Freiberg's infraction is characterized by pain in the forefoot caused by osteonecrosis, and most commonly found in adolescent females. I present here a case report of a 78-year-old female with Freiberg's infraction of the second metatarsal head in order to focus on a rare cause of foot pain among geriatric patients and its management.
Freiberg's infraction, Freiberg's disease, Osteonecrosis, Avascular necrosis, Foot pain, Geriatrics, Elderly
Foot pain is debilitating and common, especially in the geriatric population. It causes difficulty, or an inability, to ambulate which may lead to further issues such as weight gain, reliance on others for assistance, and imbalance which can lead to falls. It is important to consider Freiberg's infraction as a cause of foot pain in the elderly, even if it normally occurs in younger patients. Freiberg's infraction (also known as Freiberg's disease) is premature bone death, or osteonecrosis, of most commonly the head of the second metatarsal bone in the foot, occurring most commonly the in second decade of life [1]. I present a case of a 78-year-old female with Freiberg's infraction and discuss its impact on the geriatric population. While most articles researched showed the mean ages during adolescence and early adulthood, interestingly, a study by Helix-Giordanino, et al. had a mean age of thirty patients with Freiberg's infraction of 61 years. That article does not focus on the advanced age of the group and its impact, rather it concludes that a dorsal closing wedge osteotomy is the best way to surgically treat it [2].
A 78-year-old thin active healthy female presented to my office for severe pain located in her left foot, 2nd metatarsal phalangeal (MTP) joint. It was present for a few months duration, without any history of trauma. Conservative treatments such as non-steroidal anti-inflammatories, changes in shoe gear, and rest were attempted prior to coming into the office. Radiographs taken revealed a focal area of osteopenia, and a long second metatarsal (Figure 1). The patient was subsequently referred for an MRI which confirmed osteonecrosis of the second metatarsal head with subchondral edema, destruction and flattening of the dorsal aspect head of the second metatarsal, otherwise known as Freiberg's infraction (Figure 2 and Figure 3). After discussing the risks, benefits, and alternatives with the patient and her family, it was decided to proceed with surgical intervention.
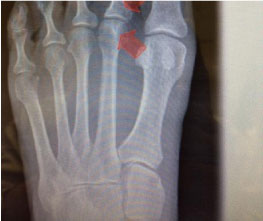 Figure 1: X-ray revealing focal area of osteopenia and long second metatarsal.
View Figure 1
Figure 1: X-ray revealing focal area of osteopenia and long second metatarsal.
View Figure 1
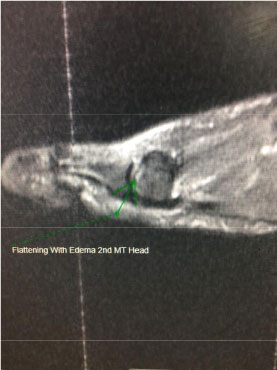 Figure 2: Sagittal view of a T2-weighted MRI image showing edema and flattening of the dorsal aspect of the second metatarsal head.
View Figure 2
Figure 2: Sagittal view of a T2-weighted MRI image showing edema and flattening of the dorsal aspect of the second metatarsal head.
View Figure 2
 Figure 3: Axial view of a T1-weighted MRI image showing destruction of the second metatarsal head.
View Figure 3
Figure 3: Axial view of a T1-weighted MRI image showing destruction of the second metatarsal head.
View Figure 3
The patient was taken to the operating room for an intraarticular dorsiflexory wedge osteotomy, to remove the areas of necrosis, and allow the plantar cartilage be rotated dorsally for proper joint articulation and movement. A curvilinear incision was made centered over left second MTP joint to allow for decreased scar tension. Using sharp and blunt dissection with care taken to protect all neurovascular structures, the extensor tendon was retracted, and the second MTP joint was exposed. Upon examination of the head of the 2nd metatarsal (Figure 4), the dorsal cartilage was noted to be denuded, with a significant amount of bone exposed where cartilage was supposed to be. At this point, a dorsal wedge osteotomy was made intraarticularly, with the apex pointed plantar proximal toward the neck of the metatarsal and a larger fragment dorsal distal in a triangular shape, and removed from the foot. The marrow in the wedge of bone that was removed was noted to be white instead of red, which denotes an avascular region (Figure 5). The plantar cartilage was then rotated dorsally and two screws for fixation were placed to prevent rotation of the metatarsal head (Figure 6 and Figure 7). The soft tissue and then skin were closed in layered fashion. The removed bone was sent to a pathologist who confirmed histologically the presence of Freiberg's infraction. The patient had no postoperative complications, and has no pain at the site two years post-operatively (Figure 8).
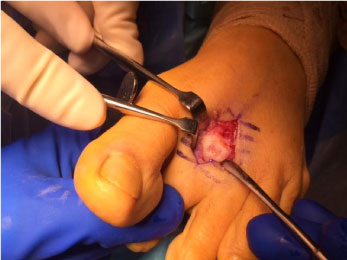 Figure 4: Head of the 2nd metatarsal dorsal aspect devoid of cartilage centrally.
View Figure 4
Figure 4: Head of the 2nd metatarsal dorsal aspect devoid of cartilage centrally.
View Figure 4
 Figure 5: Wedge of bone that was removed was noted to be white in the marrow, instead of red.
View Figure 5
Figure 5: Wedge of bone that was removed was noted to be white in the marrow, instead of red.
View Figure 5
 Figure 6: AP X-ray revealing placement of the two screws.
View Figure 6
Figure 6: AP X-ray revealing placement of the two screws.
View Figure 6
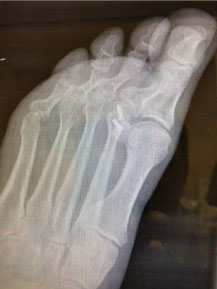 Figure 7: Oblique X-ray revealing placement of the two screws.
View Figure 7
Figure 7: Oblique X-ray revealing placement of the two screws.
View Figure 7
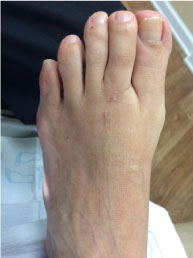 Figure 8: Clinical image of foot two years post-surgery.
View Figure 8
Figure 8: Clinical image of foot two years post-surgery.
View Figure 8
Freiberg's infraction was originally described by Dr. Freiberg in 1914, who attributed it to ischemic necrosis caused by multiple micro-traumas to the second metatarsal head. Gauthier and Elbaz later said that it was a result of subchondral fatigue fracture from excess pressure [3,4]. Other etiologies associated with Freiberg's infraction are direct trauma, arthritis, a long second metatarsal, a short first metatarsal, and hallux limitus. Viladot states that it is caused by arterial spasm [5]. It is more common in young age, females, and obese patients [6-9]. In 1959, Braddock experimented using weights dropped from various heights on cadavers feet of various ages, and noted a weakness of the epiphysis of the second metatarsal that is vulnerable to fracture, or Freiberg's infraction. These fractures occurred prior to epiphyseal maturation, i.e., during adolescence [8]. Alternatively, some suggest that wearing high heels is a cause for it to be most common in younger females [9]. It is uncommon for the individuals in the geriatric population to develop Freiberg's infraction, possibly due to the aforementioned, and from putting less stress on their feet with decreased ambulation.
In Freiberg's infraction, the joint tends to get destroyed by fragmentation of the joint, loss of cartilage, joint collapse, and flattening. Radiographic imaging may reveal a hyperemic response and seen as focal osteopenia, with later stage flattening of the metatarsal head. Magnetic resonance may show earlier signs than radiographs, including bone marrow edema in the area and arthritic changes [10]. Symptoms include unilateral forefoot pain which is increased on range of motion of the joint and on ambulation, joint stiffness, and edema. Common differential diagnoses include plantar plate ligament injury, stress fracture, capsulitis, arthritis, and neuromas.
Conservative treatments such as changes in shoe gear, non steroidal anti-inflammatories, foot orthosis offloading or limiting motion in the second metatarsal-phalangeal joint (MTPJ), and physical therapy may be initiated. Lin, et al. recommends conservative treatments for most patients as he believes that the disease is self limiting. He presents a 16-year-old female with Freiberg's infraction that was treated with rest and activity modification who was walking pain-free after two months, though there was no long term follow up [11]. Palamarchuk and Oehrlein also recommend conservative care for most patients. They bring a case report of a 20-year-old female collegiate heptathlete and dispensed a custom orthosis which relieved her pain and allowed her to compete in competitions. But, after one year, radiographs taken revealed that her Freiberg's infraction had progressed and she agreed to discuss further conservative treatments and surgical options [12]. In my opinion, when treating a patient conservatively, the patient should be informed that although conservative treatments can be tried first and may resolve the symptoms, that only surgical management can remove any loose bone fragments, clean the joint, and remove areas that are nonvascular to prevent further breakdown, and form a functional joint.
Surgical treatments may consist of joint replacement, debridement, resection of metatarsal head, bone grafting, modified Weil osteotomy with microfracturing by subchondral drilling, osteochondral autologous transplantation, and dorsal wedge osteotomies. The microfracturing technique works by bringing new blood flow from behind the subchondral plate, and cells to the area to create new cartilage. In patients with Freiberg's, where there is damage to the blood supply around the head of the metatarsal, this likely will not be successful. Biz, in 2017, presented an extraarticular dorsal wedge osteotomy at the metatarsal neck on a 31-year-old female with 8 months of unresolved pain after conservative treatments was diagnosed with Freiberg's which healed uneventfully [13]. Interestingly, in that case, the surgeons state that due to the lack of knowledge and low frequency of the disease, the infraction was not diagnosed. In a study by Ozkul, comparing resection of the metatarsal heads and extraarticular dorsal closing wedge osteotomies, significant pain relief was achieved in both groups, but there was significantly more shortening in the excision group [14]. In 2016, Lee, et al. recommends a combined Weil and closing wedge osteotomy which gave a group of 15 patients increased range of motion, and improved metatarsal length. Lee, et al. appears against dorsiflexory wedge osteotomies as he states that the fixation needs to be removed [15]. I normally don't penetrate the distal cortex with my screw across osteotomy and never needed to remove any fixation in this procedure. If the screw penetrates the distal cortex, then it would be painful and need to be removed due to the metatarsal head being a weight bearing surface. In 2013, Erdil, et al. recommended joint debridement and remodeling combined with an extensor tenoplasty when additional contracture was noted. His patients had a mean age of 27 [16]. Although the one year follow up showed good results with pain scores, I highly doubt long term success of this procedure when there is raw bone devoid of cartilage on the head on the 2nd metatarsal constantly scraping against the cartilage on the base of the 2nd proximal phalanx.
If a geriatric patient is not active, or has poor circulation, I would not recommend to perform this procedure. There are often more co-morbidities associated with patients in the geriatric population such as diabetes, high blood pressure, and surgical risks which are often not encountered in adolescence. Risks of surgical management includes infection, floating toe, transfer metatarsalgia, further surgery, nerve damage, non union, more pain, swelling, etc. Although there may be situations in which alternative surgeries are indicated, my preference for treating Freiberg's infraction is creating an intra-articular dorsiflexory osteotomy which has produced reproducible positive results as seen in this case.
In our case, a long second metatarsal was noted which may have contributed to increased pressure on the metatarsal-phalangeal (MTP) joint, and subsequent Freiberg's infraction. Although the patient only became symptomatic several months prior to her first office visit, it is difficult to know if this destructive process started years prior as we do not have any prior imaging studies for comparison. As this patient failed conservative treatments, was very active and had adequate circulation, I performed a surgical management and she was able to return to her prior state of function with no pain.
None.
The author reports no conflict of interest for this case report.
The patient gave written consent to publish her all details related to her case including pictures.