Meningiomas are the most common primary brain tumors, Orbital invasion usually invades as an extension of the sphenoid wing meningiomas. We report the case of a 54-year-old man who presented with frontotemporal intraosseous meningioma with intraorbital invasion.
Intradiploic meningioma, Intraosseous, Orbital invasion, Exophthalmos
A 54-year-old man presented with slowly progressive exophthalmos and right unilateral blindness for two years, Palpation shows a hard right temporal mass adherent to the bone. Visual acuity assessment reveals a lack of light perception and fundus examination shows papilledema. Examination of the left eye is normal, he does not present any neurological deficits. The CT scan and magnetic resonance imaging (MRI) showed an extra-axial intradiploic right frontotemporal lesion invading the external part of the orbit roof (Figure 1). For the first time, the patient underwent a lateral skin incision orbitotomy. Total resection could be performed, Histologic examination confirmed anintraosseous ectopic meningioma (WHO Grade I) a second intervention by cranial approach was programmed.
Meningiomas are the most frequently occurring benign intracranial neoplasms [1]. Although intradiploic meningiomas or primary intraosseous meningiomas are a subtype of primary extradural meningiomas, they are rare with an incidence accounting for < 2% of all such tumors and usually located in frontoparietal and orbital regions [2]. These lesions are described as slow-growing, histologically benign lesions, however, some studies indicate that intraosseous meningiomas have a higher incidence of malignant features than intradural meningiomas [3].
There are different hypotheses regarding the origin of intraosseous meningioma [4]. First, the development would be from ectopic meningocyte or from cells of the capillaries which would be trapped in the cranial sutures during embryonic development. The second hypothesis reported cases had a history of trauma in the region of the meningioma [5].
However, the latter was absent in our patient. Crawford, et al. found only 5 of 36 cases with primary intraosseous meningioma who had a history of head trauma in the same location of the tumor [6]. Clinically, most patients with intraosseous meningioma and orbital invasion, present with a slow-growing bone mass without pain, progressive and painless exophthalmos, and a very slow decline in visual acuity that can lead to blindness without associated neurological manifestations [7]. This is consistent with the clinical data of our patient. A CT scan with a bone window is necessary to detect cortical hyperostosis of the tumor as well as osseous extension. Hyperostosis is the most frequent which account for 65% but osteolysis is also reported in 35% as well as a mixed image in 6% of cases [8]. MRI appears to be more effective to evaluate the soft tissue component and extraosseous invasion. Unlike intradural meningiomas, the dural tail sign is absent in c meningiomas.
Surgical management with total resection of the lesion and all the invaded tissues, the dura mater, the muscle, and intraorbital tissues, followed by cranial reconstruction is the treatment of choice [9]. Adjuvant therapy is recommended for patients who had malignant or atypical features histologically, and/or enlarging residual tumors [10].
Intraosseous meningiomas with intraorbital invasion are rare tumors, of slow evolution, responsible for essentially ophthalmologic symptomatology. The impairment of visual function is a factor of poor prognosis. It is therefore important to inform the patient that surgery does not always guarantee visual recovery.
The authors declare no conflict of interest.
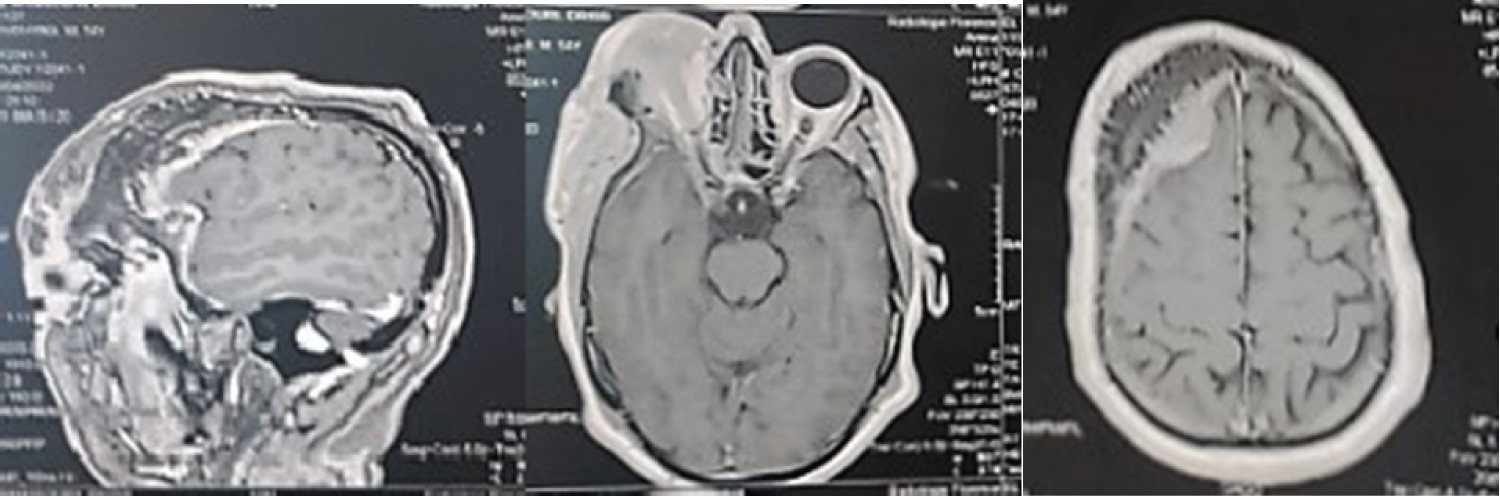
Figure 1: Axial and sagittal T1-weighted MR images after Gadolinium contrast administration, showing a Hypointense intradiploic mass with moderate peripheral enhancement.