Background: Medical students in clinical years are supposed to be independent, self-directed learner to motivate in depth learning. In response to COVID-19, medical education faculty have quickly transitioned to online formats that include COVID-19 crisis. The main purpose of this study was to assess the experience of clinical years' students with online-based learning during the COVID19 pandemic.
Method: A cross sectional survey-based study was carried out in two medical colleges. Data was collected on self-administered questionnaire satisfaction regarding clinical knowledge and skills gained via online-based learning. Statistical analysis was performed using SPSS (IBM SPSS Statistics 20.0). Data were expressed in frequencies, mean and percentages.
Results: Total 210 participants 50% from NUST and SQU, 71% female. Half of study participants (NUST-52.4% and SQU-60.0%) found online teaching ineffective. More than half of students (60.5%) experienced poor internet access. A total of 22.9% of students agreed and 50.5% of students were some extent agreed that they were able to achieve their objectives. More than two third (83.8%) or NUST and 61% of SQU students did not manage to achieve practical skills. In the questionnaire response, 88.6% of NUST and 69.5% of SQU students believed that online teaching is not sufficient to prepare clinical years students to become skilled future doctors. A significant difference (p-0.001) was observed between NUST and SQU student's responses.
Conclusions: Medical students in clinical years need in depth learning with maximum hands-on practice. The webinar teaching has impact on medical student education, affecting the practice and training. Students believed that online teaching in its current form is not sufficient to prepare clinical years students to become skilled future doctors.
COVID-19 pandemic, Clinical teaching, Medical students, Online teaching Oman
In the light of the emergency lockdowns and social distancing restrictions implemented by governments as a response to the COVID-19 pandemic, most educational institutions including schools, colleges and universities were shut close [1]. According to UNESCO, by April 1, 2020 about 194 countries had countrywide closure of schools while many other countries only closed schools in certain parts. This emergency response affected up to 93.1% of all enrolled learners globally (UNESCO, 2020) [2]. Nonetheless, the majority of these institutions turned to online platforms in an effort to adapt with the situation and to continue delivering proper education to their students. This trend was also adopted by most medical schools, applying it on pre-medical, pre-clinical and clinical years. Although some reports have shown that online teaching may have some advantages over traditional methods, it might not be the case for clinical education [3]. Clinical training is an essential requirement in any medical program, and it largely depends on bedside teaching and the interaction of student with faculty, patients, and hospital staff. Therefore, virtual teaching via online methods deprives students from much needed direct communication with patients and tutors. Hence, poses difficulties that prevent students from fulfilling their goals regarding their clinical education and prevent faculty from properly assessing students' clinical expertise [4,5].
Taking into account that pandemics, complete lockdowns and total closure of educational institutions are not very common situations, literature does not have many papers that studied the impact of these lockdowns or the shift to online-based learning on medical students, especially during the COVID-19 pandemic, as it is still a very new concern. However, the history did have some similar bouts in the recent past, like the SARS outbreak in 2003. The authors mainly focused on the response of medical schools to the outbreak of SARS, which included suspension of clinical teaching and further incorporation of technology in teaching [5,6]. However, most of these papers only outlined the responses of these medical schools and the strategies implemented to continue the teaching process. None of them actually addressed the issues students faced with the strategies applied. Moreover, a guideline, based on past and current responses were published to help medical schools plan for the process of curriculum delivery and continuation of teaching and training during this pandemic and similar situation in the future [7,8]. Additionally, a more specific guideline for the use of e learning in medical education is also available [9,10].
In an aim to explore the challenges that come along online-based learning, some papers pointed out the challenges of online learning in higher education in general. In 2018, an integrative review of more than 300 abstracts and full-text papers reported a group of barriers in online learning in medical education and suggested possible solutions [11].
The main purpose of this study was to provide a better understanding of the experience of clinical years' students with online-based learning during the COVID-19 pandemic. As this situation is no expected to end very soon and as similar situations could be expected in future, it is important to identify the challenges students faced, in order to come up with possible solutions to allow them to fully acquire the needed knowledge and skills. Identifying the limitations of online-based learning in comparison to traditional learning (classroom sessions and bedside teaching). Determining student's satisfaction about their clinical knowledge and skills they gained via online-based learning in comparison to their initial goals, determining what adjustments, regarding the curriculum, methods of online teaching and assessment tools would be helpful in improving their clinical expertise.
This is a cross-sectional study, conducted at National University of Science and Technology (NUST) and Sultan Qaboos University (SQU), Oman in relation to online-based learning in comparison to traditional learning and student's satisfaction about their clinical knowledge and skills gained via online-based learning among undergraduate medical students.
Data collected from undergraduate medical students using a self-filled questionnaire. A favorable ethical opinion was obtained from institutional ethics board and an informed consent was obtained from study participants. Survey instrument made after literature search and reviewed and agreed after several brain-storming sessions with study team members. Participants were asked to mark their response to each statement based on a 5-point Likert scale ranging from strongly disagree to strongly agree. The survey assessed various elements, including accessibility and communication challenges, theoretical knowledge and practical skills development through online-based learning.
Statistical analysis performed using SPSS (IBM SPSS Statistics 22.0). Data expressed in frequencies for questionnaire responses calculated for all variables in numbers and percentages. Independent sample t-test was applied to compare differences between continuous variables and X2-test was utilized for categorical variable. The level of significance set at 0.05.
A total of 210 participants were enrolled with mean age of 23.4 ± 1.2 (20 to 27 years) in which 61 (29%) were male and 149 (71%) were female. Equal number of participants were recruited from NUST and SQU. Female proportion was significantly (p < 0.001) higher in NUST (89.5%) then SQU (52.4%) study participants. Participants were asked about effectiveness of online teaching in delivering clinical knowledge and skills in comparison to traditional bedside clinical teaching. In both groups, almost half of study participants (NUST-52.4% and SQU-60.0%) found online teaching ineffective. No statistically significant difference was observed between both group responses (p-0.23).
In the questionnaire, students were asked multiple questions about accessibility and communication challenges during the period of online-based learning. More than half of students (60.5%) experienced poor internet access. Overall, no significant statistical difference was observed between NUST and SQU students' responses (p > 0.05).
In the questionnaire, participants were asked about their theoretical knowledge and practical skills. More than a half of the participants were agreed that they had access to all needed resources (books, case reports) and more than do not think that online-based learning alone is sufficient to acquire needed theoretical knowledge (Table 1). Overall, no significant statistical difference was observed between NUST and SQU students' responses regarding theoretical knowledge (p-0.32, 95% CI: -0.33-0.11) and practical skills (p-0.30, 95% CI: -0.25-0.08).
Table 1: Theoretical knowledge and practical skills (%). View Table 1
A total of 22.9% of students agreed and 50.5% of students were some extent agreed that they were able to achieve their objectives regarding their theoretical knowledge via online-based learning. However, 26.7% did not achieve their objectives regarding their theoretical knowledge via online-based learning (Figure 1). No significant difference (p-0.25) was observed between NUST and SQU student's responses.
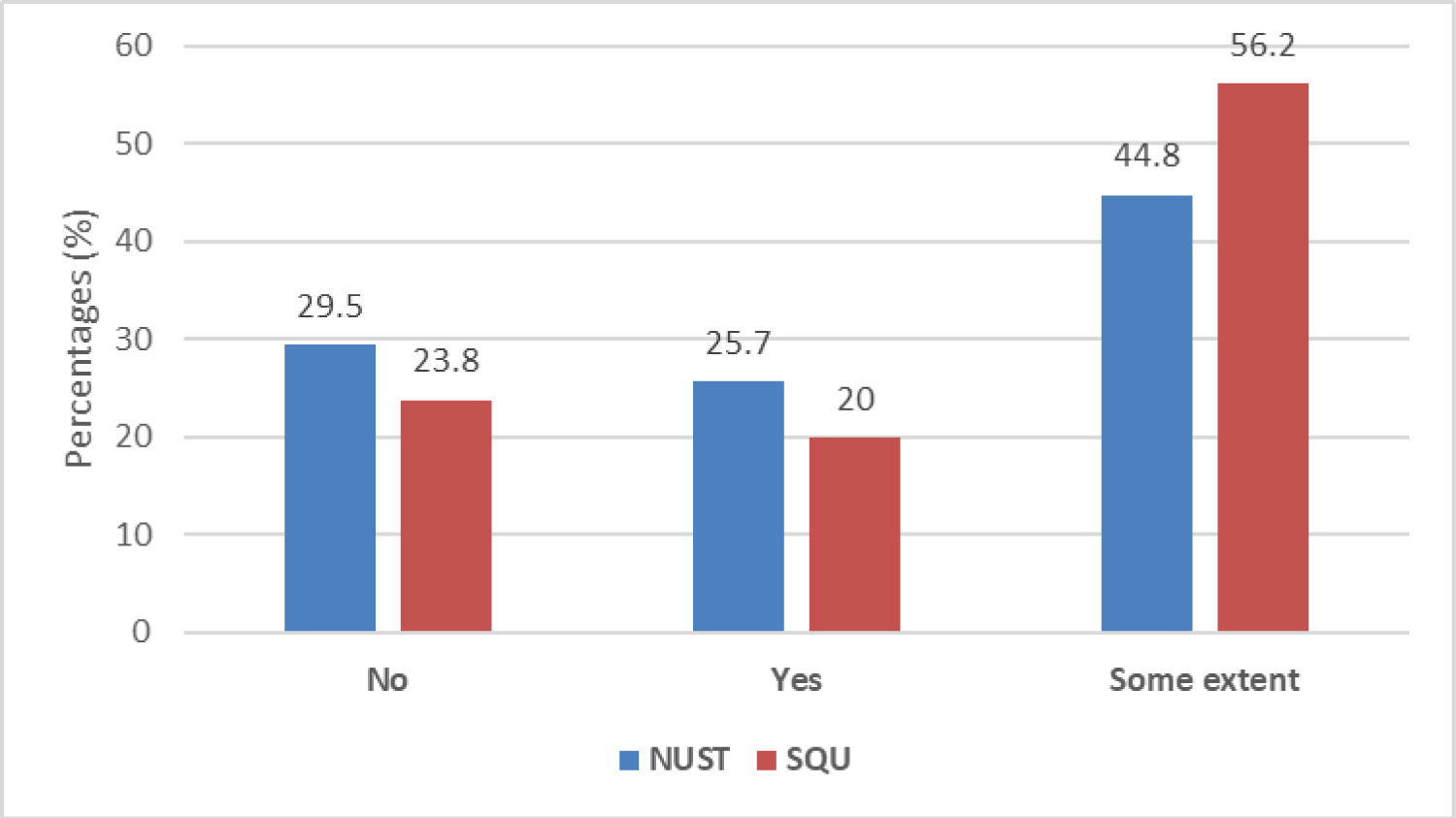 Figure 1: Theoretical knowledge by online-based learning.
View Figure 1
Figure 1: Theoretical knowledge by online-based learning.
View Figure 1
In the questionnaire, student were questioned if they were able to achieve their objectives regarding practical skills through online-based learning (Figure 2). More than two third (83.8%) or NUST and 61% of SQU students did not manage to achieve practical skills by way of online-based learning. In the questionnaire response, 88.6% of NUST and 69.5% of SQU students believed that online teaching in its current form is not sufficient to prepare clinical years students to become skilled future doctors. A significant difference (p-0.001) was observed between NUST and SQU student's responses.
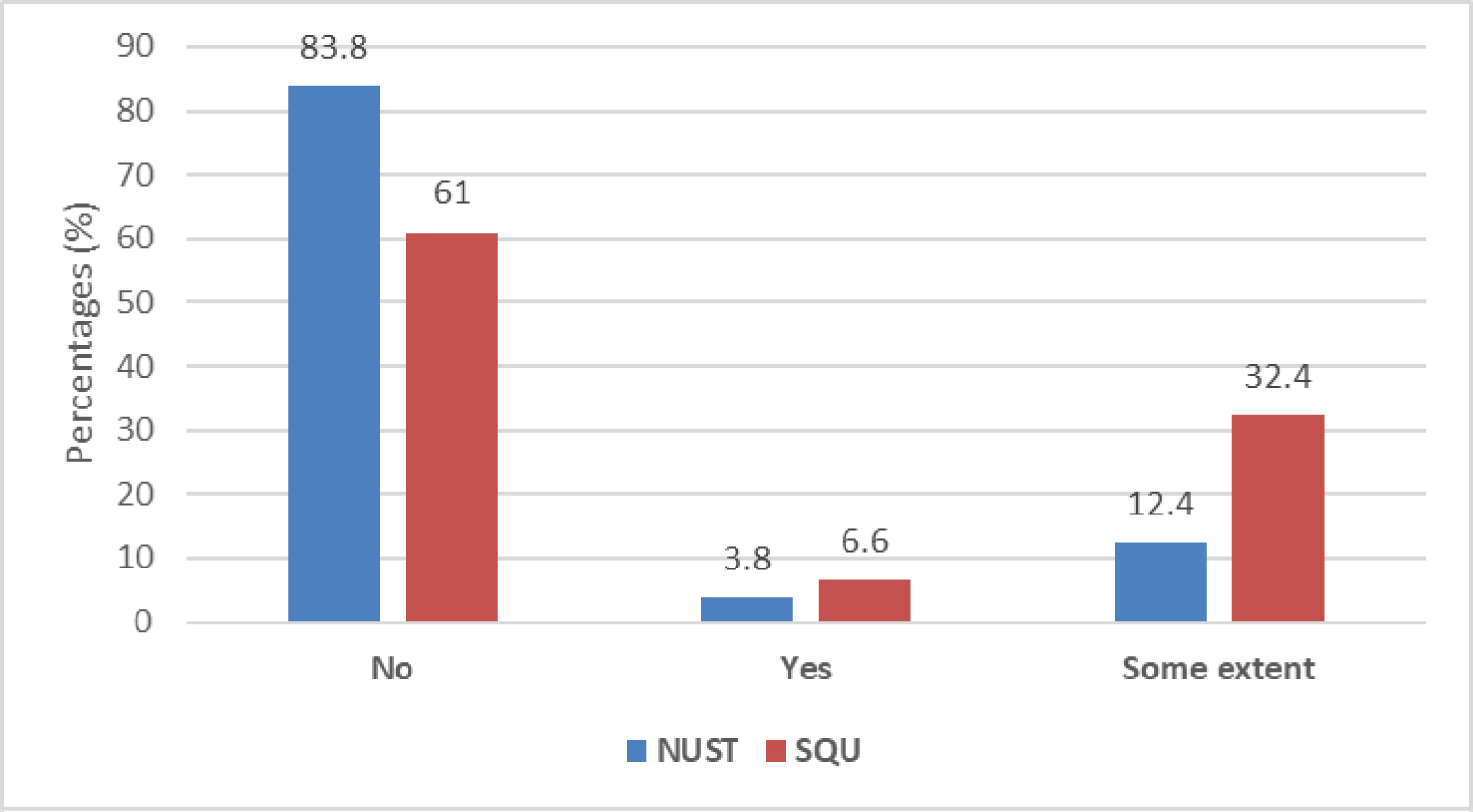 Figure 2: Practical skills by online-based learning.
View Figure 2
Figure 2: Practical skills by online-based learning.
View Figure 2
Clinical teaching is a form of interpersonal communication between a teacher and learner. It mainly involves a patient or a patient scenario; student learns how to evaluate a patient and manage the problem [12,13]. The ideal clinical teaching and learning is done in patient care area but because of COVID-19 pandemic outbreak all clinical and class room teaching is suspended [14].
Clinical teaching is a skill that must be practiced, teaching is more effective when learners identify educational needs and they are ready/motivated, take responsibility for their own learning. The teaching methods used in clinics and wards offer more diverse and effective educational opportunities [15,16]. Engaging students on webinar clinical teaching sessions is a challenging job. This mode of learning encourages students to control over their learning and allowing them flexibility over content and pace of learning [17,18].
The challenge students faced in our study internet issues and insufficient skills of student and faculty. Challenge lack of direct exposure to patient and faculty made them dis connected from real patients (Table 1). Wilcha has reported that in the times of the COVID-19 pandemic, continuation of teaching is crucial to enable the graduation of future physicians into society. The evidence suggests that virtual teaching is effective, and institutions are working to further develop these resources to improve student engagement (Figure 1). Alsharani, et al. reported in their study that educator's improved digital literacy and diverse and enriching experience extremely helpful for effective webinar teaching [19-21].
In this study students felt lack of practical skills is hindering them to achieve the goal and objectives of curriculum and cannot prepare skilled future doctor. Literature has reported that clinical year teaching is mainly self-directed learning however, teachers' guidance and feedback stimulates motivation and critical thinking process [22,23].
In our study students felt many challenges mainly internet issues, which was the main barrier in clinical teaching (Figure 2). Students reported that teaching is not effective as there is no exposure to patient and faculty as compare to live teaching in patient care. These challenging times may present a serendipitous opportunity for medical students to cultivate the personal attributes expected of a doctor in the face of adversity. The combination of recent telecommunication developments with current teaching methodologies may positively change the future landscape of medical education. Studies from Oman also support the evidence that students are very proactive in online teaching and learning and medical students have shown a positive attitude and motivation towards webinar clinical teaching [24-26].
In this study students felt more responsibility in learning however, lack of direct interaction only improved the theoretical knowledge and practical skills was not sufficient to gain on online teaching and learning. Literature has shown the same results suspension of clinical rotation during pandemic has effect on students' confidence and preparedness. Students need to maintain their wellbeing with safeguards such as proper inductions, support and supervision [27-30].
Medical education has been significantly affected by pandemic which might affect the transition from students to doctor. This study has shown that the disruption of clinical teaching has enormous effect on medical students' confidence although the teaching and learning was relevant but lack of practical skills is hindering them to achieve the goal and objectives of curriculum. Choi, et al. reported that the impact on medical students' assessment is significantly affected, as students' preparedness for examination was not appropriate during COVID pandemic [31].
There is a huge disruptive change to medical education in this pandemic and the use of technology has been rapidly and widely used to maintain appropriate teaching and learning. The goal and objective to achieve on online clinical teaching and learning needs more interactive sessions with case-based learning. Teaching and learning online on clinical cases were relevant because of their practicality but missing the human touch. The future challenge is, students to acquire knowledge more effectively and training medical competences and development of critical thinking, clinical decision-making skills which are essential for better patient care.
Authors declared no conflict of interest.
No funding was received for this work.