Extensive evidence from high-income countries has demonstrated the value of quality improvement (QI) methods yet reports of their use in LMICs are markedly limited. We aim to explore how QI can be implemented in the setting of an LMIC to remove barriers to timely antibiotic therapy for severe sepsis.
Using a mixed-methods assessment, we explored key barriers to the timely antibiotic administration for sepsis in an urban, tertiary care facility in India. This was designed as a resource-sparing exploratory investigation. We sent questionnaires to five randomly selected nurses and five randomly selected physicians working in the emergency department and tracked time point data for patients with presumed sepsis over a one-month period.
Time to antibiotics ranged in this investigation from 20 to 540 minutes (Mean: 227 minutes). A process map was drawn from these findings. Three key barriers to timely antibiotic administration were readily detected by our investigation: Delay from the admitting team antibiotic selection process, delay in family purchasing prescribed antibiotics from outside locations, and delay in the physical administration of antibiotics.
This investigation demonstrated the importance and practicality of instituting and institutionalizing QI methods in the care delivery process in resource-constrained settings. In this relatively small and low-resource assessment, key obstacles were readily detected, and furthermore without disrupting patient care. While augmented resource support and health systems strengthening are essential to improve sustainable emergency care delivery in LMICs, QI methods present a vital pathway to improve care with relatively small resource investment.
Quality improvement, Antibiotics, Sepsis, Low- and middle-income countries
The first six hours of care for severe sepsis are critical, during which each hour of delay in antibiotic treatment translates to 7.6% increase risk of a death [1]. For this reason, time-to-antibiotics treatment in the emergency department has been used as a key quality indicator in the US as well as in other high-income countries [2-4].
Sepsis, septic shock, and the end organ damage that is ultimately precipitated by severe sepsis are a substantial cause of premature mortality in low- and middle-incomes countries (LMICs) and have been shown to result in as many as one-third of deaths in children under five [5-7]. In low-resource settings, administration of antibiotics is often delayed for reasons related to inefficient delivery mechanisms and constrained resources [8,9]. A clinical audit of the Surviving Sepsis Campaign guidelines in India found that antibiotics were administered within 3 hours of ED admission in only 46.6% of cases and another study found that this was only accomplished in 62.3% of cases [10,11].
In LMICs, the clinical value of proven interventions is often limited by quality factors and the non-biologic determinants of health [12]. Quality improvement (QI) methods have demonstrated significant potential to improve the impact of these measures. However, evidence from the literature of their use in LMICs is markedly limited [13-15]. For this reason, we conducted a pragmatic quality improvement study of barriers to timely antibiotic administration in a tertiary care multi-specialty university teaching hospital in Chennai, India.
This hospital is a well-established center with 692 inpatient beds and 171 intensive care beds and has been accredited by Joint Commission International (JCI) and National Accreditation Board for Hospitals & Healthcare Providers (NABH). In this hospital, about 30% of the patients have insurance, and 70% are charged a fee for service. Patient profile characteristics indicate that 20% are from high-income families, 55% are from middle-income families, and 25% are low-income families. Out of these low-income families, 60% have insurance from the local state government for certain diseases. The emergency department is a Level I trauma center, pediatric trauma center, spinal cord injury center, stroke center and advanced cardiac care center. The ED has 40,000 annual patients' visits. There are 30 beds in the ED, with four consultants, six emergency residents, six medical officers, forty ER nurses, twenty EMTs, four administrators, and about ten ancillary staff working in the ED.
In this article, we present the results of our exploratory study, where we performed a pragmatically designed quality improvement assessment of the key factors impeding the timely administration of antibiotic treatment for sepsis. We describe the conclusions drawn from the evaluation and, in the process, demonstrate the value added even by a small-scale application of QI in an LMIC.
We designed a mixed-methods assessment to evaluate barriers to the timely antibiotic administration for sepsis in a tertiary care teaching hospital located in an urban center in India. Between September and October 2014, both qualitative and quantitative data were collected concurrently regarding the timeliness of antibiotic administration in the hospital. These results were used to determine root causes of delayed antibiotic administration.
Qualitative information was collected using a questionnaire, which was sent to key informants working in the hospital ED. A convenience sample of ten key informants were randomly selected, five of whom were emergency physicians at various levels of training, and the other five being ED nurses. Among physicians, two were female and three were male, ranging in age from 26 to 43 years. Two were residents (one first year resident and another 2nd year resident) and three were EM consultants with 5 to 8 years of experience as a consultant. Regarding the nurse respondents, all were female with ages ranging from 24 to 47 years. Experience among the nurses varied from 3 to 18 years.
The questionnaire included eight questions, both direct and open-ended (see Figure 1). The first seven questions were directed at exploring the specific processes involved in antibiotic administration in the ED while the final question asked each informant to identify three principal causes of delay in administering antibiotics. These questionnaires were completed by the key informants and then emailed to the authors. Four ED nurses dictated their answers to one of the authors (SC), who transcribed their responses.
 Figure 1: Antibiotic administration questionnaire for nurses and physicians.
View Figure 1
Figure 1: Antibiotic administration questionnaire for nurses and physicians.
View Figure 1
These responses were collected, reviewed and analyzed by the authors. The authors integrated the informants' responses to the first seven questions to construct a process map of antibiotic delivery, from the time of presentation to clinical suspicion for sepsis to antibiotic administration. We then reviewed the results and process map with the respondents for validation and feedback after its initial construction via email and then again in person. The responses to the final question regarding primary causes of delay were combined in a matrix, giving equal weight to all the responses, in order to identify the most critical barriers to timely antibiotic administration.
The care team working in the ED also recorded time data related to antibiotic administration for sepsis between September and October 2014 in a de-identified clinical log. The care team recorded timestamps for patient arrival, physician assessment, admitting consultant assessment, antibiotic administration, and disposition from the ED. This data was collected for presentations of sepsis diagnosed with systemic inflammatory response syndrome (SIRS) criteria and/or clinical suspicion with a presumed bacterial infection source (e.g. pneumonia, urinary tract infection, etc.). Time intervals from this log were tabulated and evaluated with descriptive statistics in Microsoft Excel (2010). These were then compared with the findings of the qualitative assessment, to support and quantify these results. Lastly, these findings were further triangulated by the authors' clinical experience in Indian EDs (SC) as well as EDs in other LMICs and the US (SC, LC, FG) [16].
As a project aimed at exploring the quality of routine care delivery, the Johns Hopkins Bloomberg School of Public Health Institutional Review Board office determined that this was not human subjects research and was therefore exempt from IRB review.
We received responses from all ten questionnaires distributed (n = 10). Based on our integration of the results of these questionnaires, we determined the ED process of patient presentation to antibiotic administration. An emergency physician first evaluates patients at the time of presentation. If there are signs and symptoms concerning for infection and sepsis, such as fever, hypotension, tachycardia, tachypnea, and/or altered mental status, the emergency physician will then contact the consultant or duty assistant physician from the admitting service. The admitting service consultant will then come to the ED to examine the patient and discuss potential antibiotic treatments with the ED team and the patient and attenders (i.e. patient's family, friends, spouse, etc.). Medications prescribed by hospital care teams will next be purchased by the family at the hospital pharmacy, which is adjacent to the ED, and then brought back to the care team to administer to the patient, as is common practice in many LMICs. According to two respondents, the physical process of going to the pharmacy, waiting in line, and purchasing the medication can take up to 30 minutes. The attenders and patient will typically spend some time deliberating over whether purchasing the medication is financially feasible as well. Finally, after the attenders return with the antibiotics, the nurse will administer a small test dose of the antibiotic. After waiting approximately 30 minutes to ensure that there is no allergic response, the nurse will then administer the full dose. The process map constructed from these data is outlined in Figure 2.
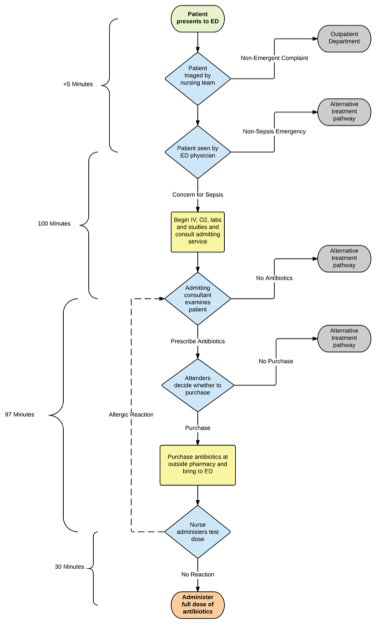 Figure 2: Process map of antibiotic administration with average time intervals.
View Figure 2
Figure 2: Process map of antibiotic administration with average time intervals.
View Figure 2
During the brief one-month assessment period, the ED care team recorded time data from eight presentations for presumed sepsis (n = 8). According to the time stamp data, there was an average of 227 minutes from the time of patient arrival to the administration of antibiotics (Range 20 to 540 minutes). The longest time intervals were between the ED physician examination and the admitting service consultant seeing the patient, 100 minutes (Range: 50 to 190 minutes), prescription of the antibiotics and administration of the test dose, 97 minutes (Range: 10 to 200 minutes), and administration of the test dose and the final administration of the full dose, 30 minutes (Range: 0 to 30 minutes) (see Table 1 and Figure 2).
Table 1: Length of time intervals between presentation and antibiotic administration. View Table 1
In the final question of the questionnaire, the respondents identified nine different obstacles to antibiotic administration (see Table 2 and Figure 3). All but one respondent listed waiting for the patient to be seen by the admitting service consultant to administer antibiotics as a significant source of delay in antibiotic administration. Four out of five nurses also cited the shortage of nursing staff in the ED as an impediment to timely administration, but only one physician mentioned this. A majority of the respondents identified patient- and attender-related factors as key barriers, in particular, the length of time taken for the attenders to decide to purchase the prescribed antibiotics and the physical process of purchasing and returning the medication.
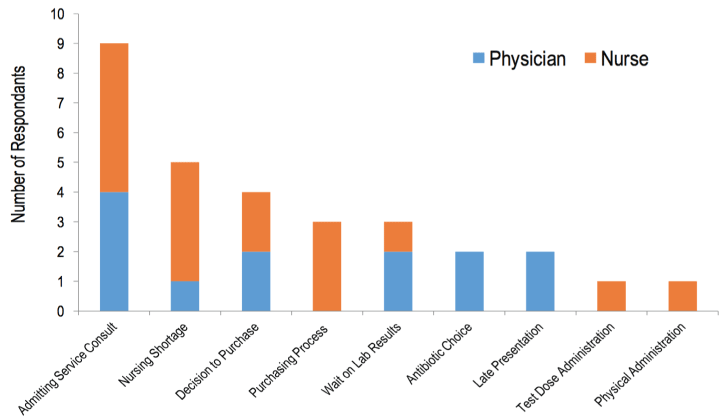 Figure 3: Total responses for each physician- and nurse-identified sources of delay in antibiotic administration.
View Figure 3
Figure 3: Total responses for each physician- and nurse-identified sources of delay in antibiotic administration.
View Figure 3
Table 2: Physician and nurse-identified sources of delay in antibiotic administration. View Table 2
Our mixed-methods quality improvement assessment revealed three key barriers to timely administration of antibiotics for sepsis: Delay to examination by the admitting team, delay in attenders purchasing and returning with prescribed antibiotics, and delay in the physical administration, including waiting for test dose results - in essence, a three delay model requiring specific interventions with each team member and administration. The delay in attenders purchasing the antibiotics was highlighted by a majority of the respondents. The delay was further divided into two categories - delay in the decision to purchase the antibiotics after considering financial constraints and the delay in the physical purchasing. While this was perceived as a major area of concern for both physicians and nurses, two of the nurses reported that the purchasing process took less than thirty minutes on average. Although this could potentially be explored in future evaluations, our quantitative assessment did not specifically address this, and it is unclear how the 97 minutes between prescription of the antibiotics and the administration of the test dose was divided. However, the most significant delay was due to waiting for the admitting team to examine the patient, causing a mean of 100 minutes delay and as much as 190 minutes in one case.
The QI team related these findings back to the ED nurses, physicians and administration. The QI team recommended that the test dose administration process be re-evaluated, particularly for extreme, life-threatening conditions such as severe sepsis. Our findings also suggested that the processes around joint prescription of antibiotics by the admitting service and ED team should be reevaluated as well, with ED providers selecting and prescribing the first dose of antibiotics or developing guidelines for broad spectrum antibiotics for presumed severe and life-threatening conditions. These concepts could be further explored in assessments of how clinicians communicate, and how training, clinical guidelines and supervisor direction may impact this element. Our review also identified discrepancies among physicians responding to the questionnaire as to whether one must wait for lab results before deciding to administer antibiotics. The team, therefore, recommended the development and use of guidelines and job aids for the approach to sepsis in the ED. Lastly, the QI team recommended a more extensive, long-term auditing process to document and follow time to antibiotics while implementing these changes in order to assess improvement and promote continuous quality improvement.
Although the results of this case study are not generalizable beyond this context, the conclusions may very well mirror those seen in other LMICs. For example, the common practice of patient attenders purchasing medications outside of the ED presents a major obstacle to timely antibiotic administration and for emergency care in general [17-19]. While this practice has been built into the care delivery practice in many resource-constrained settings, patient outcomes could potentially be improved by streamlining medication delivery for time-sensitive disease entities such as sepsis, acute coronary syndrome, and acute asthma exacerbation. Similarly, we found that better integration of emergency systems within overall hospital processes stands to streamline and expedite care. As a relatively young specialty, particularly in India and other LMICs, emergency care has yet to be fully developed and leveraged within healthcare delivery systems [20]. Delivering timely treatment to patients with a time-sensitive disease such as a septic shock is the core objective of emergency care and, as such, quality and process improvement will be essential to capitalizing on the field's potential for value creation in the future [21].
Most importantly, this exploratory study demonstrated the importance and practicality of instituting and institutionalizing QI methods in the care delivery process in resource-limited settings. In this relatively small and low-resource assessment, key obstacles were readily detected, and furthermore without disrupting patient care. Quality improvement has been applied to a wide array of disciplines since its conception in the manufacturing industry in the early 1920's [22]. In healthcare, QI has made substantial cost-saving impacts on outputs and outcomes related to infection control, hospital operations, and reducing surgical complications [23-25]. While the barriers and process failures related to service delivery in LMICs often mirror those in high-income settings, these obstacles are compounded by critical resource constraints in LMICs [3,26,27]. QI has significant potential for strengthening service delivery and health systems in LMICs and, as such, stands to be expanded upon in both large scale and modest studies such as this [28,29].
As a pragmatically designed QI investigation, this exploratory study included only ten key informants and followed only eight severe sepsis cases during the study period. Formal assessments of care procedures for sepsis would require a larger number of patients and respondents as well as a collecting data over a longer period of time to account for variability in case load and seasonal variation. While multiple perspectives were included in this evaluation, additional perspectives, such as that of pharmacists, patients, and admitting services, could also be included in future studies. While this pragmatic study design represents a significant limitation in regard to the statistical power of our findings, this did not preclude the development of robust conclusions regarding key barriers to timely antibiotic care. This potential limitation, rather, suggests the critical value of these applying such methods in resource-limited settings, as they have the potential to serve as a resource-sparing avenue to significantly increase the quality and effectiveness of proven interventions.
Sepsis is well-characterized disease entity, and the impact of early antibiotics has been repeatedly proven in high-income settings as well as in LMICS [30]. While augmented resource support and health systems strengthening are essential to improve sustainable emergency care delivery in low- and middle-income countries, QI methods represent a vital pathway to improve care with relatively small resource investment. The continued promotion of quality improvement in LMICs is critical to the development of robust health systems and emergency care systems in particular worldwide.
Blair Smart, Tashrik Ahmed and Isabella Ciuffetelli for their contribution to the study.
None declared.
None.