Noise exposure is an important factor in the management of intensive care patients [1]. There are many different causes of noise in the ICU such as equipment, monitors, staff, family plus other additional sources. Patients in the ICU are exposed to these noise sources for 24 hours a day with no respite. The noise levels can vary significantly during the day as well as significantly between patient bed-spaces. There are detrimental effects from excessive noise exposure; some of this is related to the risk of damage to a person's hearing [2]. There are; however, other concerns that need to be considered for the ICU patient. Excessive noise can affect a patient's ability to sleep, resulting in sleep deprivation [3]. High noise exposure has also been associated with increases in heart rate and blood pressure in young children [4]. There are also potential detrimental effects from loud noise with respect to the staff's health [5]. We have previously shown that in our ICU the majority of our patients experience an average noise level per minute > 80 dB. With peak noise exposure > 100 dB occurring for more than 10% of the day [6]. This is higher than the recommendation of the AAP with respect to safe noise level exposure [7].
Many patients in the ICU are sedated and ventilated due to their treatment needs. It may be that excessive noise by the patient's bedside could require extra sedation to keep the patient comfortable. The physiologic signs of light sedation may mimic a patient's response to loud noise.
The aim of this study was to monitor the patient's bedside noise over a 24 hour period. This background noise level was then compared the noise levels during periods of care when sedation boluses or increased infusion rates were required.
After IRB approval and informed parental consent patients were recruited to this study in a convenience sequential method. Entry criteria were admission to the PICU at WCHOB, intubated and receiving sedation by infusion. There were no exclusion criteria. There were no changes to the configuration to the patient's room or to the care the patient received. All routine care and procedures (i.e. intubations, central venous lines, blood draws, and daily nursing care) was not altered by this research project. Subjects were randomly chosen by room assignment. A randomized room number grid was prepared using a random number generator. If the next room was occupied then that patient was recruited, otherwise the next room on the list was taken until the next patient was recruited. The same gird was used in a continuous rotational manner.
The NoisePRO® device is an Occupational Safety and Health Administration (OSHA) approved device capable of recording the room noise level in decibels (dB) Figure 1. The noise level can be measured as frequently as every second with a high degree of accuracy and sensitivity [8]. Its use is approved in measuring occupational noise level exposure. The NoisePRO® was setup in an OSHA approved manner as used for assessing noise exposure Table 1. This involved passing a daily calibration test using the supplied 140 dB calibration device (accurate to within ± 0.1 dB). For noise measurement, the microphone was placed about 1 meter from the patient's head in a manner where it is not likely to be disturbed during patient care. The NoisePRO® recorded the average noise level (and the peak noise level during each second) a for each minute over a 24 hour period.
 Figure 1: NoisePRO® recording device. View Figure 1
Figure 1: NoisePRO® recording device. View Figure 1
Table 1: NoisePRO® recording settings. View Table 1
Data was collected from the patient's chart regarding the use of sedation: Boluses and or increases in sedation infusions were noted, the time and dose of this sedation were recorded. These sedation requirements and noise levels were then compared to ascertain correlation between noise exposure and extra sedation. Noise levels were averaged for the 5 minutes prior, 5 minutes during, and 5 minutes after a sedation change. Open or closed room location as well as patient demographics were also recorded.
Over a 6-month period, nineteen patients were enrolled in the study. There were 8 male and 11 female children with a mean age of 4.4 (± 6) years. The majority of these children were in individual rooms (n = 15). The average bedside noise level: Maximum, minimum, and mean dB were 82.2, 53.3, and 62.4, respectively Table 2. The average percent of time spent above 80 dB was about 0.1% of the 24 hour period. There was considerable variation in the noise levels the children were exposed to during the day. With the average peak noise exposure greater than 130 dB. The noise levels before, during and after the additional sedation requirement is shown in Table 3. There was no significant difference in the noise levels between these three time periods. A total of 109 boluses of sedation/increases in the infusion rates were recorded Table 4. The range showed one patient required no additional sedation and one patient required 22 boluses of sedation over a 24 hour period Figure 2. The additional sedation included: Fentanyl (63% of sedation), Midazolam (18%), Lorazepam (13%), Morphine (4%), Isoflurane (2%), and Methadone (1%). The sedation dosing used is shown in Table 5. To take into account, different beds may have different noise levels due to equipment or other reasons we also evaluated the noise levels at the sedation administration times with respect to the individual's bedside mean noise level. When comparing the peri-sedation noise levels as a percentage of the maximal and minimal noise level at each bedside, there were statistically significant differences in the percent of noise when sedation was administered compared to the bedside minimum noise level. However the noise level was 25% less than the maximum bedside levels and not clinically significantly from the bedside average noise levels during the sedation requirement.
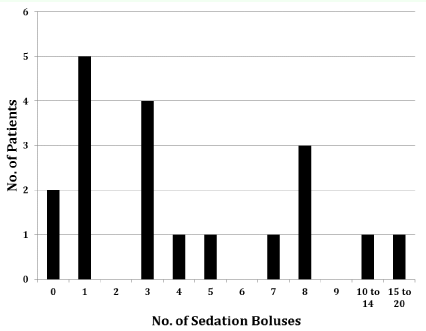 Figure 2: Number of Sedation Boluses used.
Figure 2: Number of Sedation Boluses used.
The majority of patients required 3 or less sedation boluses during the 24 hour period. View Figure 2
Table 2: Noise data. View Table 2
Table 3: Noise Levels (dB) and Sedation Administration. View Table 3
Table 4: Sedative Agents used for Sedation Changes (n = 109). View Table 4
Table 5: Doses sedation used. View Table 5
Here, we report on the first study done to look at noise levels at a patient's bedside and its effect on sedation requirements. This study showed that there was no difference in noise levels between the 5 minutes before, during, or after a sedation bolus was given. This study was done after an initial study that showed noise levels in our pediatric intensive care unit exceeded the international recommended noise levels [6]. This current study now shows that the decibels at the bedside had decreased significantly after implementing noise reduction measures. This may show that if patients' environmental noise levels are less than the maximum recommended decibels, their sedation requirements are more likely to be from their ongoing disease process and medical management and less likely from environment influences.
While there was no difference in noise levels in the periods surrounding a sedation bolus or escalation in infusion dosing, there was a difference noted between the average decibels and minimum decibels. At the time a bolus was given, the decibel level was significantly higher than the minimum decibels recorded at that bedside over the course of the day. These minimum levels recorded in our study were below the averages recorded in previous studies [6,9,10]. Also, the maximum levels were only slightly above the recommended 80 dbA. Therefore, these levels are also lower than previously documented studies. A study looking at the effects of ICU noise on normal sleep [11] determined that the degree change in exposed noise level rather than the actual maximum level was the factor that caused arousal from sleep. This again supports the thought that noise levels that are maintained below the national recommendation may play no clinically significant role in patient sedation and analgesia requirements.
Limitations of this study include that the indication for sedation supplementation was not documented, nor the efficacy of the sedation used. The doses shown in Table 6 appear to be consistent with recommended dosing for each of the agents documented. Also this is a small number of patients, and as such serves as a pilot study. A larger study looking at both levels before, during, and after sedation dosing as well as 24 hour sedation levels may better show any relationship between noise pollution and sedation needs.
Table 6: Percent of background noise level during sedation administration. View Table 6
This study describes a small cohort of patients receiving sedation infusions during mechanical ventilation without a pediatric intensive care unit. Despite our initial hypothesis, there appeared to be no difference in noise levels before, after, and during additional sedation boluses. There was no difference between the noise during boluses and the average or maximum noise levels throughout the day. However, when sedation was given there was a difference between the noise at the time of sedation and the minimum decibel noise level in the room.