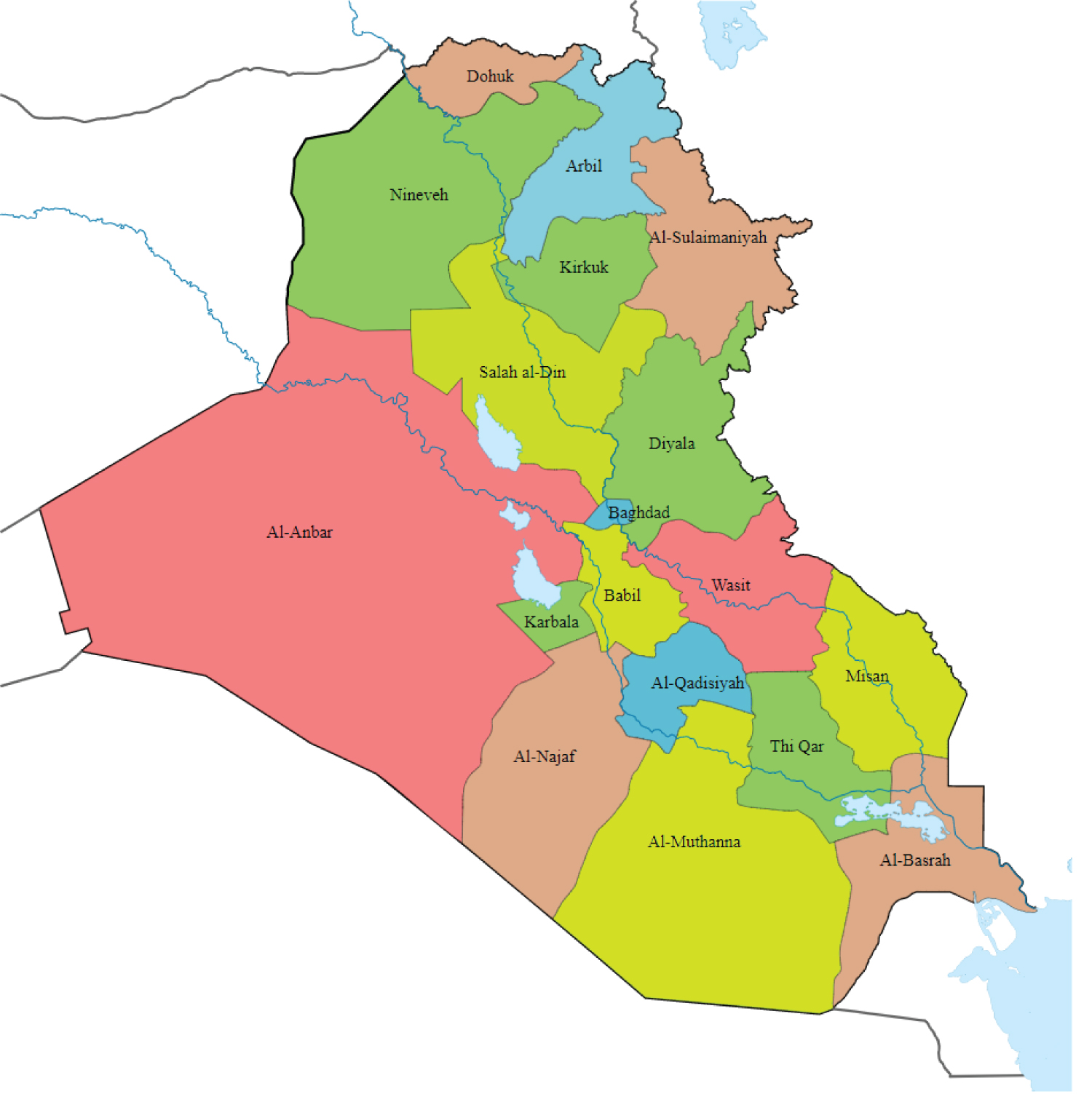 Figure 1: Map for Iraqi provinces.
View Figure 1
Figure 1: Map for Iraqi provinces.
View Figure 1
In and out patients are easier to investigate for parasitic infections. Ten surveys among all age groups were done in the middle part of the country, 4 in the Southern part and 7 in the Northern part (Table 1). However, medical history, morbidity and mortality of various parasitic infections are lacking in Iraq. Prevalence rates ranged from 7.36% to 84.67% and 0% to 18.01% of the protozoa and helminth infections respectively.
Table 1: Density grades in male group. View Table 1
School children (6-12 years old) were chosen by many workers because they are easier to deal with, represent the actual population of the communities and in various standards of living (Table 2). These data are concerned with the prevalence rates of infections among school children and not the household members of infected children.
Table 2: Density grades in female group. View Table 2
Animal handlers including veterinian, butchers and breeders could also acquire the parasitic infection at a rate of 50% in comparison to 14.8% for non-animal handlers (Table 3).
Table 3: Average range ratio of high frequency and low frequency in male group. View Table 3
The prevalence of intestinal protozoa and helminths among general populations in the middle part of the country including the capital Baghdad is illustrated in Table 4. The large samples surveyed were fairly representative of the general population. Even the prevalence rates of intestinal protozoa and helminths recorded during 2000-2020, were markedly lower than those reported in 1939 (73.9 and 41.0 for protozoal and helminths respectively) [12] but they are still representing a significant level from the public health point of view. Even so, it implants an improvement in sanitation, health and medical services.
Table 4: Average range ratio of high frequency and low frequency in female group. View Table 4
Higher prevalence rates were recorded among patients with malignant diseases due to immunosuppression caused by either the disease itself or the cytotoxic drugs or both of them (Table 5).
Table 5: Average value of energy in male group. View Table 5
Only one work has been done in Basrah on 2005 where the malnourished children with diarrhea showed a higher prevalence rate (15.4%) for protozoal infections in comparison to malnourished children without diarrhea (10.75%) for protozoa and 2% for helminths (Table 6).
Table 6: Average value of energy in female group. View Table 6
Higher prevalence rate of parasitic infection (62.5%) was observed among patients with sickle-cell anemia in comparison with non-sicklers (14.8%) (Table 7).
Table 7: Histogram of parenchyma of healthy lungs in male group. View Table 7
Almost similar prevalence rates were reported in Basrah (42.5%) and Dohuk (43.3%) as far as protozoal infections are concerned (Table 8).
Table 8: Histogram of parenchyma of healthy lungs in female group. View Table 8
Prevalence of intestinal parasitic infections is expected to be higher in rural districts and villages especially among children (Table 9). This can be attributed to the lower standard of hygiene, over-crowdness, sanitation and probably food and/or water-borne infection. Agricultural practices and animal breeding are also responsible for the recorded prevalence rates. In marsh region of South Basrah 36.4% of water samples were contaminated with intestinal parasites [13]. Nevertheless, due to the progress in establishing and developing a good water supply, electricity, paved roads and education, the prevalence rates were dropped in 2002 for helminthiasis but not for protozoan infections.
Table 9: Average histogram value of healthy lung parenchyma in male group. View Table 9
In contrast to the rural districts, the prevalence rates of intestinal parasites are markedly lower (Table 9). The recorded low prevalence rates are probably attributed to the adequate standards of living and conditions of the environmental sanitation.
No significant differences were noticed in the prevalence rates of males and females (Table 9). But nevertheless, some works have reported the prevalence rate of infection was higher among females in comparison to males. This may be due to fact that these females are housewives responsible for a house work, agricultural practices and animal breeding [14].
Lack of published papers was observed in relation to the distribution of infection among people with an age more than 21 years (Table 10). This is possibly due to sampling difficulty for the population with this wide range of ages.
Table 10: Histogram value of healthy lung parenchyma in female group. View Table 10
The presented data presented in Table 11. The protozoan parasites are highly prevalent in all examined groups including general population, hospital patients, school children in urban and rural districts reaching a rates of infection of 61.6 [15] and 88% [16]. The highest rate of infection reported for the emerging opportunistic Cryptosporidium was 18.94% [17]. A significant association was found between giardiasis and water contamination. About 31.6% of the inhabitants use storage water, while only 1.3% use sterile water bottles [18]. In addition, the use of waste water to irrigate vegetables or organic manure as a fertilizer that are eaten raw without proper washing leads to food-borne parasitic infections [19,20]. Ascariasis was detected at a lower rates of infection (Table 11). In contrast, prevalence of hymenolepiasis nana was getting higher in 15 studies out of 21 indicating a public health problem specially among children. Thus, it needs more attention for application of control measure. Enterobius vermicularis was detected only accidently because stool examination is of no value in its specific diagnosis [7].
Table 11: Entropy in male group. View Table 11
Some workers have reached a decision that the concentration stool examination methods are better than direct smear method in the diagnosis of helminthiases which might have an influence on the prevalence rate in the area or the examined population. Therefore, if this is true, there will be a close relationship between the rate of infection and the method followed for stool examination.
Although the prevalence rates of intestinal parasitic infections are varied from one area to another according to the degree of personal and community hygiene, sanitation and climatic factors are relatively common in Iraq. Intestinal protozoan, helminthic or mixed infections are prevalent among all types of communities and population samples from both urban and rural regions of Iraq. Adults and children of both sexes are infected. Therefore, an urgent and efficient preventive and control measures is essential.
Even an adequate treatment for amoebiasis and giardiasis, which are the common causes for diarrhea, is available, the morbidity is still high. The complications of invasive amoebiasis are potentially fatal and giardiasis may cause malabsorption in children [4,6,7].
Several intestinal helminthiases contribute to the general and persistence of malnutrition and reduced productivity [6,7]. Careful evaluation of the individual parasite should be continued in different regions and among different societies.
Implementing a national control program should include a primary health care, health education, family planning, water supply, paved roads, environmental sanitation, nutrition, mass treatment by new broad spectrum antihelminthics, avoid crowdness and improvement in agriculture practices. Anti-protozoal and broad-spectrum antihelminthics are available and effective at a regular mass treatment. Well trained health workers chosen from the same community are valuable in the diagnosis and treatment of various parasitic infections especially in rural areas and far villages in the country.