Acute kidney injury (AKI) is a medical emergency. It refers to a heterogeneous disorder characterized by an abrupt and usually reversible decrease in kidney function, resulting in the retention of nitrogenous waste products and in the dysregulation of extracellular volume and electrolytes. Its incidence is on the rise in both developed and developing countries, with the condition resulting in high morbi-mortality and economic burden.
To determine the average total cost in the management of acute kidney injury in each patient; specifically, to determine the direct and indirect costs of this pathology.
We used a prospective cohort study design, over a study period of four months in a tertiary hospital in Cameroon; Douala general hospital. We included all patients with an acute kidney injury hospitalised in the Internal Medicine service. The direct cost was estimated from: The cost of laboratory investigations, treatment of complications, dialysis treatment and other hospital expenses. We used: Pharmacy receipts, hospital bills, receipts of patient and guardian expenditure in the calculation of the direct cost. Indirect cost was estimated from salary allocations of the ongoing year by the public service. Linear regression analysis was used to evaluate the association among the cost, socio-demographic and clinical variables. The costs were expressed in XAF, code for the Central African CFA franc. CFA stands for "African Financial Community".
In total, 42 patients participated during this study. 22 (52.4%) patients were women. The mean age was 55.5 ± 19 years. The average total cost for the management of acute kidney injury in our study was XAF 977,556.0 ± 3,170,467 ($1,729). The median of this cost was XAF 402,473 ($712.1); IQR [XAF 212,813-628,396]. The direct cost was XAF 455,444.8 ± 383,293 387 ($656.39), which represented 47% of total cost. The median of this cost was XAF 283,687 ($501.9); IQR [XAF 182,855-459,115]. The indirect cost was XAF 521,111.2 ± 2,969,310 ($921.9). The median of this cost was XAF 335,815 ($594.1); IQR [XAF 189,680-559,098]. It represented 53% of total cost. The majority of costs were allocated for: the treatment of the aetiology, hospitalisation, dialysis and cost due to early mortality.
Despite the efforts made by public institutions, the cost of managing acute kidney injury remains high for the average Cameroonian and society; especially when the treatment involves dialysis.
Acute kidney injury, Total cost, Direct cost, Indirect cost
AKI: Acute kidney injury; AIDS: Acquired immune deficiency syndrome; XAF: Central African CFA; DGH: Douala general hospital; HBP: High blood pressure; GDP: Gross domestic product; IQR: Interquartile range
Acute kidney injury (AKI) is a clinical entity defined as a sudden decrease in renal function [1], sufficient to lead to retention of urea and other nitrogenous waste products and imbalance in hydroelectrolytic homeostasis [1,2]. It represents the culmination of various processes that can be reversed or alleviated by treatment directed against the underlying condition [1,3]. In clinical practice, the definition of AKI is based on the serum creatinine (sCr) and urine output values [4]. Therefore, The Kidney Disease: Improving Global Outcomes (KDIGO) guidelines in 2012 define AKI according to one of these criteria: increase in sCr by ≥ 0.3 mg/dl within 48 hours, or Increase in sCr to ≥ 1.5 times baseline, which is known or presumed to have occurred within the prior seven days, or urine volume < 0.5 ml/kg/hour for six hours [4].
The epidemiology of the disease is variable, as there is a great disparity in the incidence of the disease in developed and developing countries; contrast attributed to socio-economic disparities [5]. In developed countries, the incidence varies from 21 to 30% of admissions per year; depending on the place of acquisition in community, hospital or intensive care unit [4,6]. There are few studies in developing countries on the incidence of the pathology in the community using the recent definition criteria [7]. Many etiologies cause AKI; they can be classified into three groups according to pathophysiology [2,8]: Prerenal, intrinsic renal and post renal causes. Prerenal etiologies account for the most common causes (65-75%) and are related to a decrease in kidney perfusion [8]. They may occur in a variety of settings: Intravascular volume depletion, hypotension, impaired intra-renal regulation, or selective renal arteries stenosis [2,3]. Intrinsic renal causes are related to involvement of renal parenchyma in cases of acute tubular necrosis, interstitial nephritis, glomerulonephritis, and vasculitis. Post renal AKI is a renal impairment secondary to urinary tract obstruction [9].
In developing countries, disease presentation is peculiar; in urban centers, the profile is similar to that found in developed countries. It is mainly an AKI acquired in hospital, predominated by the elderly with multi-visceral failures. The major cause remains renal ischemia mainly due to sepsis and often associated with nephrotoxic drugs [10]. In rural setting, it is an AKI acquired in the community, affecting mainly young people, without co-morbidities. Within this population, specific causes include: Diarrhea, infectious diseases, septic abortion and traditional pharmacopoeia-based drugs [11,12]. In Cameroon, acute kidney injury accounts for 35.61% of nephrology consultations per year at the Douala general hospital [13]. The significant increase in the incidence of the disease worldwide, coupled with morbidity and significant mortality, make acute kidney injury a serious medical condition that imposes preventive measures, early diagnosis and adequate treatment to reduce this morbi-mortality; and thereby reduce the economic burden of the condition.
With respect to the economic burden, in England, the impact of AKI on the national health system is about £1.02 billion sterling per year, or nearly 1% of the budget [14]. Chertow in 1998 [15] in the United States estimated the additional expenditure in patients with a rise of 5 mg/l of serum creatinine to 7,500 US dollars, which is approximately XAF 4,357,500. In Canada, the care of a single patient with AKI costs is closer to $11,192 Canadian dollars or about XAF 5,085,644.8 according to the exchange rate in force on the date mentioned above. In Cameroon, despite subsidies for hemodialysis by the state, Fouda, et al. found that nearly 28% of patients with AKI and dialysis indications were not dialysed for lack of funds [13]. Also, few studies have been published in developing countries either on the direct or indirect cost related to the management of this pathology which in the vast majority of cases is due to preventable causes. Therefore, this study aimed to describe the different costs inherent in the treatment of this condition in order to determine the global cost, also called economic cost of the management of a patient with AKI. Moreover, the review of costs will make it possible to bring out the deficit on the budget of the family and the losses for the society engendered by this condition.
This was a descriptive observational cohort study. The study took place in the Department of Internal Medicine of the Douala general hospital (DGH) over a period of 4 months, from 05 January 2015 to 04 May 2015. Douala general hospital is a tertiary care facility of the health pyramid in Cameroon. It is located in the economic metropolis of the country; it has a department of internal medicine divided into two sub-units for a total capacity of 56 beds. The formation has one centre-based haemodialysis; there are two nephrologists.
This was a comprehensive sample, so all patients who met the selection criteria during the study period were recruited regardless of gender, age and race. Included in the cohort were patients with acute kidney injury who were hospitalized in the department of Internal Medicine. We excluded: Patients who did not consent, patients who did not achieve serum creatinine normalization after 3 months, and patients with acute kidney injury due to chronic renal disease.
We used the bottom-up approach for the cost calculation. In this approach, all the expenses generated and relating to each patient are collected individually by means of a questionnaire. In this study, a non-comparative cost analysis was used, and this analysis was based on the patient's and society's point of view.
The direct cost consisted of the sum of: The cost of additional examinations (related to the diagnosis of AKI, its causes and complications), cost of treatment of complications of AKI, cost of treatment of etiology of AKI, other hospital costs (this was the cost of consultations, the cost of the room and hotel services) and finally the cost of dialysis treatment. The latter took into account: The number of dialysis sessions, the dialysis equipment and the cost related to the management of all complications related to dialysis. The cost of a hemodialysis session was calculated taking into account the cost of the dialysis unit kit, the cost of water and electricity used for the functioning of the hemodialysis generators, and fixed cost paid at the hospital desk. Thus, the cost of a session was evaluated at XAF 59,235 ($104.8) at the Douala general hospital [16].
The indirect cost was calculated as the sum of: Cost related to temporary incapacity for work, cost of incapacity for work due to death, and additional expenses of families (was taken into account: Family transportation costs, their nutrition, and communication credits). The cost of temporary work incapacity was calculated according to the human capital theory. This consisted in multiplying the duration of incapacity by the daily wage (according to the professional category of the patient as defined by the ministry of the civil service) for the employees. Among the unemployed, it will be a question of multiplying this duration of incapacity by the gross domestic product/inhabitant/day. The GDP/inhabitant/day of 2012 amounting to XAF 1,501 as defined by the World Bank and the International Monetary Fund. The duration of disability was calculated by adding the number of days of hospitalization to the number of days of medical rest and days for external follow-ups. The cost of incapacity for work due to death was calculated by multiplying the lost productivity period by annual earnings or GDP per inhabitant per year.
The global cost, also called the economic cost, was calculated by summing the direct and indirect costs. The "intangible" costs or costs related to psychological harm have not been valued. The costs were expressed in XAF, code for the Central African CFA franc. CFA stands for "Communatué Financière d'Afrique", which translates to the African Financial Community in English.
AKI definition: Diagnosis of the pathology was made according to the KDIGO 2012 criteria.
AKI staging: The pathology was classified in stage 1, 2, 3 of increasing severity according to the criteria of KDIGO 2012.
Community-Acquired AKI: Patients admitted to hospital with AKI apparent based either on reduced urine output or the first SCr measured within 24 h of hospital admission.
Hospital-Acquired AKI: Was defined as the development of AKI during hospitalization, on a patient who was admitted with normal kidney function.
Type of dialysis: The method used for renal replacement therapy in our study was hemodialysis. The option available was intermittent hemodialysis. For hospitalized patients, it was done in a centre-based haemodialysis in the hospital. After discharge, hemodialysis treatments were performed in a unique dialysis center (two or three times per week) after regular travel until renal recovery function.
Renal function recovery: Was defined as the return of serum creatinine (sCr) level to the baseline. In the absence of a known baseline sCr, renal function recovery was defined in the absence of definition criteria for AKI according to KDIGO 2012.
AKI management protocol: Once the disease was diagnosed, treatment was instituted promptly. After clinical and biological assessment, two axes in the treatment were distinguished: the treatment of etiology and treatment of complications of AKI (hyperkalemia, metabolic acidosis, hyponatremia). Indications of renal replacement therapy used in our study were conforming to the recommendations of the KDIGO 2012.
Our dependent variables were: Direct cost, indirect cost, and global cost. The independent variables were: socio-demographic (age, sex, occupation, monthly income and source of funding), clinical (place of acquisition of AKI, stage of severity according to KDIGO 2012, comorbidities and etiologies), hospital (length of stay, dialysis and recovery time) and prognosis (mortality).
We used a standardized form for data collection. The collection was done prospectively and done daily during the period of hospitalization. The medical and nursing record was analyzed to record the care provided to patients. We used the hospital price schedule when billing for medical examinations, care, medication and other medical consumables. Data collection continued during outpatient follow-up and was completed after complete recovery of renal function.
The data was saved in a computer using the CS Pro version 4.1 software. The data were analyzed by descriptive and analytic statistics methods using SPSS (Statistical Package of Social Sciences) software, version 20.0. The quantitative variables were expressed on average with their standard deviation, the median and interquartile range was used when the distributions did not follow a normal distribution. The qualitative variables were expressed as a percentage. Student's "T" test and variance analysis (ANOVA) were used for the comparison of averages; non-parametric equivalents were used case dependently. Since our dependent variables were quantitative, linear regressions were used to determine the elements associated with high cost. The alpha risk was set at the 5% threshold, so a value p ≤ 0.05 was considered statistically significant.
We submitted the research project for approval to the Ethics Committee of the Faculty of Medicine and Biomedical Sciences. The authorization of the authorities of Douala general hospital has been obtained. Informed and written consent of the patient was obtained after reading and explanations. The collected data has been codified and stored in strict respect for the privacy of patients.
During the study period, we recruited 45 patients treated for AKI; 03 patients were excluded, 02 for AKI on CKD and 01 during follow-up. A total of 42 patients were included (Figure 1). Of these 42 patients: 22 (52.4%) were female; the mean age was 55.5 ± 19 years (min: 15 - max: 81 years). The most represented occupational class were retirees with 13 (31%) patients (Table 1); 23.8% of the patients were unemployed (Table 1). Approximately 22 (52%) patients had a monthly income ≤ XAF 100,000 ($176.8) (Table 1). More so, among the 11 patients (26% of our workforce) with an income > XAF 200,000 ($353.9), more than half (45.5%) were insured. During hospitalization, the source of funding was the family in 28 (67%) cases and health insurance companies in 21% (Table 1).
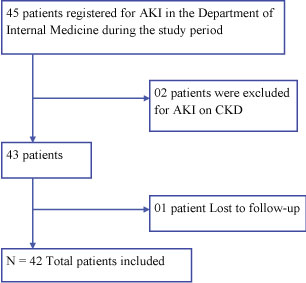 Figure 1: Flowchart illustrating the selection process. View Figure 1
Figure 1: Flowchart illustrating the selection process. View Figure 1
Table 1: Socio-demographic characteristics of patients with acute kideny injury (n = 42). View Table 1
The AKI was acquired in community in 90% (n = 38) cases (Table 2). Out of the 4 patients presenting with hospital-acquired AKI: 2 (50%) cases of AKI were related to dehydration due to polyuria induced by drug and 2 (50%) cases were related to nosocomial sepsis. Sepsis was the leading cause of AKI acquired in the community with a high frequency (N = 38, n = 26, 68.4%) in the patients. High blood pressure and diabetes were the major comorbidities identified in 13 (31%) and 06 (14%) patients, respectively (Table 2). The average hospital stay was 09 ± 5 days.
Table 2: Clinical characteristics of patients (n = 42). View Table 2
Therapeutically, the mean recovery time for renal function was 10 ± 11 days (median 07 days); it was statistically higher among dialysis patients (39 ± 25 days) than non-dialysis patients (7 ± 5 days), p = 0.008. Only 04 patients required dialysis for an average dialysis session of 7 ± 6 days (Table 3). We recorded one death following AKI at stage 3 of severity of KDIGO 2012, a mortality rate of 2.38%.
Table 3: Length of hospitalization, recovery & number of dialysis sessions (n = 42). View Table 3
It averaged XAF 455,444.8 ± 383,293 ($805.7) per patient when management was global, involving both dialysis and non-dialysis patients (Table 4). The median of this cost was XAF 335,815 ($594.1); IQR [XAF 189,680-559,098]. Most of the expenditure came from case processing (34.3% of direct cost) and other intra hospital costs (36.9% of direct cost), including the cost of room and hotel services (Table 4).
Table 4: Distribution of direct costs according to the different items of expenditure (n = 42). View Table 4
In the specific "non-dialysis" subgroup (n = 38), this direct cost was XAF 371,018.5 ± 261,387 ($656.39). The median of this cost was XAF 283,687 ($501.9); IQR [XAF 182,855-459,115]. In this subgroup, "Other intra-hospital costs" represent the main item of expenditure with 42% of the direct cost (Table 4). In the specific subgroup of "dialysis patients" (n = 4), this cost is calculated at XAF 1,257,495.0 ± 466,009 ($2,224). The median of this cost was XAF 1,431,777 ($2,533); IQR [XAF 951,675-1,563,315]. Dialysis is the largest expense item with 40.2% of direct cost (Table 5). In univariate analysis, the factors influencing direct cost in the total population (n = 42) were: length of hospital stay (r = 0.8, p ≤ 0.001), duration of renal recovery function (r = 0.7, p ≤ 0.001), stage of clinical severity (p ≤ 0.001), dialysis (p ≤ 0.001). Table 5 summarizes the elements of comparison and regression.
Table 5: Univariate analysis of the factors influencing the direct cost. View Table 5
In the total population (n = 42), the average indirect cost per patient in the management of AKI is estimated at XAF 521,111.2 ± 2,969,310 ($921,9). The median of this cost was XAF 47,260 ($83.6); IQR [XAF 25,757-47,260]. Losses from premature death account for the majority (87.6%) of indirect costs in the total study population (Table 6). In "non-dialysis" patients (n = 38), the indirect cost was XAF 61,050.8 ± 53,517 ($108.1). The median of this cost was XAF 35,512 ($62.8); IQR [XAF 25,014-95,014].
Table 6: Distribution of indirect costs according to the different items of expenditure (n = 42). View Table 6
No deaths were recorded in the non-dialysis subgroup. Transport costs are therefore 47.9% of losses (Table 6). In "dialysis patients" (n = 4), the indirect cost was XAF 4,902,183.4 ± 9,601,477 ($8,672). The median of this cost was XAF 129,770 ($229.6); IQR [XAF 66,515-9,737,851]. The cost of premature death is the most important (Table 6) of the losses (97.8%).
It was calculated as the sum of direct and indirect costs. Its average value was XAF 977,556.0 ± 3,170,467 ($1,729). The median of this cost was XAF 402,473 ($712.1); IQR [XAF 212,813-628,396]. Among the "non-dialyzed" subgroup (n = 38), the average was XAF 432,069.5 ± 304,789; ($764.4). The median of this cost was XAF 327,197 ($578.9); IQR [XAF 210,866-595,728]. Among "dialysis patients" (n = 4), the average was XAF 6,159,678.4 ± 9,831,321; ($10,897). The median of this cost was XAF 1,561,547 ($2,762); IQR [XAF 1,018,190-11,301,166]. This cost was statistically higher than for "non-dialysis patients" (p = 0.001).
Subsequently in the analysis, the main items of expenditure in the management of acute kidney injury were: Hospitalization costs, dialysis, treatment of the cause and death.
The purpose of this study was to determine the economic cost in managing acute kidney injury in the internal medicine unit of a tertiary care hospital. It was a study on the cost of illness. Costs were calculated from the point of view of the patient and society; thus, three types of costs were identified: direct, indirect cost and global or economic cost.
The direct cost defined as the value of goods and services paid for the treatment and rehabilitation of the patient was calculated on average at XAF 455,444.8 ± 383,293 (median: XAF 335,815), corresponding to 47% of the overall cost. It represents as 0.8% of the gross domestic product per active population per year in 2012 (XAF 548,018.8). This concurs to assert that it is high for the average Cameroonian.
Few studies are published on the direct costs of AKI in developing countries as a point of comparison. Chertow [15] in 1998 in the United States estimated the additional expenditure in patients with a rise of 5 mg/l of serum creatinine to 7,500 US dollars, approximately XAF 4,357,500 (according to the exchange rate). The comparison of this cost with ours was difficult because it depends on the factors related to the health system, the standard of living and the characteristics of the patients included in the study. Indeed, in the Chertow study, it was a predominantly third-age population with multiple comorbidities in a high-income country compared to ours.
There was a statistically significant difference (p ≤ 0.001) between the average direct cost for dialysis patients XAF 1,257,495.0 ± 466,009 ($2,224), which was 3.3 times higher when compared to non-dialysis patients. XAF 371,018.5 ± 261,387 ($656.39). Manns [17] in a retrospective study conducted in Canada from 1996 to 1999 estimated that the average direct cost of AKI management in patients requiring only dialysis was approximately $11,192 (XAF 5,085,644.8). The study was conducted in an intensive care unit where the daily care costs are higher than those used in the internal medicine departments, as was the case in our study, in addition to the treatment mode in Intensive care unit was continuous hemodialysis with therefore a higher operating cost than intermittent dialysis as was the case in our study.
The analysis of the direct cost highlights the weight of the cause of treatment of AKI and that of the hotel services in the management of the pathology in our study. While the cost of treating the cause of AKI represents only 34.3% of direct cost and dialysis treatment 10.6%; most of this direct cost (36.9%) is generated by "other intra-hospital costs". it is determined mainly by the costs related to hotel services (room, linen, meal tray) for a daily amount of XAF 13,900 ($24.6) and XAF 39,200 ($69.4) for the common and single rooms respectively.
Also, it should be noted that in the subgroup of dialysis patients, the patient will pay 60% of the direct cost out of his pocket, in fact the state's financial contribution is 40%, and the subsidy taking into account was XAF 5,000 ($8.9).
The indirect cost, being the value of productivity losses caused by the disease and its complications (morbidity) and by premature deaths (mortality). We added to this, the additional expenditure of families. It was calculated at XAF 521,111.2 ± 2,969,310 ($921,9); it accounted for 53% of the economic cost. Losses from premature death accounted for most of the indirect cost in the total study population (88% of the indirect cost). This effectively reflects the loss in terms of future gain on a state's economy. The additional expenses of the families represented 10% of the indirect cost. They are not negligible in a context where the implementation of health insurance is not yet effective to all Cameroonians. Productivity losses due to temporary work disability, loss of productivity caused by premature death and even additional family expenses prove that the disease does not only affect the patient's pockets (direct cost) but also affects the society in terms of productivity losses.
The global cost or economic cost of the AKI defines the sum of the direct and indirect costs to be an average of XAF 977,556.0 ± 3,170,467($1,729). In comparison, the 2015 annual gross domestic product (GDP) per capita in Cameroon was $1,335. Few studies are published in developing countries as those developed on the economic cost that can be compared. Nevertheless, by comparing this global cost with that of the other conditions within the same socio-demographic and economic environment, we see that it seems higher than the cost of stroke estimated at XAF 802,000 ($1,418) by Mapoure [18] in 2013 at the Douala general hospital. Likewise, this cost seems to be higher than that of malaria estimated at XAF 480,000 ($849.2) in 2014 in two tertiary care hospitals in Cameroon by Lakoudji [19].
All these elements help to show the economic burden of the AKI in Cameroon, where the universal health insurance system remains non-functional and where it is often the patient or his family who pays for the care. This reality is in line with the results of our study, where 67% of patients were able to pay for drugs and other intra hospital expenses thanks to the contribution of the family. Only 21% of patients had health insurance. Also, 52% of our patients had a monthly income ≤ XAF 100,000 ($176.8) against 26% who had an income > XAF 200,000 ($353.9); paradoxically, it is this income group that had the majority of the insured patients (45.5%).
Factors that contribute to increasing the costs of AKI: The variables influencing direct cost in this study were: length of hospital stay, duration of renal recovery function, stage of clinical severity and dialysis. Indeed, the stage 3 of severity is associated with the higher risks of complications, thus of recourse possibly dialysis with all the consequent expenses. Similarly, as the length of stay increases, so does the cost of hotel services. Death, on the other hand, is responsible for a huge loss of productivity, which will increase with the early death deemed premature.
AKI is a common clinical problem that is associated with increased in-hospital morbidity and mortality. Its treatment must be imperative to avoid serious complications that may be life-threatening. In order to reduce the burden of the disease, preventive measures must be instituted in all hospitalized patients. This involves identifying the procedures and conditions that are more commonly associated with AKI; identifying high-risk patients (comorbidities), earlier detection of the AKI condition using new biomarkers, optimizing fluid balance and avoiding nephrotoxins (prescribe medicines Safely) [20,21].
The limits of this study reside in the lack of characterization of the "intangible" costs defined as the distress and pain felt by the patient and the others. These effects related to the loss of well-being are real, but the main difficulty lies in the quantitative estimate or even the monetary valuation of these effects. A limit of this study could be the place of recruitment. In fact this study took place within a department of internal medicine, as well as different aspects of the AKI diagnosed in intensive care unit. Pediatrics and Gynecology were not included in this study.
We recorded one death in our study. This was the only case of glomerulonephritis diagnosed after renal biopsy. Glomerulonephritis is a serious medical condition whose treatment is long, difficult and expensive. Furthermore, the exact weight of death is difficult to define in this study because only one case was recorded. This is a limit of the study related to the size of the sample. Another limitation lies in the selection criteria. Patient who did not have a creatinine prior to hospitalization, so the failure to recover renal function within three months was a criterion of exit from the cohort because we could not know if it was a question of an AKI on chronic kidney disease or the natural course of acute kidney injury in these patients. From there, we can say that the costs generated by the transition to chronicity of the AKI have not been valued in this study.
The average global cost of managing acute kidney injury in a tertiary hospital is XAF 977,556.0 ± 3,170,467 ($1,729). The direct cost represents 47% of the overall cost. Direct expenditures are dominated by hospitalization and treatment of etiological factors. The indirect cost represents 53% of the total cost; the cost of premature death is the main factor generating this indirect cost. In our country, the guaranteed minimum wage was XAF 36,270 ($64.17). Therefore, we can say that the overall cost or economic cost of managing the AKI remains high for society and the average Cameroonian.
The authors do not declare any conflicts of interest.
"This work was supported by two of the authors: Tchuenkam Wakheu Landry and Ashuntantang Gloria". Also, the research did not receive specific funding.
‘Not applicable' in this section.
Written informed consent was obtained from the patients for data collection.
We obtained the ethical clearance of the ethics committee of the Faculty of Medicine and Biomedical Sciences of University of Yaounde I.
TWL and AG contributed in design of the study and writing of the manuscript HMP and NZ contributed in critical reading TL contributed in statistical analysis.
All authors have read and approved the final version of the manuscript.
To the medical and nursing staff of the Medicine Unit and Intensive Care Unit of the Douala general hospital for the care of the patient.
To the administrative staff of the Douala general hospital who made this study possible.
The direct cost of managing acute kidney injury is high.
This study brings again:
• An estimate of the cost of managing acute kidney injury in low-income countries.
• In addition to the direct cost, the indirect cost and hence the economic cost of the disease.