Patients with endometriomas typically present with an intraovarian mass, often associated with multiple foci of extraovarian lesions. An isolated extraovarian endometrioma is rare and represents a challenging diagnostic dilemma.
29 yr G6P3033 woman without history of gynecological malignancies presented with worsening left lower abdominal and pelvic pain over one month. Transvaginal ultrasound revealed a complex cystic mass above the bladder concerning for atypical hemorrhagic cyst versus neoplasm. Laparoscopy revealed an isolated endometrioma on the bladder peritoneum that was confirmed on histology.
Isolated pelvic endometriomas can occur in the setting of pelvic pain without peritoneal or ovarian involvement and/or adhesive disease. Clinicians should maintain suspicion for endometriosis in patients with a pelvic mass and pain regardless of the ultrasound appearance of the ovaries.
Endometriosis is one of the most common causes of pelvic pain in women of reproductive age [1] and can be a diagnostic challenge because of its diverse and nonspecific symptoms and findings. The most common sites of endometriosis are the dependent pelvic structures and include the ovaries, anterior and posterior cul-de-sac, posterior broad ligaments, uterosacral ligaments, fallopian tubes and colon. The diagnosis of endometriosis is commonly suspected based on symptoms such as pelvic pain, dysmenorrhea and/or dyspareunia. Physical exam may include reduced pelvic organ mobility, uterosacral mass or tenderness, or a pelvic mass. Presumed endometriomas may be identified by imaging [2], but ultimately the diagnosis of endometriosis or endometriomas is definitively made at the time of surgery [3]. The gross appearance can range widely with the most common being darkly pigmented lesions often described as "powder burns". However, endometriosis may also present as vesicular lesions with or without neovascularity, adhesions, or endometriomas. The majority of patients are found to have ASRM stage I or II (minimal or mild) disease [4]. Endometriomas are more often associated with pelvic adhesions in patients with stage III or IV (moderate to severe) disease [5]. Patients with an isolated ovarian endometrioma (i.e. no other evidence of endometriosis) are uncommon, and an isolated extraovarian endometrioma is even more rare [6]. Histologic confirmation of endometriosis requires evidence of endometrial glands and stroma outside of the cavity of the uterus. Associated findings of fibrotic granulation tissue, pigment-laden histiocytes, adhesions, and other signs of inflammation are common.
The patient was a 29 yr gravida 6 para 3 Ab 3, who presented to her primary care doctor with new onset of sharp left upper quadrant pain that radiated to the left inguinal area and improved at home with non-steroidal anti-inflammatories. She denied nausea, vomiting, anorexia, dysuria, or hematuria. Her last menstrual period was three and a half weeks prior and she denied any vaginal bleeding, discharge, or pruritis. She was afebrile, and her vital signs were within normal limits. She had a BMI of 36. On physical exam she had normoactive bowel sounds and left upper quadrant tenderness without rebound or guarding. She did not have costovertebral angle tenderness nor was there hepatosplenomegaly or Murphy's sign. Her urinalysis was negative. She was sent home with a diagnosis of non-specific abdominal pain to be treated with acetaminophen with codeine and asked to return for follow up in one week.
Her pain initially improved, however, she presented to the Emergency Department four days later with worsening pain in the left lower quadrant and suprapubic areas. A transvaginal ultrasound at that time revealed an 8.6 cm × 5.3 cm by 5.6 cm complex cystic mass with uniform mildly thickened septations and internal echoes in the left adnexa. There was no detectable internal blood flow, nor were there mural nodules (Figure 1 and Figure 2). The radiologist could not confirm that the left adnexal mass was ovarian, but also could not identify the left ovary independent of the mass. The right ovary and uterus were normal in appearance and size. The patient was discharged home with a preliminary diagnosis of a complex adnexal cystic mass concerning for atypical hemorrhagic cyst versus ovarian neoplasm and scheduled to be seen in the gynecology clinic for a definitive plan. She was given torsion precautions and narcotic pain medication. In the clinic one week later the patient reported that her pain had moderately improved; her abdomen was soft, non-tender, non-distended, without rebound or guarding, and with normoactive bowel sounds. Her pelvic exam was notable for tenderness to palpation along the uterus and left adnexa, with a palpable, persistent left adnexal mass.
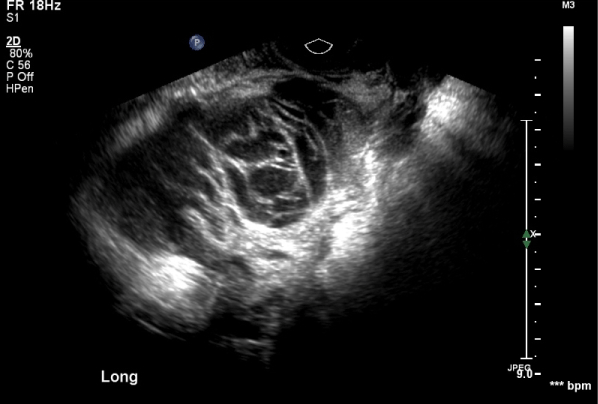 Figure 1: Long transvaginal ultrasound view of 8.6 cm × 5.3 cm by 5.6 cm complex cystic mass with uniform mildly thickened septations and internal echoes. View Figure 1
Figure 1: Long transvaginal ultrasound view of 8.6 cm × 5.3 cm by 5.6 cm complex cystic mass with uniform mildly thickened septations and internal echoes. View Figure 1
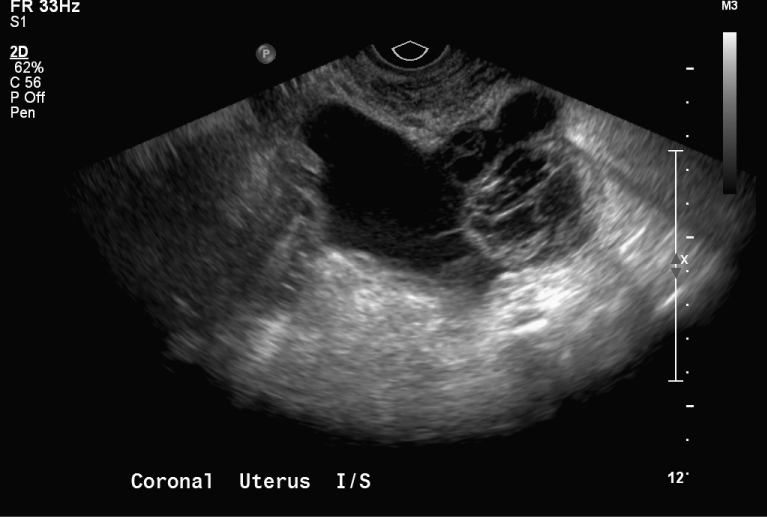 Figure 2: Coronal transvaginal ultrasound view of 8.6 cm × 5.3 cm by 5.6 cm complex cystic mass adjacent to bladder. View Figure 2
Figure 2: Coronal transvaginal ultrasound view of 8.6 cm × 5.3 cm by 5.6 cm complex cystic mass adjacent to bladder. View Figure 2
The patient underwent diagnostic laparoscopy with a preoperative differential diagnosis of atypical hemorrhagic cyst versus neoplasm. At surgery a 5 cm × 5 cm × 3 cm chocolate colored cyst was identified on the surface of the bladder serosa consistent in appearance with an endometrioma. The presumed endometrioma was also adherent to the left round ligament and the fundus of the uterus but was not in any way contiguous with the left ovary which was normal. The uterus, fallopian tubes, and right ovary were also normal in appearance, and there was no evidence of peritoneal or other intraabdominal endometriosis. There was no suggestion of a malignancy. During the process of resecting the mass, the cyst ruptured and dark-sanguinous fluid was visualized. The mass was removed, and fluid was evacuated. Pathological evaluation confirmed endometriotic cyst, with evidence of atrophic glands, hemosiderin laden macrophages (pigmented histiocytes) (Figure 3) and endometrial stroma with inflammatory response (Figure 4). The patient's postoperative course was uncomplicated and she was discharged home on the day of surgery on oral contraceptive pills. The patient recovered well and she was without pain on follow up exam.
 Figure 3: 20X magnification image with evidence of blood, stroma, containing (arrow) hemosiderin laden macrophages (pigmented histiocytes). View Figure 3
Figure 3: 20X magnification image with evidence of blood, stroma, containing (arrow) hemosiderin laden macrophages (pigmented histiocytes). View Figure 3
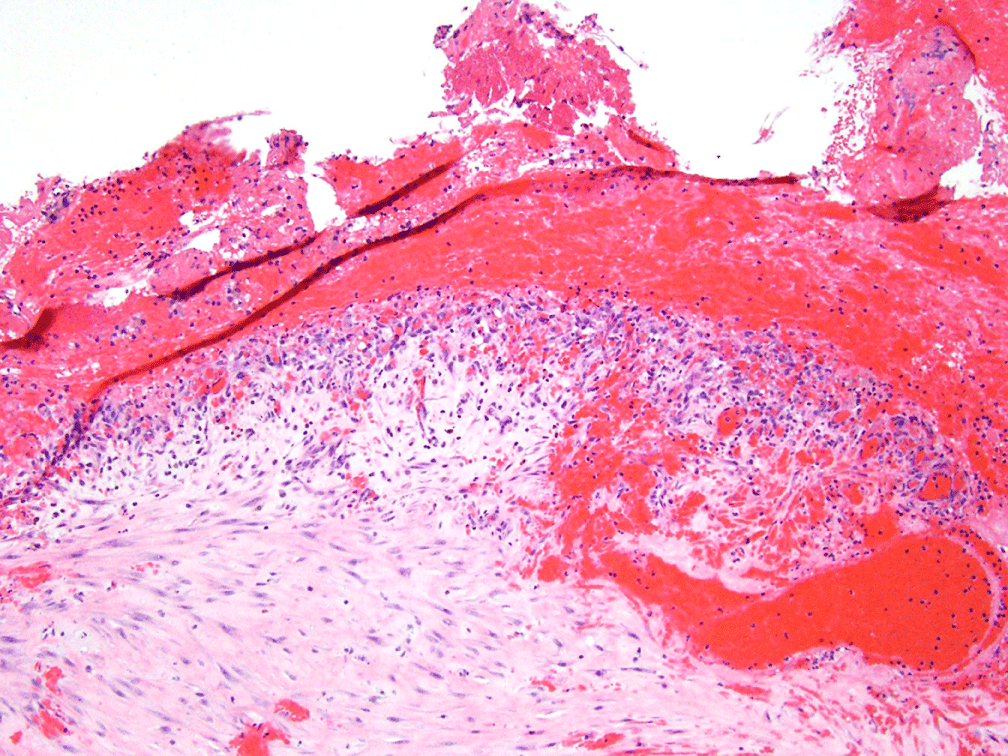 Figure 4: 4X magnification image showing evidence of blood, stroma, and inflammatory response. View Figure 4
Figure 4: 4X magnification image showing evidence of blood, stroma, and inflammatory response. View Figure 4
This case describes an atypical presentation of endometriosis. Despite being extraovarian, a complex pelvic mass in a reproductive age female can be endometriosis. The patient's history, complaints, and imaging were concerning for a hemorrhagic cyst or malignancy; there was a low suspicion for endometriosis in light of the patient's multiparity and atypical symptoms. However, her exploratory laparoscopy revealed a histologically-confirmed endometrioma without peritoneal or ovarian involvement or adhesive disease. Though it is well-known that endometriosis may be subclinical and not visualizable at laparoscopy [7], it is nevertheless surprising that the patient had a single, isolated endometrioma without other findings of endometriosis. Even more unusual was the fact that this woman had no evidence of infertility. It could be hypothesized that the endometrioma as seen in this patient is in some ways different from typical deep endometriomas, which is frequently multifocal [8]. However, the gross and histologic appearance was fairly characteristic. It is possible that retrograde menstrual flow led to seeding adjacent to the bladder surface. This case clearly emphasizes the importance of maintaining a broad differential diagnosis and considering endometriosis in women with pelvic pain and a mass, even in atypical clinical contexts.