Foot restoration after massive bone and soft tissue loss is a daunting task for surgeons. Existing literature has highlighted various methods of reconstruction. Masquelet technique, use of vascularised and non-vascularized fibular grafts, use of latissimus dorsi, serratus anterior in combination with rib grafts, iliac crest grafts have been described. There is, however, no report in the literature demonstrating use of rib bone grafts as a delayed reconstruction option. In our case, we performed a 2-stage procedure, first using a free gracilis flap for soft tissue coverage and then, weeks later, the second stage was undertaken where the rib was harvested and used as a bone graft in the metatarsals. There was low morbidity with this approach as highlighted by the speedy recovery and minimal analgesic requirement. We avoided the potential complications of scapula winging and pleural fibrosis associated with latissimus dorsi and serratus anterior grafts.
Bone loss, Soft tissue defect, Delayed reconstruction, Rib graft, Gracilis flap, Metatarsal fractures
ATLS: Advance Trauma Life Support
Complex and multiple metatarsal fractures in the same foot present a challenge to the orthopaedic team especially when there is segmental bone loss [1,2]. Much as amputation remains a reasonable option in these injuries, a salvage procedure where feasible is the preferred option. A number of methods have been described in the literature to manage traumatic segmental bone loss, both in long bones and also in the foot. The techniques include use of iliac crest bone graft [3], vascularised and non-vascularised fibular graft [4,5], and the Masquelet technique [6]. There are limited reports in the literature of using rib osteomyocutaneous flaps to manage traumatic bone defects [7-11]. We report a case of a complex open fracture leading to significant metatarsal bone loss that we managed successfully with delayed rib bone graft after soft tissue coverage with a gracilis free flap.
A 25-year-old soldier was involved in a blast and suffered multiple superficial and deep soft tissue injuries. His main osseous injuries were in his left foot, where he suffered fractures of his second, third, fourth and fifth metatarsals. These metatarsal injuries were open fractures with segmental bone loss and soft tissue loss with significant contamination (Figure 1 and Figure 2). He also had a large soft tissue defect from damage to his calf complex with no involvement of the neurovascular structures on the unilateral side (Figure 3). He was initially managed as per ATLS principles ensuring physiological stability. He then went on to have acute debridement of the multiple soft tissue injuries planned in conjunction with the plastic surgery team.
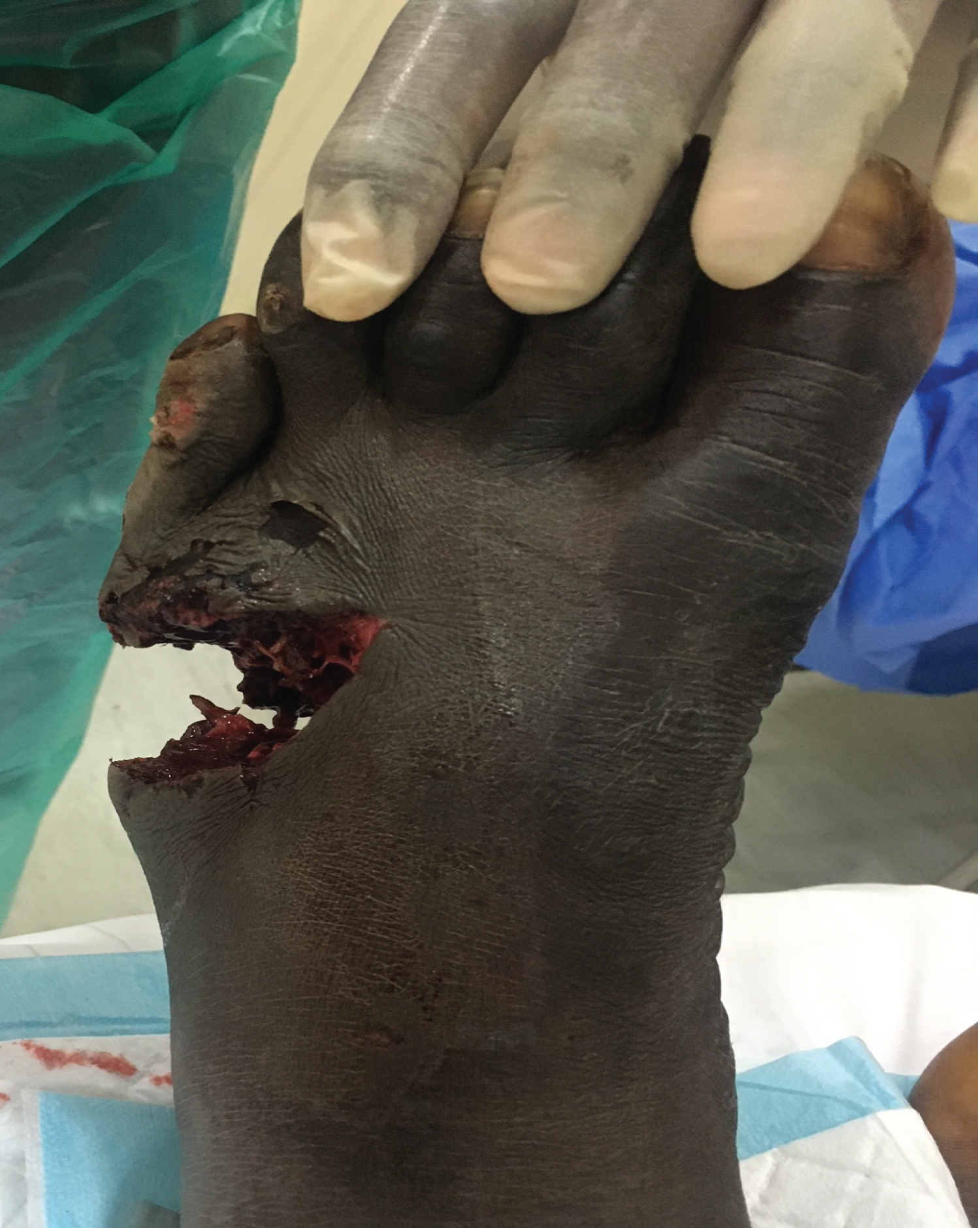 Figure 1: Soft tissue loss with contamination. View Figure 1
Figure 1: Soft tissue loss with contamination. View Figure 1
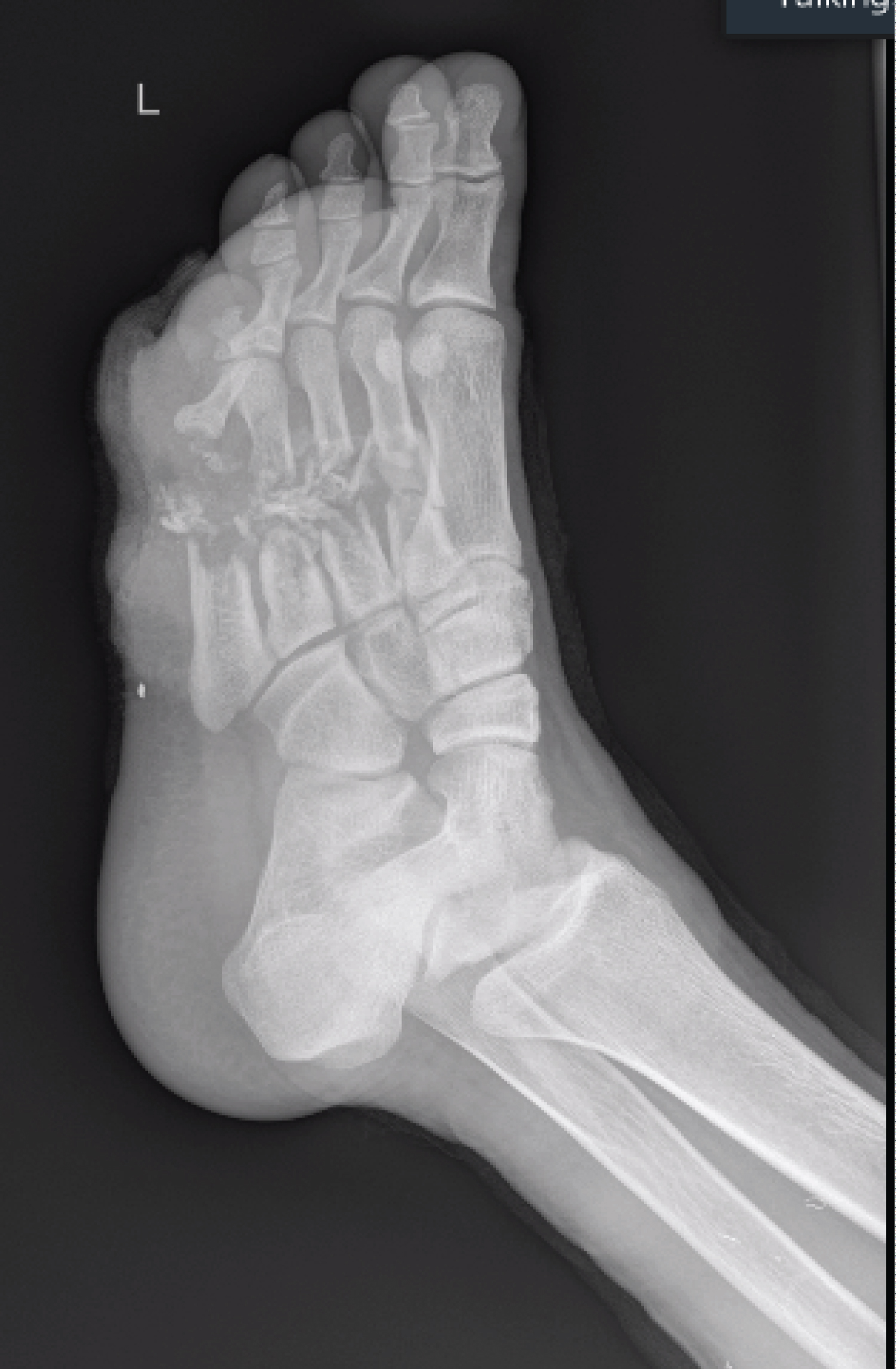 Figure 2: Radiograph shows segmental bone loss. View Figure 2
Figure 2: Radiograph shows segmental bone loss. View Figure 2
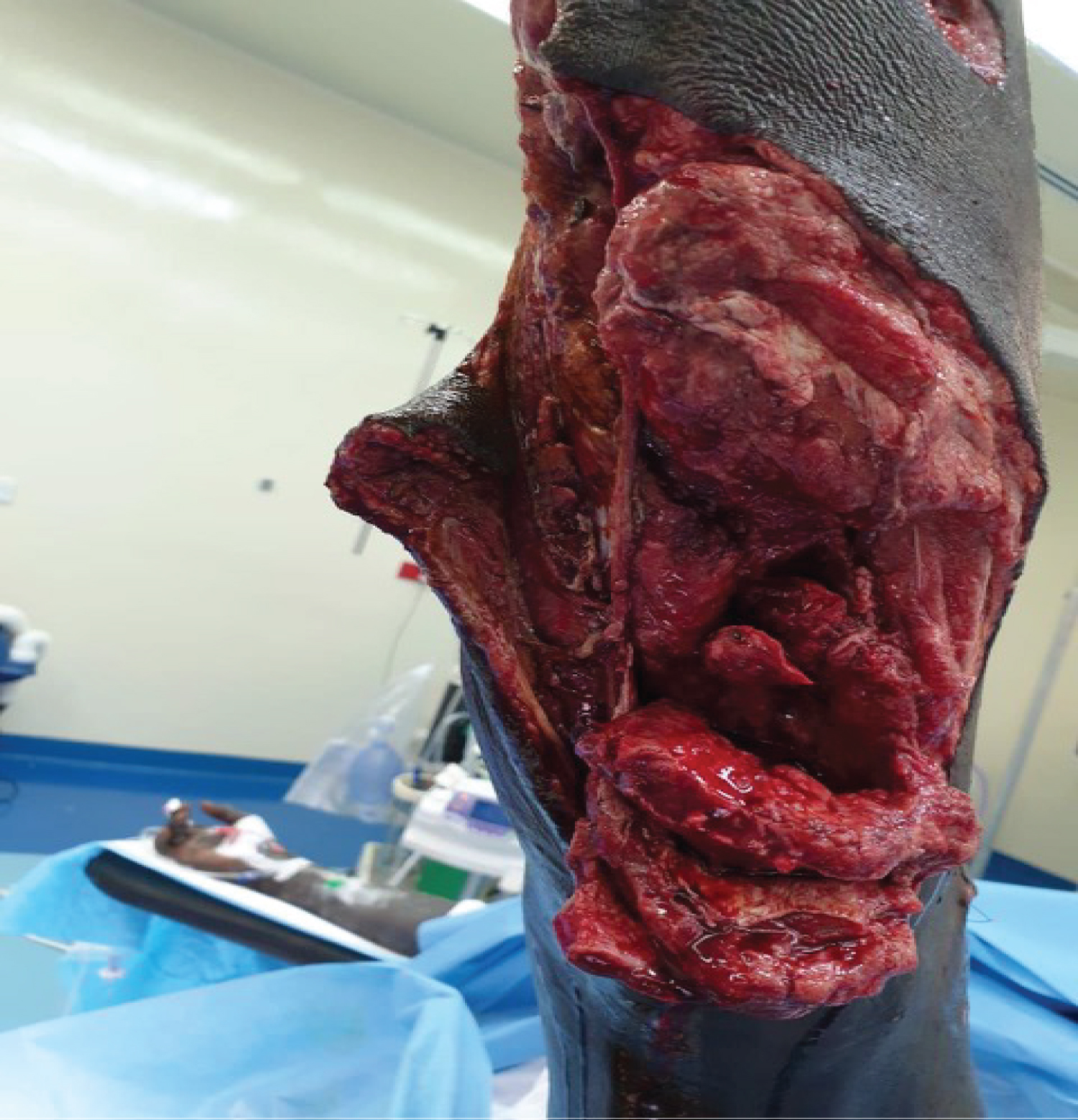 Figure 3: Soft tissue defect on the calf. View Figure 3
Figure 3: Soft tissue defect on the calf. View Figure 3
In his left foot, he underwent multiple episodes of soft tissue and bone debridement to reduce the contamination, resulting in a significant soft tissue defect and further bone loss. He had serial vacuum assisted dressings to aid wound healing and to manage contamination. He remained on intravenous antibiotic cover during this debridement phase. The contamination was controlled after three wound washouts in theatre. Six days following the injury, he went on to have a vascularised gracilis free flap pedicled on the dorsalis pedis artery.
The free flap got infected for which multiple debridements were performed to salvage the graft. The graft eventually healed well. There was partial regeneration of his second metatarsal bone on X-rays taken ten weeks post-injury (Figure 4), however, no similar activity was observed in the third, fourth and fifth metatarsals.
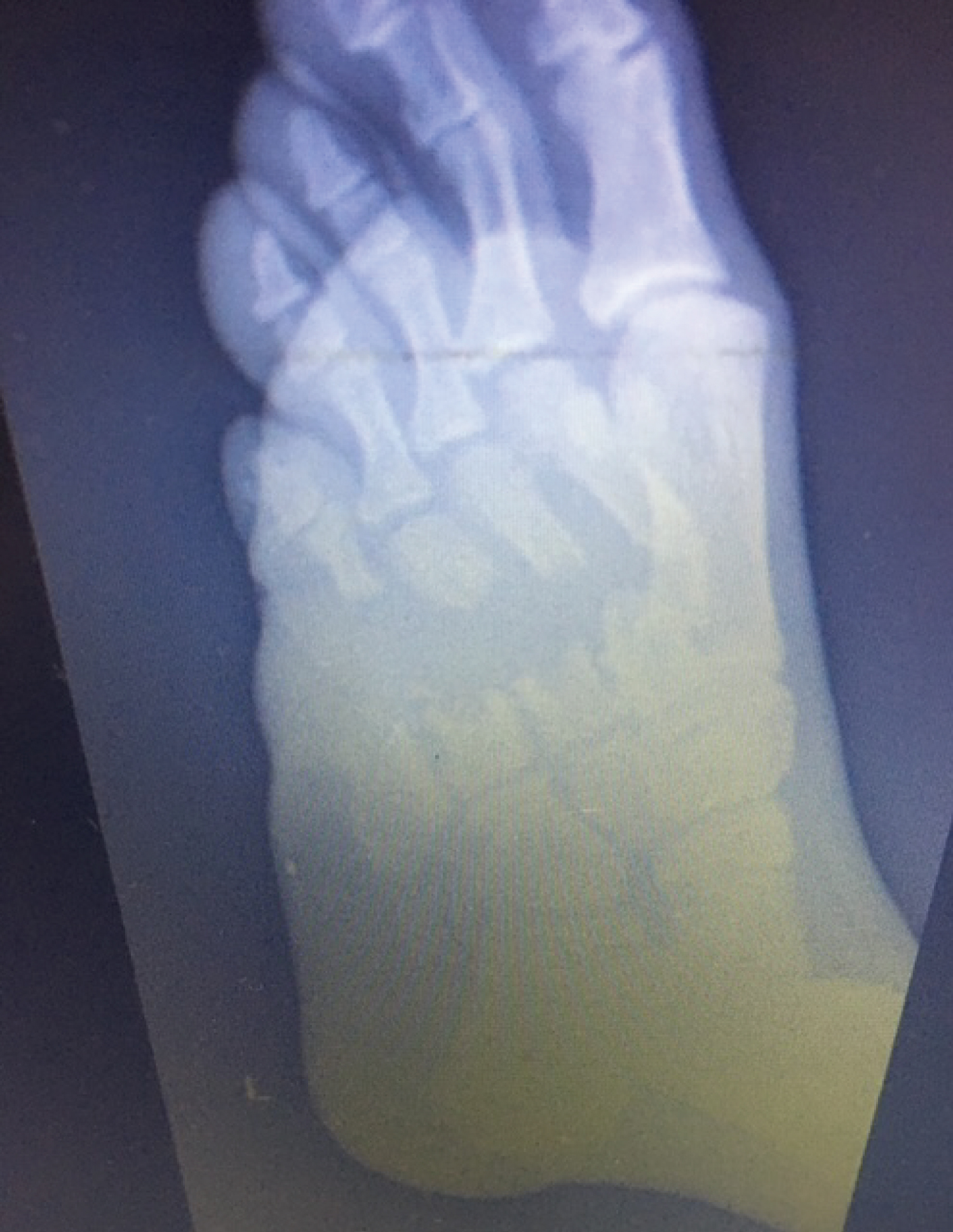 Figure 4: Regeneration of 2nd Metatarsal. View Figure 4
Figure 4: Regeneration of 2nd Metatarsal. View Figure 4
For the persistent bone loss and lack of foot rigidity in stance and on weight-bearing, we elected to proceed with bone grafting of the 3rd and 4th metatarsal in order to give him a stable foot to allow efficient weight bearing. The little toe was unsuitable for reconstruction due to the absence of the metatarso-phalangeal joint and extensive metatarsal loss. The patient was reluctant to have the terminal digit amputated and the distal segment was left in situ attached to the foot (see foot picture). The plan was made to use rib bone graft as his total bone defect (3rd and 4th metatarsals) was approximately 7 cm. He had only recovered from multiple lower limb soft tissue debridements and skin healing by secondary intention in his calf which made a fibular graft less viable.
Iliac crest bone graft was also considered, but the volume of tri-cortical bone required was likely to lead to significant donor site morbidity and increased risk of iliac wing fracture. Informed consent was taken and the procedure was performed in conjunction with the plastic surgery team.
The rib graft harvest procedure was performed under general anaesthetic with the patient positioned supine with 30 degrees of cranial tilt allowing for good access. The right arm was forward flexed and adducted across his chest to expose the ribs. The 7th rib was harvested with a longitudinal incision through the periosteal sleeve and taking care to protect the neurovascular structures and the pleura. 8 cm of rib was harvested which was adequate for the planned fixation with a small amount of redundancy (Figure 5). The rib harvest wound was closed in a layered fashion over a drain with 2-0 vicryl followed by 3-0 monocryl sutures to the skin.
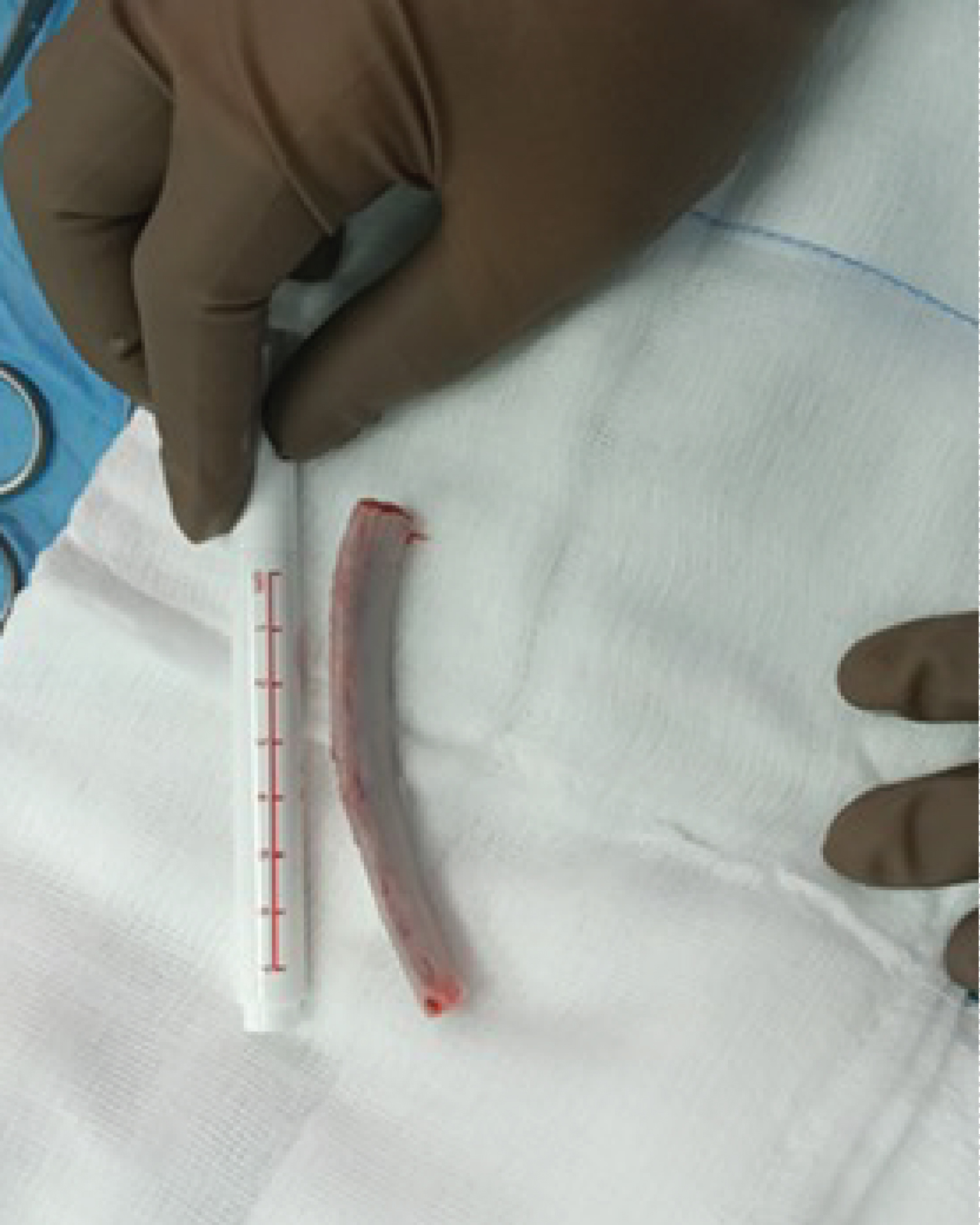 Figure 5: Harvested rib graft. View Figure 5
Figure 5: Harvested rib graft. View Figure 5
The foot was prepared and draped in the usual sterile fashion with a thigh tourniquet applied. The healed gracilis flap was approached laterally and elevated, progressing medially to the vascular pedicle. The second metatarsal was not included in the fixation given its proximity to the vascular pedicle and risk of compromising the vascularity of the flap. Additionally there was radiological evidence of bone regeneration progressing to union noted in the 2nd metatarsal.
The bone defects were measured out with attention paid to restoring the metatarsal cascade. The bone deficits were 4.3 cm in the 4th metatarsal and 2.2 cm in the 3rd metatarsal. The rib graft was divided then prepared and fashioned to fit into the 2 measured zones of bone loss. We ensured that compression was achievable by placing a slightly longer segment of rib graft than the measured gap.
A good approximation of the metatarsal head cascade was demonstrated radiographically. We used the Arthrex® foot plating system to secure the bone graft with locking screws into the metatarsal head, metatarsal base and screws to secure the graft onto the plate (Figure 6). Stable fixation was confirmed by clinical examination on the operating table and with intraoperative fluoroscopic pictures. The wound was thoroughly irrigated and the flap was closed with interrupted non-absorbable sutures.
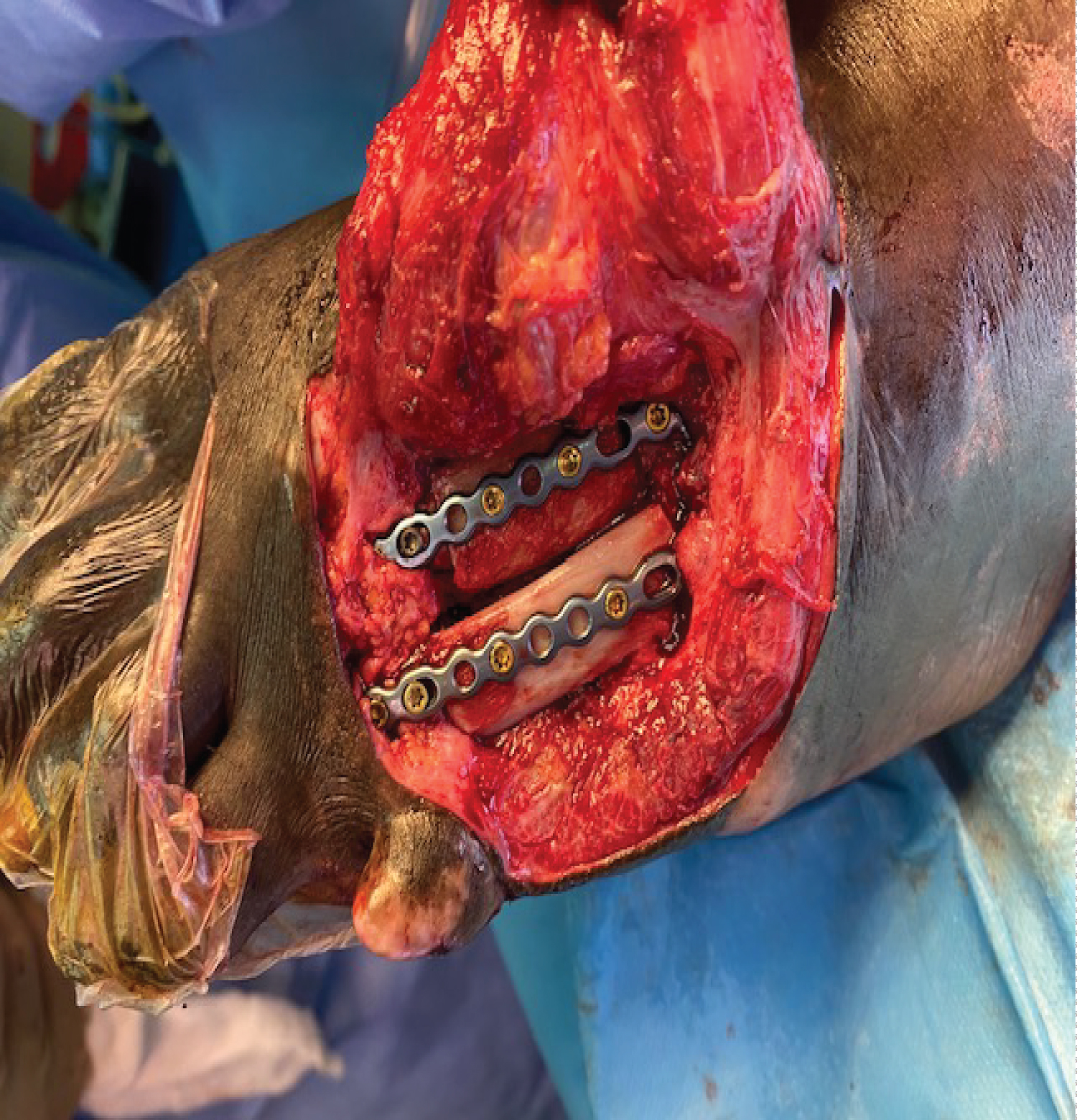 Figure 6: Intra-operative picture of graft fixation. View Figure 6
Figure 6: Intra-operative picture of graft fixation. View Figure 6
The patient had a nerve block to his foot and additionally had patient controlled analgesia for the rib graft donor site for two days, and after four days, he was almost fully pain free both in his left foot and donor site, and was only on non-opiate oral analgesia.
His flap healed uneventfully within 2 weeks and his radiographs were satisfactory (Figure 7 and Figure 8). He was comfortable enough to partially weight bear in a full cast avoiding any forefoot loading at that stage.
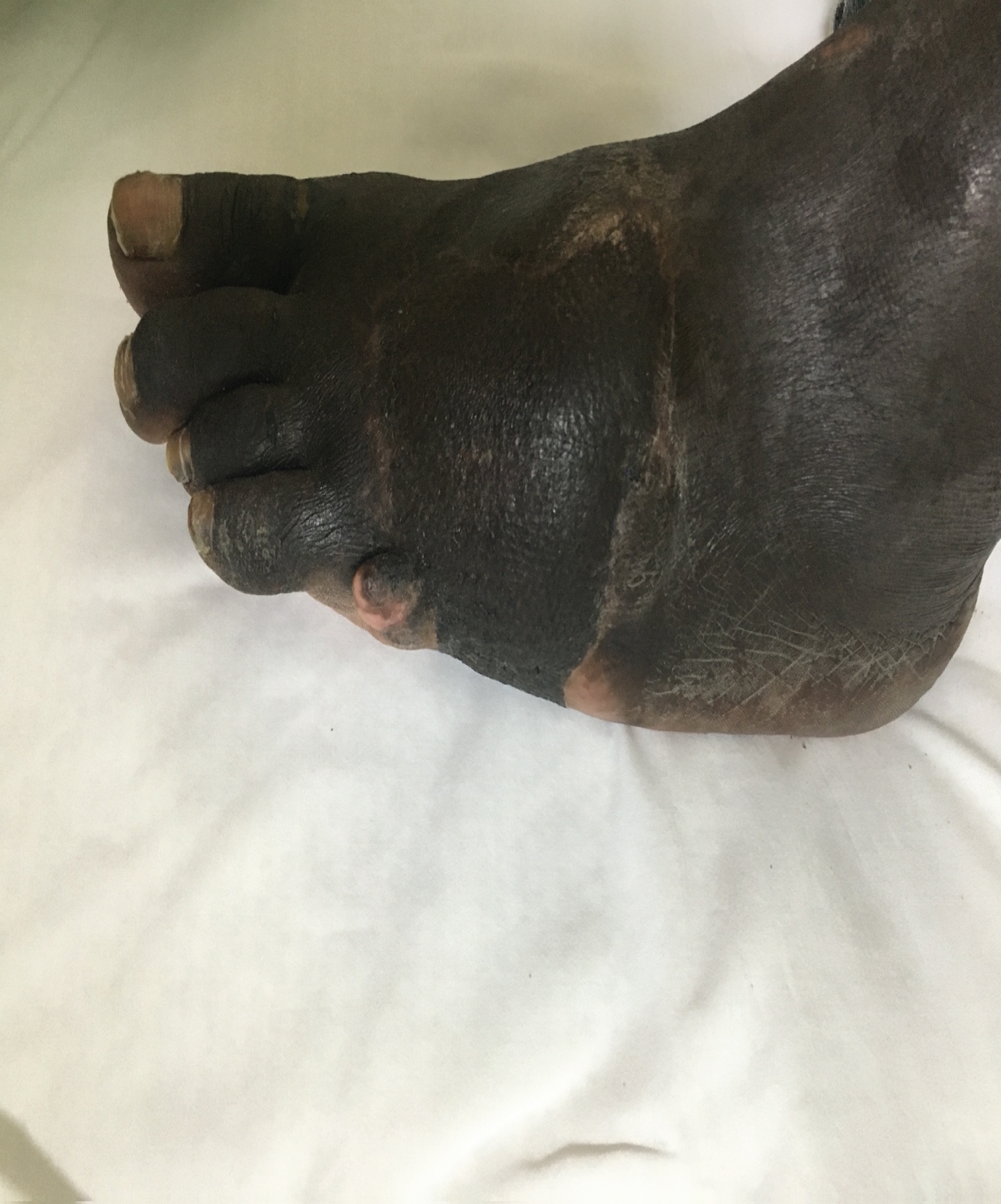 Figure 7: Healed flap. View Figure 7
Figure 7: Healed flap. View Figure 7
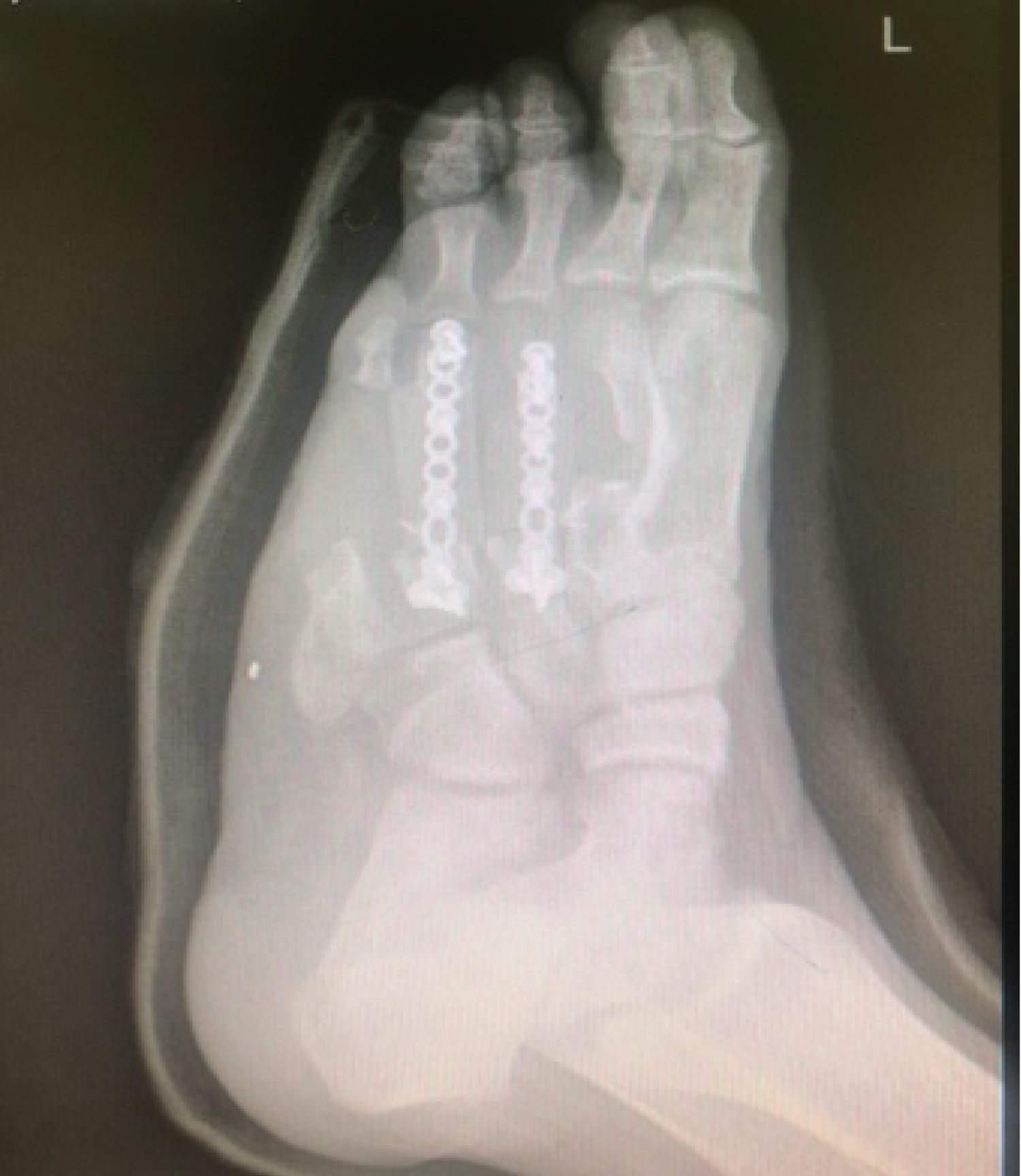 Figure 8: radiograph at 2 weeks. View Figure 8
Figure 8: radiograph at 2 weeks. View Figure 8
His radiographs at 6 weeks showed that the bone had united (Figure 9) and he was able to comfortably fully weight bear (see Video in appendix) with normal footwear.
 Figure 9: Rib graft union at 6 weeks. View Figure 9
Figure 9: Rib graft union at 6 weeks. View Figure 9
Video 1: Patient weight bearing at 6 weeks post rib grafting with normal gait pattern. View Video 1
Committing to salvage a foot with complex soft tissue injuries and bone loss is a significant challenge for the trauma surgeon. Serial soft tissue and bony debridements are critical initially to minimise the risk of infection. This is followed by performing coverage of open wounds with various soft tissue flap choices described in the literature including gracilis, rectus abdominis, serratus anterior and latissimus dorsi [11]. Finally bone stabilisation is pursued once the soft tissues are managed. This may be achieved over multiple stages as relayed in this report.
When there is adequate metatarsal bone, standard fixation is adequate with little or no cancellous or synthetic graft required. With increasing bone loss, the options are determined by the extent of bone loss and donor site morbidity. This must be balanced against the merit of undergoing amputation.
Amputation following lower limb trauma has a long and established history [12]. As recently as the mid19th century, mortality following amputation was as high as 50% [13]. Despite developments, it is still not a benign procedure, with risks including bleeding, infection, stump irritation, wound dehiscence, and persistent phantom pain. In addition to these organic complications, patients also have to contend with their often negative perceptions of living without a limb, the potential drop in quality of life, and the social stigma associated with the loss of a limb [14].
Limb salvage is the general preference, if a functional, plantigrade, painless and supple foot can be achieved. Blast injuries, however, pose a particular threat to the prospect of limb salvage as a significant amount of energy is transferred through the foot, fracturing bones and damaging soft tissue in the primary blast. This is followed by contamination by debris and direct blunt trauma in the secondary and tertiary blast injuries. The need for thorough debridement in order to prevent morbidity from sepsis is a well understood concept and often requires multiple trips to theatre often ending in significant tissue defects. Only once the tissues in the wound are clean can the reconstructive options be considered.
For large bone defects, induced membrane techniques e.g. Masquelet [15] have been used, where the defect is managed in two stages - in the first stage, after thorough debridement a cement spacer is utilised to fill the defect, allow the formation of the membrane and also to prevent the invasion of fibrous tissue. The area is then temporarily stabilised. The pseudo-membrane forms around the spacer and 6 to 8 weeks later, in the second stage, the membrane is incised, the spacer removed. The space is filled by cancellous autograft, which forms cortical bone over months, aided by the vascularity and growth factors present in the pseudo-membrane. This method has been used successfully to manage metatarsal bone loss [16]. Biological methods such as iliac crest and vascularised fibula bone grafts are also widely known [17-29] and their use in reconstruction of complex metatarsal fractures is well documented.
Georgescu, et al. [7] described the use of a muscle rib flap in the reconstruction of a patient with post-traumatic metatarsal and soft tissue bone loss, as did Kitsiou, et al. [8], using a serratus anterior and rib graft in their in their case series of four patients. Kurokawa, et al. [9] also used a serratus anterior muscle and 2-rib osteomyocutaneous free flap to reconstruct 4 metatarsals with extensive bone loss. Thomas, et al. [10] described the use of a serratus anterior vascularised rib composite flap to reconstruct the hallux metatarsal and the overlying soft tissues, noting that the patient remained ambulatory several years after the reconstruction. Trignano, et al. [11], in a reconstruction of a chronic complex foot injury, used a composite latissimus dorsi and serratus anterior and rib free flap. Battiston, et al. [21] used a similar flap in the reconstruction of a forefoot after oncological resection.
In all the above reviews, either a latissimus dorsi or serratus anterior vascularised osteomuscular or osteomyocutaneous flaps were used for soft tissue and metatarsal bone defects with the procedures performed in a single stage. There is, however, no report in the literature demonstrating use of rib bone grafts as a delayed reconstruction option. In our case, we performed a 2-stage procedure, first using a free gracilis flap for soft tissue coverage and then, weeks later, the second stage was undertaken where the rib was harvested and used as a bone graft in the metatarsals. There was low morbidity with this approach as highlighted by the speedy recovery and minimal analgesic requirement. We avoided the potential complications of scapula winging and pleural fibrosis associated with latissimus dorsi and serratus anterior grafts.
We were able to harvest adequate structural graft to allow for the fixation of the two metatarsals. Kay, et al. [1] demonstrated adequate stability using a gracilis free flap tunnelled through the wound and metatarsal defect of a patient who had shot himself through the foot with a shotgun, without the need for bone graft. In our case, there was persistent skeletal instability in the lateral foot 3 months after debridement and given his high functional status, we elected to proceed with the bone graft. The bone graft incorporated rapidly and he was able to fully weight bear six weeks after surgery with a normal gait pattern.
To the authors' knowledge, this is the first report of a two-stage rib bone graft to a metatarsal defect after soft tissue coverage with a gracilis flap. This technique may be a valuable addition to the options available in the treatment of these complex and potentially devastating injuries.
This report highlights the use of gracilis graft and rib bone graft to bridge defects in segmental metatarsal fractures with bone loss and soft tissue loss. The shape of the rib was suitable for the metatarsal gap and offered a robust graft option. There was surprisingly little donor site morbidity, which may have been partly down to the fact that an isolated rib harvest was performed without taking the latissimus dorsi or serratus anterior muscles. The outcome demonstrates that rib bone graft is a viable option in the surgeon's armamentarium when challenged with complex bone loss affecting multiple metatarsal bones. The harvesting is safe and a significant amount of bone graft can be obtained with minimal morbidity.