Chronic thromboembolic pulmonary hypertension (CTEPH) is a form of hypertension pulmonary due to a mechanical obstruction of pulmonary arteries, which is caused by organized fibrotic thrombi. Consequences of pulmonary artery obstruction are an increase in pulmonary vascular resistance with pulmonary hypertension and heart failure [1].
The main chest CT findings in CTEPH are the artery pulmonary enlargement and failure fill branches. Since there is a network of anastomotic channels linking the pulmonary and bronchial circulation, the bronchial arteries also present higher pressure in CTEPH, and neo-vascular formation may occur [2]. We report a case of a CTEPH patient that developed fistulas between the bronchial and coronary circulation.
A 42-years-old-male patient presented sudden dyspnoea and was diagnosed with acute PE, and started treatment with warfarin. Despite the treatment, the dyspnoea worsened over the years. He was then referred to our pulmonary hypertension center. On admission, he presented functional class III, pulse oximetry of 90%, severe lower limbs edema. At echocardiography, systolic pulmonary artery pressure was 112 mmHg, with signs of severe right ventricle dysfunction. CT scan demonstrated signs of CTEPH associated with marked bronchial arteries dilation (Figure 1). The right heart catheterization showed mean PAP 60 mmHg, PVR 12.9 W, CO 3.8 L/min. Coronary angiography demonstrated collaterals between the right coronary artery and bronchial circulation (Figure 2). These appeared to contribute to myocardial ischemia, evidenced by a myocardial nuclear scan.
Chronic thromboembolic pulmonary hypertension (CTEPH) is a unique form of pulmonary hypertension which the main therapeutic option in CTEPH is pulmonary endarterectomy (PEA), a surgery that removes the occluding material of pulmonary vessels, as well as the vascular endothelium. Coronary-bronchial fistulas have been described in CTEPH and can account for 30% of the systemic blood flow, but are not a frequent finding. In this case, collaterals were so relevant that they induced myocardial ischemia during a cardiac nuclear scan. Recognition of such vascular abnormality is important for appropriate surgical planning, in which PEA can be considered together with coronary revascularization.
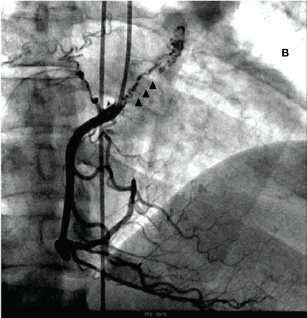
Figure 1: CT scan showing signs of CTEPH associated with marked bronchial arteries dilation.
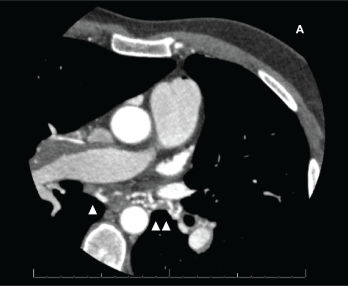
Figure 2: Coronary angiography showing collaterals between the right coronary artery and bronchial circulation.