Background: Rapid developments in technology demand the use of various electronic devices in daily life. Adolescents and younger adults are reported to consume more technology compared to other age groups. Examining the health implications of device use may assist with population level prevention and wellness strategies and stakeholder education.
Objective: To systematically examine the literature regarding the effects of electronic device usage on the musculoskeletal system in adolescents and young adults.
Method: Four electronic databases (OVID Medline, PubMed, EBSCOhost, and Scopus) were searched for peer-reviewed articles published in English between 2011 and 2021. All selected articles were critically appraised and examined for risk of bias. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were used to report data.
Result: Sixteen articles met the inclusion criteria. The evidence synthesis revealed an association between electronic device use and musculoskeletal impairments. Notably, excessive use and non-neutral postures during the use contributed to musculoskeletal discomfort and disorders. Neck, upper and lower back, and upper extremities were the most affected body regions.
Conclusion: Prolonged use of electronic devices and maladaptive postures while using may contribute to musculoskeletal impairments in adolescents and young adults.
Occupational therapy, Posture, Upper extremity, Pain, Electronics
Technology has become an integral part of our lives. To access technology, people use electronic gadgets. During recent years, touchscreen smartphone devices have become increasingly accessible to all ages and budgets and therefore, are often commonly used on a daily basis [1]. Approximately 61% of the global population use the internet, 67% use a mobile device, and 56.8% actively use social media. Additionally, social media usage has increased by 13.1% in the past 12 months [2]. Due to the greater accessibility of and higher demand for technology, a resulting dependency has developed in educational and employment settings. Further, the recent pandemic has caused a shift toward and surge in the electronic device usage for work and educational purposes.
The use of electronic devices, including mobile computers, leads to frequent deviation from neutral body positioning, such as non-neutral posture, sustained posture, repetitive motions, and awkward movements that causes stress to musculoskeletal system. This can result in ergonomic difficulties which may contribute to development of musculoskeletal disorders (MSDs) [3]. MSDs are defined as injuries and/or disorders of the muscles, tendons, cartilage, joints, and spinal discs [4].
Literature reveals a strong association between device use and musculoskeletal issues. Xie, et al. explored the physical demands imposed on muscles and joints in different body regions through the use of electronic devices and found that typing on the computer placed higher demand on the neck and back muscles (upper and lower trapezius) and hand muscles (wrist and finger extensors) compared to touchscreen typing [5]. They also found that greater demand was placed on the neck extensors and thumb muscles during texting on touchscreen smartphones. Kaya Aytutuldu, et al. also found a strong association between symptoms in the upper extremity and those who regularly used computers at work [6]. Yu, et al. reported that head and neck issues were associated with poor placement of the screen in mobile computer users (laptop/tablet) [7].
The positioning of devices in relation to the users was found to be a contributor to the risk of back pain and the symptom severity is influenced by factors such as posture, devices used, duration of use, and gender [8,9]. Yoakum, et al. examined the influence of anthropometric factors such as height, weight, and sex of individuals on neck positions when using devices. They attributed the degree of impact of neck flexion to sex and height characteristics, and posited that females experience more mandibular protrusion with device use than males [10].
Evidence indicates that smartphone usage may also lead to musculoskeletal impairments related to the hand, such as pain near the base of the thumb, De Quervain's tenosynovitis, and osteoarthritis of the first carpometacarpal joint [11-13].
MSDs have huge economic implications for society. The costs related to MSDs include, but are not limited to medical expenses, disability, and lost income. The direct and indirect costs related to MSDs, from 2004-2006, were estimated to be $576 billion and $373 billion respectively [14]. Individuals with MSDs may experience disability and reduced quality of life, which in turn may affect their participation in daily occupations, including education and work, leading to income loss. Employers may incur costs related to decreased productivity and increased absenteeism of their workforce. In 2012, 29% of days off from work were attributed to MSDs [14].
Device usage is popular among youth. The prevalence of device usage was found to be high among young adults and adolescents [15]. Many young adults and adolescents own and use gadgets like cell phones, tablets, and laptops. They use devices to communicate, learn, play, and pursue hobbies. The literature is limited in identifying the effects and long-term implications of device usage among young adults and adolescents.
As prolonged electronic device usage is generally believed to be associated with MSDs, it is possible that the prevalence of MSDs will increase alongside the rise in technology consumption. Given the prevalence and high economic implications of MSDs, it is essential to examine the contributing factors to develop effective prevention and stakeholder education strategies. Hence, this systematic review attempts to examine the current evidence on the effect of electronic device usage on the musculoskeletal system in young adults and adolescents.
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines served as the model for this systematic review [16]. The first six authors determined the search terms with guidance from the institution's librarian (Table 1). To determine initial eligibility, authors reviewed article titles and abstracts from the following databases: Scopus, Ovid, PubMed, and EBSCOhost. Two additional sources were located from reviewing the search results' reference lists. Risk of bias and level of evidence were determined for each reference extracted, based on the guidelines recommended by the American Occupational Therapy Association (AOTA) [17-19]. To determine the reliability of the evidence, bias was graded as low, moderate, or high. The authors used the following inclusion and exclusion criteria to select articles for the review. Disagreements in article selection were resolved through discussion and consensus. A summary of article exclusions with reasoning is presented in the PRISMA diagram (Figure 1).
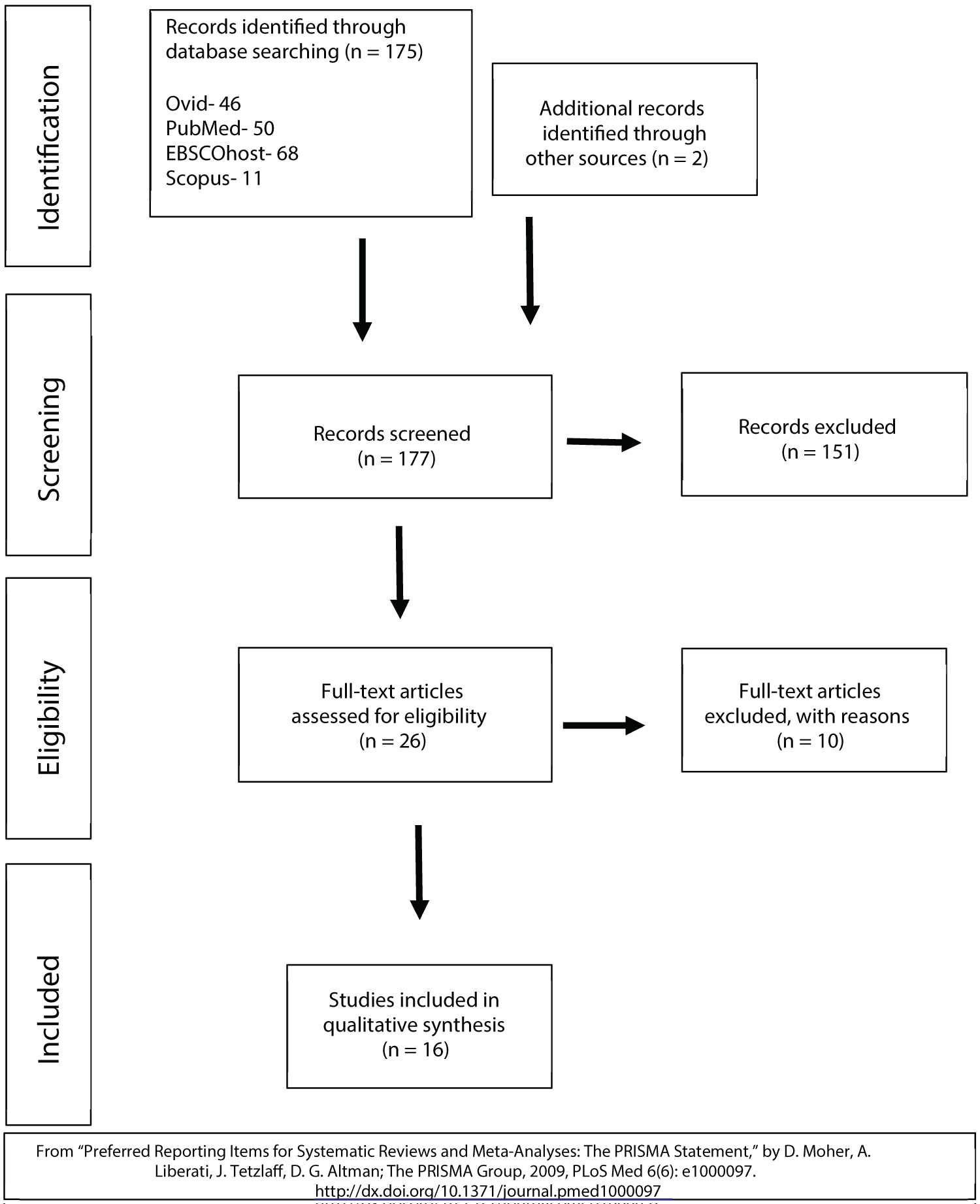 Figure 1: PRISMA diagram.
View Figure 1
Figure 1: PRISMA diagram.
View Figure 1
Table 1: Search strategies and databases. View Table 1
We used the following inclusion criteria to identify articles for this review: (i) Articles published in peer-reviewed journals between 2011 and 2021; (ii) Articles published in English; (iii) Articles that included human participants aged between 10-35 years; (iv) Articles that met a minimum evidence level of 3B as per the evidence table recommended by the AOTA [17]; and (v) Articles that focused on musculoskeletal issues associated with electronic usage. For this review, we considered the use of smartphones, handheld gaming devices, tablets, laptops, and computer devices as electronic usage.
We excluded articles that used electronics as a form of treatment for musculoskeletal diseases and studies that focused on additional factors for effects on the musculoskeletal system other than electronic usage. We also excluded articles that had participants with pre-existing mental or musculoskeletal disorders which could potentially be confounding factors. Two studies were excluded after initial review due to having a low level of evidence, and participants outside the criteria age, respectively [20,21].
Of the 16 articles that met the inclusion criteria, eight were identified as level 2B evidence [22-29] and eight were level 3B evidence [30-37]. The authors examined all 16 articles for risk of bias using the NIH Quality Assessment Tool for Before-After (Pre-Post Studies) with No Control Group (Table 2) [18]. Fifteen articles were determined to have low risk of bias [22-31,33-37] and one was determined to have moderate risk of bias [32]. In seven studies, [23,24,26,29,32,33,35] the authors utilized a self-report survey or questionnaire as the outcome measure collecting data related to pain level, location, and type, presence of numbness/tingling, presence of bruxism (teeth grinding), and diagnosis of temporomandibular disorder. In eight studies [22,27,28,30,31,34,36,37], the authors reported using quantitative assessment measures to collect data related to posture, spinal kinematics, joint positioning and angles, and pain. In one study [25], authors examined the results using both types of outcome measures (a self-report questionnaire on perceived musculoskeletal discomfort and quantitative assessment measures of posture and upper extremity positioning).
Table 2: Risk of bias. View Table 2
The selected studies examined electronic usage pertaining to general amount/duration of use, age at start of use, frequency of use, time of use per week, positioning during usage, purpose associated with use, and types of electronic devices used. Electronic devices used included cellphones/smartphones/mobile phones, tablets, desktop computers, laptop computers, and gaming devices.
Table 3 presents the evidence synthesis. To determine the effect of electronic usage on various body segments, the following analysis groups the articles by the regions of the body reported to be affected (head and neck, upper and lower back, and upper extremity).
Table 3: Evidence table. View Table 3
Twelve studies provided evidence of the effects of electronic usage on the cervical spine. From these studies, 12,253 participants were investigated for the effects of electronic devices on the musculoskeletal system.
Elserty et al. [23] found that the most common area for discomfort was the neck region. Korpinen & Paakkonen [33] and Queiroz et al. [35]. reported that about half of their study participants experienced neck related symptoms. Most of the neck problems appear to be related to increased neck flexion. Tapanya, et al. found that greater neck flexion during smartphone use showed increased biomechanical burden on the cervical spine, resulting in more musculoskeletal discomfort and risk of injury to the area [28]. Short, et al. found a trend that cervical neck flexion during smart phone use could contribute to deformity over time [36]. Similarly, Szucs, et al. found that using a tablet, whether supported on a table or held in the hands, produced the greatest amount of forward head shift and neck flexion [27].
The duration of device usage was reported to contribute to neck related symptoms. Gustafsson, et al. explored the relationship between number of texts sent per day and physical symptoms and found that a higher number of texts sent was associated with neck pain [24]. Lin, et al. found an association between duration of electronic use and posture, with the neck being one of the body regions showing a 13-38% joint movement increase from the middle to end of a typing session [25]. Pais, et al. also assessed long term device usage on neck flexion. The findings indicated a negative association between the duration of digital device use and neck flexion ability [34]. Silva, et al. found that an average electronic device use of 583 minutes per week was associated with pain in the cervical region [26].
Non-neutral postures and patterns of device use were also reported to contribute to musculoskeletal symptoms around the neck region. Douglas and Gallagher used x-rays to examine the effect of trunk position on various intervertebral joints in the cervical spine, including sitting in a reclined, semi-reclined, or upright posture and reported increased demand on the neck in each position when compared to neutral [22]. Toh, et al.'s study revealed a prospective association between the patterns of mobile touch screen device use and musculoskeletal symptoms in adolescents [29].
Aside from the musculoskeletal symptoms related to the cervical spine, one study [32] revealed symptoms related to the temporomandibular joint. In this cross-sectional study, the authors surveyed 578 young adult participants (18 to 35 years of age) on the effects of modern cellular technology on various aspects of life using a self-report questionnaire. The findings indicated that the stress associated with information received by cellular technology and the stress of overuse increased the risk of temporomandibular disorder and bruxism. The study also revealed additional negative consequences including chronic orofacial pain and irreversible damage to hard dental tissue structures.
Eight studies found effects of electronic usage on the upper and lower back. In total, 11,691 participants were identified and studied for the impacts on the upper and lower back.
The back appears to be the region most impacted by device use. Back pain after prolonged device use was reported by nearly two thirds of participants in several studies [26,35]. The factors reported to contribute to neck symptoms also contributed to upper and lower back symptoms. For instance, the duration of device usage [24,26,29] and non-neutral postures [30,31] contributed to musculoskeletal discomfort in the upper and lower back.
The pattern of and posture during use may also contribute to back problems. For instance, walking while using a handheld device was shown to have an impact on spinal positioning, including increase in thoracic kyphosis, lumbar lordosis, and trunk inclination [30,31].
Eight studies focused on the effect of electronic use on the upper extremity in 10,143 participants through quantitative measures and self-report questionnaires and surveys. Overall, the evidence illustrated that electronic use did impact upper extremity positioning in various joints.
Two studies revealed increased wrist ulnar deviation during gadget (smartphone, tablet, etc.) use [36,37]. One of these studies also noted increased radial deviation at the wrist while holding a tablet [37]. Two studies noted higher wrist extension measurements during tablet use [25,37]. Lin, et al. further specified the postures that cause extreme wrist flexion while typing on a tablet and reported that lying in bed has extreme values compared to having the tablet on lap or desk [25].
Device use also affected the positioning of proximal upper extremity joints. Short, et al. highlighted the general trend of flexed elbows and thumb flexion during smartphone use [36]. Szucs, et al. found significant anterior shift and flexion in the shoulders when tablets were supported by a table during the use [27].
Several studies revealed the association between device use and pain in their upper extremities. Silva, et al. reported that 20% of the study participants reported pain in the upper limbs after electronic usage [26]. Toh, et al. stated that device use at baseline was associated with shoulder pain at one year follow-up [29]. In Queiroz, et al.'s study, close to half of the participants reported symptoms in upper extremity joints [35]. Younger (15-year-olds) participants who used at least two electronic devices reported more symptoms.
Lin, et al. found a positive association between the duration of electronic use and musculoskeletal symptoms of pain and discomfort in the upper extremity [25]. Gustafsson, et al. reported an association between upper extremity symptoms such as shoulder pain, numbness/tingling in the hand, etc. and the number of texts sent per day at a one-year follow-up [24].
This systematic review examined the impacts of electronic device use on the musculoskeletal system in adolescents and young adults. A majority of the studies explored the impact of using various electronic devices on multiple body regions. Of the 16 studies evaluated, eight were level 2B and eight were level 3B evidence; thus, the level of evidence for the effect of technology use on the presence of musculoskeletal symptoms is of moderate strength [17]. Overall, the findings suggest that the musculoskeletal system is almost always affected by maladaptive postures and positioning associated with device use and the duration of device use and long-term effects are expected. The following paragraphs discuss each of these findings and offer some general insights on handling these issues.
Non-neutral and maladaptive positions were seen to increase the prevalence of musculoskeletal symptoms in the neck and upper extremities. This could be due to the type of gadgets used (handheld devices), usage pattern and behavior (prolonged use, holding them in hands while using, walking while using smartphones, etc.), and the environment (high or low surface in relation to the user) in which the devices are used. Ergonomic solutions may help mitigate the issue [21].
When considering ergonomic solutions, it is important to understand that ergonomics is about the fit between the user, device, and environment. The usage environment of gadgets needs careful attention as it may contribute to non-neutral or maladaptive posturing. For instance, using gadgets while lying or sitting on a bed may contribute to maladaptive posture of neck and upper body. Gadget use in a sitting posture with a neutral back is generally considered a safe position. To optimize device usage in sitting, mounting devices may be considered. For handheld devices (tablets and smart phones, etc.), mounting devices such as tablet cases, mounting stands, tablet cradles, etc. may be considered. For users who input data through tablets, a keyboard case may be considered. For adolescents accessing gaming technology through gadgets, head mounted virtual reality technology may be considered to encourage neutral posture. Traditional office computer work ergonomic solutions such as adjustable table, office chair with adjustable components, keyboard tray, etc. may help desktop and laptop users.
The users must be encouraged to reflect on their usage pattern and behavior periodically. To promote such reflection, several smart gadgets offer usage data that may provide insight into the duration of use. Additionally, educating users about potential issues may help them appreciate how much they may compromise their health for convenience in usage of electronic gadgets.
Aside from the external modifications and changes in usage pattern and behavior, engaging in stretching and strengthening exercises may help gadget users avoid musculoskeletal issues.
The findings of this review also showed that the prolonged use of electronic devices has an increased negative effect on the body. Aside from the actual device usage, other related variables such as sex [23,26,33,34], presence of a paid job, excess weight [26], and level of exhaustion [32,33], were reported to predict the musculoskeletal symptoms.
Stakeholder education on these predictive factors is the key to mitigate the musculoskeletal issues among young gadget users. Several software ergonomic applications are available in the market that alert the users periodically regarding the duration of usage. For instance, a user may set a timer to go off when it is two hours. The users may be encouraged to download and use these applications on their devices. Measures that promote healthy lifestyle, effective stress management, and work-life balance may also help mitigate musculoskeletal issues in young workers.
The strengths of this systematic review include the examination of the impact of electronic device usage on all body regions, inclusion of studies with moderately large sample sizes, and the consideration of all technological devices that are being utilized on a daily basis. The limitations include the lack of higher-level evidence (level I) and longitudinal studies to examine long-term effects. Also, some studies included in this review were conducted in a laboratory setting rather than natural settings.
The findings have implications for multiple stakeholders, such as healthcare professionals (physicians, occupational therapists, ergonomic consultants, etc.), device manufacturers, teachers, and employers.
• Healthcare professionals may begin to assess and document device usage behavior during annual physical examinations and/or preventive visits to generate data and educate the public on the potential impact of device overuse on the musculoskeletal system.
• Rehabilitation professionals, such as occupational therapists, when providing care to adolescent or young adult patients with musculoskeletal issues, should assess the patient's device use behavior as part of their evaluation. Further, they should educate the individuals who are at risk for developing MSDs on proper body mechanics, ergonomic principles, and environmental modifications associated with device use.
• Electronic device manufacturers may be more competitive if they are more mindful of the musculoskeletal issues associated with device use when designing and manufacturing the device and should include information related to the safe usage of their products inside the product package and on their websites.
• Teachers should ensure that adolescents are using devices and gadgets in moderation to complete educational activities.
• Employers need to ensure that their young workers have proper work/office environment to optimally position and safely use electronic devices to complete work responsibilities.
The emergence of the modern technology era and increased dependency on electronic devices over the last two decades may continue to increase the prevalence of musculoskeletal conditions. Hence, it is essential for the healthcare community to be cognizant of the impacts of device usage on body systems and ways to effectively manage them, through high-quality rigorous research. Longitudinal studies may help identify the long-term impact of device usage on the musculoskeletal system. Further, studies spanning across age groups, gender, population with different anthropometrics, bodily regions, devices used, etc. may reveal additional insights. Furthermore, studies exploring the effectiveness of ergonomic interventions in managing the musculoskeletal symptoms secondary to device usage may yield valuable insights with practice implications.
The use of various electronic devices is associated with musculoskeletal symptoms in multiple regions of the body, specifically the head and neck, upper and lower back, and upper extremity in adolescents and young adults. Maladaptive postures and prolonged device use contribute to the musculoskeletal symptoms. Future research examining the effect of usage of specific devices, such as a smart phone, gaming device, etc. on bodily systems may further our understanding of the human-device interaction and yield valuable insights for stakeholders. Longitudinal studies examining the long-term impact of device usage may help validate and generalize these preliminary findings and provide additional insights.