Objective: Comparison of the SOFA score with a newly developed "triage score" and evaluation of the consequences of simulated triage of ICU patients on the outcome.
Methods: Retrospective explorative data analysis of 213 patients treated on Intensive Care Units of community hospitals in Western Austria during the first and second wave of the COVID-19 pandemic.
Results: AUROC curve values of the new triage score ranged from 0.73 to 0.85 depending on the time point of the assessment. Simulated triage resulted in exclusion of up to 11% of patients with favourable outcome dependent on the threshold value for initiation or continuation of critical care of the particular score used. Successive exclusion of patients with the highest scores results in withdrawal of therapy in 10% of survivors when more than 25% of all patients are selected for discontinuation of treatment.
Conclusions: The new triage score has better prognostic significance than the SOFA score alone and can serve as a basis for prioritisation decisions. The influence on the outcome is reflected by the level of the cut-off-value of the applied score and the amount of patients refused.
AUROC: area under the receiver operating characteristic; CPC: Cerebral Performance Category; GCS: Glasgow Coma Scale; ICU: Intensive Care Unit; SOFA: Sequential Organ Failure Assessment; TS: triage score
Prioritisation, Triage, Resource deficiency, Scoring systems, Decision making
When the COVID-19 pandemic reached the European continent, hospitals in many regions were overwhelmed by the massive influx of patients and no more capable to treat every patient admitted, especially those in critical condition [1-3]. To cope with the expected shortage of intensive care resources - besides measures to increase surge capacity - a protocol for the allocation of critical care was developed and implemented in five general hospitals in Western Austria. One element of this protocol is the assignment of a newly created triage score for every patient in the Emergency Departments (upon admission) and in the Intensive Care Units (ICUs) at fixed time points in case of impending shortage. The latter is defined as 70% saturation of all available intensive care resources. The score serves to allocate the supply on a ranking order, with first priority for patients with the lowest scores, representing those the highest probability for survival. With the objective to evaluate this score in regard of its prognostic significance and to examine the potential influence on the outcome of the patients undergoing the allocation process, a study was conducted testing its effects within a simulated triage of critically ill patients.
The study was designed as a retrospective explorative data analysis. The evaluation was performed a posteriori on critically ill patients treated during the first and the second wave of the pandemic. The study population consisted of adult patients treated on Intensive Care Units of five community hospitals in a region with approximately 450.000 inhabitants over two time periods: from March 15th until May 15th 2020 and from November 1st 2020 until January 31st 2021. Inclusion criterion was admission with any condition (injury or disease) requiring intensive care. Both COVID-19 positive and negative patients were included. Exclusion criteria were presence of a patient's provision excluding critical care or a futile prognosis of the underlying disease.
For every patient included, the SOFA score (Sequential Organ Failure Assessment) was calculated at four time points: On admission, after 24h, 48h, and 120h of treatment on the ICU. For patients treated longer than five days, a final score was calculated on the day of discharge from the ICU (= time point last). The newly developed triage score (TS) was assigned for each patient at the same time points. The factors accounting for the TS are age, severe comorbidities and the SOFA score (Table 1). For survivors, neurological outcome was evaluated when the patient was discharged from the ICU using the Cerebral Performance Category (CPC).
Table 1: Calculation matrix of the triage score in the allocation protocol. View Table 1
Triage simulation was performed by two different approaches. First, the effect on the outcome by exclusion of patients on the basis of a specific cut-of-value for the SOFA score respectively the TS was evaluated. The objective was to define a value which separates the patients with good outcome from those with adverse ones.
Second, the effect on the outcome by exclusion of patients on the basis of the highest (not numerically specified) scores was evaluated. Resource deficiency was simulated by successively excluding patients beginning with the highest and proceeding with lower scores. The executive board of the region's hospitals gave its consent to the study. The Institutional Review Board of the region's government (Ethikkommission Land Vorarlberg) waived the need for informed consent (IRB no.: EK-0.04-365).
During the two study periods, a total of 213 patients were included, 16 patients had to be excluded due to missing outcome data. Data of 197 patients remained for final analysis. Of these patients, 129 could be analyzed after 120h; 68 were discharged or died before.
The prognostic significance of the triage score was dependent on the time point of the assessment: the area under the ROC-curve (receiver operating characteristic) increased from 0.73 on admission to 0.85 at time point last. The correspondent values for the SOFA score were 0.61 and 0.82.
Triage simulation, approach 1: When triage was performed on the basis of a predefined threshold value for the triage score, 11/99 patients (11.1%) with a favourable outcome were excluded from ICU treatment on admission when setting the limit at six points. One patient (1%) was excluded when setting this limit equal to eight. A threshold of six was chosen, because in an interim analysis worse outcomes in patients with a TS of six or above were observed.
When triage was performed on the basis of a SOFA score's threshold value, 6/99 patients (approx. 6%) with a favourable outcome were excluded from ICU treatment when setting the limit for admission at 11 points, one at SOFA=13. Triage of patients after 120h stay on ICU resulted in withdrawal of therapy in none of the patients with favourable outcome, when setting the limit for continuation of treatment at a TS equal to six and in one patient using a SOFA score of 11. A SOFA score of 11 was also suggested in other recommendations for the prioritisation of ICU patients [4,5]. However, it has been recently shown that the SOFA score alone has insufficient discriminant accuracy when used for triage in ventilated COVID-19 patients [6].
Triage simulation, approach 2: with triage on the basis of the available ICU capacity, those patients having the highest TS will not be admitted or will be discharged from ICU with the objective to preserve the resources. Applying this strategy, 10% of survivors would have been excluded after sorting of 50 patients, which corresponds to 25.3% of the study population. Since this rate is independent of the time point, when using the TS, there is no difference if the prioritisation is made on admission or at any time during the stay on the ICU. In other words, when the resources are sufficient to accommodate 75% of all patients requiring critical care, the allocation according to the protocol results in refusal of maximum 10% of surviving patients. The question, if this number is acceptable (even in a public health disaster) may be subject of further discussion and cannot be answered by the study. Exclusion of the patients with the highest SOFA scores results earlier in exclusion of 10% of survivors, namely after sorting of 35 patients (17.7%) upon admission and 45 patients (22.8%) after 120h on ICU, respectively.
Several limitations of the study have to be noted. First, a higher sample size may have produced more reliable results. However, the results are more influenced by the heterogenity of the studied patients, which reflects the reality. Second, although the application of the SOFA and the triage score relies on clearly defined parameters, errors in calculating the score cannot be excluded in every case. Third, the neurological outcome has been determined, when the patient was discharged from the Intensive Care Unit. Of course, this assessment may differ several weeks or months later. Fourth, the study has been conducted in a sparsely populated region with relatively high standard of medical care and existing surge capacity. Comparability with other countries - especially in dense populated regions outside Western Europe - is therefore limited.
In the light of the findings, it would be most fair to first offer intensive care to every patient needing it, and only to exclude patients from further treatment after a given period of time, since both scores are more robust at later time points after admission. Nevertheless, the precondition for this strategy is a reserve of resources. On the other hand, the level of the cut-of-value can be adjusted according to the saturation of the capacities. A start at a level of eight for the TS (and 13 for the SOFA score) might be reasonable, with lowering this level to six (resp. 11) when there is an impending exhaustion of resources, since the outcome with a TS of eight or higher is poor (Figure 1 and Figure 2).
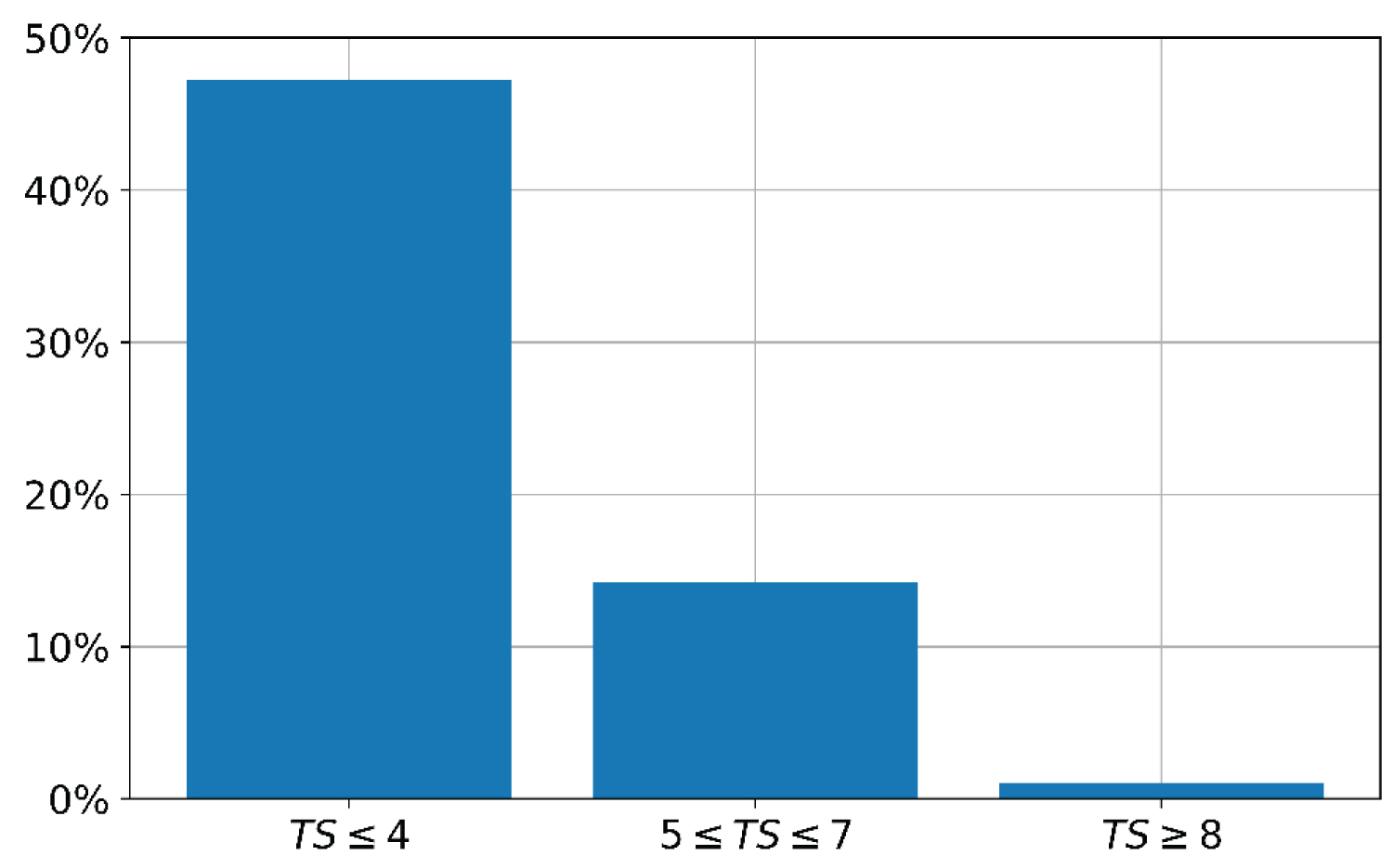 Figure 1: Proportion of surviving patients according to the triagescore upon admission. View Figure 1
Figure 1: Proportion of surviving patients according to the triagescore upon admission. View Figure 1
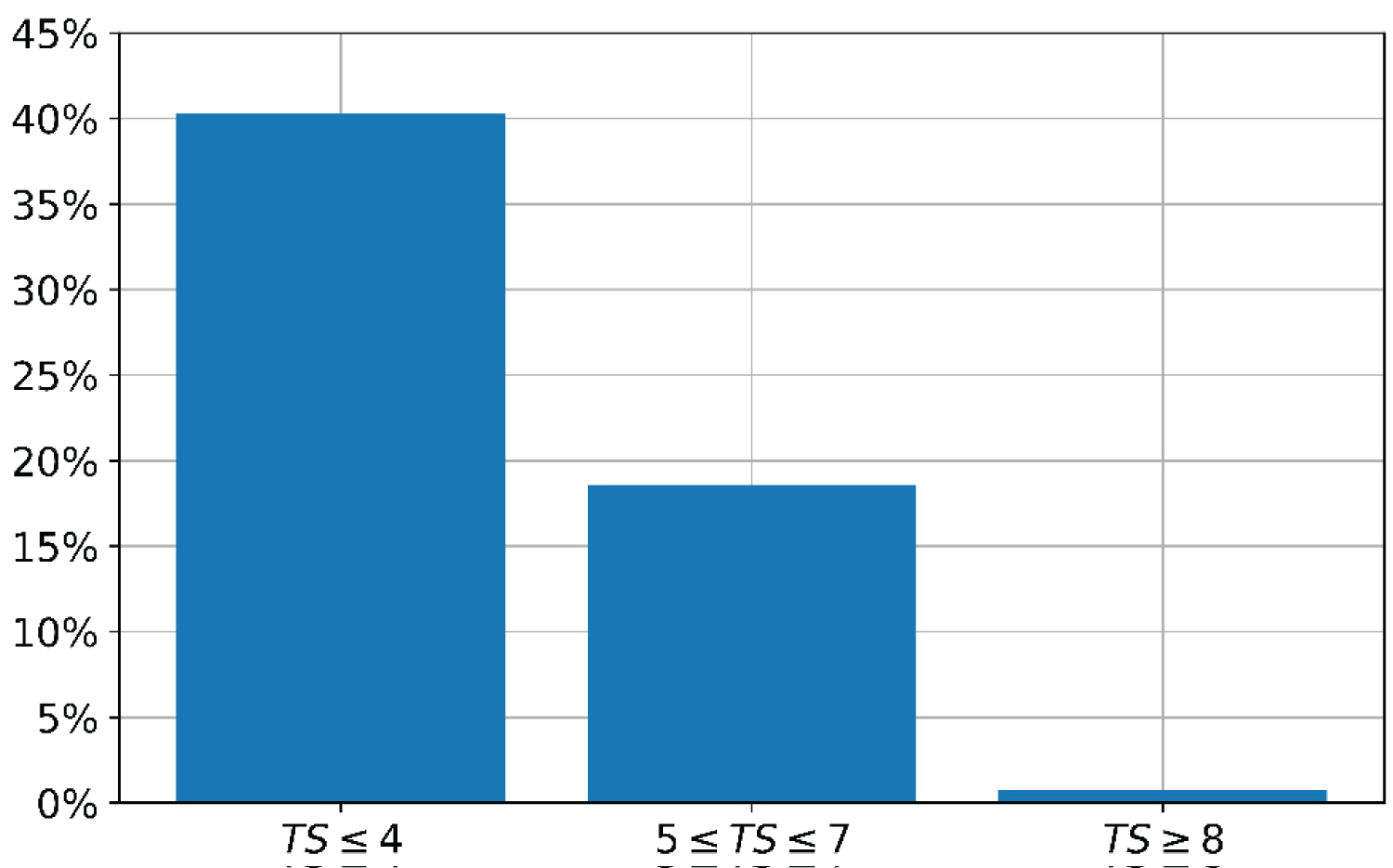 Figure 2: Proportion of surviving patients according to the triagescore at 120h. View Figure 2
Figure 2: Proportion of surviving patients according to the triagescore at 120h. View Figure 2
In the study population, setting the level at eight points for the TS, resulted in one lost patient overall, but also in only eight additional vacant beds, compared with 35 beds with a cut-of-value of six points. Another option is to set two different cut-of-values: One for patients on admission and a lower one for those on the ICU, giving more patients the chance for initiation of advanced therapy.
When prioritisation is made by exclusion of patients with the highest scores (without defining a cut-of-value), the extent of the influence on the outcome is depending on the degree of the shortage and, thereby, the amount of rejected patients: in the study, simulated exclusion of up to one fourth of all patients led to a rejection of maximum 10% of patients who survived in real life (regardless of their performance, since this may improve over time). This finding can be extrapolated to settings with variable capacities: when triage on the basis of the highest scores is initiated, a slight effect on the outcome (exclusion of less than 10% of surviving patients) has to be anticipated while the capacity is sufficient for a minimum of 75% of the population in need. The question, whether the limit of 10% is tolerable may be subject of further discussion and cannot be answered by the study. Anyway, a further decrease of the resources will result in an unjustifiable loss of patients. The integration of other factors, like milder comorbidities and frailty, in the calculation of the TS may improve the prognostic accuracy and will be considered in a revised version of the allocation protocol [7,8].
In conclusion, the newly developed triage score correlates well with the clinical outcome and has better prognostic significance than the SOFA score alone. Therefore, it may serve as a basis for prioritisation decisions. Simulated triage influences the outcome especially when lower thresholds values are used, or larger amounts of patients are excluded for therapy. The assessment of ICU patients should be made after a predefined time period of at least 120 hours.
Each author contributed equally to this manuscript.
None declared.
None.