Avascular necrosis of the femoral head is a progressive disease characterized by bone ischemia which evolves to subchondral collapse in more than 85% of patients. We describe a case of an early stage idiopathic avascular necrosis of the femoral head in a female patient that was characterized by bone marrow edema involving the whole femoral head and the majority of the femoral neck with a small subchondral fracture and slight applanation of the femoral head. This condition was suspected by physiatrist after the detection of substantial effusion in the hip joint during ultrasound examination and confirmed after magnetic resonance imaging. The patient was treated with hyperbaric oxygen therapy with complete regression of both the clinical symptoms and the MRI findings. Clinical Rehabilitation Impact: Ultrasound examination during physiatrist evaluation can help in establishing the early diagnosis and in reducing the number of hip arthroplasties caused by avascular necrosis.
Avascular necrosis, Hyperbaric oxygen therapy, Physical medicine, Ischemia
Avascular necrosis (AVN) of the femoral head, also known as osteonecrosis, is a progressive disease characterized by bone ischemia, which evolves to subchondral collapse in more than 85% of patients. It affects the young population usually in their late 30s or early 40s [1]. Sometimes it is difficult to detect the early phase of AVN as it can be asymptomatic for a prolonged period of time, or have non-specific symptoms. Localized pain is the dominant symptom and increases with weight-bearing or other forms of pressure load.
Both physical therapy and reducing the pressure load are efficient in pain reduction, but do not affect disease progression. Attempts to reverse the process of bone degradation with non-invasive procedures or procedures less invasive than surgery are still ongoing. Biomechanical agents like extracorporeal shock wave therapy, electromagnetic therapy and medications such as bisphosphonates, anticoagulants, and vasodilators have all shown some efficacy in delaying disease progression in the early stages (prior to the femoral head collapse) but are still not in routine usage.
During the early stages of AVN, the widely accepted surgical procedure is core decompression, while total hip arthroplasty remains the most common way of treating secondary osteoarthritis following femoral head collapse (i.e. the final stage of AVN).
Our hypothesis is that hyperbaric oxygen therapy (HBOT) is ideal for treating stage I or II of AVN on the Ficat-Arlet scale or Steinberg classification system, since it restores tissue oxygenation, reduces edema and restores venous drainage [2]. This case report illustrates a patient who has been treated with HBOT and who had complete reversion of the edema and ischemia in the AVN of the femoral head with a concurrent subchondral fracture. The use of hyperbaric oxygen therapy in this indication is still under research and not used in everyday practice.
A female patient (aged 52 years) underwent a physiatrist examination a month after initial pain in the right hip area had appeared. The pain was localized to the right hip area, to the ipsilateral buttock, and to the greater trochanteric region. Symptoms were exacerbated with weight-bearing. An orthopedic surgeon previously treated her for suspected pertrochanteric and bursitis, and 40 mg of Depo-Medrol was administered locally. No beneficial effect was observed. A rheumatologist ruled out inflammatory connective tissue disease and recommended physical medicine treatment. On the first physical examination, the patient walked in aided by two sub-axillar crutches and her right foot had no contact with the floor. She reported that similar symptoms had occurred earlier on two previous occasions: 20 years ago during her 36th week of pregnancy and 6 years ago during an intensive aerobic workout. On the prior two occasions, the pain lasted two weeks and she was able to walk despite pain in her right hip area. She also reported that during the last week, the pain radiated anteriorly from her groin area through to her right knee.
Clinically, limited movement in the right hip was observed: flexion 0/90°, rotations, both internal and external, 0/30° and 0/25° respectively and painful abduction 0/40°. Both the straight leg test against resistance and the "log roll test" with passive internal and external rotations, provoked pain. FABER test revealed limited external rotation in the right hip and the patient reported pain in the groin and buttock area on the right side. The right greater trochanter was painful on palpation. Pain assessment on the visual analogue scale (VAS) was 8/10 and the right sacroiliac joint was slightly painful on palpation (VAS 3/10). The left hip joint had no movement limitation. Initially we prescribed high intensity laser therapy (HILT) and ultrasound therapy (1.0 W/cm2) on the greater trochanteric region, as well as on the right hip joint. After ten sessions, pain in the greater trochanteric region decreased to VAS 4/10. No pain was reported in the right sacroiliac joint.
Considering the patient still experienced pain upon weight-bearing, on the follow-up examination, a diagnostic ultrasound (US) of both hip joints was performed by the physiatrist (Figure 1). Significant effusion of the right hip joint led to a magnetic resonance imaging (MRI) of both hip joints (Figure 2). The MRI revealed an ischemic lesion of the entire head and neck of the right femur with edema, including slight applanation of the femoral head and a small subchondral fracture (Steinberg classification system, grade I). Upon consultation with an orthopedic surgeon, the patient was referred for HBOT. Consequently, this choice of therapy was proposed for two months after the initial symptoms appeared.
 Figure 1: Ultrasound examination of both hip joints. Effusion in the anterior synovial recess in the right hip (left side) vs. normal finding on the left hip (right side). e- marks effusion.
View Figure 1
Figure 1: Ultrasound examination of both hip joints. Effusion in the anterior synovial recess in the right hip (left side) vs. normal finding on the left hip (right side). e- marks effusion.
View Figure 1
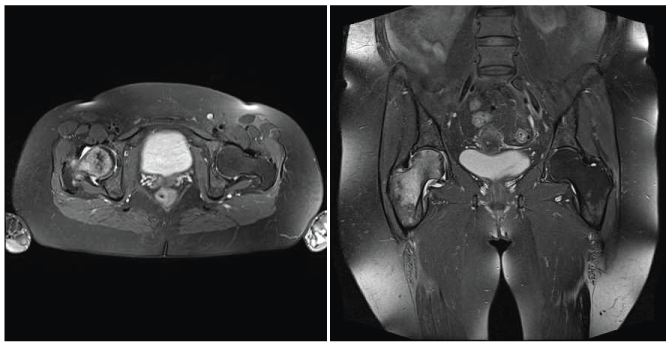 Figure 2: MRI of both hip joints. Subchondral fracture of the right femoral head, an ischemic lesion and edema of the right femoral head and neck (left side of picture). Axial and coronal images in T2.
View Figure 2
Figure 2: MRI of both hip joints. Subchondral fracture of the right femoral head, an ischemic lesion and edema of the right femoral head and neck (left side of picture). Axial and coronal images in T2.
View Figure 2
In total, the patient underwent 40 treatments of breathing oxygen at a partial pressure of 2.2 Bar for 60 minutes per day, 5 days a week, as used by Reis, et al. [3].
Usual adverse events of HBOT are fatigue and lightheadedness, but serious events like oxygen poisoning, damage to the lungs, rupture of the middle ear, damage to the sinuses and changes in vision can be seen. Our patient experienced none of the adverse effects.
At the end of the HBOT she felt much better. There was full mobility of the right hip joint, and the pain subsided. Six weeks after the last HBOT treatment, a control MRI revealed complete regression of the ischemic lesions of both the head and neck of the right femur (Figure 3). Six months later on the follow-up examination, the patient reported walking normally unaided by crutches during the entire period after undergoing HBOT. Control diagnostic US showed no effusion in the right hip joint. She was advised not to engage in any impact sports with potential for high load to be exerted on the hips, but to swim and/or do cycling instead.
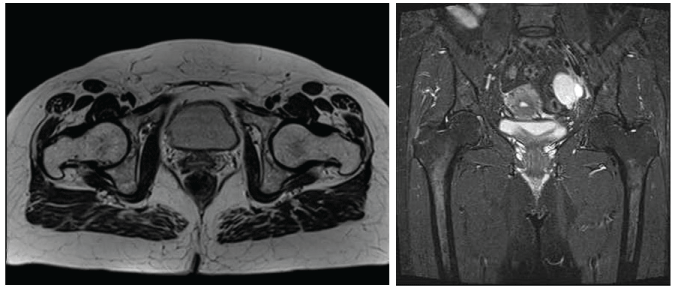 Figure 3: Control MRI of both hip joints 6 weeks after HBO2 treatment shows complete resolution of the ischemic lesion and edema. Axial image in T1, coronal image in T2.
View Figure 3
Figure 3: Control MRI of both hip joints 6 weeks after HBO2 treatment shows complete resolution of the ischemic lesion and edema. Axial image in T1, coronal image in T2.
View Figure 3
AVN of the femoral head is responsible for approximately one out of ten arthroplasties [4]. The etiology of this clinical condition is uncertain, and possibly multifactorial. It can be of a traumatic, atraumatic and idiopathic nature. About 30% of all AVN are idiopathic [5]. No matter what the reason for AVN is, it's pathophysiology is always the same and includes reduced blood perfusion in bone tissue, local hypoxia, diminished cell energogenesis, and loss of structural strength [6]. If the condition lasts long enough, complications like fractures, edema, osteoporosis, and collapse ensue. HBOT treatment can be used to completely reverse the process of ischemia prior to the irreversible bone collapse.
In this case the patient had a complete rheumatologic examination prior to seeing us (i.e. physiatrists), therefore some of the more common reasons for AVN, such as idiopathic hyperlipidemia, coagulopathies, chronic liver disease or systemic lupus erythematosus, were excluded. As for the other AVN risk factors, the patient reported that she had never smoked tobacco, that she drinks about 3 dL of red wine at lunch, and that she had never used systemic corticosteroid therapy. Furthermore, she had never had injuries such as hip dislocation and femoral head or neck fractures. Since no predisposing factors could be identified in our patient, we presumed that the unilateral AVN of the femoral head was, in fact, idiopathic.
Patients with idiopathic AVN sometimes report similar pain and limitation of hip movement in their history. These attacks usually last for a shorter period of time (one or two weeks). Our patient also had two prior episodes of hip pain: one during her pregnancy and one after an intensive workout. The pain and limitation of movement lasted for one month in this patient. This is not long enough to detect osteoporosis on radiographs of the femoral head, because it usually takes 2 months from the first symptoms until the detection on radiograph images.
Vitality of the bony tissue is the result of the finely balanced functions of different cells. The functions of these cells are energy dependent, and in hypoxic conditions, anaerobic production of ATP is insufficient for adequate performance of these specialized cells. The function of osteoblasts is more energy dependent, and ceases earlier while osteolytic processes still prevail. This accounts for the dubious rationale for bisphosphonate usage to slow down the progression of a subchondral fracture.
If AVN is suspected and the plain radiographs are normal, a MRI examination is indicated in most diagnostic algorithms. Association Research Circulation Osseous (ARCO) incorporated MRI results as one of the parameters in their classification of AVN of the femoral head [7] while Ficat-Arlet [8] and Steinberg classification system [9] firstly used only plain radiographs. It is established that MRI has 90 - 100% sensitivity and 100% specificity in the detection of AVN of the femoral head.
In our patient we opted for a MRI, when the first 10 treatments with physical therapy failed to show full mobilization of the right hip joint and after ultrasound detected significant effusion in the right hip joint (Figure 1). The MRI showed significant bone marrow edema and a small subchondral fracture with only slight applanation of the femoral head, which placed this patient in grade I of ARCO classification, and therefore suitable for HBOT.
The treatment of femoral head AVN needs to be proactive in its concept. Efficient timing of HBOT during the treatment of AVN is an important question to be answered. In the earliest stage of AVN, characterized by pain that increases on pressure load or weight-bearing but with only bone marrow edema on MRI, the patient has a strong chance of recovery with unloading of the painful joint and physical therapy alone. This is confirmed by histological studies that suggest the earliest symptomatic stage of AVN is preceded by bone marrow edema [10]. Experimental work on animals concludes that HBOT does not prevent the occurrence of AVN but instead promotes and accelerates healing.
If the condition progresses and the MRI detect a subchondral fracture, HBOT merits serious consideration. If the subchondral fracture leads to serious anatomical damage, HBOT hardly causes any effect, and may be considered only within the postoperative period to enhance healing and to prevent complications in high-risk patients like those with diabetes mellitus.
Mont, et al. reported in their systematic review that simple unloading of the affected leg showed radiological progression of the disease in the majority of patients with medium and large lesions of the femoral head and in 32% of patients with small lesions [11]. Therefore an expectative method is not sufficient and additional medical or surgical management should be considered within a timely manner.
Since HBOT is an efficient method of delivering oxygen into hypoxic blood-deprived tissues, its use in AVN is logical, to say the least. A high content of dissolved oxygen in the arterial plasma diffuses into tissues and reaches areas where red blood cells containing hemoglobin are not readily available. It is reasonable to expect that restoring the optimal tissue oxygen level will thus enable restoration of the cell function. Furthermore, hyperoxia causes vasoconstriction, which can reduce edema and compartment pressure in the damaged bone. This all leads to reduced intraosseous pressure, better microcirculation and eventual neovascularization. This effect is similar to the one made by operative core decompression of the femoral head.
Study by Reis, et al. showed regression of the MRI changes in 12 out of 16 Steinberg stage I femoral heads with AVN in humans [3], in addition Camporesi, et al. followed up their patients for 7 years after HBOT and they all showed clinical improvement and none underwent total arthroplasty of the hip joint [12]. However, HBOT is still considered controversial in the early stage of AVN, due to the limited data available [5].
We describe a case of an early stage idiopathic AVN of the femoral head, that was characterized by substantial bone marrow edema involving the whole femoral head and the majority of the femoral neck and a small subchondral fracture with slight applanation of the femoral head. The patient was treated with HBOT and the outcome was complete, long-lasting regression of both the clinical symptoms and the MRI findings. Appropriately timed professional cooperation between the orthopedic surgeon, the physiatrist, the radiologist and the expert/doctor who coordinates the hyperbaric oxygen therapy is crucial in aiding the reduction of the number of hip arthroplasties caused by AVN. Ultrasound examination during physiatrist evaluation can help in making the early diagnosis.
We are grateful to Dijana Gugić, MD, PhD and Rebecca Grimes, medical student, for their kind remarks after critical reading of this case report.
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.