The acute management of broad complex tachycardias in the Emergency Department (ED) can often pose a significant challenge, not just for the more inexperienced of doctors. This is often due to the potentially lethal nature of this arrhythmia, the perceived complexity of ECG interpretation or handling of antiarrhythmic drugs. Whilst most doctors are aware that broad complex tachycardias are in the vast majority of cases related to structural abnormalities e.g. previous myocardial infarction, it is less well known that ventricular tachycardias can also occur in people with structurally normal hearts. Differentiation of the two is important as treatment is very different.
Normal heart VT, Idiopathic VT, Benign VT
About 90% of all broad complex tachycardias are of ventricular origin, this percentage increases to over 95% if there is a history of ischaemic heart disease (e.g. prior MI) or cardiomyopathy, i.e. a structural abnormality. This mere statistical fact can be used as a pre-test probability when dealing with patients presenting to the Emergency Department (ED) with broad complex tachycardias. Algorithms exist to differentiate between the causes of broad complex tachycardia, but they are often complex and not easily remembered. Heart rate or degree of hemodynamic compromise do not help differentiate between VT or SVT, contrary to common belief. Occasionally supraventricular rhythms (e.g. AV-(nodal)-re-entry-tachycardia [AV(N)RT], atrial fibrillation/flutter or atrial tachycardia) can present with broad QRS duration, if there is aberrant conduction down to the ventricles due to pre-existing or rate-related (functional) bundle branch block, or pre-excitation due to an accessory pathway. Paced rhythms or artefacts are other reasons for wide QRS complexes.
Two cases of patients presenting with broad complex tachycardias are described here:
A 31-year-old previously fit and well man presented to the emergency department (ED) with sudden onset palpitations and mild shortness of breath. This had started whilst out cycling competitively. He never had any similar symptoms before, his past medical and family histories were unremarkable, and he did not drink excessively or use illicit drugs. On examination he was apyrexial, hemodynamically stable, heart rate was 160 bpm, blood pressure 120/70. The rest of the physical examination was unremarkable. His admission ECG is shown in Figure 1, demonstrating a regular monomorphic tachycardia with a QRS duration of 118 ms, right bundle branch block morphology and left axis deviation. As per ALS guidelines he was treated with vagal manoeuvres and incremental doses of Adenosine for presumed SVT. This was unsuccessful, and the treating physician decided to arrange DC cardioversion. Whilst this was prepared, the patient reverted spontaneously to sinus rhythm.
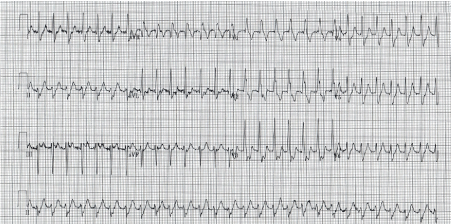 Figure 1: Fascicular VT: A regular monomorphic tachycardia with a QRS duration of 118 ms, right bundle branch block morphology and left axis deviation.
View Figure 1
Figure 1: Fascicular VT: A regular monomorphic tachycardia with a QRS duration of 118 ms, right bundle branch block morphology and left axis deviation.
View Figure 1
A 60-year-old man presented to ED with a 24-hour history of intermittent palpitations causing mild dizziness. His past medical history included "a procedure to his heart for palpitations" a few years prior, performed at a different hospital. He did not remember the exact details. In the meanwhile, he had moved to house and was lost to follow-up. On examination he appeared well, clinical examination was unremarkable. Vital signs showed a heart rate of 180 bpm, blood pressure was 100/80. His ECG is shown in Figure 2, demonstrating a regular broad complex tachycardia with inferior axis (QRS positive in leads II, III, aVF and negative in aVL) and left bundle branch block morphology. He was given 8 mmol magnesium and a bolus of 300 mg intravenous Amiodarone but required emergency DC cardioversion when his blood pressure dropped to 70/40 a few minutes into the Amiodarone infusion. Over the next 24 hours he had further non-sustained runs of broad complex tachycardia with a similar morphology.
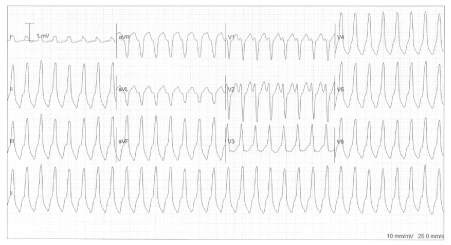 Figure 2: Right ventricular outflow tract (RVOT)-VT: A regular broad complex tachycardia with inferior axis and left bundle branch block morphology.
View Figure 2
Figure 2: Right ventricular outflow tract (RVOT)-VT: A regular broad complex tachycardia with inferior axis and left bundle branch block morphology.
View Figure 2
It is less well known that there is a subset of ventricular tachycardias that occur in people with structurally normal hearts. These arrhythmias have a benign/excellent prognosis, and are often called "idiopathic VTs", "benign VTs" or "normal heart VTs". Reports of sudden cardiac deaths are extremely rare. Treatment options include medication or catheter ablation. The two most common syndromes have been presented here, fascicular tachycardia in case 1, and right ventricular outflow tract tachycardia (RVOT-VT) in case 2.
Fascicular (ventricular) tachycardias most commonly arise from foci in the left posterior fascicle of the left bundle branch, likely due to a re-entrant circuit there. They usually occur in young males, often triggered by stress or exertion. They are often misdiagnosed as SVTs instead of VTs (as in the case presented) due to their relatively narrow QRS duration, though the right bundle branch block morphology with left axis deviation reveal their origin to be in the left posterior area of the heart. They are not responsive to Adenosine but will ordinarily respond to Verapamil. Accordingly, they are also known as "Verapamil-sensitive idiopathic left ventricular tachycardia" [1]. Patients can be maintained on calcium channel blockers, but radiofrequency ablation is possible and offers a permanent cure. The patient discussed in the above case underwent this procedure and has since been symptom free.
Right ventricular outflow tract (RVOT) tachycardias originate from cells around the RVOT [2]. Left ventricular outflow tract VT exists, but is rarer. Similar to fascicular VTs the paroxysms are often triggered by exercise, then characteristically causing bouts of sustained VT. Often symptoms like palpitations are mild and syncope or sudden cardiac death is rare. The ECG pattern characteristically is of a left bundle branch block appearance with strongly inferior axis (positive QRS in leads II, III and aVF). Commonly frequent ventricular ectopy, couplets or salvos of non-sustained ventricular tachycardias are seen. The tachycardia is characteristically sensitive to iv Adenosine, and symptoms are usually well controlled long-term with beta-blockers, calcium channel blockers or type IC antiarrhythmics (e.g. Flecainide). Ablation of the focus is a possible long-term curative option for patients that remain symptomatic. The main differential diagnosis for LBBB/inferior axis tachycardias is arrhythmogenic right ventricular cardiomyopathy/dysplasia (ARVC/D). VTs from this condition don’t usually terminate with Adenosine. Often the characteristic ECG pattern of RVOT-ventricular tachycardias are not recognized and patients are treated as per ALS guidelines with Amiodarone. The latter, apart from achieving cardioversion in only about 20% of cases in the first hour [3], often causes hypotension itself, mistaken as hemodynamical deterioration from the tachycardia and leading to (unnecessary) DC-cardioversion. In this case obtaining the patients old notes revealed that the procedure he was referring to was a prior RVOT-tachycardia ablation. His maintenance beta blockers were increased which lead to suppression of his symptoms, and he was referred for redo-ablation as an outpatient.
In summary, patients presenting with broad complex tachycardias can with over 90% certainty assumed to be in ventricular tachycardia, especially if there is a history of ischaemic heart disease/previous MI [4]. Standard ALS guidelines should be followed when treating these cases. The experienced physician should be aware though that "normal heart VTs" do in fact exist, and ideally be able to recognize and treat or refer them accordingly [5].
None declared.
None.