To understand the diagnosis and treatment strategies for vaginal dysbiosis (VD), and the efficacy of Palomacare® vaginal gel as an adjuvant treatment and for relapse prevention.
The Palomascopia study was a digital survey conducted from January to March 2021. The data was analyzed once collected.
In Spain, 61% of gynecologists perform a vaginal culture to diagnose VD. To treat bacterial vaginosis 67% of gynecologists, prescribe topical antibiotics and 17% recommend prebiotics, meanwhile 71% of gynecologists recommend topical antifungals as the treatment of choice for candidiasis and 9% recommend prebiotics.
As an adjuvant treatment for fast healing and to obtain a balanced microbiota in VD, 66% of the gynecologists frequently recommend moisturizing and restorative gels, 79% often recommend prebiotics and 74% recommend a specific product for intimate hygiene. To avoidor delay relapses, 68% of the gynecologists recommend moisturizing and restorative gels, 79% recommend prebiotics and 74% recommend a specific product for intimate hygiene (Figure 1).
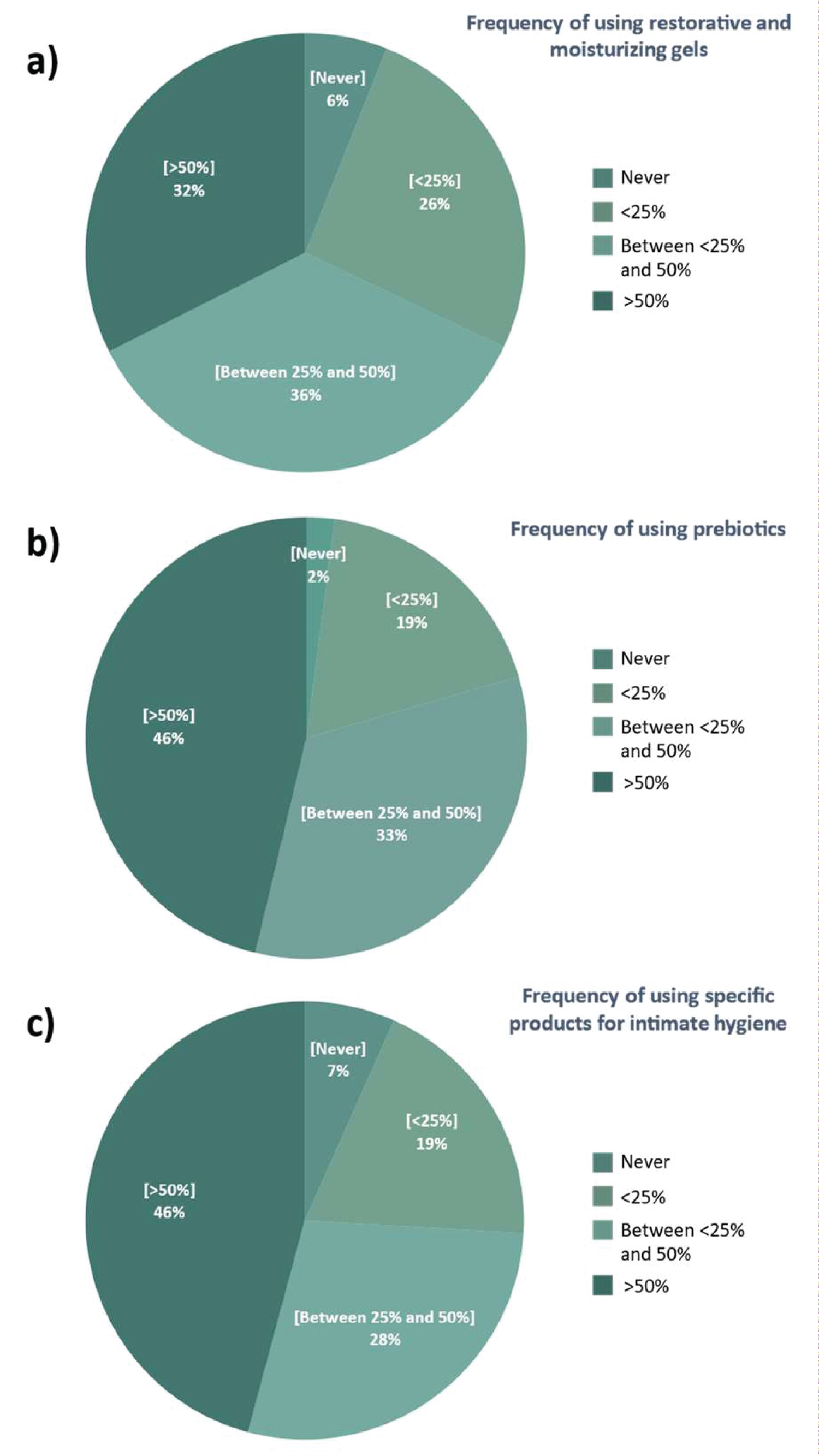 Figure 1: Vaginal infections and relapses (a) Bacterial vaginosis; (b) Vulvovaginal candidiasis.
View Figure 1
Figure 1: Vaginal infections and relapses (a) Bacterial vaginosis; (b) Vulvovaginal candidiasis.
View Figure 1
Palomacare® is recommended as an adjuvant treatment for VD by 79% of gynecologists, 85% observed an improvement in the healing process and 84% observed a reduction in VD recurrences.
Despite the growing resistance of microbes to antibiotics and antifungals, they both remain the first choice for treating vaginal dysbiosis. However, most gynecologists recommend vaginal prebiotics, moisturizing, and repairing products as an adjuvant to pharmacological treatment. Combining naturally sourced ingredients Palomacare® is a non-hormonal vaginal gel containing these three characteristics in one product. As such, most of the gynecologists surveyed perceive it as an effective adjuvant treatment for vaginal dysbiosis, improving healing, and reducing relapses.
Vaginal dysbiosis, Palomacare®, Palomascopia survey
The group of microorganisms living inside or on the surface of human body are known as the microbiota, and their genomic constitution is referred to as the human microbiome. The human microbiota normally consists of symbionts that are benefiting from the host. These may not have an effect (commensalism) on the host's functionality, immunity and health, or they may have a positive effect (mutuality) or a negative effect (pathogenic) [1]. Each woman's vaginal microbiota (VM) is distinctive and unique. It can vary throughout life and fulfills an important role in reproductive health. A wide variety of species - but mostly lactobacilli - cohabit together on the vaginal epithelium, immersed in a dynamic microenvironment and exposed to constant hormonal changes [2]. These species are thought to play key protective roles, including regulating pH in the vagina via lactic acid production, producing various bacteriostatic and bactericidal compounds, or by competitive exclusion [3]. Even though a balance of bacterial species might be predictor of healthy status, a disturbance in the community's composition could imply the origin of multiple diseases.
Vaginal dysbiosis (VD) is a situation whereby the vaginal microbiota experiences a reduction in the predominant population of lactobacillus, with their gradual or total replacement by anaerobes such as Gardnerella vaginalis, Candida spp, Mycoplasma hominis, Mobiluncus spp. and Bacteroides spp. [4]. Vaginal health disorders with a microbial etiology account for over 90% of the causes of vulvovaginitis (VV), of which 4 clinical types are described: bacterial vaginosis, vulvovaginal candidiasis, trichomoniasis and aerobic vaginitis [3]. Women with VV may or may not present one or more of the following non-specific vulvovaginal symptoms: Changes in volume, color or odor of vaginal discharge, itching, burning, irritation, redness, and pain [5].
Antibiotics can be useful for some patients, but many women still report relapses and dissatisfaction after treatment. However, using antibiotics does not seem to be a long-term solution, given the growing emergence of multi-drug resistant microbes [6]. Due to the world health organization (WHO) recommendation for a rational use of antibiotics to reduce their resistance, other strategies have emerged, such as antiseptic treatments, lactic acid and pre and or probiotics. The latter are a useful additional therapy in the management of VD, enabling reestablishing the fragile balance of the vaginal microbiota, without adverse effects [7].
Both comfort and patient sensation are important in determining overall satisfaction with any vaginally administered product. In this regard, Palomacare® is a non-hormonal, moisturizing and repairing vaginal gel, developed using niosomal and phytosomal technology, which enables the active ingredients to penetrate into the lower layers of the vaginal epithelium. It contains prebiotics that favor the growth of beneficial bacteria to the detriment of pathogenic or opportunistic bacteria. It also contains niosomes of hyaluronic acid and beta-glucans, aloe vera, and phytosomes of Centella asiatica, which help to rebalance the vaginal microbiota and moisturize and repair the vaginal mucosa [8,9], providing a complete action as an adjuvant treatment and preventing VD.
The objective of this survey was to clarify the situation of VD treatment in Spain and to understand the perceived efficacy of Palomacare® as an adjuvant treatment do VD and to prevent relapses.
The Palomascopia survey was conducted from January to March 2021 (inclusive). The digital questionnaire contained fifteen questions relating to the diagnosis and treatment of VD and the use of a non-hormonal vaginal gel containing hyaluronic acid, β-Glucan, Centella asiatica and prebiotic (Palomacare®) as an adjuvant treatment and for preventing relapses during clinical practice with patients over 18 years of age. The survey targeted Spanish gynecologists. Data was sent automatically and analyzed using a chatbot digital tool. Data quality was ensured through double-entry Microsoft Excel®.
773 Spanish gynecologists participated in the survey, with the vast majority (99%) considering VV as a major concern for women. VD can be easily diagnosed when the vaginal pH is ≥ 4.5 (one of the Amsel criteria) [10]. Nevertheless, 57% of gynecologists do not measure pH or carry out a fresh sample microscopic examination during consultation (58%), despite being a quick, inexpensive test. 61% of doctors always perform a vaginal culture during diagnosis.
When it comes to treatment, 67% of gynecologists prescribe topical antibiotics as their first treatment choice for bacterial vaginosis caused by Gardnerella vaginallis, while 17% already initially recommend prebiotics. When caused by the opportunistic fungus Candida albicans, 71% of gynecologists recommend topical antifungals as the first treatment choice. Azoles are the preferred treatment. However, failure to clear the infection with this antifungal is a growing issue [11]. Surprisingly, 9% of gynecologists already use prebiotics as a first treatment option for vaginal candidiasis.
The administration of prebiotics or beneficial microbes to the mucosal surface has been also suggested as an adjuvant treatment for preventing vaginal infections along with relapses [12]. In this regard, 66% of the gynecologists frequently recommend moisturizing and restorative gels, 79% often recommend prebiotics and 74% recommend a specific product for intimate hygiene as an adjuvant to an antibiotic, and/or antifungal treatments to aid faster healing and microbiota rebalancing. With the aim of avoiding or delaying relapses, 68% of the gynecologists frequently recommend moisturizing and restorative gels, 79% recommend prebiotics and 74% recommend a specific product for intimate hygiene.
Regarding their experience with Palomacare®, the adjuvant treatment of VD appeared as the first reason for recommendation for 20% of gynecologists, along with 25% who mainly prescribe Palomacare® to treat unspecific vulvovaginitis, 24% to treat genitourinary syndrome, among other indications [13,14].
Most gynecologists (79%) had already recommended the use of Palomacare® as a VD adjuvant treatment. 85% have observed an improvement in the healing process and 84% have observed a reduction in VD relapses among patients treated with Palomacare®. These improvements may be justified due to its mucosal moisturizing, repairing and microbiota balancing properties, corroborating the results obtained by Palacios, et al., [13] regarding repairing the cervicovaginal mucosa among patients with inflammatory cytology [8,9,13,15]. Also, Palomacare's prebiotic, Bioecolia®, has provided evidence of bioselectivity that favors beneficial bacterial strains, promoting competitive inhibition of pathogens, re-establishing the lactobacillus balance, even for more severe cases of dysbiosis (Figure 2).
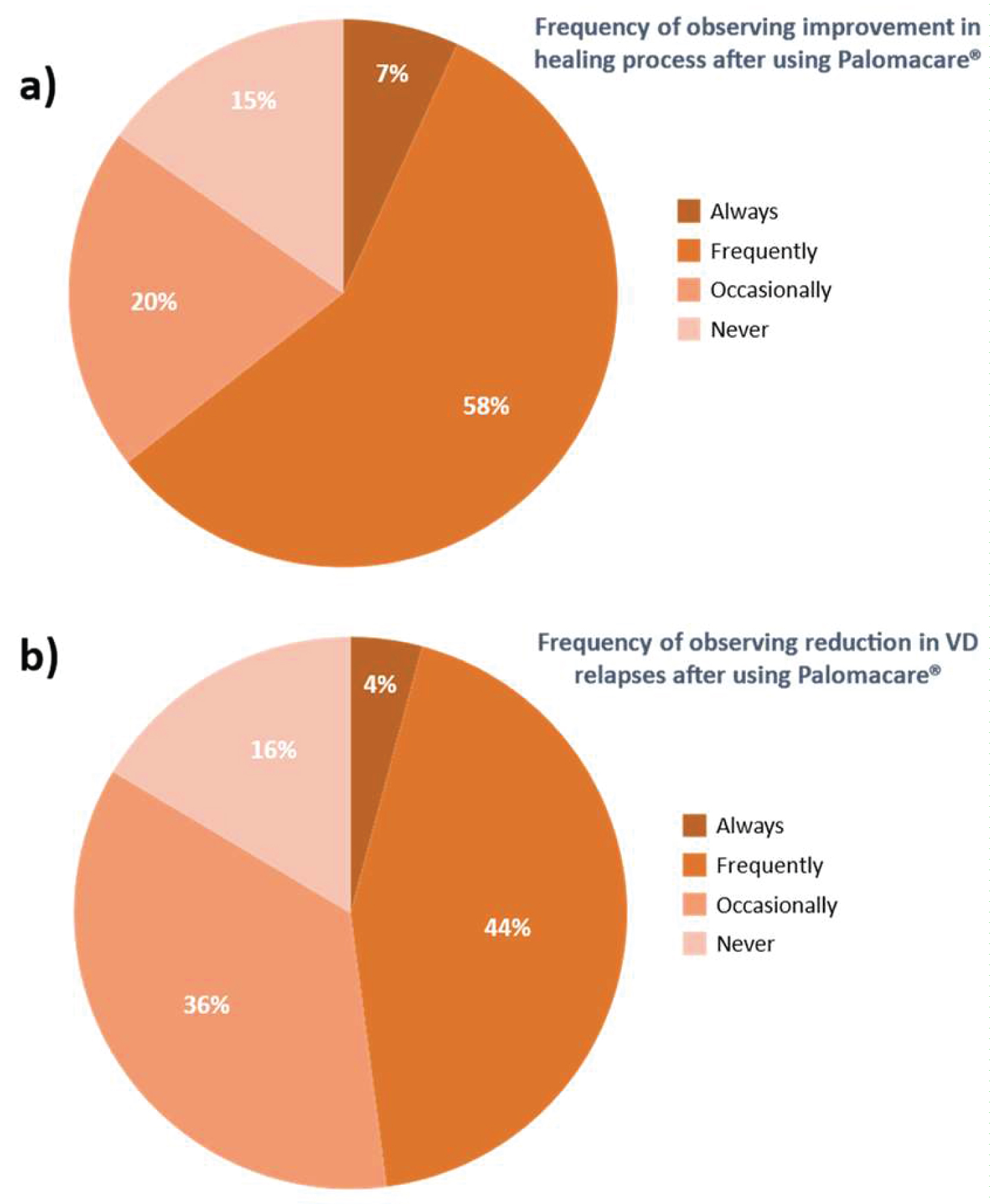 Figure 2: Situations in which Palomacare® is prescribed.
View Figure 2
Figure 2: Situations in which Palomacare® is prescribed.
View Figure 2
The data collected using the Palomascopia survey proved useful for understanding vaginal dysbiosis treatment in Spain. Though pH measurement is an inexpensive and quick test, most gynecologists do not do it. Moreover, antibiotics and local antifungals are the first choice for treating vaginal dysbiosis. However, some doctors are starting to prescribe prebiotics. It is worth noting that most gynecologists recommend moisturizers, repairers, and prebiotics as adjuvants to standard treatment in order to obtain a better healing percentage and fewer relapses. In this sense, Palomacare® contains these three characteristics in one product, with most gynecologists surveyed perceiving it as an effective adjuvant treatment that improves healing and reduces relapses.
The authors have no funding or conflicts of interest to disclose.
All authors have contributed equally to the work.