The authors report the case of a 14-year-old girl with Melkersson-Rosenthal syndrome in its classical form, with the triad of recurrent peripheral facial paralysis, upper lip edema and fissured tongue. A rare disease of unknown etiology, it has a chronic and progressive course, and clinical diagnosis is usually by exclusion. An individualized, multidisciplinary approach is fundamental for the treatment of the symptoms and avoids complications and permanent sequelae. The therapeutic options are varied, though most commonly include corticosteroid therapy and nerve decompression surgery.
Melkersson-Rosenthal syndrome, Peripheral facial paralysis, Labial edema, Fissured tongue
The most frequent etiology of facial paralysis is its idiopathic form (Bell's palsy), which occurs in 80% of cases and generally presents complete resolution in most cases and without the occurrence of relapses. In patients that suffer from Melkersson-Rosenthal syndrome (MRS), paralysis in the face is recurrent, accompanied by lip edema and a plicate or fissured tongue (Figure 1). This classical triad is observed in 8 to 25% of patients, though it is more frequent in women in their 2nd and 3rd decade of life. The most common initial finding is orofacial edema [1-3].
MRS is a rare disease of unknown etiology, chronic and progressive course, with neuro-mucocutaneous involvement that affects orofacial innervation. Edema on the face, the predominant manifestation of the syndrome, occurs in 80 to 100% of cases, with the most common location being the upper lip, although other areas of the face, such as the chin, cheeks, periorbital region, oral mucosa, tongue and gums, may be affected. This edema, which mimics acquired or hereditary angioedema, is caused by extravasation of plasma that is mediated by bradykinin or histamine, into the subcutaneous or submucosal tissue [3,4]. In its initial phase, the edema may regress quickly in hours or days, but, after numerous relapses, its regression may be difficult, and can generate localized fibrosis that will culminate in a deforming aspect [5]. This syndrome is not often observed in its complete form (labial edema, plicate tongue and peripheral facial paralysis), since monosymptomatic or oligosymptomatic variants are more usually found. Early manifestations are possible at any age [6].
The predominant theory is that it is of multifactorial genesis, and MRS does not have specific biomarkers. Its clinical diagnosis is usually via exclusion. The observation of familial inheritance and the suggestion of a relationship with autosomal translocation t(9;21)(p11;p11) supports the hypothesis of genetic predisposition [4,7]. Histopathological examination, however, can help to exclude other conditions and allows us to further characterize the underlying inflammatory process, which can help to better understand the mechanisms of the disease [7].
The therapeutic proposals are quite varied and include oral prednisone at a dose of 1 mg/kg/day, on its own or in combination with antibiotics such as tetracyclines, clofazimine, dapsone or minocycline, among others. Other therapies described are facial nerve decompression surgery and facial rehabilitation [2,4,6]. In addition to Bell's palsy, the differential diagnosis of MRS includes chronic inflammatory diseases, infectious diseases characterized by granulomatous infiltrate, rosacea, contact dermatitis and allergic reactions [4].
A 14-year-old female patient sought outpatient care with complaints of edema in the upper lip, pain in the face and peripheral facial paralysis on the right side for 5 days (Figure 1). She cited a similar episode of peripheral facial paralysis on the right side at 11 years of age, for which she did not receive treatment, and the symptoms disappeared spontaneously. The patient denied associated symptoms on the most recent occasion.
 Figure 1: Patient with labial edema and plicate tongue on the first appointment.
View Figure 1
Figure 1: Patient with labial edema and plicate tongue on the first appointment.
View Figure 1
On physical examination, she presented grade IV (House-Brackmann) peripheral facial palsy (PFP), on the right side andmarked edema of the upper lip and plicate tongue. No lacrimal, conjunctival or palate alterations were observed. Electroneuromyography (Figure 2) showed moderate intensity, chronic myelin impairment of the right facial nerve and no signs of recent ongoing denervation. Serologies, including for Lymedisease, were negative.
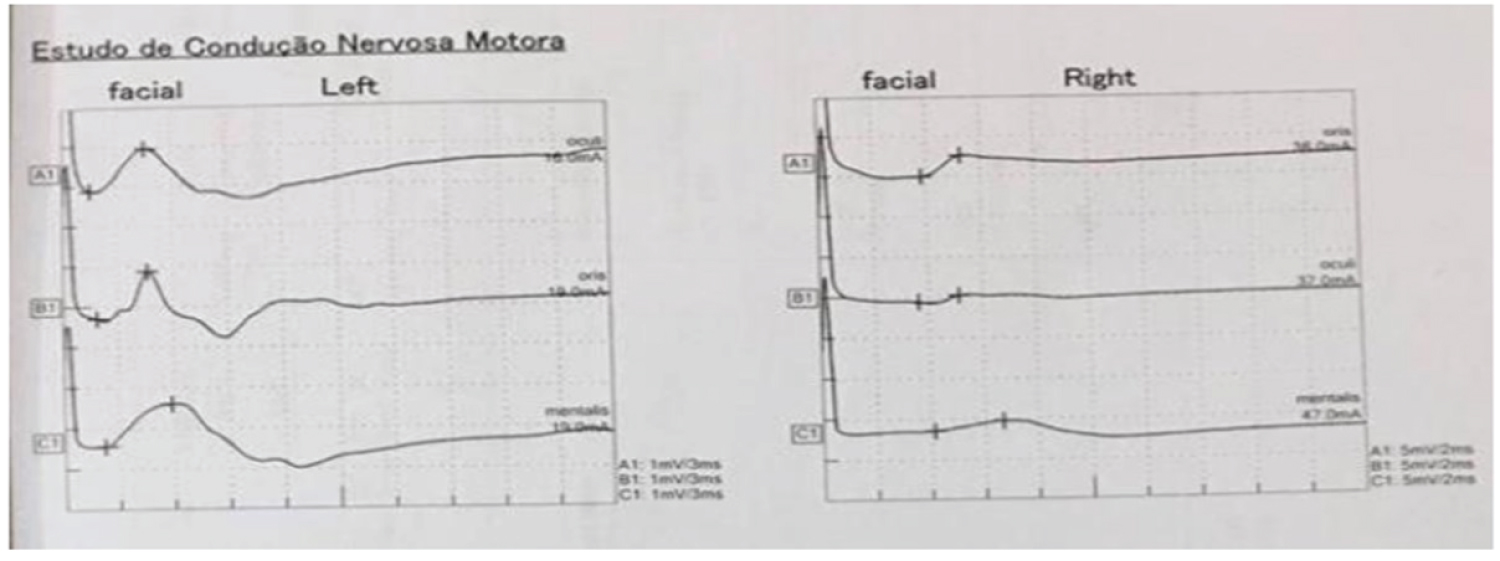 Figure 2: Electroneuromyography exam results.
View Figure 2
Figure 2: Electroneuromyography exam results.
View Figure 2
Faced with this triad of clinical manifestations, and in the absence of evidence suggesting other pathologies, the diagnosis of Melkersson-Rosenthal syndrome was established. The treatment instituted was corticotherapy and neuromuscular physiotherapy, which provided gradual improvement. One month after of the onset of the condition, the patient presented bilateral tinnitus and frontal headaches. After 5 months, the patient presented significant improvement inthe facial paralysis (House-Brackmann grade II) and reduction of the lip swelling (Figure 3).
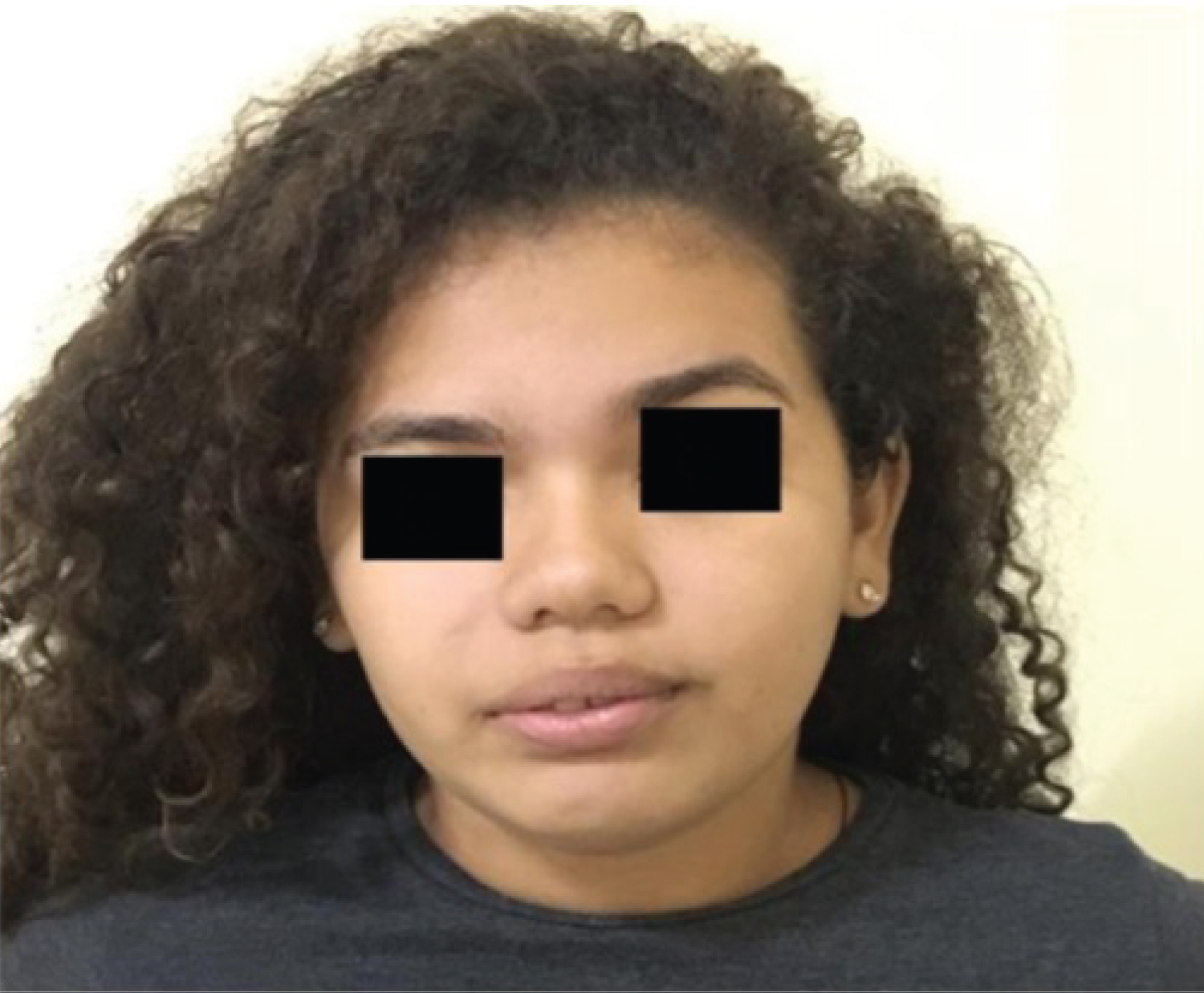 Figure 3: Patient after 5 months of treatment with corticotherapy and neuromuscular physiotherapy.
View Figure 3
Figure 3: Patient after 5 months of treatment with corticotherapy and neuromuscular physiotherapy.
View Figure 3
Melkersson-Rosenthal syndrome is an unusual granulomatous inflammation of the facial region, which is probably caused by a neurovascular dysfunction that leads to hyperpermeability of the vessels and consequent facial edema. According to the literature, its highest prevalence is among young female adults. The above-mentioned patient presented the classic triad of MRS and is in the age group in which the disease is common [8,9].
In the monosymptomatic form of the syndrome, a fissured tongue is present in about 17% of patients over 70 years of age, while only 0.37% of people under 10 years of age manifest this symptom. Thus, age appears to be linked to this manifestation. There is also a dominant inheritance trait that explains the etiopathogenesis of this characteristic [3,5].
Other symptoms may be associated, which characterize the involvement of other cranial nerves, such as headache, tinnitus, difficulty speaking or eating, loss of taste, salivary hypersecretion or sialorrhea, lacrimal secretion disorder and conjunctival irritation. Among these, headache and bilateral tinnitus were reported by the patient in this case. According to González (2001), more than 80% of cases are accompanied by other functional symptoms.
In view of the atypical nature of the patient's symptoms, it was decided to broaden the etiological search for processes that could present self-limited and recurrent facial paralysis. Serologies for myopathies, Lyme's disease and hepatitis were all negative for our patient. Other possible causes includedan infectious origin (herpes virus), lip malformations, angioedema, Ascher's syndrome, among others. However, most were easily diagnosable [2].
In the past, it was believed that MRS was the initial stage of orofacial presentation of Crohn's disease in some patients and therefore should be evaluated and followed up for the presence of gastroenterological symptoms. However, in several studies and literature reviews, this association has not been established. Martinez, et al. (2011) performed a mean follow-up of 8.8 years (SD ± 6.68, range: 1-17 years) and none of the patients were diagnosed with Crohn's disease or any other granulomatous disease.
Currently, there is no gold standard therapy, and the treatment remains largely symptomatic. Numerous approaches have already been proposed, but since this is an infrequent process, there are no placebo-controlled studies to evaluate the effectiveness of different treatments. Combination therapy with intralesional triancinolone, along with clofazimine or dapsone, is one of the most widely used therapeutic options [3].
Other treatments described include prednisone, hydroxychloroquine, sulfasalazine, antihistamines, tetracyclines, metronidazole, macrolides, thalidomide and infliximab. However, the clinical course and therapeutic response of patients can be unpredictable, and, on many occasions, there may be spontaneous remissions or recurrences [10].
The classical triad is evident in this case, making the diagnosis purely clinical. Biopsy of the skin of the edema, especially of the lip, would be necessary in oligo or monosymptomatic cases and would show non-necrotizing granuloma in the dermis.
Melkersson-Rosenthal syndrome is a relevant disease, poorly recognized and sometimes undiagnosed that can cause social and functional damage to affected individuals. An individualized and multidisciplinary approach is fundamental in the treatment of the disease in order to avoid complications and permanent sequelae.
The authors report that there are no conflicts of interest. The authors declare that this work is original and has not been submitted to any other journal.
Approved by the Research and Ethics Committee of the Adriano Jorge Hospital Foundation, Manaus, AM under approval number: CAAE: 27615519.7.0000.0007
None.