The presence of gas in joints or soft tissues is usually indicative of infectious pathology or degenerative diseases [1]. However, the presence of gas inside the medullary canal in the diaphysis of long bones is an uncommon condition, and it is often associated with fractures or previous surgeries.
We present the case of a 29-year-old man who suffered an open supraintercondylar femur fracture, treated with debridement, surgical scrub with saline solution, and stabilization by external fixator, and in a second stage with a definitive osteosynthesis, which after being washed with pressure gun presented abundant intramedullary gas non-related to infectious pathology but possibly related to a pulsatile jet lavage during surgery.
The patient is a 29-year-old man with no history of interest, who was taken to our hospital on November 2015 approximately one hour after suffering a high energy traffic accident. He was a motorbike rider hit by a car riding at high speed. He was received at the emergency department where advanced life support measures were applied. After the stabilization of the patient, the body-CT showed contusive focus in both pulmonary bases, discarding other internal emerging lesions.
In the radiological series, we identified an AO32-B2 (3: femur; 2: diaphyseal; B: with a wedge fragment; 2: bending wedge) fracture of the left femur, an open AO33-C2 (3: femur; 3: distal; C: complete articular fracture; 2: articular simple, metaphyseal multifragmentary) supraintercondylar fracture of the right femur with Gustilo-Anderson type IIIA (Figure 1A), and an AO34-C1 (3: femur; 4: patella; C: complete articular; 1: transverse) non-displaced fracture of the right patella. Extensive wound cleaning was immediately performed at the emergency department, with manual irrigation using saline solution, as well as debridement of the most superficial contaminant material and temporary approximation of the wound edges. According to our hospital open fracture protocol, intravenous antibiotherapy was initiated with cefuroxime 1 g every 8 hours for 3 days and gentamicine 240 mg every 24 h for 3 days.
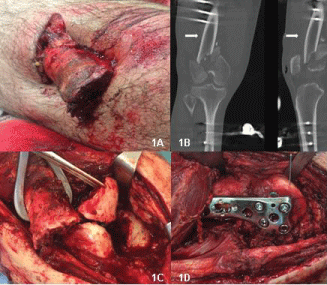 Figure 1: A) Image of the open fracture grade IIIA, with exposure of the femoral diaphysis; B) CT after the external fixation, with bone windowing, confirming a supraintercondylar fracture of the right femur and a non-displaced transverse fracture of the right patella. Isolated, subtle air bubbles can be depicted in the adjacent soft tissues, but not into the medullary canal of the femoral diaphysis (arrows); C) Intraoperative images where the supraintercondylar fracture is exposed; D) Definitive osteosynthesis with a condylar plate.
View Figure 1
Figure 1: A) Image of the open fracture grade IIIA, with exposure of the femoral diaphysis; B) CT after the external fixation, with bone windowing, confirming a supraintercondylar fracture of the right femur and a non-displaced transverse fracture of the right patella. Isolated, subtle air bubbles can be depicted in the adjacent soft tissues, but not into the medullary canal of the femoral diaphysis (arrows); C) Intraoperative images where the supraintercondylar fracture is exposed; D) Definitive osteosynthesis with a condylar plate.
View Figure 1
He was taken to the operation room where we conducted first an antegrade intramedullary nailing of the left femur with a Synthes Expert femoral nail, using a traction table. Secondly, on the right femur, we performed a resection of the wound edges according to Friederich, a debridement of the contaminating deep tissue and the fracture focus, manual wound cleaning with saline irrigation, and temporary fixation of the supracondylar fracture with an external fixator (Hoffman II, Synthes). Given the fact that the patella fracture was non-displaced, there were no more surgical procedures.
Subsequently, a CT scan of the right knee was performed in order to complete the preoperative studies so we could make a good surgical planning (Figure 1B), which did not show any intraosseous air bubbles. After a favorable evolution of the soft tissues of the right femur, four days after the accident we did another manual wound cleaning with saline, a resection of the devitalized tissue, an open reduction (Figure 1C), and a definitive osteosynthesis with bicondylar cannulated screws and a plate (VA-Condylar, Synthes®, Figure 1D) through an anterolateral subvastus approach. The osteosynthesis of the patella fracture was performed with a percutaneous cannulated screw to favour early mobilization.
During the postoperative evolution, the patient initiated the passive rehabilitation with Kinetec on the right leg until 60° of flexion, and total charge and total active range of movement was allowed on the left leg, but it was interrupted because he had a fever episode with an active exudation through the surgical wound, from which samples for culture were taken. He needed surgical debridement obtaining purulent articular material that was cultured. Afterward, we did a wound cleaning with 12 liters of saline irrigation using a pressure gun (Cleanest TM) wich suctions the liquid at the same time. In the immediate postoperative period, we initiated empirical treatment with intravenous linezolid 600 mg/12 h and voriconazole 400 mg/12 h. Subsequently, we withdrew voriconazole due to the growth of an E. faecalis in both cultures, preoperative and intraoperative. The Enterococcus was isolated, with no growing of any other bacterial species. We changed linezolid for intravenous ampicillin 2 g/6 h according to the antiobiogram, and we added rifampicin 600 mg/12 h, as he was carrying osteosynthesis material. The local evolution was correct, with an initial rehabilitation without pain and keeping wounds without exudation. However, he presented again a fever episode. After doing cultures of all possible focus (Urinary, Chest, Hemoculture), ciprofloxacin-sensitive Klebsiella pneumonia grew in the urine, so we initiated a directed antibiotherapy with oral ciprofloxacin 500 mg/12 h for 10 days.
However, given the concern of the medical team due to the possibility of the existence of another infectious focus at the level of the fracture concomitant to the urine infection, a second CT scan of the knee was performed (Figure 2). We objectified the presence of an important amount of intramedullary gas. This was discussed with the Infectious Diseases Unit considering the possibility that the gas was secondary to an infection. Nevertheless, given the good clinical evolution and once the UTI (Urinary Tract Infection) was treated, the proper postoperative local evolution, the absence of collections in CT scan, and the unique finding of gas in the thigh (which, in turn, didn’t seem to be related with the isolated germ, as the enterococcus is not a gas producer), we decided to perform watchful waiting under active clinical-analytical surveillance, removing all antibiotic therapy after 12 days.
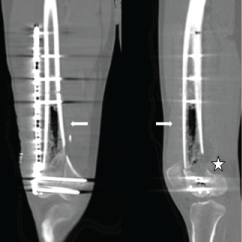 Figure 2: Last CT in coronal (left image) and sagittal (right image) planes with bone windowing, at the same level than Figure 1. A wide presence of air into the medullary canal of the right femoral diaphysis can be depicted (arrows). A posterior cortical defect is shown (next to the star).
View Figure 2
Figure 2: Last CT in coronal (left image) and sagittal (right image) planes with bone windowing, at the same level than Figure 1. A wide presence of air into the medullary canal of the right femoral diaphysis can be depicted (arrows). A posterior cortical defect is shown (next to the star).
View Figure 2
Given the good clinical, functional and analytical evolution of the patient, we considered that the finding of gas in the CT scan performed after the debridement by enterococcus was a "casual" finding not related to the germ that produced the infection, which may be a result of cleansing with a pressure gun. The evolution was favorable, with an articular balance of flexo-extension 20°-0° during the immediate postoperative, without repeating fever episodes and keeping a good appearance of the wounds. After a year of follow-up, the articular balance is of 70°-0°, without pain, and with an autonomous gait without assistance.
The presence of air into the joints, named as "vacuum phenomenon" is defined as a radiolucent collection representing gas that appears at sites of negative pressure [2]; the gas comes out of solution because of the reduced pressure. This phenomenon can be a normal finding on radiographs of various joints. It may also be a sign of disease, such as intervertebral disk degeneration on vertebral body osteonecrosis. Gas aspirated from the nucleus pulposus has been shown to consist of nitrogen.
Moreover, in the absence of penetrating trauma, intracapsular gas bubbles in CT (Computerized Tomography) have been found such reliable indicators of recent hip dislocation and may be the only objective finding of this injury [3].
The presence of gas into the joints or soft tissues was first described in 1981 by Ram CR, et al. [4] stating that, in the absence of trauma that would justify the entry of gas into the bone tissue, the intramedullary gas is the result of microorganisms infiltrating the bone secondary to infections surrounding soft tissues, thus infecting the medullary cavity. Osteomyelitis with an extramedullary gas formation is usually generated by anaerobic microorganisms [1], and it is not uncommon to visualize them in complementary tests which help us with the diagnosis. There have also been cases of polymicrobial osteomyelitis [5], among which anaerobic germs were included. The most common locations are the pelvis, tibia, fibula, femur and vertebrae [6] and sometimes they are related to diseases such as lymphangiomatosis, necrosis, neoplasia, fractures, penetrating trauma, or previous surgeries [7], or even in relation to gaseous gangrene in diabetic feet [8].
Other causes of intraosseous gas are the exceptional pneumocysts [9] which are described as air-filled cavities inside the bone. Normally they are accidentally discovered, but they can be mistaken with aggressive lesions. Within their low frequency, they are usually located in those vertebrae affected by degenerative diseases, although they can also be found in joints that have been subjected to traction [10], since it generates a negative intra-articular pressure that favors the gas accumulation inside the joint.
The different joint or medullary canal irrigation techniques are being studied [11], comparing conventional methods versus the incorporation of new techniques in which pressure systems are used [12] with good postoperative results, although it is yet to define which systems are the better to provide more benefits while minimizing risks. So far, the pulsatile pressure cleaning are not exempt of complications, as there have been described the compartmental syndrome [13], pulmonary air embolisms [14], etc., while it has also been observed that these new technologies can reduce the risk of fat embolism and improve the performance of surgical debridement [15] by reducing the recurrent index of infections.
In Luey, et al. [5], it is stated that the presence of endomedullary gas in the axial skeleton is pathognomonic for emphysematous osteomyelitis. However, in our case, the existence of intramedullary gas was not secondary to an infection or pneumocysts. The CT scan performed before the definitive surgery didn’t show any intra-articular or interosseous collection, neither gas inside the joints or the surrounding tissues, after having performed a manual cleaning with saline irrigation. Following the pulsatile debridement with a pressure gun that was required after an infection by E. faecalis (the only time when pressure cleaning was performed) we did a new CT scan in which we could observe gas inside the joint and the medullary canal. There was no evidence of radiological signs of osteomyelitis and, given the absence of clinical symptoms characteristic to this pathology, the absence of gas production by E. faecalis, and the support of complementary tests, the presence of intramedullary gas could be attributed to the use of irrigation with a pressure gun.
In the case presented here, and as seen in the picture Figure 2, his femur presented a posterior metaphyseal cortical defect that could favor the entrance and spread of air through the diaphyseal canal. We can conclude that, in the presence of intramedullary gas in imaging tests as the only finding, without clinical and analytical alterations which could suggest an infection, the use of a pressure gun for a pulsatile intrasurgical cleaning must be considered as a possible mechanism responsible for the existence of air at the level of soft tissues and inside the medullary canal. Of course this conclusion should be made after discarding most common causes of intramedullary bone gas, besides infection, like penetrating trauma, pneumocysts or emphysematous osteomyelitis.