Brain metastases are considered to be the most common malignant brain tumors in adults, and constitute a major challenge in oncology. The objective of our study is to analyze the epidemiological, clinical and paraclinical parameters of patients with brain metastases and treated by encephalic radiotherapy during the year 2020 at the Mohamed VI center of the Ibn Rochd CHU.
This is a descriptive retrospective study of 57 patients treated for brain metastases by brain radiotherapy in toto over a period of one year from January 2020 to December 2020 at the Mohamed VI center for the treatment of cancers. . Data was collected using a form duly completed from patient files.
The median age was 54 years with extremes ranging from 33 to 79 years, a female predominance was noted with a sex ratio of 1.11. The evaluation of the general condition made it possible to classify the patients of performance index status '1' in 75.4% of cases.
70.2% of cases had multiple brain metastases, 26,3% of cases had a single metastasis and 2 cases had three brain lesions (Figure 1). The primary was of bronchopulmonary origin in 57.9% of cases, of mammary origin in 38.6% of cases, and of renal origin in 2 cases (Figure 2). The discovery of brain metastases was synchronous with that of the primary in 49% of cases and metachronous in the rest of the cases.
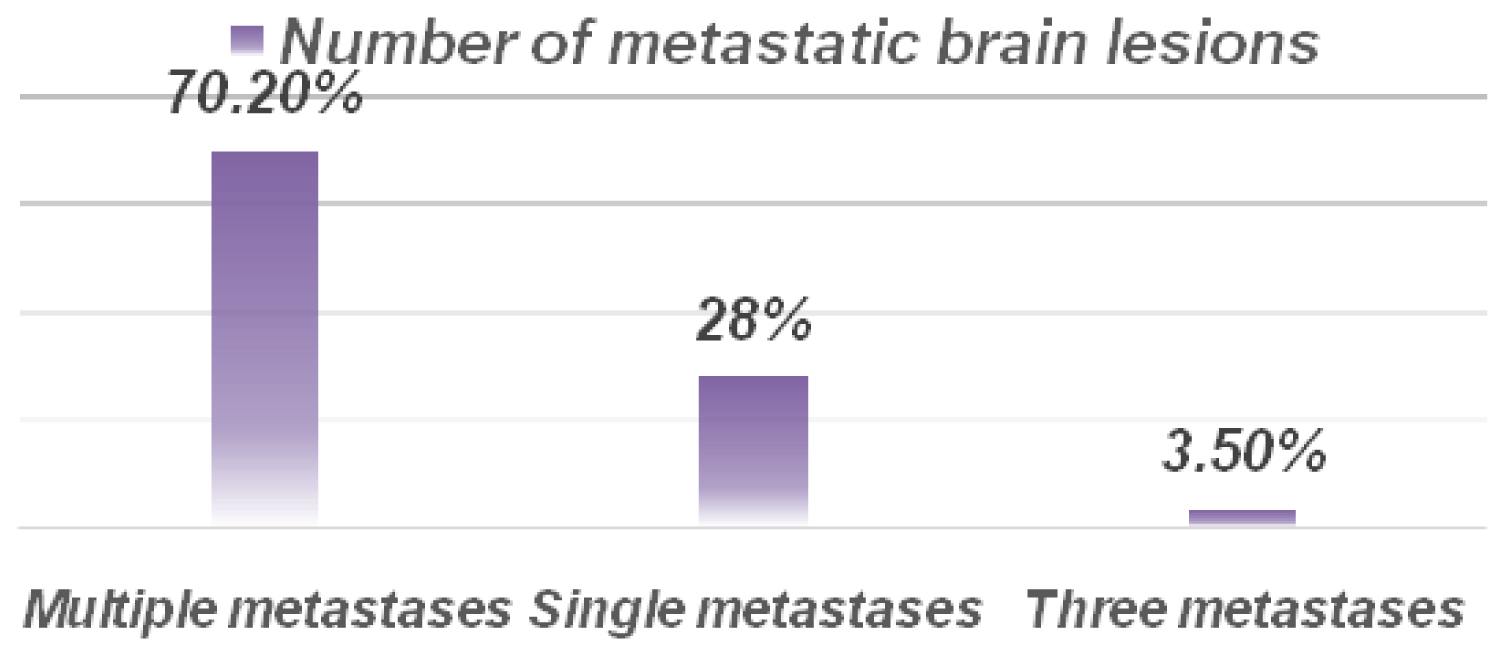 Figure 1: Number of metastatic brain lesions.
View Figure 1
Figure 1: Number of metastatic brain lesions.
View Figure 1
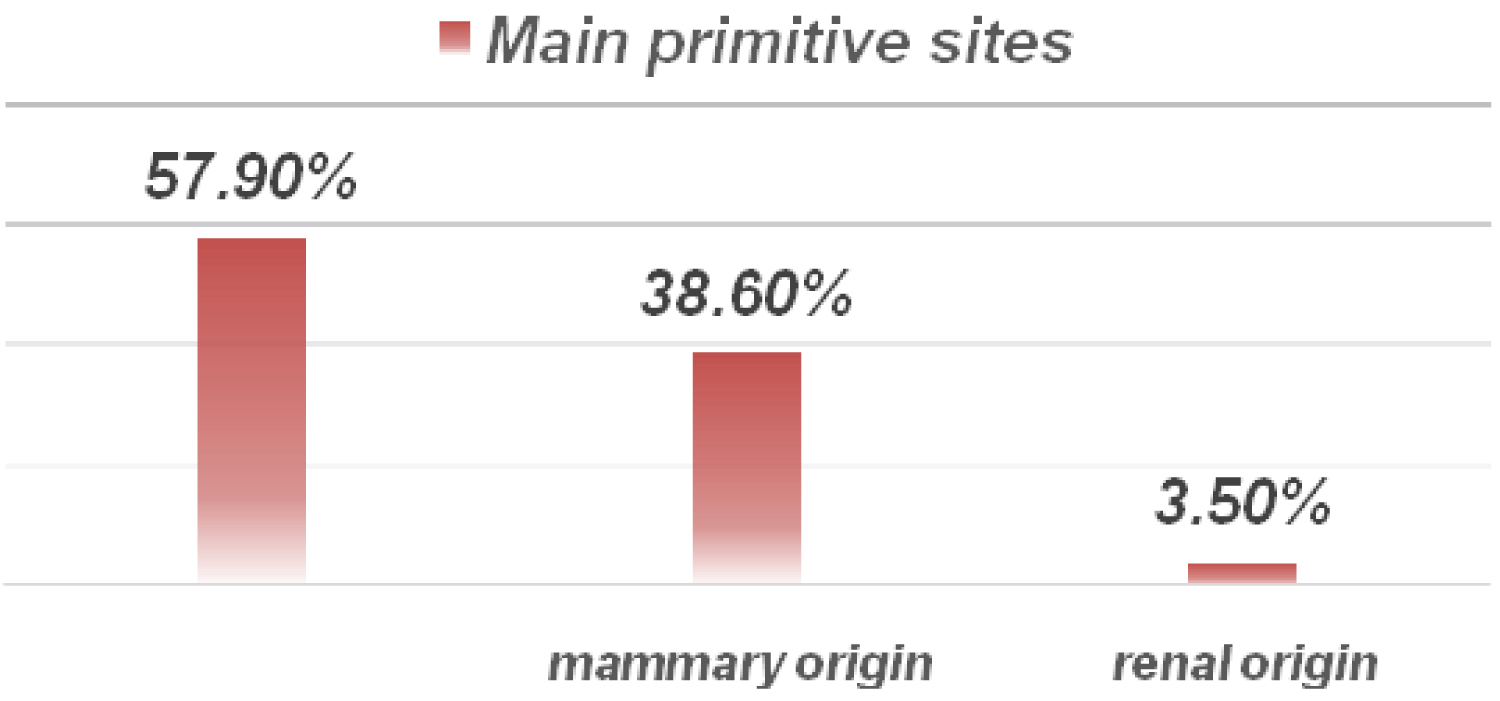 Figure 2: Main primitive sites.
View Figure 2
Figure 2: Main primitive sites.
View Figure 2
Most patients showed signs of brain extension at the time of diagnosis. 35% of the patients suffered from a neurological deficit and 47.4% from an intracranial hypertension syndrome. However, the discovery of secondary cerebral localization was fortuitous in 10 cases. 52.6% of cases had other metastatic sites (Bone, Lung).
All patients underwent 3D conformational radiotherapy of the brain in toto with a dose of 30 Gy in 10 fractions in 15.8% of cases, 20 Gy in 4 to 5 fractions in 79% of cases and 16 Gy in 4 fractions in 3 cases. An additional boost of 3 * 3 Gy was received in 4 patients. However, surgical excision before radiotherapy was only performed in 5 cases (Figure 3).
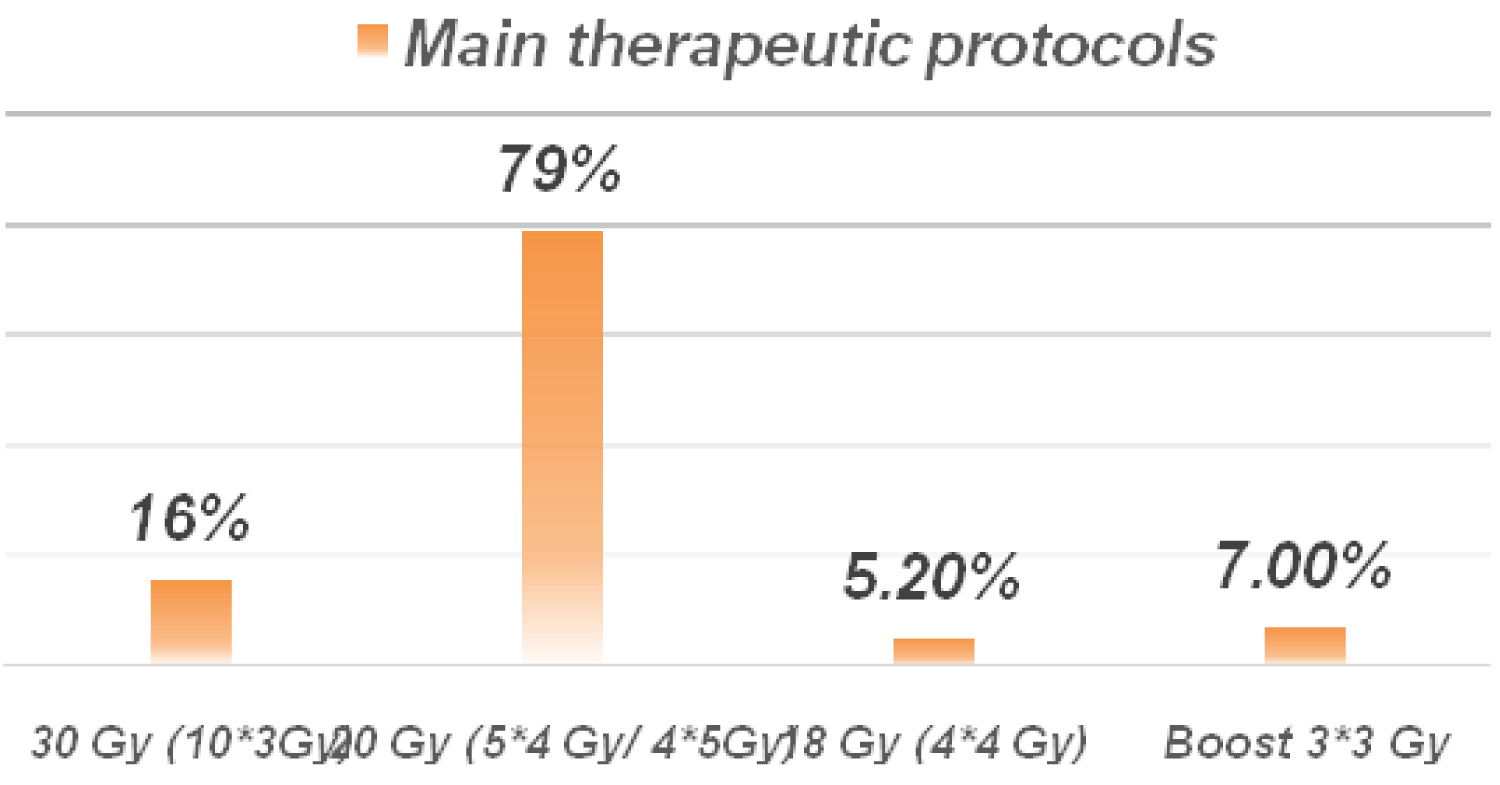 Figure 3: Main therapeutic protocols
View Figure 3
Figure 3: Main therapeutic protocols
View Figure 3
All symptomatic patients were put on corticosteroid therapy initially by the injectable route for three days then relayed by the oral route.
At the evaluation; 54.4% of patients improved their quality of life with a recovery of their autonomy and an improvement in verbal fluency. 19.3% of cases had a complete response without local recurrence. 15.7% of cases worsened their neurological symptoms and 10.5% of patients were lost to follow-up after the end of brain radiation therapy.
The median survival time was 5.2 months that of recurrence-free survival of the five operated patients was 7.8 months.
The characteristics of cerebral metastases and the type of primary cancer are an important determinant for the prognosis; therapeutic management must take into account the predictive criteria for local control; and the early detection of this pejorative localization.