Foreign body ingestion is a very common reason for access to the Emergency Department and in most cases, it doesn't cause symptoms; in case of fishbones, intestinal perforation is rare but possible. In this report, besides the typical picture of bowel perforation, we found atypical symptoms due to the specific location.
We present a case of a 70-year-old man who presented to the Emergency Department complaining abdominal pain and several syncopes; a CT scan of the abdomen revealed the presence of a foreign body in the pyloric area, which was removed by surgical intervention and resulted to be a fishbone. Both abdominal and neurological symptoms disappeared.
We suppose that the specific location of fishbone, in the area when the pyloric branches of left vagus nerve run, can explain both the abdominal symptoms and the vasovagal syncope, through a sympathetic inhibition mechanism: Emergency physicians and emergency surgeons must be aware when dealing with symptoms apparently discordant that could be attributable to one common factor.
Foreign body ingestion is a very common reason for access to the Emergency Department (ED): Most of foreign bodies don't need any procedure and leave gastrointestinal tract spontaneously; about 20% require endoscopic removal; surgery is needed in about 1% of cases [1].
Reviewing the world literature, we found a multitude of reports about ingestion of peculiar foreign bodies; some of them require a high index of suspicion, due to their specific shape: A recent paper by Jo, et Al. describes two cases of toothpick-ingestion-induced colon injury, mimicking diverticulitis. Both cases required a surgical intervention for removal [2].
Another "unusual" foreign body, although lower in incidence, is a toothbrush: It's ingestion is usually related to psychiatric disorders such as bulimia, schizophrenia or generalized eating disorder and always requires an early endoscopic or surgical removal [3].
Fishbone ingestion is quite frequent in the general population and often occurs in children older than 1-year-old [4]. Although they are ponty objects, gastrointestinal perforation is a very uncommon event and it usually affects the ileum; moreover, patients rarely remember FB ingestion and refer to the ED with non-specific symptoms, such as nausea and abdominal pain [5]. We describe the case of a patient who presented to the ED with vague abdominal pain and several episodes of syncope; a CT scan showed a foreign body in the pyloric zone, just outside the stomach, which revealed to be a fishbone at laparoscopic exploration.
A 70-year-old man presented to the ED complaining of abdominal pain and three or four episodes of syncope: Both of them were lasting for one week and no particular triggers were described at admission. He revealed that syncope was always preceded by sensation of bradycardia and nausea; at further investigation, he reported that never suffered episodes of transient loss of consciousness before.
His past medical history was significant for arterial hypertension, obesity and type II diabetes. Vital signs included: Temperature 38.5 ℃, pulse 130 beats/min. blood pressure 170/100 mmHg, and a pulse oximetry 95% on ambient air. Neurologic and chest examination were normal. Cardiac examination revealed a regular rate and rhythm, without murmurs or gallops; there was no jugular venous distension or hepatosplenomegaly; peripheral edema was absent. Abdominal examination revealed a distended abdomen and a moderate tenderness - without rebound - in the right upper quadrant.
Laboratory tests were significant for a hematocrit of 32.7% and a hemoglobin of 10.7 g/dL. The white blood cell count was 16.880 × 10^3/ul and c-reactive protein was 29.7 mg/dl; troponin level was into normal range and EKG was substantially normal.
Abdominal ultrasound was performed, but no alterations were observed. Considering abdominal presentation and blood test results a CT scan of the abdomen was then performed. It showed a thickening of stomach in the pyloric area, without signs of perforation, and the presence of a linear foreign body measuring 17 mm in length, lying just between the gastric wall and the liver (Figure 1).
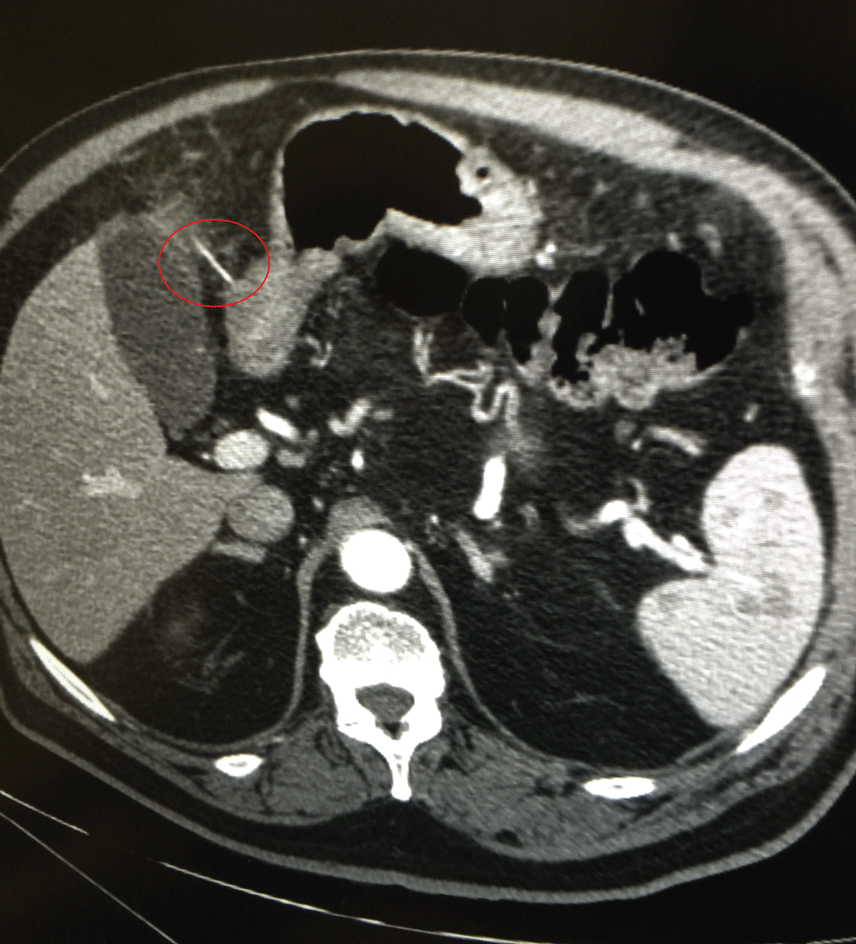 Figure 1: CT scan: A linear foreign body, measuring 17 mm in length, is lying between the gastric wall and the liver; a thickening of stomach in the pyloric area is present, without signs of perforation. View Figure 1
Figure 1: CT scan: A linear foreign body, measuring 17 mm in length, is lying between the gastric wall and the liver; a thickening of stomach in the pyloric area is present, without signs of perforation. View Figure 1
 Figure 2: Intraoperative picture at laparoscopy: A pointed foreign body, compatible with a fishbone, is found between the stomach and the liver; a local inflammatory process is also observable.
View Figure 2
Figure 2: Intraoperative picture at laparoscopy: A pointed foreign body, compatible with a fishbone, is found between the stomach and the liver; a local inflammatory process is also observable.
View Figure 2
A further anamnesis was made, and the patient revealed a fish dinner one week before.
At that point, we decided for exploratory laparoscopy, which confirmed what observed by CT scan (Figure 2); the fishbone was then removed, and all symptoms disappeared, including syncopes. The patient was then discharged four days after surgery. A Holter-EKG was also prescribed, and no alterations were observed during the 24 hours of monitoring; a Doppler ultrasound study of carotid arteries was negative too.
Foreign body ingestion is quite frequent in children; it is not so common in the adult population and carries a higher frequency in males than in females [6]. Most foreign bodies are eliminated spontaneously within 5-10 days after ingestion and most of the patients don't even realize their presence.
In some cases, they can stop and cause obstruction and visceral perforation, mostly when they reach an area where anatomical narrowing is present, such as the cricopharyngeus muscle, aortic arc, left main stem bronchus, gastroesophageal junction, pylorus, duodenal sweep, ileocecal valve and anus [1]. Obviously, a sharp object, like a fishbone, carries a higher risk of perforation, up to 35% [7]: Typical clinical symptom is acute abdominal pain and differential diagnosis includes appendicitis, diverticulitis and peptic ulcer perforation.
Moreover fishbones, such as glass and plastics, are usually invisible under standard X-Ray [6] but can be detected under abdominal CT-scan, like in this present case; non-operative management, i.e. endoscopic removal, has to be considered as the first-choice treatment but surgery becomes necessary if clinical presentation is particularly severe or in case of life-threatening complications like hepatic abscess, sepsis and retroperitoneal hematoma [8].
Besides the typical presentation, additional symptoms can develop due to the specific location of foreign body: In our case, the fishbone was just in the pyloric area. As is well known, the left vagus nerve runs from the lesser curvature in lesser omentum as far as the pyloric antrum, where it divides into pyloric branches; it is likely that vagal afferents were activated by this foreign body, the mechanism of which may be similar to "deglutition syncope", where the stimulation of the vagus results in sympathetic inhibition and peripheral vasodilatation, thus leading to hypotension and syncope [9].
In literature we also found several cases describing recurrent syncope caused by lung cancer that resolved when tumour size decreased during chemotherapy: Authors describe a vasovagal mechanism due to mechanical compression on vagus nerve [10].
In conclusion, ingestion of fishbones must be suspected in patients admitted to the Emergency Department with abdominal pain and reporting ingestion of fish before the onset of symptoms; besides common presentations, a high index of suspicion must be kept when location of fishbone, and generally of all foreign bodies, can cause atypical clinical pictures due to specific irritation of anatomical structures, such in our case.
The authors declare that there are no conflicts of interest.