Specific criteria have been developed for the diagnosis of acute myocardial infarction in patients with right ventricular pacing, but not for patients with bi-ventricular pacing. We present a case of a patient with a biventricular implantable cardioverter defibrillator (BiVICD), who presented with symptoms consistent with acute coronary syndrome (ACS), new ST elevations of the inferior leads, and was found to have acute occlusion of right coronary artery (RCA). In conclusion, this case highlights that in patients with suspected ACS with biventricular pacing, dynamic ST segment elevation may be a sign of acute transmural infarction and can localize the infarction territory.
Bi-ventricular pacing, STEMI, AMI, PCI, Sgarbossa
Successful treatment of acute myocardial infarction (AMI) via percutaneous coronary intervention is largely dependent upon accurate and timely diagnosis of potential tissue death via electrocardiogram (EKG) findings. As this often occurs in an emergency room or critical care setting, it is important for these physicians who may first encounter these EKG abnormalities to have a high suspicion for ischemia. This can prove to be a diagnostic dilemma in patients with artificially paced rhythms, as they may cause misleading ST and T wave abnormalities which can be difficult to distinguish from true ischemic changes. Given the significant overlap in patient populations at increased risk for acute coronary syndrome (ACS) and those with pacemakers or implantable cardioverter defibrillators (ICDs), this potential for missed diagnoses is particularly troublesome. In the past, inhibition of artificial rhythms to better assess the underlying rhythm or serial EKGs were utilized to identify ACS, however this has the drawback of potentially delaying appropriate medical management. To address this concern, specific criteria have been developed for the diagnosis of AMI in patients with right ventricular pacing [1]. However, no such standards have been established for patients with biventricular pacing. We present a case in which ST segment elevation in the inferior leads on a biventricular paced rhythm assisted with the diagnosis of AMI involving the RCA.
An 81-year-old man presented with sudden onset chest pain, shortness of breath and hypotension with a blood pressure of 84/60 mmHg. He had a history of coronary artery bypass graft (CABG) and bioprosthetic mitral valve replacement 5 years ago followed by implantation of a biventricular ICD for severe left ventricular systolic dysfunction, NYHA Class-III CHF symptoms and a left bundle branch block (LBBB). Compared with prior available baseline EKG (Figure 1a), his EKG showed A-V sequential biventricular pacing at rate of 60 bpm and new 2 mm ST segment elevations in Lead II, III, aVF as well as ST segment depression and T wave inversions in the anterolateral leads (Figure 1b). An emergent cardiac catheterization was performed showing acute thrombotic occlusion of the proximal right coronary artery (Figure 2a). Successful percutaneous coronary intervention was performed with drug eluting stent placement in the proximal right coronary artery leading to resolution of the patient's symptoms (Figure 2b).
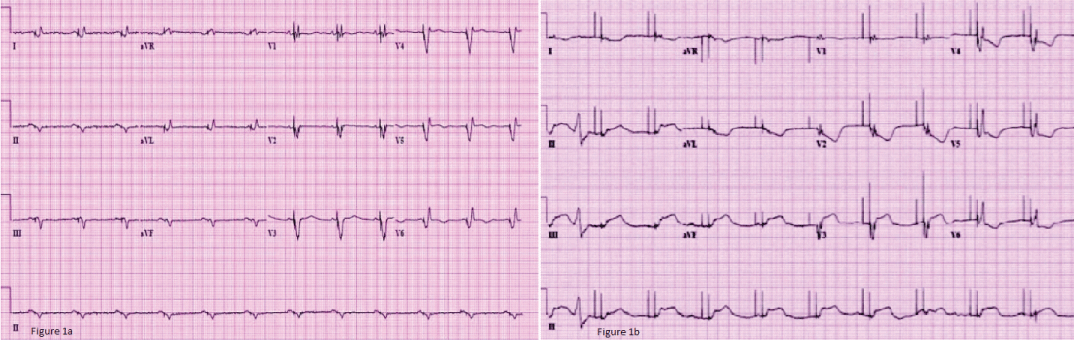 Figure 1: a) Baseline EKG with sequential A-V Biventricular pacing; b) EKG at presentation showing biventricular pacing and ST segment elevations in the inferior leads with ST segment depression and T wave inversions in the anterolateral leads. View Figure 1
Figure 1: a) Baseline EKG with sequential A-V Biventricular pacing; b) EKG at presentation showing biventricular pacing and ST segment elevations in the inferior leads with ST segment depression and T wave inversions in the anterolateral leads. View Figure 1
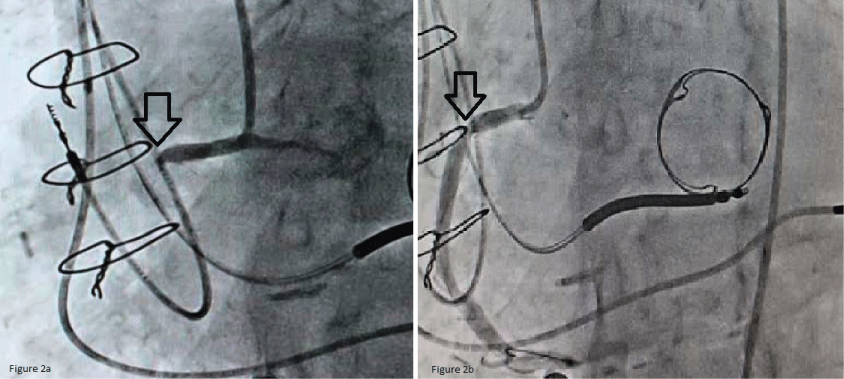 Figure 2: a) Diagnostic coronary angiography with complete occlusion of the proximal right coronary artery; b) Successful angioplasty with stent resulting in restoration of normal blood flow to the Right Coronary Artery. View Figure 2
Figure 2: a) Diagnostic coronary angiography with complete occlusion of the proximal right coronary artery; b) Successful angioplasty with stent resulting in restoration of normal blood flow to the Right Coronary Artery. View Figure 2
As health care providers in the emergency and critical care setting are often the front line in diagnosis of AMI, it is important for them to be able to utilize EKG findings for diagnosis. Pre-existing abnormal depolarization or repolarization makes this difficult, however. Sgarbossa's criteria have been well established as a modality of identifying AMI in patients with native LBBB as well as right ventricular paced rhythm which can look like a LBBB [2]. This case highlights that in some patients with biventricular pacing, dynamic ST segment elevation may be a sign of acute transmural myocardial infarction and can potentially localize infarction territory similar to patients without ventricular pacing and suspected ACS. Development of additional diagnostic EKG criteria, similar to Sgarbossa's, could help in identifying patients with biventricular pacing in need of timely coronary interventions [3].
None of the authors have any conflict of interest or funding associated with this publication.