Salmonella infection is significantly common in sickle cell patient compared with general population. Salmonella osteomyelitis in sickle cell patient is typically seen in the diaphysis of the long bones. We are presenting a case of salmonella spondylodiscitis in a homozygous sickle cell patient. The organism was isolated from the spine and was managed conservatively with antibiotic therapy as per susceptibility result. The treatment was guided by clinical and laboratory response.
Salmonella, Sickle cell disease, Spine, Osteomyelitis
SCD: Sickle Cell Disease; VOC: Vasoocclusive Crisis; IV: Intravenous
Sickle cell disease (SCD) is a hereditary blood disorder characterized by formation of hemoglobin S. It is a major public health problem, caused by mutation in β-globin chain of hemoglobin, resulting in glutamic acid being substituted by valine amino acid [1]. SCD is associated with significant morbidity and mortality. Patients with SCD carry more risk of developing complications including vasoocclusive crisis (VOC), fatal acute chest syndrome, splenic infarction, hemolytic crisis and osteomyelitis [2].
Salmonella osteomyelitis is more common in sickle cell patients. Although Salmonella osteomylitis in sickle cell patient is commonly diagnosed in long bones, only few cases of spinal Salmonella infection has been described [3-5].
We are presenting a case with brief review of literature on lumbar Salmonella spondylodiscitis in SCD.
A 13-year-old boy with homozygous SCD, presented to our hospital with chronic moderate low back pain and intermittent fever. The back pain radiates to left lower limb. There was no history of urinary or bowel incontinence. He was admitted under hematology care two months before his presentation with bacteremia and chest infection. Blood culture revealed Salmonella and he was treated with intravenous (IV) ceftriaxone.
Upon presentation to our hospital, his clinical examination revealed high temperature of 38.3 °C and positive bilateral straight leg test at 60 degrees. There was no back tenderness and no neurological deficits.
At presentation, the leukocyte count was 14, ESR 115 and CRP was 93. The plain radiograph was not clear due to bowel gasses, but revealed possible erosion at L5/S1 with decrease in intervertebral disc space and sclerosis (Figure 1). MRI showed L5/S1 spondylodiscitis with intravertebral collection (Figure 2). The patient under went CT-guided biopsy and blood culture was also performed. Given the clinical and past history of Salmonella infection, the diagnosis of Salmonella spondylodiscitis was suspected. The diagnosis of Salmonella was confirmed by biopsy culture which grew Salmonella livingstone sensitive to cotrimoxazole, ampicillin, ceftriaxone and chloramphenicol. The blood culture result was negative. He received four weeks of ceftriaxone and two weeks of oral ciprofloxacin. His CRP has normalized three weeks after starting the antibiotic therapy.
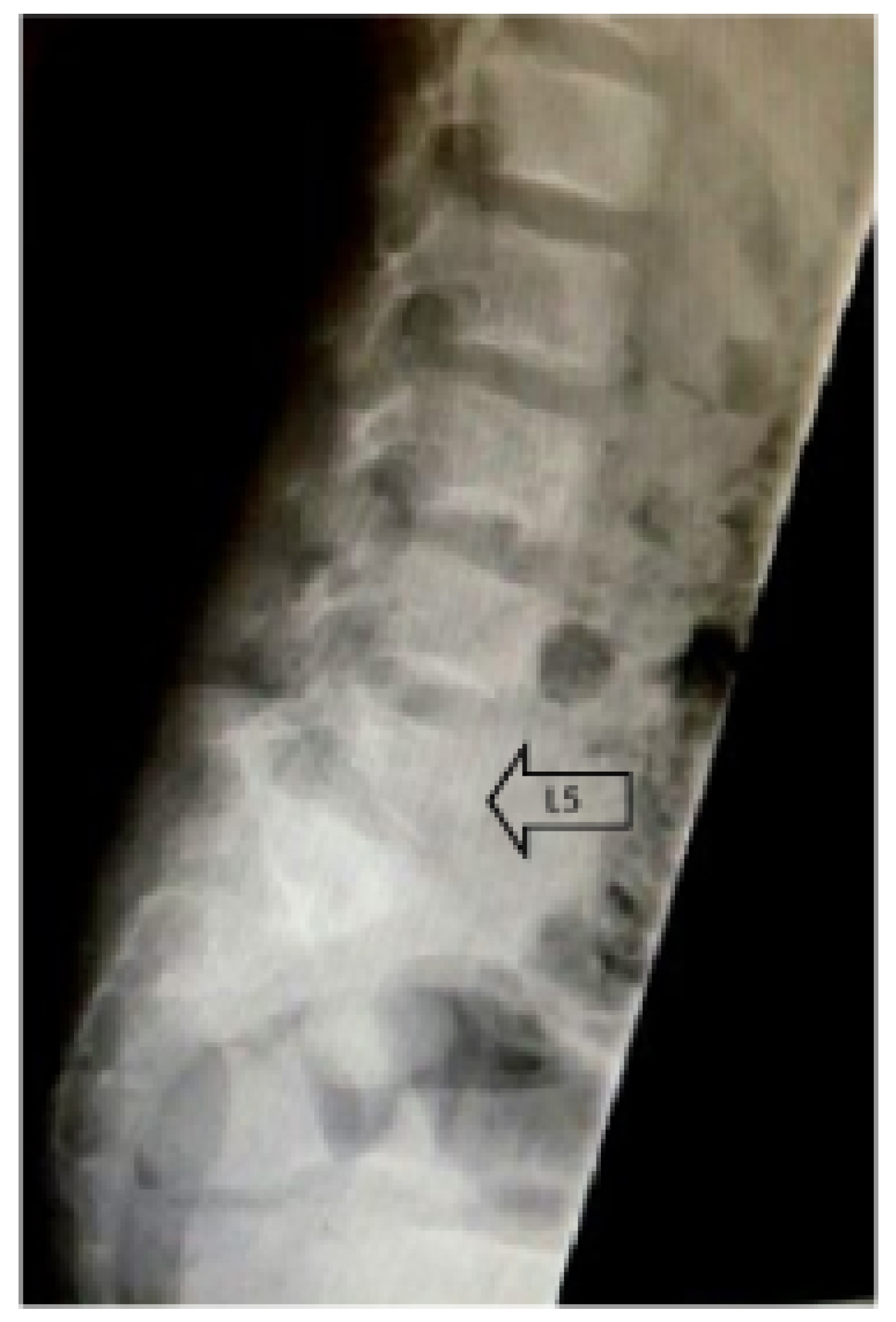 Figure 1: Lateral radiograph of the patient showing loss of L5 height and decrease in intervertebral disc space of L5/S1 and erosion of the endplates.
View Figure 1
Figure 1: Lateral radiograph of the patient showing loss of L5 height and decrease in intervertebral disc space of L5/S1 and erosion of the endplates.
View Figure 1
 Figure 2: Sagittal T2 weighted MRI showing loss of height and abnormal heterogenous signal intensity of L5 vertebral body and intervertebral disc (white arrow). It also shows abnormal marrow signal intensity involving L3, S1 and S5 vertebrae which are likely represents changes related to sickle cell disease (black arrow).
View Figure 2
Figure 2: Sagittal T2 weighted MRI showing loss of height and abnormal heterogenous signal intensity of L5 vertebral body and intervertebral disc (white arrow). It also shows abnormal marrow signal intensity involving L3, S1 and S5 vertebrae which are likely represents changes related to sickle cell disease (black arrow).
View Figure 2
The patient was seen two months after discharge and he was relatively asymptomatic and his follow-up radiograph showed healed sclerosis at L5/S1 level (Figure 3).
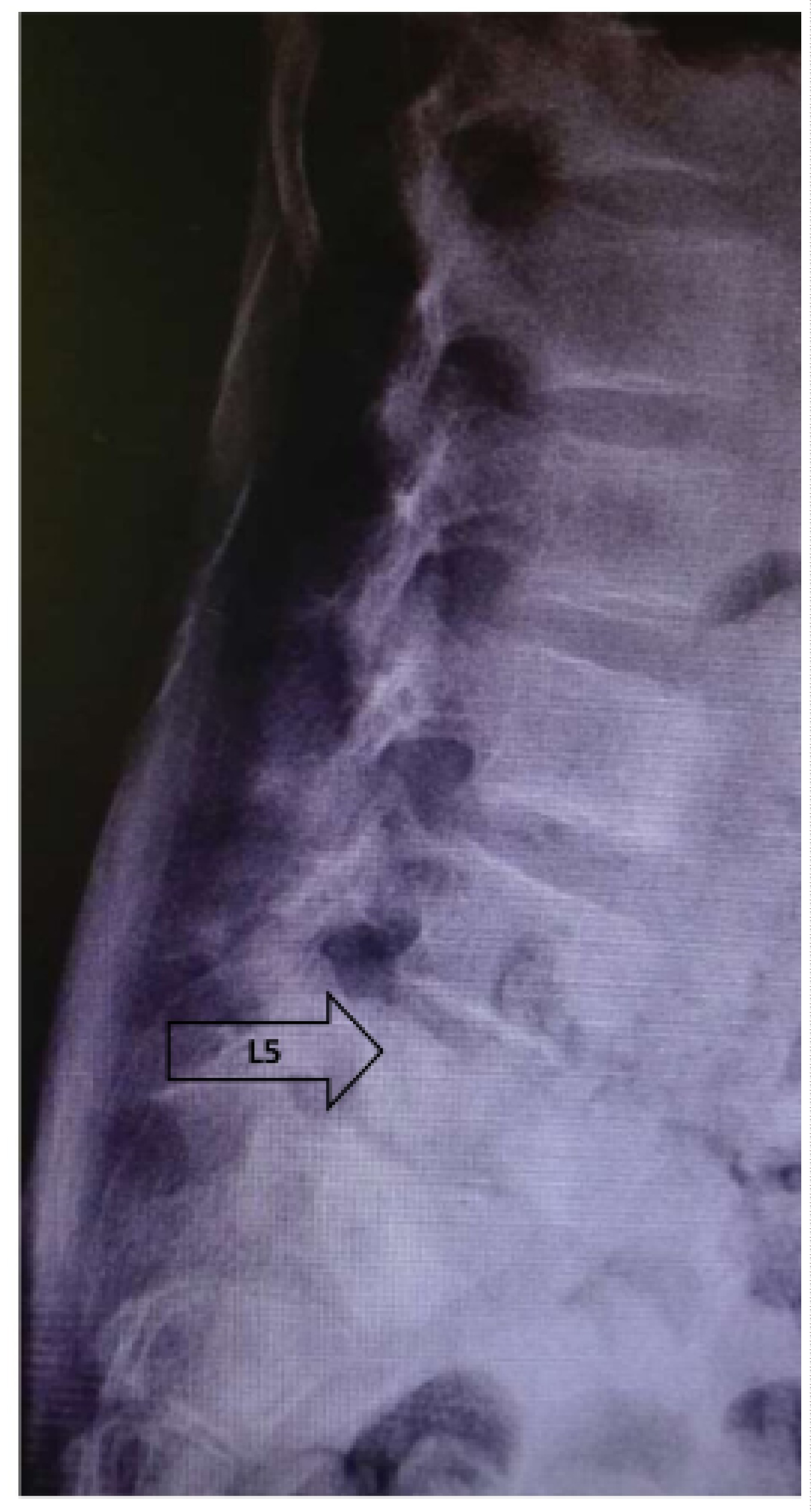 Figure 3: Follow-up lateral view radiograph revealed healed L5 vertebra.
View Figure 3
Figure 3: Follow-up lateral view radiograph revealed healed L5 vertebra.
View Figure 3
SCD is known to have profound and significant implication on the spine. The spinal manifestations of SCD can be acute or chronic, and includes spinal VOC crisis, infection, vertebral infarction, compression fracture and osteoporosis [1,6].
Infection is considered a major cause of morbidity and mortality among patients with sickle cell disease [6]. Furthermore, sickle cell patients are particularly susceptible to develop infection compared with general population. Functional asplenism is the main factor contributing to the increase in the rate of the infection in SCD patient [7]. Other mechanism includes reduction in functional activity of complement system [7]. In addition, some causes are linked to genetic and mechanical factors which are related to chronic hemolysis and ischemia [7].
Salmonella is gram negative bacilli of Enterobacteriaceae family [8]. There are two main species of Salmonella; Salmonella enteric and Salmonella bongori [9]. Salmonella is a rare cause of osteomyelitis with only 0.8% of all Salmonella infections seen in the musculoskeletal system [10]. Although Salmonella typhi is the main cause of Salmonella osteomyelitis, cases of paratyphi and nontyphi forms had also been reported [9,11-13].
Salmonella osteomyelitis is a rare condition accounts for 0.5% of all musculoskeletal infection [3]. Salmonella osteomyelitis commonly invades the diaphysis of the long bone. The bone is vulnerable to infection in SCD patients as a result of microcirculation impairment and ischemia [7].
The incidence of osteomyelitis in SCD patients is 2% to 5% [14]. Although Staphylococcus aureus is the commonest organism causing pyogenic osteomyelitis in SCD, Salmonella species are more prevalent in SCD patient compared to non-sickle cell patients [15,16]. Furthermore, hematogenous spread of other organism like Klebsiella has also been reported in the literature [17]. The incidence of Salmonella infection in the spine is 0.45%. It is commonly diagnosed in the lumbar spine followed by the cervical spine [18,19] and typically occurs as a result of hematogenous spread [20].
Back pain and fever in sickle cell patient should raise the suspicion of vertebral osteomyelitis [5]. Chills, nausea and lower limbs pain are other less common clinical features. Vertebral infarction in SCD patients and osteomyelitis can present similarly with back pain, fever and raised inflammatory markers [5,21]. The current case presented typically with low back pain and fever proceeded by bactremia.
The diagnosis Salmonella spondylodiscitis is typically confirmed by images and isolating the organism from the blood or the site of infection [9]. Hence open or image-guided biopsy and cultures from affected intervertebral disc may be of great value in establishing the diagnosis of vertebral osteomyelitis, identifying the microorganism, and therefore guiding anti-microbial treatment. In our case the blood culture failed to grow the organism, which is possibly due to the course of antibiotic he received before coming to our institute.
Salmonella epidural abscess may result in neurological complication and very rarely compression myelopathy [22,23]. A few cases of Salmonella psoas abscess along with vertebral osteomyelitis have also been reported in the literature [24].
Salmonella spondylodiscitis in usually seen in immunocompromised patients like SCD, leukemia, diabetes and patient on long term steroid. However, spondylodiscitis caused by Salmonella has also been reported in immunocompetent patients without any predisposing factors [9,25,26]. Therefore, Salmonella osteomyelitis should be suspected in immune competent patient with recent gastrointestinal infection [9].
Sickle cell anemia patients are more prone for Salmonella infection compared with general population [19]. The main reason is not fully understood but possible pathogenesis is thought to be due to bloodstream spread of Salmonella, which seeds through devitalized and ischemic gastrointestinal wall, which is compromised via chronic vascular sickling. The impairment of reticuloendothelial system and macrophages due to chronic hemolysis and failure of liver to clear blood-borne bacteria are other possible factors.
Antibiotic treatment should be guided by antibiotic sensitivity test of isolated Salmonella. Although in the current patient the blood culture grew Salmonella and received antibiotic but the organism was still surviving at the spine. This probably due to insufficient antimicrobial treatment received. Recently, there has been emergence of antibiotics resistance in different parts of the world. The most commonly used antibiotic therapies are ceftriaxone, ciprofloxacin and chloramphenicol [27]. The current patient responded very well to a course of IV ceftriaxone followed by oral ciprofloxacin. The response was monitored via clinical and laboratory assessment.
The indications for surgical treatment for Salmonella spondylodiscitis are similar to the indication for other causes of pyogenic vertebral osteomyelitis which includes neurological involvement, instability, presence of collection and refractory cases [26]. The main goals of surgical treatment are to decompress the neurological structures, debridement and to provide instrumental spinal instability.
SCD patients have significantly increased risk of peri-operative complication when undergoing instrumented spinal surgery. One of the important intra-operative complications is VOC and measures should be taken to avoid it, including avoiding hypoxia and adequate hydration [1]. The high rate of complication is related mainly to osteoporosis which can result in vertebral compression fracture and pedicle screws related consequences, like pedicle fractures, screw loosening, and pull out [1]. Surgical site infection is another common complication [28].
Generally, complications of spinal osteomyelitis in SCD are rare and they include sepsis, spinal deformity, vertebral pathological fracture, and neurological complications [23,29].
The main limitations of this case report include a relatively short follow-up period. Further clinical and radiological assessments of the patient to look for long term complications like spinal deformity or recurrence of the infection are essential.
Salmonella spondylodiscitis in SCD is rarer than osteomyelitis in other bones. Isolating the organism from the blood or the infection site; either as image guided or open biopsy is critical for making the diagnosis. The infection can be successfully treated with antibiotic therapy guided by sensitivity studies.
The patient’s brother was informed that data and images concerning the case would be submitted for publication, and he provided consent.
Nil.
There are no conflicts of interest.
SAH: Literature review, manuscript preparation, corresponding author. REK: Idea of study, manuscript review. KHG: Literature review. ABS: Literature review, obtaining study consent. TAM: Manuscript preparation, participate in preparing the manuscript.
All authors have contributed equally.