Limited research has been conducted in the United States in which exposure to solar UVB light is studied in a natural setting as a strategy to improve vitamin D status in institutionalized older adults.
This pilot study aimed to determine if sunlight exposure therapy on one-quarter body surface area three times per week for one month during summer (July-August) midday hours, to produce 500 IU vitamin D, improved intervention participants’ (n = 6) vitamin D status. Control group participants (n = 4) received the usual care, which included occasional sunlight exposure. The study also evaluated therapy adherence and attendance to outdoor activities that facilitated the therapy. Serum levels of 25 hydroxyvitamin D [25(OH)D] were measured at baseline and at study-end..
Five men and five women, patients of a skilled nursing facility in Sunnyvale, California, with daily vitamin D intake greater than the Recommended Dietary Allowance levels, skin types II, III, IV, and V and mean age (± SD) of 73 ± 15 years were recruited.
All four intervention group participants with vitamin D insufficiency status [serum 25(OH)D 50-75 nmol/L] at baseline observed change to sufficiency status [serum 25(OH)D > 75 nmol/L). All control group participants with insufficiency status (n = 2) at baseline remained insufficient. Mean change in serum levels of 25(OH)D between groups was not statistically significant. Adherence to sunlight exposure sessions was high with a mean number of sessions (± SD) attended of 14 ± 2 out of sixteen possible scheduled sessions.
This pilot study demonstrates that the population studied adheres to sunlight therapy when support is provided, however in order to evaluate the benefits of sunlight therapy for institutionalized older adults, larger studies would be needed to attain statistical significance.
Older adults, Improve vitamin D, Insufficiency status, Sunlight, Skilled nursing facility
• An individualized summer sunlight exposure therapy for older adults, three times per week, on 25% of BSA, in combination with dietary supplementation above Recommended Dietary Allowance levels may improve vitamin D insufficiency status to sufficiency.
• Skilled nursing facility patients adhere to short-term sunlight exposure therapy when the infrastructure is adequate and support is provided.
Widespread avoidance of sun exposure and the use of sunscreens have increased the prevalence of vitamin D inadequacy among Americans and worldwide [1,2]. Older adults with limited access to sunlight in the Northern Hemisphere are at greater risk for vitamin D deficiency and insufficiency [3,4]. Researchers have found vitamin D deficiency and insufficiency in institutionalized older adults despite the use of vitamin D supplementation [5]. Positive attitudes in institutionalized older adults toward outdoor activities and sun exposure suggest the potential for effective outdoor sun exposure programs [6].
The Institute of Medicine (IOM) and the Endocrine Society agree that blood levels of 25 hydroxyvitamin D [25(OH)D] > 50 nmol/L are necessary to avoid abnormalities in calcium, phosphorus, and bone metabolism; however, only the Endocrine Society recognizes the benefits of serum 25(OH)D > 75 nmol/L to increase the efficiency of intestinal calcium absorption [3,4]. Recent research shows that serum levels of 25(OH)D below 75 nmol/L in older adults are associated with increased risk for falls, cancer, cardiovascular disease, and bone fractures [2,7-9]. For the purpose of this study, we have adopted the Endocrine Society’s clinical practice guidelines that define serum levels of 25(OH)D < 50 nmol/L as vitamin D deficiency, 50-75 nmol/L as insufficiency, and > 75 nmol/L as vitamin D sufficiency [4].
Naturally occurring vitamin D in food is limited; thus, humans cannot maintain vitamin D sufficiency from food alone [4]. Ultraviolet-B (UVB) radiation from sunlight (Wavelength 290-315 nm) is a natural, safe, and effective source of vitamin D [10]. Exposure to sunlight allows the body to synthesize up to 90% of vitamin D requirements, without the risk of toxicity [11,12]. In most areas of the United States (between latitudes 29.0 N. and 42.5 N.) the young healthy population can synthesize 1000 International Units (IU) vitamin D3 in minutes from sun exposure of one quarter Body Surface Area (BSA) during summer midday hours [13,14].
The majority of in vivo studies that analyze the effects of UVB light in humans rely on artificial sources, and their results may not be applicable to a natural setting [15-18]. Limited research has been conducted in the United States in which exposure to solar UVB light in a natural setting is studied as a strategy to improve vitamin D status in institutionalized older adults. Vitamin D synthesis from solar UVB radiation depends on a person’s age, skin type, amount of skin exposed, time of day of exposure, and amount of ambient UVB light available (based on altitude, latitude, and time of year) [4,13]. People living in the San Francisco Bay Area in California would have different sunlight exposure requirements, and possibly different cultural views towards sunlight, than individuals living in other parts of the world.
The purpose of this pilot study was to determine if vitamin D status of older adult Skilled Nursing Facility (SNF) patients in Santa Clara County, CA improved with increased sunlight exposure. In addition, the study evaluated the adherence to summer natural sunlight exposure therapy and outdoor activities that facilitate sunlight exposure.
The study population consisted of five men and five women living in a SNF with a population of 172 residents, located in Sunnyvale, California (latitude 37.4°N, longitude 122.0°W, and surface altitude 0.0405 km above sea level). Residents were eligible for inclusion if they were aged ≥ 50 years, ambulant or able to move outdoors with the use of wheelchair, able to follow study directions, and had no history of skin cancer, major burns on hands, arms and/or face, and no contraindication for sunlight exposure. The nursing facility staff randomly assigned participants to control and experimental groups; however, randomization was lost because one control group participant began outdoor physical therapy three times per week and was shifted to the experimental group. Participants gave written consent prior to group randomization. The San José State University Institutional Review Board approved this study.
The intervention consisted of sunlight exposure, three times per week for one month during summer (July-August) midday hours. Intervention participants exposed one quarter BSA (arms, hands, face and neck) for the amount of time it takes young healthy individuals to reach one quarter Minimal Erythemal Dose (MED) and produce the equivalent to 1000 IU vitamin D (approximately 500 IU vitamin D in older adults) [14]. Percentages of BSA were based on the Lund and Browder Chart for skin burns: face 3.5% and neck 2%, arms 14%, hands 6%, legs 14%, and thighs 18%. The length of sunlight exposure per session was calculated using a validated web-based tool that relies on latitude, longitude, altitude, ambiance, surface type, total ozone column (Dobson Units), date, time of day of exposure, Fitzpatrick’s skin type (I-VI), percent BSA exposed, and desired dietary equivalent dose of vitamin D [19]. Appendix A shows a list of the calculated sunlight exposure times by date per skin type.
The facility chef led outdoor cooking activities every Monday, Wednesday and Friday between 1030 hrs and 1130 hrs, at the wheelchair accessible, outdoor patio and vegetable garden on the SNF premises. The outdoor activities were designed to encourage experimental participants to spend time in the outdoors so that they could be offered the opportunity to expose skin to direct sunlight. Control group members were not discouraged from participating in the outdoor activities which were held under a canopy, however they were not invited to participate in the intervention. Three employees from the SNF nutrition department assisted as chaperones and accompanied intervention participants while outdoors and during sunlight therapy sessions. On sunlight therapy session days, chaperones approached intervention participants for interest in outdoor cooking activities, and gave them the option to expose 25% BSA to sunlight between 1100 hrs and 1130 hrs. Experimental participants not interested in participating in outdoor cooking activities were encouraged to sit/walk around the vegetable garden to accomplish sunlight exposure therapy. The control group received the usual care, which may have included occasional exposure to sunlight.
Precautions were taken to reduce the risk for falls and sunburn. Chaperones accompanied participants to, from, and during each session to prevent falls. Sunscreen and shade (e.g. umbrellas, tree shade) were offered as soon as the effective amount of sunlight exposure was reached. UV light protecting sunglasses and water were offered on every session to prevent eye discomfort and dehydration. Sunlight exposure therapy was offered only in weather temperatures between 20 ℃ and 27 ℃, and cloudiness less than 50%. Chaperones were asked to report any complains of discomfort and/or excessive sun exposure.
Non-fasting blood samples were collected during morning hours at baseline and at study-end. Baseline samples were taken 12 days prior to the initial intervention and study-end samples 6 days after the final intervention. The Laboratory Corporation of America (LabCorp, Sunnyvale, CA, USA) conducted the serum 25(OH)D test using immunochemiluminometric assay performed on DiaSorin Liason (DiaSorin Inc., Stillwater, MN, USA).
Age, gender, ethnicity, skin type, typical levels of sun exposure and sunscreen usage were self-reported on a simple-choice questionnaire. Appendix B shows questionnaire used to collect demographics and sun exposure history. At baseline, the SNF dietitian provided participant’s height, weight and daily vitamin D consumption from food and supplements. Body mass index (BMI) (kg/m2) was calculated using participant’s weight in kilograms and height in meters.
Every session, chaperones recorded length of sun exposure, percent BSA exposed to sunlight, total time spent outdoors and attendance to outdoors cooking activities.
The data were analyzed using SPSS version 22.0 (SPSS, Chicago, IL, USA). Independent student’s-t test was used to examine significant differences at baseline and study-end between groups. P values < 0.05 were considered statistically significant and the results were expressed as mean ± Standard Deviation (SD).
The San José State University Nutrition, Food Science, and Packaging Department’s Circle of Friends Research Assistance Award supported this work. The sponsor had no role in the study design, subject recruitment, data collection and analysis, decision to publish or preparation of the manuscript.
Participants were mainly of White/Caucasian ethnicity (n = 8), with skin types II (n = 1), III (n = 6), IV (n = 2), and V (n = 1), and a mean age of 73 ± 15 years. At baseline, none of the participants were vitamin D deficient, six had insufficiency and four were at sufficiency levels. Mean total daily vitamin D intake in both groups was above the Recommended Dietary Allowance (RDA) (600 IU for individuals age 50-70 yrs, and 800 IU for age > 71 yrs) [3]. Nine out of ten participants reported pre-study typical sun exposure of less than 60 minutes per week (< 30 minutes n = 5, 30-60 minutes n = 4), and the majority (n = 7) never using sunscreen while outdoors. There were no significant differences between the two groups. A comparison of demographic and clinical characteristics of participants by group at baseline is presented in Table 1.
Table 1: Baseline demographic and clinical characteristics of study participants by group allocation. View Table 1
Adherence to sunlight exposure sessions was high with a mean number of sessions attended of 14 ± 2 out of sixteen possible scheduled sessions. One session was cancelled do to cloudiness > 50%. Five of the six intervention participants met or exceeded their calculated sunlight exposure time. Mean average percent BSA exposed by intervention participants was 23 ± 4.4. Statistical significant difference between groups was found for: average sunlight exposure (< 0.0001), average percent BSA exposed to sunlight per session (< 0.0001), and number of sunlight exposure sessions attended (< 0.0001). Without the encouragement of chaperones, attendance to scheduled outdoor cooking activities by control group participants was observed. The mean number of outdoor cooking activities attended was not significantly different between groups with 8 ± 4 by intervention group and 3 ± 4 by control group. Table 2 shows a comparison between participants, on sunlight exposure therapy adherence, time spent outdoors per session and attendance to outdoor cooking group activities.
Table 2: Comparison by participant of the average length of calculated and recommended sunlight exposure sessions, average sunlight exposure time per session, average percent BSA exposed to sunlight per session, number of sunlight exposure sessions attended and number of scheduled outdoor activities attended. View Table 2
Over the period of 1 month, two intervention participants with insufficient vitamin D status at baseline observed the largest increase in serum 25(OH)D (22.5 nmol/L) by study-end. Mean change of serum 25(OH)D levels was similar between groups with an increase of 11.2 ± 11.0 nmol/L in the intervention group and 9.7 ± 5.2 nmol/L in the control. No significant difference was observed in the overall vitamin D level change between groups at study-end; however, Figure 1 shows that all (n = 4) intervention group participants with an insufficient vitamin D status at baseline improved status to sufficiency by study-end, while all (n = 2) control group participants with insufficiency status at baseline remained insufficient. Regardless of group placement, all participants with sufficiency status at baseline maintained sufficiency.
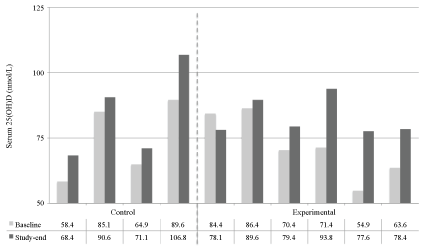 Figure 1: Serum levels of 25(OH)D for all participants at baseline and study-end. Note: Baseline and study-end values are in nmol/L. The dashed vertical line between columns 4 and 5 seperates results for the control and the experimental group. Serum levels of 25(OH)D < 50 nmol/L represents deficiency status. Serum levels of 25 (OH ) D > between 50 and 75 nmol/L represent insufficiency status. Serum levels > 75 nmol/L represents sufficiency status. All participants of 25(OH)D > 50 nmol/L (above defiency status) at baseline and study-end. View Figure 1
Figure 1: Serum levels of 25(OH)D for all participants at baseline and study-end. Note: Baseline and study-end values are in nmol/L. The dashed vertical line between columns 4 and 5 seperates results for the control and the experimental group. Serum levels of 25(OH)D < 50 nmol/L represents deficiency status. Serum levels of 25 (OH ) D > between 50 and 75 nmol/L represent insufficiency status. Serum levels > 75 nmol/L represents sufficiency status. All participants of 25(OH)D > 50 nmol/L (above defiency status) at baseline and study-end. View Figure 1
Baseline serum 25(OH)D levels of participants in this study were consistent with those observed in a previous study analyzing vitamin D levels in older adult nursing home residents receiving vitamin D supplementation. Hamid, et al. studied vitamin D status in older adult (age > 65 yrs) nursing home residents receiving vitamin D supplementation (72% receiving 400 IU, 12% 600 IU, and 7% 800 IU), and found insufficiency in 50% of the population and deficiency in 16%, and suggested the need for greater vitamin D supplementation doses to reach vitamin D sufficiency [5]. All participants in our study exceeded current vitamin D RDA with a daily average in dietary vitamin D intake of 1328 ± 238 ranging from 960-1720 IU. None of the participants had serum vitamin D deficiency levels at baseline; however six out of ten (60%) had insufficiency serum vitamin D levels. Researchers have previously suggested that vitamin D intake for adults should be ≥ 2000 IU per day in the absence of adequate sun exposure to achieve and maintain vitamin D sufficiency [20]. This is in line with more recent data supporting supplemental vitamin D dose recommendation of 1500-2000 IU/d for people older than 50 yrs to maintain serum 25(OH)D above 75 nmol/L [4].
The positive effects of artificial UVB light on serum 25(OH)D levels in older adults have been demonstrated on multiple occasions; however, one limitation of these studies is that the results cannot be applied to a natural setting [15,16]. This study explored the effects of moderate sunlight exposure therapy in a natural setting as an additional vitamin D source for SNF older adult residents already receiving oral vitamin D from food and supplements. Two earlier studies conducted in Japan (12 months in length) and New Zealand (4 weeks in length), that analyzed the effects of daily natural sun exposure on serum 25(OH)D levels in older adult nursing care residents, were able to demonstrate significant increase in serum 25(OH)D levels after daily sun exposure greater than 15 minutes [21, 22]. Neither study explained how exposure times of 15 minutes (Japan study) and 15 and 30 minutes (New Zealand study) to natural sunlight were determined, or whether the volunteers received any form of oral supplementation.
Given concerns in the general population about the negative effects of excessive sun exposure, this study relied on a validated UVB light exposure calculator in order to provide safe and effective solar UVB light levels. The web-based calculator was designed for young healthy individuals and did not take into consideration participant’s age. It has been demonstrated that epidermal stores of 7-dehydrocholesterol available in the skin for serum 25(OH)D synthesis declines with age, and that young individuals (age 8-18 yrs) produce at least twice the amount of 25(OH)D than older adults (77-82 yrs); suggesting that older adults may require twice the sun exposure time as younger individuals to produce similar serum 25(OH)D levels [23]. We calculated that participants of this study would produce approximately 500 IU vitamin D with each sunlight exposure session.
It is difficult to attribute improvements in vitamin D status observed in intervention participants with insufficiency status at baseline solely to sunlight exposure, as all non-sunlight exposure participants also saw an increase in serum 25(OH)D levels during the same time interval. A recent study conducted in Australia that evaluated the effects of solar UVB light (30 to 40 minutes in morning) on SNF older adults with duration of 1 year, did not find statistical significant difference in the overall change in serum 25(OH)D levels between control and intervention groups, and revealed difficulties in obtaining ongoing adherence to the treatment [24]. In contrast, participants in both the control and treatment groups of our study chose to participate in structured outdoor activities, indicating that the availability of these activities may enhance treatment compliance. Chaperone support and outdoor facilities of the SNF may have been key factors in the compliance of participants providing support and an inviting environment for outdoor activities. No intervention related complaints were recorded for falls, discomfort or sunburn during the study. Given that intervention group participants had skin types II, III, and IV; findings of this study may not apply to an elderly population with skin types I, V and VI.
From a clinical perspective the most important finding of this study is related to those participants who were at a vitamin D insufficiency status at baseline. All participants in the intervention group with a vitamin D insufficiency status at baseline improved to sufficiency status by study end; comparatively all participants in the control group who had an insufficiency status at baseline remained at an insufficiency level by study-end. The lack of significant statistical difference in the overall change in serum vitamin D levels between our two groups could be attributed to the low number of participants (n = 10). Additional studies in a larger population would need to be conducted to determine if the trends observed in the present study are likely to be observed in a larger population.
In conclusion, this pilot study of an older adult population living in a SNF in Sunnyvale, CA demonstrates that adherence to an individualized summer sun exposure therapy, three times per week, on 25% of BSA, is feasible when outdoor activities and support are provided. In order to evaluate the benefits of sunlight therapy for institutionalized older adults, larger studies would be needed to attain statistical significance.
The sponsor of the submitted article had no role in the study design, subject recruitment, data collection and analysis, decision to publish or preparation of the manuscript. The opinions expressed in this article are those of the authors alone and do not reflect in any way those of the institution to which they are affiliated. There are no conflicts of interest to be declared.