Challenges in mandibular bony defect reconstruction still exist. The use of compacted autogenous particulate corticocancellous bone, together with a human humerus allograft presents an exciting opportunity to simplify the reconstruction of such defects. This is especially the case when the surgery may be done in one stage via an intra-oral approach. We present a case where all of the above have been incorporated for the reconstruction of the mandible.
Mandible, Reconstruction, Allogenic conduit, Autogenous bone graft
The cellular biology of bone healing is an ongoing topic for research. Whilst it is understood that several growth factors interact with the cells of bone, the exact understanding of how this works remains an enigma. As early as 1956 it was already discovered that bone heals in two distinct phases, with the first early phase resulting in bone quantity and the second in quality [1].
The use of particulate corticocancellous bone (PCCB) has been proven to be successful [2], with increased osteogenesis and decreased complications when compared to cortical grafts [3].
The use of allogenic bony cribs as a graft carrier has been reported in several studies [4-6].
South Africa seems to be plagued by patients with late presentation of benign odontogenic tumours such as Ameloblastoma. These patients invariably require ablative surgery to render them disease free, but the subsequent reconstruction of the mandible remains challenging, when trying to select appropriate techniques and graft material.
We revisit the concept of making use of an allogenic carrier in conjunction with the use of PCCB for the reconstruction of mandibular bony defects.
A 17-year-old male patient presented with right-sided facial asymmetry, and a large bony mass that was painless could be palpated in the lower jaw. The teeth of the involved hemi-mandible were mobile, and there was paraesthesia of the distribution of the lower right inferior alveolar nerve. The patient presented with no systemic compromise, and was otherwise well. A benign neoplasm (Ameloblastoma) was suspected and confirmed via incisional biopsy of the right hemi-mandible (Figure 1). A right-sided hemi-mandibulectomy with disarticulation, was subsequently performed via an intra-oral and pre-auricular approach. A preformed reconstruction plate with add-on condyle (DePuy Synthes CMF, West Chester, PA) was used together with an alloplastic Temporomandibular joint (TMJ) fossa (Zimmer Biomet CMF, Jacksonville, FL) (Figure 2). An allogenic demineralised humerus (Bone SA, Bramley, Johannesburg, South Africa) was used as a conduit for a compacted autogenous PCCB graft, harvested from the anterior iliac crest. This bone conduit was then secured to the reconstruction plate (Figure 3) and the intra-oral access closed in two layers. Maxillomandibular fixation (MMF) was applied (released after 4 weeks), and a nasogastric feeding tube (NGT) inserted. The Patient was fed for seven days via NGT and was kept on antibiotic prophylaxis and analgesia for that duration, and then discharged from hospital. Follow-up occurred at regular intervals for 18 months after the surgery (Figure 4).
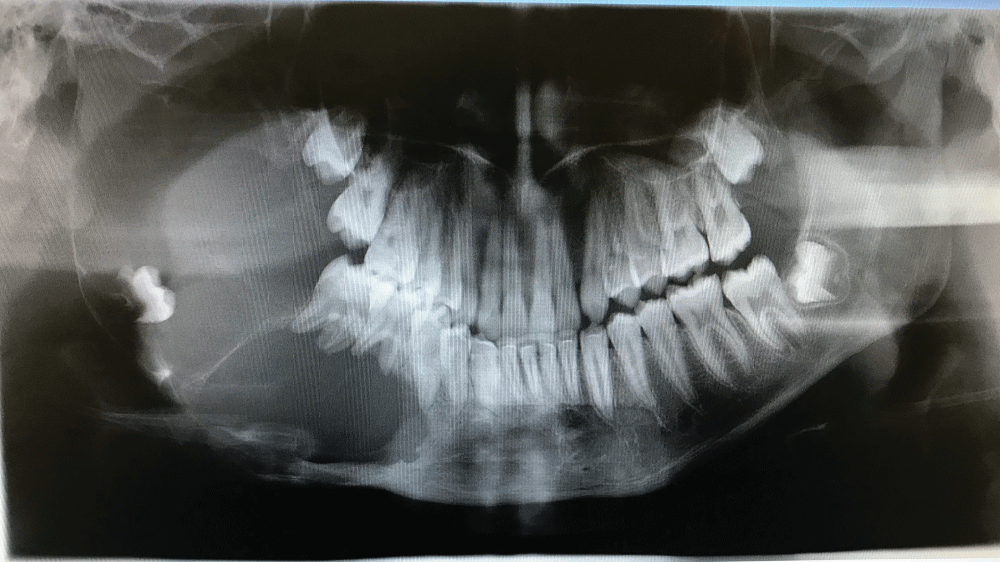 Figure 1: Pre-operative OPG showing the extent of the ameloblastoma involving the entire right hemi-mandible, and including the mandibular condyle and coronoid process.
View Figure 1
Figure 1: Pre-operative OPG showing the extent of the ameloblastoma involving the entire right hemi-mandible, and including the mandibular condyle and coronoid process.
View Figure 1
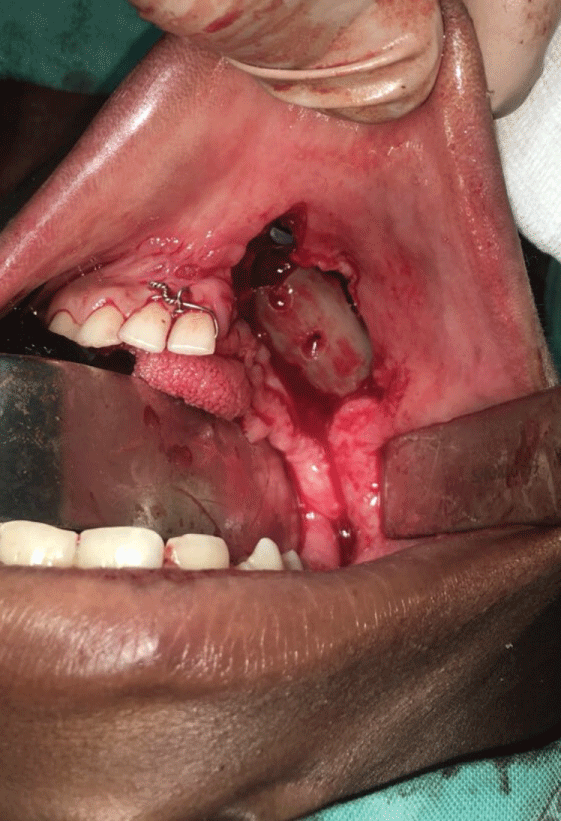 Figure 2: Photograph shows the intra-oral access, and the demineralised humerus conduit containing the PCCB; attached to the reconstruction plate.
View Figure 2
Figure 2: Photograph shows the intra-oral access, and the demineralised humerus conduit containing the PCCB; attached to the reconstruction plate.
View Figure 2
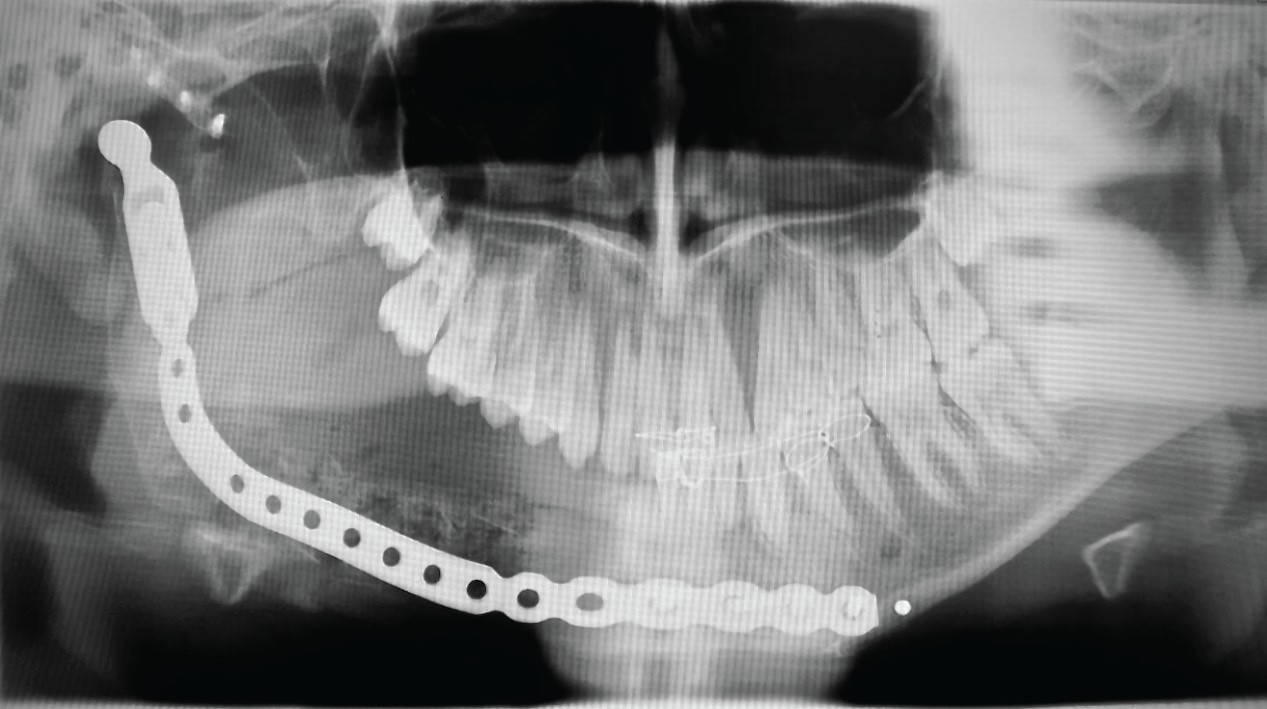 Figure 3: Post-operative (4 weeks) OPG showing a reconstruction plate with early and immature bone graft.
View Figure 3
Figure 3: Post-operative (4 weeks) OPG showing a reconstruction plate with early and immature bone graft.
View Figure 3
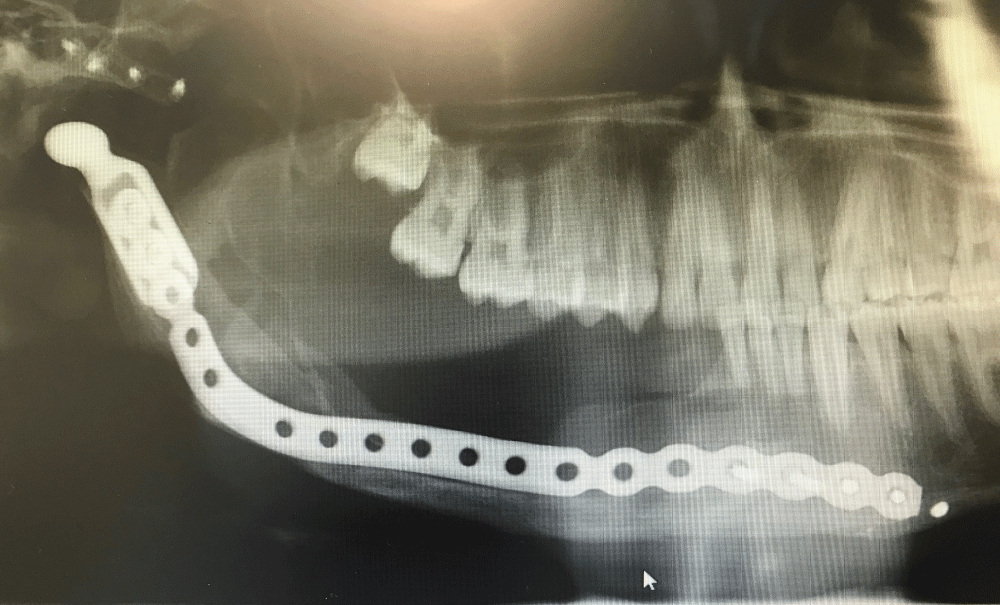 Figure 4: Post-operative (12 months) OPG depicting a now mature ossicle ready to receive dental implants and rehabilitation of the dentition.
View Figure 4
Figure 4: Post-operative (12 months) OPG depicting a now mature ossicle ready to receive dental implants and rehabilitation of the dentition.
View Figure 4
The use of free vascularised bone grafts have their role to play, especially when they are part of a composite flap used to reconstruct defects with extensive soft tissue loss. The role of non-vascularised bone grafts cannot be underestimated, especially when dealing with defects resulting from benign pathology or trauma. This mode of reconstruction inherently carries less morbidity for patients, and is a relatively simple procedure to perform. Ferretti, et al. describe an elegant and successful technique of bony reconstruction of the mandible [2]. Our technique is believed to be a further simplification of established grafting methods, on the basis that it is performed as a single stage procedure, and the bone augmentation via a trans-oral approach.
Since it is performed via an intra-oral approach, the aesthetic result of the surgery is most agreeable to patients. The allogenic humerus takes two weeks to prepare, and once packaged may be stored for up to 2 years in refrigerator, which means that cases may be planned on a whim. This bone in non-immunogenic and carries no risk for transmission of infectious disease as it is Gamma irradiated (25 kGy) further, all donors are tested for HIV; Syphilis; Tuberculosis and Hepatitis B & C. By utilising a demineralised humerus, the PCCB is contained and less likely to disperse, allowing for a reduction of MMF to 4 weeks. The volume of the graft is also less, thus allowing harvesting mostly from the anterior ilium. The humerus acts in the same way as the spacer used by Ferretti, et al. in maintaining the overall dimension of the graft bed. Finally, the anatomical morphology of the humerus resembles the native mandible; thus facilitating the placement of dental implants and subsequent oral rehabilitation. The fact that this procedure may be performed as a single surgery, means that many more patients may be treated; at considerably less financial cost (the bone retails at a cost of around USD 140 for 10 cm shaft and USD 280 for 20 cm shaft). This case report forms part of an ongoing and larger study of this procedure and technique at our institution.
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
There are no conflicts of interest to declare.
No ethics approval required.