To assess the improvement of knee contractures in five patients with transtibial amputation, after treatment with Segmental Muscle Vibration (SMV), added to general physical therapy.
Ten patients, with restrictive knee contractures, were divided in two groups: group A, with 5 patients, received physical therapy and SMV; group B received only physical therapy. All patients were treated for 2 hours/daily, 5 days/week with conventional physical theapies; to this protocol, a daily treatment with SMV was added for 20 sessions in patients of group A: 10 sessions of dynamic slow wave (20 Hz), with decontracting and draining action, were performed; succesivily 10 session of dynamic medium wave (50 Hz), with trophic action, were added. Knee and hip ROM were measured, using a goniometer, before (T0) and after (T1) 30 days of treatment.
After 20 sessions of treatment, all patients of group A obtained a greater improvement in knee extension of lower limb amputee rather than patients of group B (p < 0.0001).
SMV, when added to general physical therapy, could be a valid support improving, in a short-term period, knee contractures in patients with transtibial amputation.
Lower limb amputation, Segmental muscle vibration, Knee contractures
Rehabilitation of the lower limb amputee should begin as soon as amputation is performed. Presurgical period includes medical stabilization, patient assessment for amputation level, pain control, psychological support and a functional rehabilitation program [1]; in postsurgical period wound care, edema control, functional rehabilitation [1-5] (especially prevention of hip and knee contractures, ROM and strengthening exercises), pain management (including phantom limb sensation) [6] and skin problems (such as pressure/shear ulcerations, infections, verrucose hyperplasia) [7,8] are included. Joint contractures are frequent complications in amputees [1]: initial treatment consists of an intensive stretching program; besides, extension devices, like knee immobilizers, can also provide relief.
Aim of our study is to evaluate the efficacy and the possible improvement that Segmental Muscle Vibration (SMV) could provide as adjuvant therapy in reducing knee contractures in patients with transtibial amputations, when added to classic physical therapy, in a short-term period: we report five patients improved after treatment with SMV and general physical therapy compared with five patients treated only with general physical therapy.
Ten transtibial amputation patients with restrictive knee contractures and low/nothing hip contractures were randomly divided in two groups: group A, with five patients, received physical therapy and SMV; group B, with other five patients, received only physical therapy. Data patients are summarized in (Table 1). All participants signed an informed consent form to the treatment in accordance with the Declaration of Helsinki; according to the law of our Country this study does not need any ethics committee approval. All patient were hospitalized in the same rehabilitation clinic (Rehabilitation Medical Center "CMR", Sant'Agata de' Goti, Benevento, Italy) for 40 days, in a period from January to April 2016, and visited by the same physiatrist: knee and hip ROM were measured using a goniometer, before (T0) and after (T1) 30 days of treatment. The same therapist treated all patients, with the same rehabilitation protocol including stretching program, ROM and strengthening exercises (especially in knee and hip extensors); a knee extension board was fitted underneath the wheelchair to promote knee extension. All patients were treated for 2 hours/daily, 5 days/week; to this protocol, in patients of group A, a daily treatment with Segmental Muscle Vibration (SMV) was added for 20 sessions. After 30 days of physical therapy and treatment with SMV, the last 10 days of hospitalization were used to perform the deambulation training with prosthesis. In both groups, X-rays were performed at T0, to assess bone structures; besides, an ultrasound evaluation was performed to assess the connective and muscular tissues of lower limb amputee (T0), and evaluating possible changes in tissue after treatment with SMV in patients of group A (T1).
Table 1: Patients data at T0: Sex, age, cause and time since amputation, knee and hip ROM (knee flexion is measured in patients with hip flexed) in group A and group B. View Table 1
Segmental Muscle Vibration (SMV) is a particular kind of acoustic energy, that could be used to low frequency (slow waves: 25-50 Hz) with decontracting, analgesic and draining action; mid frequency (medium waves: 50-80 Hz) with trophic and toning action; high frequency (fast waves: 80-120 Hz) with action on spasticity and hypertone [9]. SMV can be used in static or dynamic way: static waves are continuous, while dynamic waves alternates activity phases with rest intervals. SMV therapies were performed with a suitable and authorized commercial device (Horus, Akropolis, Rome, Italy) using dynamic waves, applied for 6 seconds, with 2 seconds of rest. The Horus is an acoustic-wave vibratory device composed of a control unit and 3 multiple probe transducers with 4 head transducers each for the transmission of the vibratory stimulus. The acoustic production device generates an acoustic wave that is induced within the probe cavities and then translated into a vibratory stimulus within the transducer heads that are fixed to the body surface with elastic bands. 10 sessions of dynamic slow wave (20 Hz), with decontracting and draining action, were performed (the first 5 sessions for 20 minutes, then the next 5 sessions for 30 minutes); successively 10 session of dynamic medium wave (50 Hz), with trophic action, were performed (the first 5 sessions for 20 minutes, then the next 5 sessions for 30 minutes). Four head transducers were positioned on the quadriceps muscle of the lower limb amputee (two on the lateral and medial vastus, and two on the rectus femoris, proximally and distally on the muscle), while the patient was in supine position with extended hip and knee joints. Probes were installed by the same therapist who worked on the rehabilitation protocol.
T-student test was used to analyze data and any statistical differences from T0 to T1 and at T1 in two groups.
After 20 sessions of treatment, all patients of both groups obtained an improvement of knee extension: in group A, mean knee extension improved from T0 (+ 25° ± 5°) to T1 (+ 5° ± 2°) (p < 0.0001); similarly in group B an improvement of mean knee extension from T0 (+ 27° ± 4°) to T1 (+ 13° ± 4°) (p = 0.0001) was observed (Table 2). However, comparing data at T1 in two groups, there is an improvement statistically significative in patients treated with coadiuvant treatment of SMV rather than patients treated only by general physical therapy (from + 5° ± 2° of group A, to + 13° ± 4° of group B, p < 0.0001). Table 3 to ultrasound evaluation, in two patients of group A, a marked thickening and soaking of subcutaneous adipose tissue, with signs of hyperechoic lobular organization, were observed, particularly in correspondence of the third distal of quadriceps muscle (about 8 cm from the patella*, a maximum of 2.4 cm thickening of subcutaneous adipose tissue was observed) figure 1 and on the residual limb; in other patients of group A and B, a normal thickness and echogenicity of muscle and subcutaneous tissues were observed. After 20 sessions of SMV treatment, in these two patients of group A, a reduction in thickness/soaking and lobular organization in subcutaneous adipose tissue were obtained (a maximum of 1.3 cm thickening was observed in the same side*) figure 2; in remaining patients of both groups no tissues modification were observed after treatment with physical therapy and SMV. To X-rays, in all patients of both groups A and B, typical signs of osteoarthritis were observed.
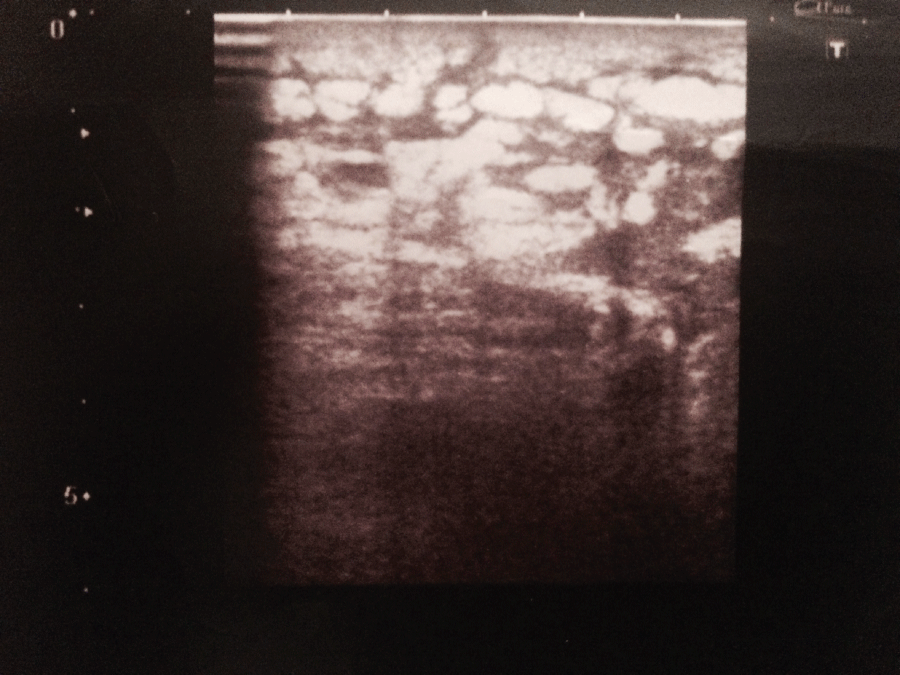 Figure 1: Marked thickening and soaking of subcutaneous adipose tissue in correspondence of the third distal of quadriceps muscle (about 8 cm from the patella, a maximum of 2.4 cm thickening, with signs of hyperechoic lobular organization, were observed).
View Figure 1
Figure 1: Marked thickening and soaking of subcutaneous adipose tissue in correspondence of the third distal of quadriceps muscle (about 8 cm from the patella, a maximum of 2.4 cm thickening, with signs of hyperechoic lobular organization, were observed).
View Figure 1
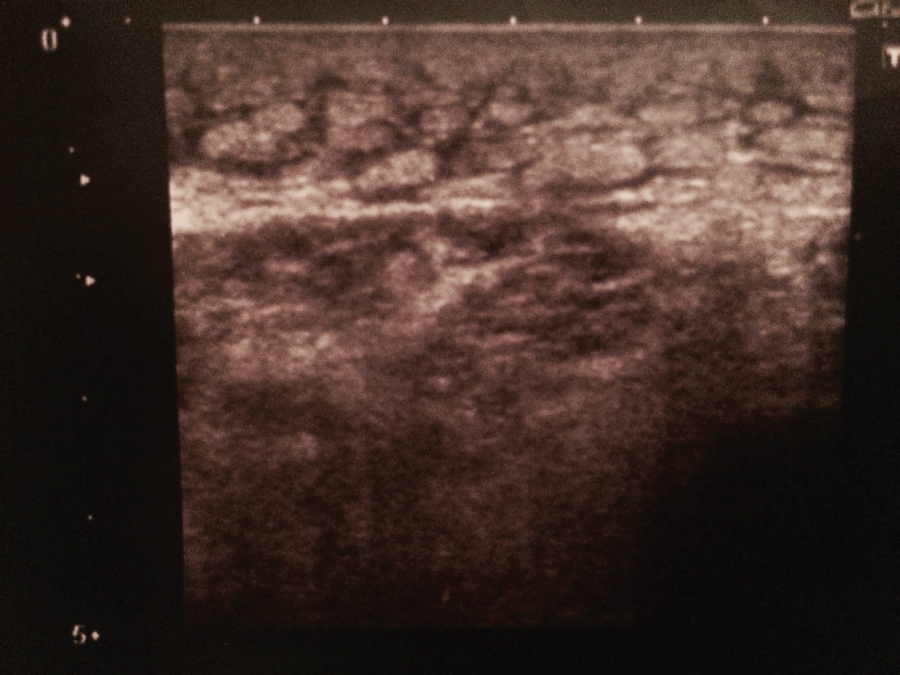 Figure 2: Reduction in thickness/soaking and lobular organization in subcutaneous adipose tissue (about 8 cm from the patella, a maximum of 1.3 cm thickening was observed), after 20 sessions of SMV treatment.
View Figure 2
Figure 2: Reduction in thickness/soaking and lobular organization in subcutaneous adipose tissue (about 8 cm from the patella, a maximum of 1.3 cm thickening was observed), after 20 sessions of SMV treatment.
View Figure 2
Table 2: Knee extension ROM improvement, from T0 to T1. View Table 2
Table 3: Knee extension ROM differences at T1. View Table 3
Segmental Muscle Vibration (SMV) is a special form of acoustic energy, used in different rehabilitation fields, such as musculoskeletal pain, neuro-rehabilitation and sport medicine [9,10]. The effect of vibration on flexibility might involve a shift of the pain threshold and the stimulation of muscle spindle and Golgi tendon organs, causing the inhibition of muscle contraction [10]. Vibratory stimulation of the muscle spindle may produce Ia input, which modulates the recruitment thresholds and firing rates of motor units [10,11]. Issurin, et al. [9] proposed that vibration increases excitatory inflow from muscle spindles to the motor neuron pools and reduces the inhibitory impact of Golgi tendon organs, due to accommodation to vibration stimuli. Ribot-Ciscar, et al. [12] proposed that vibration, producing centrally localized neural changes, reduces the perception of tendon stretching, due to a decreased spontaneous firing rate in the muscle spindle primary endings after vibration. This may contribute to the increased flexibility after vibration. The level of Golgi tendon organ excitation is therefore a possible mechanism for the muscle flexibility after vibration [10,13,14]. Considering these mechanisms, Bakhtiary, et al. [15] reported how localized application of vibration improves passive knee extension in women with reduced hamstring extensibility; other similar studies [16-18] described how joint mobility changes when low frequency vibration were associated with stretching exercise. Lundeberg, et al. [19] showed that SMV produces analgesic effects during and after the procedure: one of these mechanisms is explained by Broadbent, et al. [20], which reported how vibration therapy reduces plasma IL-6 and muscle soreness; besides, reduction of the pain contributes to muscle elongation [20]. We proposed that the vibratory action at low energy should have an important action to reduce thickening and soaking of edematous subcutaneous adipose tissue: these decontracting and draining SMV properties, in fact, could be used to reduce edema and increase muscle flexibility on knee contractures; successively trophic SMV properties should be used to enhance the quadriceps muscle action, in order to increase the extensor action of the muscle. All these conditions could be considered and included in the rehabilitative program of amputee patients as a valid support anticipating prosthetic times and deambulation training.
The use of Segmental Muscle Vibration in flexion contractures of lower limb amputees remains an exciting area for future research. Further studies are still needed to choose the optimal frequencies, amplitudes and vibration duration, in order to enhance patient rehabilitation protocol, and anticipate the prosthetic process. We can conclude that, although the poor cases of our study, SMV, when added to general physical therapy, could be considered a valid support improving, in a short-term period, knee contractures in patients with transtibial amputation.