Tubercular mastitis is a great masquerader and is an extremely rare entity as extra-pulmonary tuberculosis even in endemic countries like India and incidence accounts for 4% of breast lesions.
We report a case of primary TB of breast in a elderly female presenting as diffuse upper left breast lump with indurated and ulcerated overlying skin along with retraction of nipple. Clinically suspicion was of abscess and duct ectasia. Fine needle aspiration cytology (FNAC) of breast lump with touch imprint smears was done. FNAC showed epithelioid cell granulomas, Langhans type of giant cells with the presence of acid-fast bacilli on Ziehl Neelsen (ZN) stains.
FNAC diagnosis of tubercular mastitis is a useful tool for the proper management and treatment of patient thus avoiding unnecessary surgery.
Tuberculosis, Breast abscess, FNAC, Duct ectasia
AFB: Acid Fast Bacilli; ATT: Anti Tubercular Treatment; CB-NAAT: Cell Based Nucleic Acid Amplification Test; FNAC: Fine Needle Aspiration Cytology; PAP: Papanicolaou; PCR: Polymerase Chain Reaction; ZN: Ziehl Neelsen
Tubercular mastitis is a great masquerader and is extremely rare, especially in elderly patients. Extra-pulmonary breast tuberculosis is a rare clinical entity with an incidence ranging from 0.1% in developed countries to about 4% in highly endemic countries like India [1,2]. Tuberculosis of breast is a disease of younger age group; uncommon in older females with breast mass which may mimic carcinoma, whereas younger patient usually manifests signs of pyogenic breast abscess [3,4]. The clinical signs of mammary tuberculosis can be insidious and nonspecific, often simulate signs of breast carcinoma or breast abscess. Mammary tuberculosis usually affects young, multiparous, lactating women although it may also be seen in males in 4.5% of cases [5]. The aim of this case is to highlight the importance of FNAC as the first investigation of choice in diagnosing breast tuberculosis, especially in older female presenting with retraction of the nipple and also saving the patient from other invasive diagnostic procedures.
A 52-year post-menopausal female presented in the surgical outpatient department of our hospital with diffuse swelling in left upper inner quadrant breast and retraction of the nipple for 2 years. She was referred to the department of pathology for FNAC with a clinical differential diagnosis of breast abscess and duct ectasia.
On examination besides the left breast lump, a small ulcer was present over the inflamed skin with excoriation and pus discharge near the areolar lesion (Figure 1). She denied any history of loss of appetite, weight loss, fever, night sweats, pain, cough or respiratory and systemic symptoms. There was no history of exposure to tuberculosis. No evident axillary lymphadenopathy was present. All vital signs, as well as blood/urine analysis/chest X-ray, were normal. She had done incision and drainage for left breast abscess 1 year back. FNAC reported earlier from outside lab as breast abscess. She took antibiotics treatment, but no recovery was seen. Patient's mammography report showed irregular nodular density and multiple tubular dilated structure with echogenic debris and no intraluminal mass in retro-areolar lesion of breast. Radiological suspicion was duct ectasia.
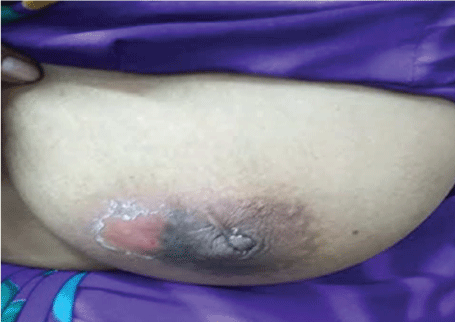 Figure 1: Picture showing diffuse upper left breast swelling and retraction of the nipple with pus discharge near the areolar lesion. View Figure 1
Figure 1: Picture showing diffuse upper left breast swelling and retraction of the nipple with pus discharge near the areolar lesion. View Figure 1
The patient underwent FNAC of left breast lump with touch imprint smears in our department of pathology and laboratory medicine. Minimum four slides each for Giemsa and PAP stain were prepared from the aspirated material. Imprint smears prepared from the pus oozing out from the inflamed skin were stained with ZN staining for acid-fast bacilli (AFB).
Cytological smears revealed epithelioid cell granulomas, Langhans giant cells, lymphocytes and clusters of fibroblastic cells. Imprint smears from the pus showed degenerated and intact neutrophils with foamy macrophages and necrotic debris (Figure 2a, Figure 2b and Figure 2c). The ZN stain revealed classical pink colored beaded rod-shaped AFB (Figure 2d). The final report of tubercular mastitis was given. CB-NAAT testing of the FNAC sample for Mycobacterium tuberculosis was positive with rifampicin sensitivity. Followed by culture for M. tuberculosis was advised which also confirmed the tubercular infection. She was also started on anti tubercular treatment and responded well with ATT on follow up of 6 months.
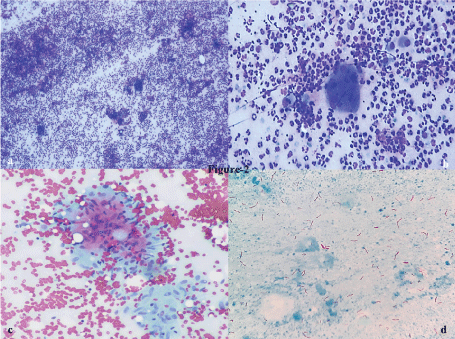 Figure 2: FNAC smears showing mixed inflammatory cells comprising of degenerated and intact neutrophils, lymphocytes with foamy macrophages, epithelioid cell granuloma on a necrotic background. ZN stain for AFB was positive (Giemsa, PAP, ZN, x40). View Figure 2
Figure 2: FNAC smears showing mixed inflammatory cells comprising of degenerated and intact neutrophils, lymphocytes with foamy macrophages, epithelioid cell granuloma on a necrotic background. ZN stain for AFB was positive (Giemsa, PAP, ZN, x40). View Figure 2
The tuberculosis is highly endemic in India, but still tuberculosis of breast is an extremely rare entity. The causative agent M. tuberculosis can infect multi-system organs resulting in disseminated extrapulmonary tuberculosis. However, the organs like spleen, muscle, and breast confer resistance to the multiplication of M. tuberculosis, and hence tubercular mastitis has a low incidence. The disease is commonly seen in women between 20 and 50 years of age, especially among multiparous, lactating and immunocompromised females where breast is more sensitive to infection and trauma. Primary breast tuberculosis is extremely rare [6], or secondary may be as a result of hematogenous spreading, retrograde spread from axillary lymph nodes or direct extension from the lung, pleura, mediastinum and articular lesions [6,7]. In the present case, the patient was immunocompetent, and she had no focus of TB elsewhere in the body.
Clinical presentation is extremely variable, often presenting as round nodular lumps with indurated tissue, often with fistula formation, but is rarely associated with pain and breast discharge. In its advanced form, breast tuberculosis is characterized by invasion of the skin, with skin and nipple retraction creating the peau-d'-orange. Our case had diffuse left breast lump with nipple retraction along with a small ulcer near the areolar lesion depicting advanced lesion of tuberculosis with a long history of 2 years.
Radiological imaging modalities like mammography or ultrasonography are unreliable in distinguishing it from carcinoma because of the variable pattern of presentation [8]. Diagnosis is ideally by demonstration of AFB in the breast tissue by ZN stain or culture [9]. In the present case sono mamography revealed features of duct ectasia while FNAC revealed epithelioid granuloma with the presence of AFB positivity on ZN staining.
It is known that the demonstration of AFB from the lesions is usually difficult with bacilli being isolated in only 25-30% of cases and AFB identified in only about 12% of patients [10]. It may not be possible to recover AFB from any site, including the breast. However, TB should be suspected in a patient who has a recurring breast abscess after adequate drainage on previous occasions as our patient had a recurrent history of breast abscess with an episode of incision and drainage 6 months back.
In cytology, the presence of granulomatous inflammation with caseation necrosis and the demonstration of the acid-fast bacilli by ZN staining is suggestive of tubercular mastitis. However, the confirmation has to be done if only granulomatous inflammation is reported in cytology. Identifying acid-fast bacilli is particularly difficult in tubercular mastitis due to the low bacilli load in such tissues. In most cases, classical granulomatous inflammation and caseous necrosis on cytology supported by anyone confirmatory test like culture report are sufficient for initiating ATT instead of performing invasive biopsy procedures.
Tuberculous mastitis is uncommon even in countries where tuberculosis is highly endemic. It can mimic breast abscess or cancers clinically so FNAC acts as a first-line screening modality may lead to proper diagnosis and treatment of the patient. It helps in avoiding other expensive ancillary diagnostic tests such as mammography, PCR, and unnecessary surgery. Breast TB should be suspected when there is a poor response to antibiotics used for the treatment of breast abscess, especially in a TB endemic country. This case thus substantiates the fact that the clinicians should always keep a broad spectrum of differentials in breast lesions to avoid erroneous diagnosis.
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published, and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
None.
There are no conflicts of interest.