A collaborative approach is important in the management of patients, in order to facilitate discussion, and allow cross-checking, in order to achieve the optimal outcome for patient care. Here we present a case, where a collaborative approach allowed the pre-operative identification of an unusual site of metastasis for recurrent papillary thyroid cancer, leading to the change of treatment plan.
We present a 57-year-old male with recurrent papillary thyroid carcinoma. He was previously treated with total thyroidectomy, left-sided neck dissection levels 2-4, 6 in 2018 for papillary thyroid carcinoma. A 6.5 cm thyroid mass was removed. Histology showed extrathyroidal extension and lymphovascular invasion. 18 out of 38 lymph nodes were positive. Postoperatively adjuvant radioactive iodine was offered, however, this was declined by the patient.
4 years post-surgery, the patient developed a new right-sided neck lump. A core biopsy was obtained, and this showed recurrent papillary thyroid carcinoma. CT showed involvement of bilateral cervical lymph nodes, as well as upper mediastinal lymph nodes. There were non-specific lung nodules in both lungs suggesting possible metastasis. TSH was normal.
The patient's case was discussed at the multidisciplinary meeting. The patient's ECOG status is 0. The recommended treatment was bilateral neck dissection, level 6 clearance and thyroid clearance, followed by post-op radioactive iodine.
Pre-operative discussion with the radiologist showed a right parapharyngeal lump, which was not present in the scan four years prior.
The patient underwent the above operation. Bilateral level 6 lymph nodes were cleared, and dissection was followed along the brachiocephalic trunk towards the aortic arch. Level 7 dissection was performed removing 2 lymph nodes in the mediastinum. The pharapharyngeal lump was explored superiorly following the internal carotid artery and vagus nerve. The lump was found in the parapharyngeal space and removed. Right side levels 2 to 5 neck dissection was performed, followed by revision left neck dissection. No significant tissues in levels 2a and 3. Levels 2b, 4, 5a and b dissection were performed.
The patient was admitted to the hospital for observation and discharged post-op day. Post-op recovery was unremarkable.
Histology showed malignancy in Delphian node, parapharyngeal node, and mediastinal node. Right neck dissection showed 5 out of 51 lymph nodes positive. Left neck dissection was clear of malignancy.
The patient was referred to radiation oncology as planned; however, the patient did not attend 3 consecutive appointments despite social worker's input. He was lost to follow up.
For clarification of anatomical terms, the terms prestyloid space is used interchangeably with parapharyngeal space, and post-styloid space with carotid space, or retropharyngeal space. Sometimes parapharyngeal space is used to cover both parapharyngeal and retropharyngeal spaces. In much of the literature, the definition of the term parapharyngeal space is not clearly defined. Here the term parapharyngeal space is used loosely to cover both spaces [1].
20-50% of well-differentiated thyroid cancers have regional lymph node metastasis, normally along the internal jugular and recurrent laryngeal lymph nodes [2]. Lymphatic metastasis of thyroid cancer normally occurs initially to central neck levels 6 and 7, then to lateral neck levels 3, 4 and 5 [3]. Common distal metastatic sites include bones and lungs [4].
Parapharyngeal and retropharyngeal metastasis are very rare, with a reported incidence of 0.43% to 12.5% [2]. 64% of parapharyngeal lymph nodes metastasis are found in the context of recurrence after previous surgery [2]. It is proposed that this could be due to retrograde lymphatic drainage secondary to scarring from previous surgery [3]. Less commonly parapharyngeal metastasis can be found as part of the disease at initial diagnosis, or as the only nodal involvement at initial diagnosis [2].
Tumours of the upper poles of the thyroid gland may skip level 6 and directly metastasise to the lateral neck [3]. It is proposed that the posterior part of the thyroid gland is directly linked to the parapharyngeal nodes through lateral retropharyngeal nodes, via a defect in fascia behind the superior constrictor muscles. It is proposed that metastasis to the parapharyngeal space occurs through the upper thyroid gland, ascending to retropharyngeal space via the posterosuperior collecting vessel, and then subsequently to parapharyngeal space, due to this defect [2,5]. The rare, reported cases all reported the primary tumour with only parapharyngeal metastasis on initial diagnosis were found in the superior pole of the thyroid gland [6]. Other mechanisms include reported cases of ectopic thyroid in the parapharyngeal space, or by direct extension of a tumour along the neurovascular bundle [4].
The patient presented in this report was asymptomatic from parapharyngeal mass, which is frequently the case. Only when reaching a size of 2.5-3 cm, the mass can start to produce symptoms. Wang, et al. performed a retrospective study on 25 patients with parapharyngeal metastasis of differentiated thyroid cancer [6]. 42% of patients had preop symptoms related to parapharyngeal mass, including globus sensation, dysphagia, neck pain, headache, cough, painless mass under the angle of the mandible, Horner syndrome, Vernet syndrome, and involvement of mandibular division of trigeminal nerve [3]. There are also cases reporting symptoms of unilateral aural fullness and facial numbness [1].
Up to 35% of patients with papillary thyroid cancer will have metastatic nodal disease on imaging, with normal examination findings. Histological nodal metastasis is present in up to 80% of these patients. Radiological evaluation is an extremely important part of preop planning as surgery is the main stay of treatment for thyroid cancer [7].
Other rare locations of nodal metastasis include, retrocarotid, sublingual, axillary, intraparotid, supraclavicular, and area superficial to strap muscles [7].
The risk of recurrence is about twice in lateral neck nodal disease compared to the central neck compartments. The risk of recurrence in rare sites of nodal disease is not well studied [7].
There are various approaches to parapharyngeal mass removal - transcervical, transoral or transcervical, transparotid, mandibulotomy and mandibular swing, transmastoid, infratemporal fossa [1]. Transoral resection is only appropriate in nodal metastasis < 2.5 cm to 3 cm [1,8]. The approach depends on the size and location of the tumour. Mandibulotomy and mandibular swing provides better access to the inferior half of the parapharyngeal space. The Transparotid approach provides access to the lateral aspect of the parapharyngeal and retropharyngeal space [1].
Newer approaches include transcervical approach assisted with endoscopic visualization, allowing better visualization of anatomical structures and minimization of complications [1,2]. However there is no study comparing outcomes between open surgical approaches VS video assisted or endoscopic approaches. These are mostly in the form of case reports in the literature.
Lastly it is important to remember that in this case, thyroid papillary carcinoma is the most likely diagnosis given the patient's recurrent disease, however, there is a wide range of possible parapharyngeal tumours including salivary gland tumour metastasis (most commonly), chordoma, lipoma, lymphoma, chemodectoma, rhabdomyoma, chondrosarcoma, desmoid tumour, dermoid, ameloblastoma, amyloid tumour, ectomesenchyoma, fibrosarcoma and plasmocytoma [8]. Sharma, et al. also reported a case in a young female initially diagnosed as paraganglioma [5].
While nodal metastasis in papillary thyroid carcinoma does not significantly impact overall survival especially in patients aged less than 55 years of age, it does increase the risk the recurrence. The risk of recurrence is related to the size (especially > 3 cm) and number of lymph nodes (especially if > 5 nodes) involved. Extranodal extension is a poor indicator of survival due to the increased risk of distal metastasis.
This case report highlights the importance of thorough pre-op imaging and discussion between surgeon and radiologist. The parapharyngeal metastasis could have been missed if not specifically looked for in the pre-operative scans. It was particularly important in this patient to excise the rare location of metastasis, due to the lack of adjuvant radioactive iodine treatment.
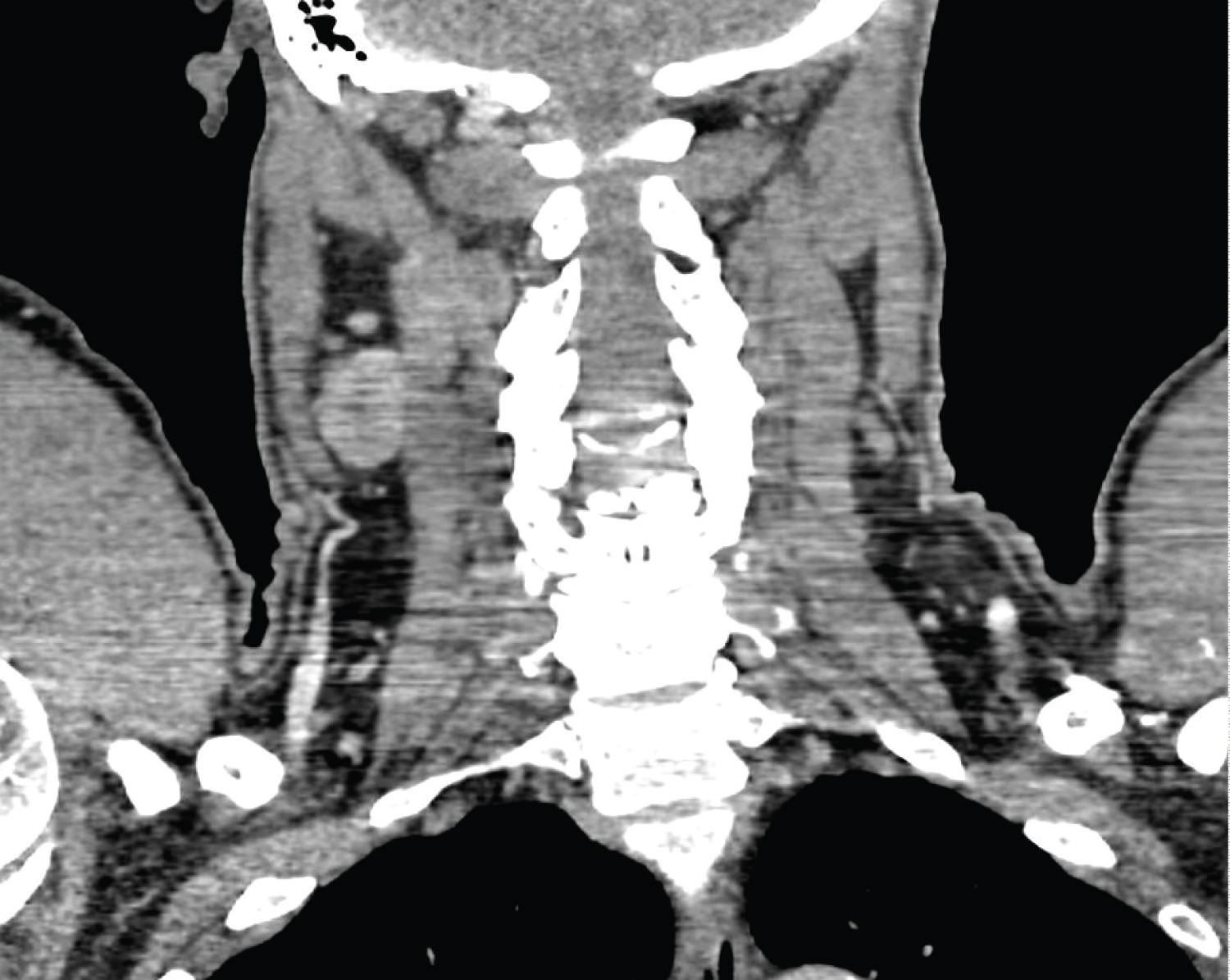 Figure 1: Parapharyngeal lump found on pre-op CT.
View Figure 1
Figure 1: Parapharyngeal lump found on pre-op CT.
View Figure 1