Extremely preterm infants, < 28 week of gestational age, (ELGANs) continue to need high levels of health-care post-discharge from the NICU. We studied post-NICU hospital contacts of this highly vulnerable population and present data from infants treated in our health network.
Retrospective cohort study of ELGANs treated at the tertiary NICU of Monash Health (2010-2013) and discharged within our network's catchment area. Demographics, inpatient, and outpatient information (initial NICU and subsequent admission up to 18 months of corrected age) were collated. Comparative analyses were performed for infants who were readmitted compared to those who were not.
41 of 76 (54%) infants required hospitalization with 92 admission episodes. 81 episodes were general pediatric ward admissions while 11 were to the PICU/HDU. Viral bronchiolitis was the leading cause for admissions. Meningitis in neonatal period was more common among patients who required hospital re-admission.
Ex-ELGAN required readmission primarily due to viral bronchiolitis. In our study population, neonatal meningitis was more common in patients who required post NICU discharge hospital re-admission.
Extremely Low Gestational Age Neonate (ELGAN), Hospital readmission, Long term follow up
AIHW: Australian Institute of Health and Welfare; ANZNN: Australia New Zealand Neonatal Network; APH: Ante Partum Hemorrhage; BPD: Broncho Pulmonary Dysplasia; CGH: Casey General Hospital; CPAP: Continuous Positive Airway Pressure; DGH: Dandenong General Hospital; ED: Emergency Department; ELGANs: Extremely Low for Gestational Age Newborns; GA: General Anaesthesia; IVH: Intraventricular Hemorrhage; MMC: Monash Medical Centre; NEC: Necrotizing Enterocolitis; NICU: Neonatal Intensive Care Unit; PCR: Polymerase Chain Reaction; PETS: Paediatric Emergency Transport Services; PEG: Percutaneous Endoscopic Gastrostomy; PICU: Paediatric Intensive Care Unit; PDA: Patent Ductus Arteriosus; RSV: Respiratory Syncytial Virus; PHT: Pulmonary Hypertension; ROP: Retinopathy of Prematurity; V-P Shunt: Ventriculo-Peritoneal Shunt
Re-hospitalization after initial discharge from NICU for preterm infants has been examined in various settings across the world [1-13]. Reasons for re-hospitalizations in extreme preterm infants can be related either to medical (bronchiolitis, lower-respiratory tract infection, asthma, reflux disease) or to surgical (PEG related problems, V-P shunt related issues, hernia repair) causes. Researchers have attempted to ascertain neonatal [1,3,9,12] and socioeconomic risk factors [9,12,13] to establish at risk groups for readmission postneonatal discharge for very preterm and extremely preterm infants.
Within Australasia there are few studies highlighting subsequent outcomes of infants born preterm [1,2,9,14-18]. Some of these papers were from the pre-surfactant era where neonatal care was significantly different from current neonatal care [15-18]. Others included very pre-term infants (born before 32 weeks of gestation) and late preterm infants [2,9]. Some of them were based on weight rather than gestation age [1]. Hospital readmissions as an outcome of ELGAN is only reported in one study so far within Australasia [14].
We are presenting data from a geographically defined population in metropolitan Melbourne highlighting various aspects of re-hospitalizations including PICU admissions. Our main aim was to look for possible neonatal risk factors leading to postdischarge readmission. We aim to obtain data that will help us to counsel parents at the time of discharge from NICU.
This study was carried out in Monash Children's Hospital, Clayton (MMC), which is a part of the Monash Health network. It is a tertiary care pediatric and perinatal referral centre in the south-east of Melbourne. Monash Health has a catchment area of six local government councils caring for a population of over one million Victorians. Monash Newborn is a tertiary perinatal and surgical unit where over 1000 newborns are admitted each year. Monash Children's provides tertiary pediatric care through Monash Medical Centre, Clayton (MMC) and secondary pediatric care through Dandenong General Hospital (DGH) and Casey General Hospital (CGH) and has over 30,000 yearly pediatric in patient episodes. MMC offers a full range of general pediatric, pediatric subspecialty and pediatric surgical inpatient and outpatient services including pediatric intensive care services. DGH and CGH offer general pediatric inpatient services mainly, while pediatricians review outpatients in their private rooms.
We included all newborns born on or before 27 + 6 weeks of gestational age (Extremely low gestational age neonates) at MMC or transferred to our neonatal unit from the catchment area of Monash Health. Patients were identified using our neonatal database, which contributes prospective data to the Australia and New Zealand Neonatal Network (ANZNN) registry [19]. Patients were eligible for inclusion if they survived to discharge home and resided within our geographic catchment area. The most recent available address from either emergency department visits or outpatient visits or from inpatient admission records was used to judge eligibility of a neonate for this study.
Neonates born during the period of July 2010 to March 2013.
Retrospective cohort.
1) Neonates born out of defined geographic location and 2) Neonates with major congenital malformations, as defined by AIHW [20].
After obtaining data from unit's ANZNN database we used our health network's Scanned Medical Record (SMR) to collect clinical and demographic data. Standard ANZNN data definitions were used. Birth details such as mode of delivery, gestational age, APGAR scores, birth weight, twin or higher order pregnancy were recorded from the neonatal discharge summary. Information on neonatal course such as duration of invasive mechanical ventilation required in NICU, diagnosis of Bronchopulmonary Dysplasia (BPD), presence or absence of Patent Ductus Arteriosus (PDA) or Pulmonary Hypertension (PHT), and Intraventricular Hemorrhage (IVH) were recorded from observation charts, echocardiography reports and ultrasound reports. Discharge details such as duration of stay at MMC, mode of feeding, discharge weight and use of home oxygen were obtained from the discharge summary. Diagnosis of PDA and presence of pulmonary hypertension were based on the documented opinion of pediatric cardiologists. Presence of IVH and its grading were based on the cranial ultrasound assessment by the pediatric radiologist using the Papile classification [21]. Neonatal meningitis was diagnosed on the basis of abnormal Cerebrospinal Fluid (CSF) results and documented opinion from the pediatric infectious diseases specialists.
The health network's scanned medical record which is used across all three hospitals was used to review inpatient medical records. Data collected until corrected age of 18 months included: Number of admissions, admitting hospital, admitting team, admitting ward (Paediatric ICU, Paediatric HDU or Paediatric ward), any need for escalation of respiratory support, final diagnosis by the treating team, total days required for each admission, mortality if any and cause of death. Nasopharyngeal aspirates were sent in selected cases at the discretion of the treating physician. Viral identification is usually performed in our laboratory by PCR. We aimed to identify neonatal risk factors for re-hospitalization by comparing neonatal demographic for patients who were admitted to those who were not admitted.
Corrected age when home oxygen therapy was completely ceased was obtained from scanned medical records. Immunisation records and records regarding Palivizumab were also obtained.
For continuous data, if data was not distributed normally than outcome was presented as median and range quartile or else mean and standard deviation was used. For categorical data frequency and percentage were used. Comparisons of binary outcomes were made by using Fisher's exact test. Comparisons of continuous data among 2 groups were made by using Mann-Whitney U test. P value was considered significant if it is below 0.05. We did not conduct Bonferroni's test to address the problem of mass significance.
This study was approved by the hospital ethics committee (Ref No-14404 Q).
A total of 127 ex-ELGAN patients were discharged alive during the prescribed study period. One baby was excluded in view of his associated complex congenital heart disease requiring transfer to a cardiac surgical hospital; one baby was not discharged from NICU even at 18 months of corrected age; and one baby was transferred to another tertiary care hospital and hence further neonatal data were not available. 48 babies were discharged to geographic regions outside of our hospital's catchment area. Finally, 76 newborns who were discharged to the geographical catchment area were included for this study See the (flow chart). Their clinical profile is summarized in Table 1.
Table 1: Neonatal and demographic data for study population. View Table 1
Important features are highlighted in Table 2. 41 patients had 92 re-admission episodes which summed to a re-admission rate of 54%. Out of these 19 (44%) patients had just 1 admission, 8 patients had 2 admissions and 14 patients had 3 or more admissions within 18 months of their corrected age. The highest recorded number of admission episodes by a single patient was 6.
Table 2: In-patient admissions for study population. View Table 2
Final diagnosis as recorded by treating team has been displayed in Figure 1. Respiratory causes were the leading discharge diagnosis (71/92, 68%), with bronchiolitis the most common diagnosis. Nasopharyngeal swab or aspirates were sent in 48 episodes of admissions related to respiratory causes, hence in 23 admission episodes swabs were not considered. Picornavirus was the most frequent virus isolated (20/48, 42%) followed by Respiratory Syncytial Virus (RSV) (12/48, 25%). Parainfluenza (3/48), Adenovirus (3/48), Influenza (1/48) and Bordetella Pertussis (1/48) were the other pathogens isolated. Samples were negative in 8 out of 48 samples. 20 elective procedures were recorded during 22 elective admission episodes as illustrated in Figure 2.
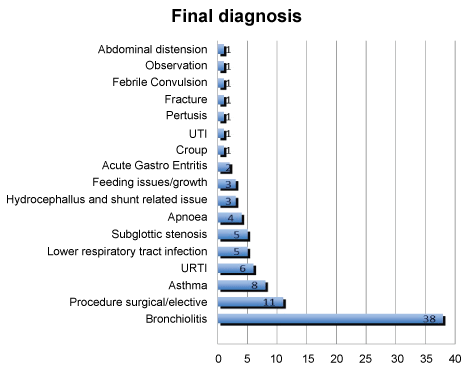 Figure 1: Final diagnosis during admission.
View Figure 1
Figure 1: Final diagnosis during admission.
View Figure 1
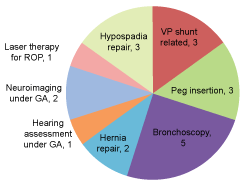 Figure 2: Various procedure performed during admissions.
View Figure 2
Figure 2: Various procedure performed during admissions.
View Figure 2
Most admissions occurred at MMC (82%) while CGH (10%) and DGH (8%) provided a minor contribution. Nearly half (47 out of 92) of the patients were admitted under the general paediatric unit, followed by paediatric respiratory unit (25/92). Paediatric surgery (3/92), pediatric gastroenterology (3/92), paediatric urology (2/92), ENT (4/92) and neonatology (4/92) were the other admitting units.
A significant proportion of our admissions were related to bronchiolitis (38/92, 41%). 25 patients had 38 admission episodes related to bronchiolitis, with 11 requiring two or more admissions. Median corrected age for admission related to bronchiolitis was 4.7 months (Range quartile 5.5). Median duration of admission for all the patients with bronchiolitis was 4 days (range 1 to 79 days, range quartile 6). Seven of these 38 required ICU admissions. RSV was isolated in 10, while Picornavirus was isolated in 13. In 14 out of 38 (37%) episodes, patients were still receiving home oxygen therapy prior to their hospital admission related to bronchiolitis. Information about the immune prophylaxis for RSV was not consistently documented.
Features of ICU admissions have been described in Table 3. Nine patients required 10 ICU admissions (11% of total admissions). Of the seven bronchiolitis admissions, 3 patients required invasive mechanical ventilation, 2 patients required CPAP and other 2 were managed with high flow.
Table 3: Features of patients requiring PICU admission. View Table 3
Two out of 10 admissions were for subglottic stenosis and both of them required high flow as respiratory support. One admission was diagnosed to have severe pertussis and was managed with nasal high flow support.
Possible risk factors and comparison of the demographic features have been displayed in Table 4. Patients treated for meningitis in the neonatal period and singleton in comparison to twins was more likely to require hospital readmissions.
Table 4: Possible risk factors for admission. View Table 4
We have got data of 34 patients out of 36 patients who were discharged with home oxygen therapy from NICU. Median corrected age when oxygen was completely ceased was 4.5 months (range quartile - 5.5). Out of 34 patients 2 patients were still on home oxygen therapy even at 18 months of corrected age. One infant required high flow oxygen support at home.
Our re-admission rate of 54% is quite similar to previously reported rates from various international settings 50% [1,3,14]. Previous Australasian data describes a readmission rate of 42% for VLBW infants [9] and 55% for very preterm infants [2].
Respiratory aetiologies as the predominant cause for hospital re-admission has been reported by many researchers [1,2,13]. Interestingly, bronchiolitis related to Picornavirus was more common in our study than RSV - a different pattern to previous reports [21,22]. RSV related bronchiolitis is an established outcome in infants born preterm. Unfortunately, we did not have reliable data on RSV immune prophylaxis, so we are unable to draw firm conclusions regarding its effect in our NICU graduate population.
In our cohort, procedure-related elective admissions were common as reported in other publications [13].
Data about ICU admission in ex-ELGANs are not well reported in the literature. Mourani, et al. concluded that small preterm infants have substantial risk of re-admission in ICU [23]. In their study 30% of total admissions resulted in PICU and two thirds of these required mechanical ventilation for an average 11.6 days. Our patient cohort had a rate of ICU admission of 11% of total admissions and among these 30% of episodes required mechanical ventilation. The predictor of ICU admission in Mourani, et al. study was male sex and intraventricular hemorrhage. We had a higher number of males in patients admitted to the ICU (77.7%), however, none of our patients requiring ICU admission had persistent abnormalities of their head ultrasounds. Four out of 10 (40%) of ICU admissions in our study were related to RSV infection. Greenough, et al. in their retrospective review concluded that RSV hospitalization in patients with chronic lung disease is associated with increased ICU admission, and longer duration of ICU stay [6].
Various studies across the world have tried to ascertain the neonatal risk factor for post NICU discharge hospital re-admission [1-3,8-13]. Ambalavanan, et al. in their recent publication using classification and regression tree analysis concluded that neonates who spent > 120 days during their NICU admission for pulmonary reasons had a 66% re-hospitalization rate compared to 42% without such stay [3]. Among studies from Australasia, Elder, et al. found diagnosis of chronic lung disease during NICU admission as a significant risk factor for hospital re-admission [9], while Gray, et al in their prospective analysis, though concluded that preterm infants required higher rate of hospital readmission, they were unable to find any specific neonatal risk factor responsible for higher re-admission rate. In our cohort we found meningitis in neonatal period was more common in patients who required hospital re-admission. This finding can be explained by the fact that meningitis in neonatal period will certainly prolong the NICU stay which is an established risk factor for subsequent post NICU discharge re-admission. However, as we had a smaller number of patients in our cohort, we would like to interpret this finding with caution. We also find that twins were less likely to require re-admission in comparison to singleton, we believe this finding is a result of smaller number of twin included in the study.
Home oxygen therapy in preterm infants is an interesting and perhaps under-reported outcome. Within Australasia, we could find 3 studies highlighting this outcome [24-26]. Complete weaning off home oxygen therapy varied between 4.5 to 6 months of corrected age in these studies. This is quite comparable with our study.
Study was conducted at a tertiary referral centre with availability of almost all pediatric specialties making data more reliable. Though our sample size was also small our findings are consistent with findings reported from elsewhere. Viral isolation for respiratory diagnosis is strength of this study. The limitations of our study were its retrospective design of chart review. Although this can be subject to bias [27]. We attempted to minimize this by structured, reproducible methodology and restricting data collection to reliably recorded outcomes. Many patients were discharged out of our health service's geographical catchment area; these excluded patients may reduce the external validity of our results. Unfortunately, socio-economic data and RSV immune prophylaxis were not consistently recorded for many patients. We did not consider the effect of mass significance in our analysis this perhaps could affect the overall result.
Hospital re-admission for infants born at extremely low gestational age is common. Respiratory conditions are the most common reason for re-admission to the ward and PICU. The majority of PICU admissions are related to respiratory conditions, particularly bronchiolitis. Neonatal meningitis was more common in patients who required re-admission following NICU discharge. We propose a case registry or a prospective study to address ongoing uncertainty relating to predictors of outcomes for ELGANs.