Pseudomelanosis of the upper gastrointestinal tract is rare and classically associated with oral iron intake, upper gastrointestinal bleeding, diabetes mellitus, end stage renal disease and antihypertensive medication use. Duodenal involvement is well described, but only few cases of combined stomach and duodenal involvement have been reported to date. The lesion is indolent but can mimic more concerning entities like malignant melanoma. We report an 84-year-old man who presented with lower gastrointestinal bleeding and was found to have areas of blackened gastric and duodenal mucosa on endoscopy, which was confirmed as gastric and duodenal pseudomelanosis on microscopy.
Stomach, Duodenum, Histopathology, Endoscopy
Pseudomelanosis in the upper gastrointestinal (GI) tract is infrequently seen. While it is associated with oral iron intake, upper GI bleeding, diabetes mellitus, renal disease and hypertension, its precise etiology remains elusive. Pseudomelanosis is more frequently identified in the duodenum (pseudomelanosis duodeni) and terminal ileum (pseudomelanosis ilei), with stomach involvement being extremely rare. The lesion is benign but can appear similar to malignant melanoma on histology. We describe one patient with pseudomelanosis of the stomach and duodenum, followed by a brief discussion of this benign entity.
An 84-year-old man presented for follow up colonoscopy and esophagogastroduodenoscopy (EGD) after being treated for lower GI bleeding of unclear etiology and iron deficiency anemia. He also began hemodialysis at that time for management of end stage renal disease (ESRD). In addition to ESRD, his past medical history was significant for gastroesophageal reflux disease, constipation, type 2 diabetes, hypertension, hyperlipidemia, and prostate cancer status post-radiotherapy. His medications included metoprolol, carteolol, amlodipine, hydralazine, aspirin, simvastatin, cholecalciferol, senna, allopurinol, latanoprost and sevelamer. Aside from a one-time 100 mg IV push of iron sucrose during dialysis, he had not been receiving supplemental iron. He had a colonoscopy 5 years prior which was only significant for benign polyps.
EGD showed a hiatal hernia in the gastroesophageal junction, blackened patches and fine black spots in the antral mucosa, as well as fine black spots in the duodenal mucosa (Figure 1). Colonoscopy showed 7 benign sessile polyps (Tubular adenomas), multiple diverticula and internal hemorrhoids, but no evidence of melanosis (Melanosis coli) in the large intestine. Histopathological examination revealed coarse brown pigment in the lamina propria of the stomach and duodenum distributed extracellularly and within macrophages (Figure 2). Iron stain was positive in these regions, and stronger in the stomach than the duodenum (Figure 2). A clear etiology of the patient's lower GI bleeding was not discovered, although straining from constipation and internal hemorrhoids were suspected.
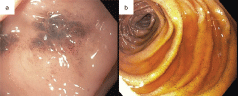 Figure 1: Endoscopic images of the stomach and duodenum A) The gastric mucosa has patchy black pigment but is otherwise unremarkable; B) The duodenum has finer, speckled black pigment.
View Figure 1
Figure 1: Endoscopic images of the stomach and duodenum A) The gastric mucosa has patchy black pigment but is otherwise unremarkable; B) The duodenum has finer, speckled black pigment.
View Figure 1
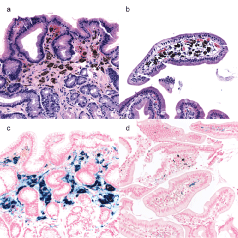 Figure 2: Pictomicrographs of representative stomach and duodenum A) The gastric antrum shows black submucosal pigment (H&E 40x); B) The duodenum shows similar submucosal pigment (H&E 40x); C) Iron stain highlights the antral submucosal pigment (Iron 40x); D) Iron stain highlights some, but not all the duodenal pigment (Iron 40x).
View Figure 2
Figure 2: Pictomicrographs of representative stomach and duodenum A) The gastric antrum shows black submucosal pigment (H&E 40x); B) The duodenum shows similar submucosal pigment (H&E 40x); C) Iron stain highlights the antral submucosal pigment (Iron 40x); D) Iron stain highlights some, but not all the duodenal pigment (Iron 40x).
View Figure 2
Melanosis of the lower GI tract (Melanosis coli), original described in 1829, is a common finding on colonoscopy [1]. It is uncommon in the duodenum and extremely rare in the stomach, described in 1976 and 2000, respectively [2,3]. In the large intestine, melanosis has been attributed to long term laxative use in patients with chronic constipation, presenting as lipofuscin deposits in the colon which may extend to the distal ileum [4]. More proximal involvement is distinct, consisting of ferrous sulfate as opposed to lipofuscin, and having a separate set of associated risk factors [4-6]. Melanosis in the upper GI tract is thus termed "pseudomelanosis". Gastric and duodenal pseudomelanosis are clinically inconsequential with no known long-term sequelae but are nevertheless striking and often unexpected on endoscopy and pathologic assessment.
The endoscopic and histologic features described in this patient are characteristic. Endoscopy typically shows speckled mucosal pigment, which is black to brown and spotty in distribution [6]. On pathology, there are pigment laden macrophages in the lamina propria of the involved stomach and segment of bowel [7,8]. Similar histology may be seen in malignant melanoma, hemosiderosis and charcoal ingestion. Of note, these characteristic features are not universally present. One study found the classic endoscopic appearance was only present in 35% of pseudomelanosis duodeni cases. Iron stain tends to be positive but was found to be negative in 18% of pseudomelanosis duodeni cases in the same study [7].
Chronic oral iron therapy has been suggested as one possible etiology of pseudomelanosis, as has antihypertensive medication use [7,9]. Interestingly, iron has been noted to be coupled with sulfur within macrophages in pseudomelanosis patients, which has been postulated to disrupt normal iron transport [5]. Drug-based sources of sulfur, such as antihypertensives, and non-drug-based sources of sulfur are likely responsible for this finding [7]. Less progress has been made on how other risk factors contribute to gastric and duodenal pseudomelanosis.
The patient had no significant history of supplemental iron use, aside from a single intravenous administration, nor evidence of upper GI bleeding as has been described in prior case reports. However, in addition to using antihypertensives, he had ESRD, hypertension and diabetes, all of which are reportedly associated with pseudomelanosis of the upper GI tract [8].
In summary, this 84-year-old man was found to have pseudomelanosis of the stomach and duodenum following workup for lower GI bleeding. He had multiple ailments thought to be risk factors for pseudomelanosis. His bleeding did not return, and he did well following his procedure and diagnosis.