The aim of this systematic review was to review the recent literature regarding the effect of heat waves on mortality in elderly adults. A systematic search of the literature, was conducted by two reviewers during March 2018, using three electronic databases (PubMed, Web of Science, and Scopus). The PRISMA guidelines were used for the quality assessment of the published studies. The literature search identified a total of 345 articles, while only 24 studies met the inclusion criteria and were included in this analysis. Overall, the results from these studies show that, although recent advances in technology allow scientists to predict heat waves, thereby enabling health agencies to alert the public with heat advisories, the number of heat wave-induced deaths remains high. The underlying reasons for these increases in heat-wave-induced mortality remains unclear, highlighting the need for developing evidence-based thresholds for the activation and implementation of actions plans to protect the health of heat-vulnerable elderly populations.
Extreme heat events, Older, Aging, Deaths, Heat stress, Heat shock, Hyperthermia
Extreme heat conditions are considered a major threat for public health and can induce many health complications to the urban populations. With a predicted rise in the frequency and intensity of extremely hot weather due to changing climate, heat exposure is presenting an increasing challenge to the health and safety of heat-vulnerable populations such as elderly adults. Such extremes have resulted in the deaths of 70,000 in Europe in the summer 2003 [1] and 55,000 in Russia during the summer 2010 heat wave [2]. The immense burden placed on the health care systems worldwide as a result of these heat waves has been unequivocal [3]. When people are exposed to heat, especially when temperature remains atypically high for several days such as occurs during the summer months, they can suffer from potentially deadly illnesses such as heat exhaustion and heat stroke quickly [4]. Elderly with pre-existing health conditions are particularly vulnerable as exposure to even short periods of heat can aggravate their health conditions by worsening disease-specific symptoms [5]. Accordingly, a correlation between high ambient temperatures and negative health outcomes exists. Epidemiological evidence demonstrates a 2-5% increase in all-cause mortality for a 1 ℃ increase in average daily temperature during hot temperature periods [6]. However, extreme heat events occurring in spring or early summer pose an even greater threat to health in the elderly because of their lack of acclimation [7].
A heat wave is usually considered a prolonged period of excessive heat. According to Gasprarrini and Armostrong [8] a heat wave is defined as a period where for ≥ 2 repeated days the daily mean temperature is at or above the 98th percentile of the warm season daily mean temperature. Moreover, the intensity, the duration and the time in the season that it appears, are the main characteristics of each heat wave [8]. Moreover, as the rapidly aging population relocates to large urban centres to be closer to essential health and social care services, they are likely to experience some of the highest temperatures during hot weather periods. This is because of the urban heat island where temperatures within major metropolitan cities (e.g., London, England; Toronto, Canada, New York City, USA; Paris, France) can be as much as 10 ℃ greater than the surrounding rural areas [9-11]. These elevated temperature are primarily due to the design and density of buildings and by other manmade changes which includes asphalt roads and pathways, removal of trees, elimination of open green space areas, others [12].
Elderly persons are typically considered those who are aged 65 years or more [13]. Natural ageing can be characterized by a complex process, in which progressive age-specific deteriorations of internal physiological systems inevitably impair the body's capacity to respond appropriately to internal and external stressors [14-16]. As recent studies show, this includes deterioration in their ability to dissipate heat [17-19], a process pivotal in the maintenance of normal core temperature especially in extreme heat conditions. Specifically, older adults take longer to respond to increases in ambient air temperature than their younger counterparts [20]. This response is due to age-related reductions in heat loss responses of sweating [21,22] and skin vasodilation [23-27], which are paralleled by marked impairments in the whole-body heat dissipation [18], and occur independently of the individual's level of acclimation [23]. As a consequence, elderly people are less heat tolerant and are at an increased risk of heat-related morbidity and mortality [17,28].
Given the fact that the population over age 65 years is steadily increasing [29] the numbers of heat related illnesses and deaths are likely to rise exponentially. Accordingly, there has been an increased urgency to address this important public health issue. This is evidenced by the fact that the number of articles (total of 507 based on search term "heat wave mortality" and "elderly") published in PubMed are appearing with increased frequency (~16 articles per year) over the past five years (Figure 1). Experts suggest that appropriate health prevention and management programs could greatly limit heat-related morbidity and mortality in heat vulnerable populations such as the elderly [30,31]. To contribute towards addressing these concerns, the aim of this systematic review was to review the recent literature regarding the effect of heat waves on mortality in elderly adults.
 Figure 1: Evolution of Publications that revealed using the keywords of "heat wave mortality" and "elderly" clearly showing a growing interest in this field. A total of 223 articles appeared with increasing frequency through time reaching a peak of 16 articles/year during the past seventeen years.
View Figure 1
Figure 1: Evolution of Publications that revealed using the keywords of "heat wave mortality" and "elderly" clearly showing a growing interest in this field. A total of 223 articles appeared with increasing frequency through time reaching a peak of 16 articles/year during the past seventeen years.
View Figure 1
The current review included epidemiological studies that report on epidemiological data regarding the effect of heat waves on elderly mortality. A systematic search of literature was conducted by two reviewers during March 2018 using three electronic databases (PubMed, Web of Science and Scopus). The PRISMA guidelines were used for the quality assessment of the published studies [32]. Studies were selected using inclusion and exclusion criteria. Studies were included in the study if: 1) Results for elderly mortality rates during heat waves were presented; 2) Results for the effect of "heat waves" on "elderly mortality" as a sub-population were reported; and 3) The study was written in English. Studies were excluded when they: 1) Did not present the number of deaths during "heat wave" periods but only the relative risk for mortality or models for the daily mortality prediction; 2) Did not evaluate the elderly mortality but mortality rates in other age groups and 3) Were studies published only in abstract form. Studies identified in the search were initially examined using the information presented in the title and abstract. Thereafter a full evaluation of the full-text copy of the article was conducted to determine if it met all inclusion criteria.
A total of 345 articles were identified in the search. Of these, 85 full-text articles were reviewed for eligibility and only 24 studies met the inclusion criteria (Figure 2). Articles were excluded for the following reasons: 12 referred to animal, pregnancy, and infant mortality during heat waves; 22 examined the impact of heat waves mortality on specific chronic diseases; 5 studies were review articles only; 16 studies evaluated the relative risk of mortality or presented models for the prediction of daily mortality; 6 studies evaluated the impact of heat waves in different aged groups but no on elderly. The 24 studies included in our review provided estimates of heat-related mortality in the elderly during heat waves that encompasses different geographically locations (Figure 3 and Table 1).
Table 1: Epidemiological studies on elderly mortality during heat waves. View Table 1
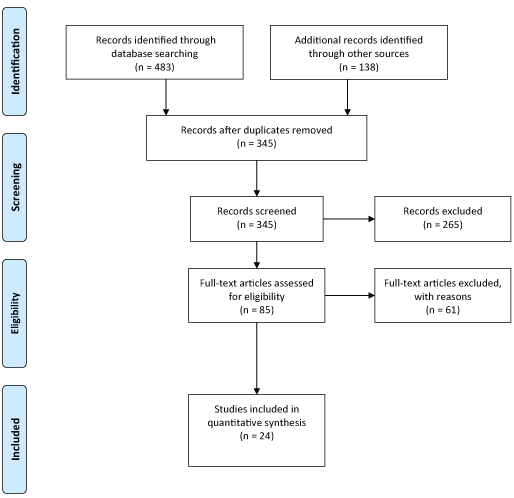 Figure 2: Flowchart of the progress of the literature screening.
View Figure 2
Figure 2: Flowchart of the progress of the literature screening.
View Figure 2
 Figure 3: Geographical areas (marked with light blue) where the elderly mortality rates have been assessed in the studies evaluated in the current review.
View Figure 3
Figure 3: Geographical areas (marked with light blue) where the elderly mortality rates have been assessed in the studies evaluated in the current review.
View Figure 3
The majority of the identified studies examining the effects of heat waves on mortality in the elderly present epidemiological data based on the European heat wave of 2003, when temperature extremes were observed in many parts of Europe over a prolonged period varying from 10 days to one month [33]. Accordingly, an epidemiological study by Conti, et al. [34], which examined the impact of heat wave in 21 different regions in Italy, found that the number of deaths among people of 75 years of age and older increased by 21.3% during the heat wave occurring in 2003 compared to 2002, with similar mortality rates between men and women. However, the authors identified locations of high-risk such as in north-western cities of Italy where higher mortality rates were observed [34]. More precisely, elderly mortality rate was highest in Turin (44.9%), Trento (35.2%), Milan (30.6%) and Genoa (22.2%), which are generally characterized by cold weather [34]. The authors hypothesized that the underlying reason for this disparity was acclimatization, since hot weather in the aforementioned cities is less common and, thus, inhabitants are less likely to be tolerant to high temperatures. Indeed, another study by, D'Ippoliti, et al. [35] showed that cities in the Mediterranean region such as Athens Greece, which experience higher average ambient temperatures during heat waves, have a reduced mortality rate in the elderly as compared to more temperate northern European cities such as London, England [35]. This finding has been attributed to more frequent exposure to temperatures extremes and generally higher day-to-day ambient temperature conditions [36,37]. As shown by Lan, et al. [38], heat adaptation may be a more important determinant of heat-related mortality in heat vulnerable populations than previously thought. They reported a marked surge in mortality rate in older adults during the 2010 heat wave (> 35 ℃) in the large metropolitan city of Harbin, China, which typically experiences cool ambient temperatures (- 18 ℃ to 23 ℃) during the summer period. The authors surmised that the residents were likely less heat acclimated and consequently were at greater risk of heat-related illness or death [38]. In contrast, Åström, et al. [39] showed no differences in daily number of deaths (as assessed between the months of May through to September (the 15th of each month) from 2002 to 2008) in older adults (≥ 50 years) living in Rome and Stockholm, two very distinct regions in terms of climate type. In fact, the population of older adults were found to be equally vulnerable to detrimental health effects of a heat wave.
Another important determinant is the time of year that the heat waves occurs. When extreme heat events occur in late spring or early place, accordingly the elderly are at an increased risk of a heat-related injury or death. This is because they have not benefited from improvements in heat dissipation that occur with progressive exposure to heat that would typically occur over the spring and summer period [4,40]. Indeed, heat vulnerable individuals are likely to gain some level of acclimation by the mid-to-late summer period that would provide some level of protection against the detrimental health effects of exposure to extreme heat conditions [4,40]. Smoyer [41], who compared the elderly mortality rates during two different heat wave periods, showed that although the higher ambient temperature was recorded in Missouri during an August heat event (1995), the number of deaths in July was comparatively higher despite a relatively lower ambient temperature. In addition, Son, et al. [8], who examined the impact of heat waves on mortality rates across various age groups in seven cities in Korea, showed that a one day delay in the occurrence of the heat episode was associated with a 0.2% reduced in the risk of a heat-related death.
Conti, et al. [34] showed that heat-related mortality in the elderly is also influenced by the duration of the heat wave. Similarly with the study by Conti, et al. [34], in Frankfurt, Germany the numbers of deaths during the heat wave in 2003 were high (32.7 case per day for a period of 11 days) and the following heat wave periods that occurred in the next decades did not reach these numbers [42]. However, this can be explained in large part by the fact that the duration of 2003 heat wave was 12 days as compared to the relatively shorter heat waves (4 days in 2006, in 2010 and in 2015), albeit of comparable intensity occurring thereafter within the recording period [42]. These findings highlight the cumulative effect on human health that can occur with prolonged heat events.
Since the European heat wave of 2003, extensive work has been done to implement appropriate heat alert systems as well as heat management strategies to protect the vulnerable populations. The implementation of these protective strategies appears to be having a positive impact on population health. This is evidenced by a study by Green, et al. [43] who found a relative reduction to prior events during the heat wave of 2013 (from 1st of June until 15th of September) [43]. These findings were thought to indicate that health officials in England had implemented health protection measures and prevention strategies that were successful in alleviating the level of thermal strain experienced by the elderly during the heat wave. The mean daily central England temperature was 22.7 ℃ with a peak recorded temperature of 29.7 ℃. Given that temperatures in South European countries typically range above this level, it becomes clear that lack of acclimatization plays an important role in elderly heat waves-induced mortality in England.
A comparable pattern of response was also reported by Borrell, et al. [44], who showed that elderly women in Barcelona, Spain had a significantly greater mortality rate relative to men, indicating that the sex plays an important role in heat wave mortality. According to the authors, the main reason for this finding was the fact that in Barcelona the rate of women older than 75 years living alone is higher compared to men (13% of men and 30.9% of women). Moreover, another key factor, which was responsible for the increased mortality was the socioeconomic status as individuals with low educational level showed increased number of deaths. Similarly, Bogdanovic, et al. [45] reported higher mortality rates in women 75 years of age and older compared to their age-matched male counterparts [45]. They attributed these results to the greater life expectancy for women compared to men [45]. Indeed, it is well established that women live 5 to 10 years longer than men [16]. Noteworthy, Diaz, et al. [46] who analysed the health-effects of summer heat waves on mortality rates in the elderly (> 65 years) in Madrid, Spain for the period of January 1, 1986 to December 31, 1997, showed that for every degree the temperature rises above 36.5 ℃, the rate of mortality increased by as much as 28.4% with women being again the most vulnerable [46].
It has been suggested that ethnicity and skin color does not play a role in elderly mortality [47], while others found that people of African origin are at higher risk of a heat-related death [48]. Madrigano, et al. [49], showed that African non-Hispanic individuals were more likely to die during to heat waves. However, the differences were likely due to the disparity in socioeconomic status and not skin color. Indeed it has been shown, as previously reported, that low socioeconomic status is associated with an elevated risk for a heat-related death [49].
In general, extreme temperatures can have dramatic consequences on human health. Prolonged exposure of elderly adults to heat wave can induce hyperventilation, dyspnea, dehydration [50], as well as cardiovascular events [51]. Heat-induced aggravation of underlying cardiovascular and respiratory conditions is considered a key factor increasing excess mortality during heat waves [52-54]. A number of studies are in agreement that the elderly populations are the most vulnerable to detrimental health effects of heat waves due in large part to their impaired ability to dissipate heat and therefore regulate body core temperature [28]. This is exacerbated by the fact that elderly individuals have a reduced thirst sensation and experience greater levels of dehydration [55], which is exacerbated by medication use. However, apart from age, the socioeconomic and educational status seems to play a role, because people with low socioeconomic and educational status proved to have greater risk of mortality [53,56,57,]. For example, during heat waves access to centers or buildings with air-conditioning plays an important role in circumvent the risk of heat-related illness and deaths in vulnerable populations. Residences or buildings without air conditioning can reach excessively high ambient temperatures that can exceed the physiological adaptive capacity of vulnerable population groups [58,59]. Indeed, studies show that the number of deaths during heat waves increases for people outside hospitals compared to people in hospitals who have access to air-conditioned facilities [57,60]. In addition, in large cities where the density of the buildings is high, the temperatures are even more increased compared to the countryside, creating the well-known heat island effect [61,62]. Furthermore, it has been found that elderly people who live in places with little green-space and/or in old buildings are more vulnerable to heat mortality [63]. Moreover, the low economic status could lead to limiting access to health care departments, and this could in turn increase the risk for heat wave mortality [59]. Finally, it has been found that when elderly adults are exposed to high temperatures during the day and nighttime for several days continuously, heat-related mortality increases. This is likely due to the prolonged nature of the exposure where the individual is unable to recover adequately during the typically cooler night period [64].
As temperatures continue to rise due to the climate change, the frequency of heat waves will likely increase in the future [61]. Although the recent advances in technology allow scientists to identify when extreme weather temperatures will occur in the different regions and public messaging of heat related events has improved over the past decade, the number of deaths due to heat wave mortality remains high. The underlying reasons for this trend is unclear albeit better education and increased awareness of the detrimental health effects of heat waves may help reverse this trend. Considering all these factors, additional policy actions are required to enhance the public health awareness regarding the deleterious effects of heat waves on human health. Finally, the results of all these studies strengthen the need to review and update heat waves mitigation plans in each country as well as the need for National Health Departments to develop new prevention strategies in order to protect the people and minimize the consequences of extreme heat. Moreover, in many regions the reason for the heat waves mortality was the acclimatization and accordingly strategies that could reduce this risk should be developed. Thus established systems for preventing the effects of heat waves should be developed and implemented across the world.