COVID-19, caused by the new Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2), causing a global pandemic, causes severe tissue damage and death. The leading pathophysiology of COVID-19, which affects many organs, especially the lungs, is severe acute respiratory distress syndrome (ARDS), and respiratory failure due to ARDS is the main cause of death. Mesenchymal stem/stromal cells (MSCs) show multipotent differentiation property. They are also potent immune regulators that secrete immunomodulatory factors, interacting with various immune cell types such as T cells, B cells, dendritic cells, and macrophages. Furthermore, MSC secretes a wide variety of paracrine factors that can modulate inflammation and promote tissue regeneration. Because of these properties, MSCs can repair damage to the lungs and alleviate ongoing lung inflammation, including ARDS. In this review, current clinical studies of MSC in the treatment of COVID-19 are summarized and its place in treatment is emphasized.
COVID-19, Clinical trial, Mesenchymal stem cell, Therapy
The newly identified virus, which causes a severe respiratory disease dominated by pneumonia caused a pandemic that arose from Wuhan city of China in late 2019 and spreaded to the World. The virus belongs to Coronavirus family and thus, it was initially named "2019 Novel Coronavirus" (2019-nCoV) by the World Health Organization (WHO). While the disease was named as Coronavirus disease 2019 (COVID-19) by WHO, the Coronavirus Working Group (CSG) of the International Committee on Virus Taxonomy has identified 2019-nCoV as the sister of severe acute respiratory syndrome coronaviruses (SARS-CoV), which appeared in 2002 and caused fatal respiratory illness in humans [1], based on its phylogenetic and taxonomic relationships and have published a study in which they propose to name severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) [2,3]. On February 19, 2020, a group of virologists suggested that it is different from SARS-CoV in terms of its biological, epidemiological and clinical features and that it is incorrect to call 2019-nCoV as SARS-CoV-2. Based on the clinical, virological and epidemiological features and the uncertainty of the novel coronavirus, they named the disease human coronavirus 2019 (hCoV-19) [4]. SARS-CoV-2 term is commonly used in many studies in despite of the disagreements between the different virologist groups on the nomenclature of the virus.
SARS-CoV-2, identified as a novel RNA coronavirus and belongs to the same family with SARS-CoV and Middle East respiratory syndrome coronavirus (MERS-CoV), has RNA nucleic acid which is approximately 30 kb long with a 5' cap structure and a 3'-poly-A tail and single-stranded. Homotrimers of Spike (S) proteins that form the protrusions on the surface of Coronaviruses having at least 6 open reading frames (ORF) encoding primary structural proteins including spike, membrane (M), envelope (E), and nucleocapsid (N) provide the binding of the viral proteins to the host receptors. M proteins have transmembrane domains that contribute to virus morphology and nucleocapsid binding, and the E protein is involved in virus formation and pathogenesis. On the other hand, the N protein is responsible for the viral packaging and encapsulation of the genome into virions (Figure 1) [5,6]. Besides, the activation of the entry of SARS-CoV-2 requires the proteolytic processing of the S protein with host proteases including transmembrane protease serine protease 2 (TMPRSS2), cathepsin L and furin which participate in the cleavage of the S protein. It was found that TMPRSS2, which is highly expressed in many tissues, is co-expressed with ACE2 in nasal epithelial cells, lungs and bronchial branches [7].
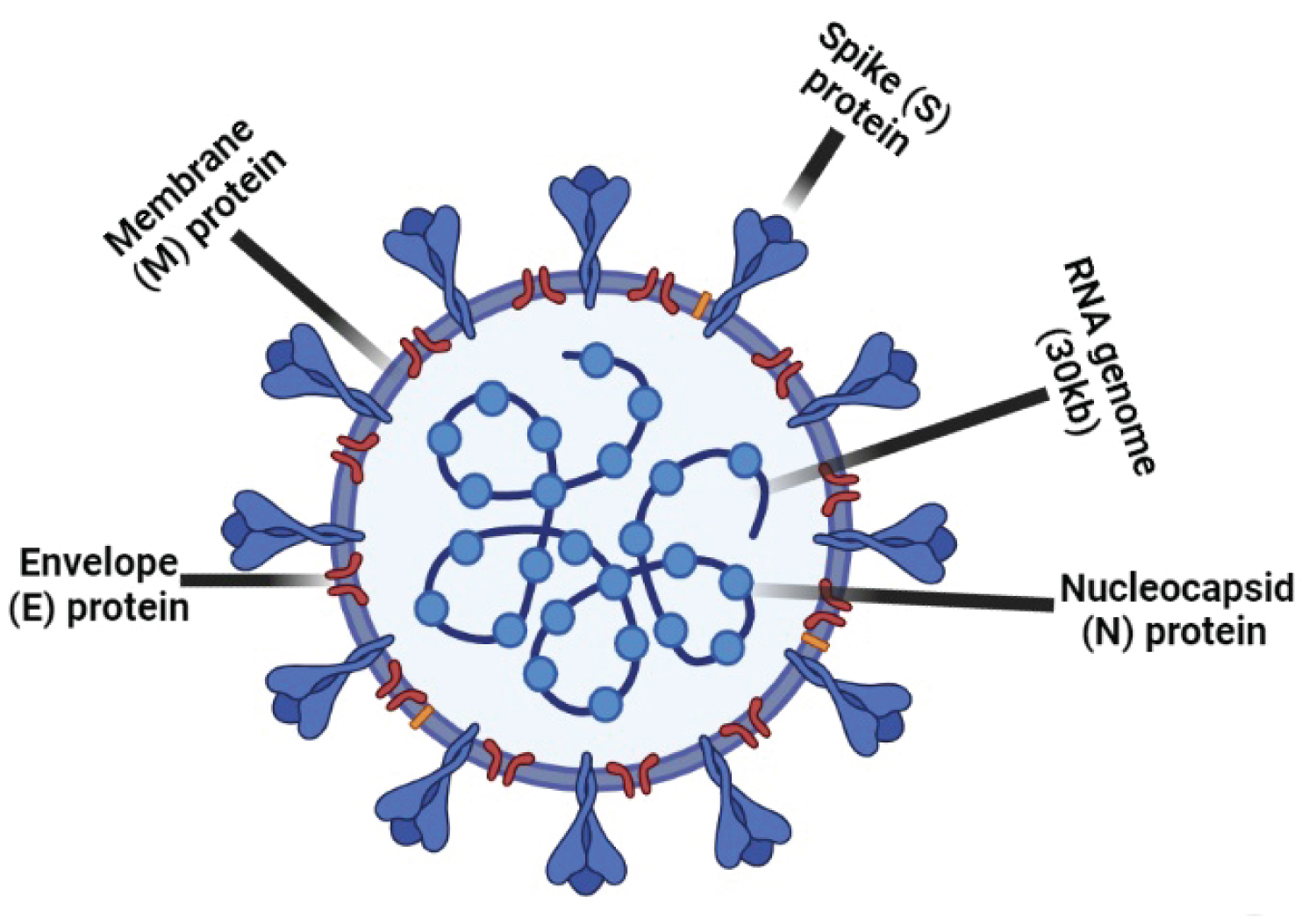 Figure 1: Structure of SARS-CoV2. The spike protein (S) provides binding to the host receptor; the envelope (E) protein together with the membrane (M) protein forms the viral envelope and determines its form; M proteins have transmembrane domains that contribute to virus form and nucleocapsid binding; the N protein is responsible for packaging and encapsulating the genome into virions.
View Figure 1
Figure 1: Structure of SARS-CoV2. The spike protein (S) provides binding to the host receptor; the envelope (E) protein together with the membrane (M) protein forms the viral envelope and determines its form; M proteins have transmembrane domains that contribute to virus form and nucleocapsid binding; the N protein is responsible for packaging and encapsulating the genome into virions.
View Figure 1
SARS-CoV-2 binds to the same receptor with SARS-CoV, angiotensin-converting enzyme 2 (ACE2) for the infection [8]. ACE2 receptor is mostly found in the endothelium of coronary arteries and vascular, smooth cells of vessels, heart myocytes and fibroblasts, intestinal cells, tracheal and bronchial cells, type 2 pneumocysts of lungs and kidney epithelial cells [8]. During COVID-19 infection, the main target of coronavirus infection is the lung. However, the wide distribution of ACE2 receptors in the organs and the affinity of the virus for ACE2 receptor cause the infection in many systems such as the heart, gastrointestinal tract organs, kidney, and liver [9].
SARS-CoV-2, which has become outbreak, can be transmitted through contaminated droplets, hands or surfaces, together with the aerosol transmission from person to person [10]. The disease affecting more than 199 countries, has caused major outbreak in the USA, Italy, central China, Spain, Germany and Iran [6]. The patients with SARS-CoV-2 infection show the symptoms ranging from mild to severe, however the majority of the population are asymptomatic. At the beginning of the disease, the most frequently reported symptoms are fever, fatigue, cough, myalgia and dyspnea [11]. However, the cases suffered from the severe organ damage have been reported as a result of severe responses of the immune system [12].
WHO has reported that in addition to fever, fatigue, dry persistent cough and shortness of breath, which are the most common symptoms of COVID-19, certain patients may experience runny nose, sore throat, nasal congestion, pain and diarrhea. It is also reported that certain patients experience loss of taste and smell [13,14]. It is now accepted that the respiratory symptoms of COVID-19 are highly heterogeneous, ranging from minimal symptoms to acute respiratory distress syndrome (ARDS) and significant hypoxia. In addition, the very short interval between the onset of symptoms and the development of ARDS suggests that the respiratory symptoms may progress rapidly [15]. Since there is no definitive treatment approach, the supportive treatment has been intensively and effectively applied in the management of the current medical treatment. To develop a definitive therapy, various drugs including lopinavir-ritonavir, remdesivir, hydroxychloroquine and azithromycin, have been tested in clinical trials [15-17], but there are no data to prove them as a definitive therapy yet. However, research and diagnostic studies accelerated with the supportive policies of the countries to develop vaccines against the disease with the publication of the genetic sequence of SARS-CoV-2 on January 11, 2020 and the clinical tests in humans began for the first COVID-19 vaccine candidate on March 16, 2020 [18]. Nowadays, several COVID-19 vaccines that developed many companies from different countries are used worldwide.
Although many countries try to prevent further spread of the virus and terminate the pandemic by implementing social distance and quarantine policies to, the vaccination that has been clinically tested and started to be implemented maintains its importance on the termination of outbreak. Despite that, the cases of re-infection and the significant rate in the presence of anti-vaccine population are the main problem for overcoming the outbreak. This situation causes the observation of severe clinical and death cases that do not respond to treatment. In addition to the combined use of supportive and antiviral drugs in treatment, immunotherapies aimed to reduce the pathological changes and tissue damage in the lungs have a great importance. Mesenchymal stem cells (MSCs) are used as an immunotherapetical option in treatment as a result of available clinical trial data (ClinicalTrials.gov) due to their immunomodulatory, anti-inflammatory and regenerative properties. In this review, we aim to focus on the present state of mesenchymal stem cell applications in the treatment of COVID-19 by providing a clinical perspective from which we will review our current knowledge about COVID-19.
Immunopathology of SARS-CoV-2 is initially developed with pneumonia which likely occurs in two phases. The process which begins with the viral replication resulting in direct virus-mediated tissue damage continues with the recruitment of effector immune cells resulting a local and systemic inflammatory response. The development of pulmonary disease with COVID-19 infection results in increased vascular permeability leading to microthrombi deposition, in addition to extrapulmonary pathogenesis including olfactory dysfunction, gastrointestinal symptoms and cardiac, hepatobiliary, and renal dysfunction. These extrapulmonary symptoms do not only occur with viral injury to the tissue cells, vessels, or neurons but also, with cytokine storm, tissue and vascular damage induced by auto-antibody [19].
In infection with SARS-CoV-2, the over-response of active immunity, which also induces tissue inflammation along with viral attack, can cause damage to the respiratory tract and lung tissues. Autopsy evaluations showed that the lesions in the lungs were caused by viruses and caused extensive alveolar epithelial damage and inflammatory cell infiltration. Alveolar lining cell necrosis causes a variety of cellular destruction. These damages result in increased alveolar-capillary membrane permeability and loss of ventilated lung tissue. In addition, some patients have fibrous accumulation in the lungs, mural fibrosis and microcystic honeycomb appearance. However, COVID-19 patients appear to be more likely to develop severe thrombotic disorders and diffuse thrombosis with microangiopathy [20].
SARS-CoV-2 infection stimulates innate and adaptive immune responses in patients, and accordingly, uncontrolled inflammatory response and abnormal adaptive immune response cause the tissue damage. The importance of the adaptive immune system components and their regulation with cytokine release lead the studies to highlight the relationship between cytokine release and COVID-19 outcome. CD4+ T cells from the adaptive immune member participate in the production of virus-specific antibodies and CD8+ T cells destroy the viral infected cells [8]. Lymphopenia is commonly observed in severely symptomatic patients. The numbers of CD4+T cells, CD8+T cells, B cells and natural killer (NK) cells are significantly reduced in these patients, and monocytes, eosinophils and basophils are also found in low level. The increases in neutrophil count and neutrophil-to-lymphocyte ratio are generally associated with higher disease severity and severe clinical outcome. As symptoms begin to improve, the numbers of CD4+ T cells, CD8+ T cells, B cells, and NK cells tend to return to normal [21]. In COVID-19 patients, an extent increase has been identified in lymphopenia, lymphocyte activation and dysfunction, granulocyte and monocyte abnormalities, as well as high cytokine levels, immunoglobulin G (IgG) and total antibodies [22,23]. The studies have reported that immunoglobulin (IgG) antibodies against S proteins which its production is stimulated by SARS-CoV-2 virus along with IgM may resulted in lung injury during the acute infection period of SARS-CoV-2 [19].
The findings reported from the studies to understand the pathophysiology of COVID-19 showed that the elevation of clinical inflammatory markers is prognostic and also provides the important information about the severity and mortality of the disease. In patients with more severe clinical course, the elevated C-reactive protein levels, lactate dehydrogenase, serum ferritin and serum IL-6 were detected. High inflammatory markers observed throughout the entire clinical course in patients with severe clinical course and subsequent death and as a result of the higher prevalence of ARDS in patients with high inflammatory markers, a proinflammatory cytokine profile emerged. According to the plasma cytokine profile of 41 patients with pneumonia, it was reported that cytokines such as IL-1β, IL-1Ra, IL-7, IL-8, IL-10 and interferon (IFN)-γ were observed in higher concentrations. According to the study data of 21 patients, very high levels of IL-1β, IL-2 receptor (R), IL-6, IL-8, IL-10 and TNF-α were detected in plasma of the patients with moderate or severe disease symptoms [15,24,25]. It has also been reported that patients with COVID-19 have high amounts of IL1B, IFNγ, IP10 and MCP1, possibly leading to activated T-helper-1 (Th1) cell responses. In addition, the higher amounts of GCSF, IP10, MCP1, MIP1A and TNF-α in patients who need to be admitted to the intensive care unit, compared to patients who do not need the intensive care unit, suggests that the cytokine storm observed in the patients is related to the severity of the disease. At the same time, 2019-nCoV infection also increases the secretion of T-helper-2 (Th2) cytokines (e.g., IL4 and IL10) that suppress inflammation in these patients [15]. The immunopathogenesis of COVID-19 is summarized in Figure 2. Figure 2 is prepared by modifying the article [23]. Briefly, from the immune system cells, stimulated inflammatory cells including monocytes, macrophages and neutrophils participate in inflammation by producing proinflammatory cytokines, and enzymes released from neutrophilic granules and thus cause the necrosis in tissue surrounding cells. During COVID-19 infection, the proinflammatory cytokines and chemokines released from inflammatory cells are associated with clinical symptoms. It was demonstrated that increased proinflammatory cytokine and chemokines in patients with severe COVID-19 may result in the suppression of CD4 + and CD8 + T cells and regulatory T cells and thus enhance the inflammatory responses and induce the cytokine storm resulting in tissue and organ damage [8].
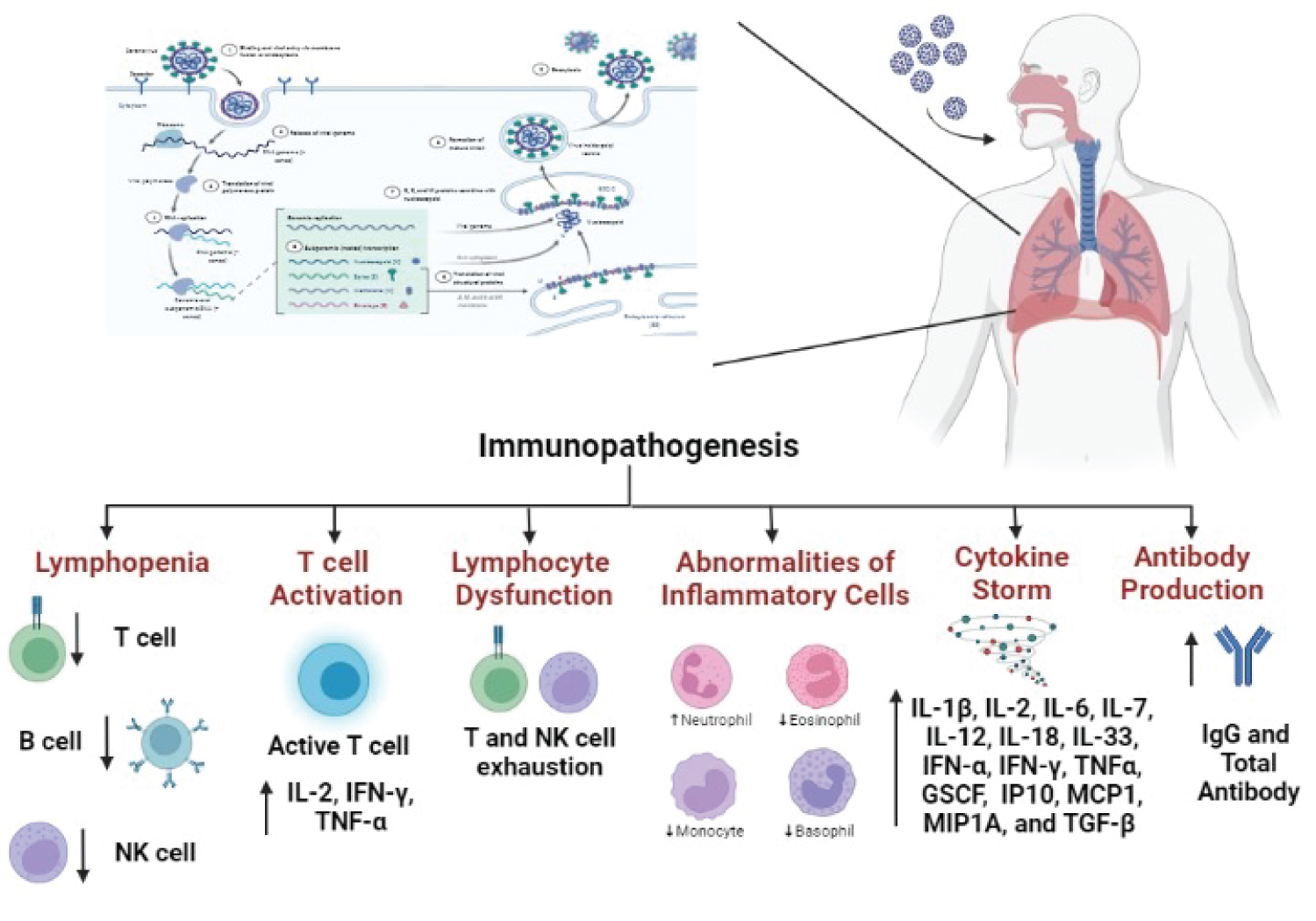 Figure 2: COVID-19 immunopathogenesis. In the pathogenesis of COVID-19, lymphopenia, T-cell activation, lymphocyte dysfunction, inflammatory cell abnormalities, increased cytokine and antibody production are observed.
View Figure 2
Figure 2: COVID-19 immunopathogenesis. In the pathogenesis of COVID-19, lymphopenia, T-cell activation, lymphocyte dysfunction, inflammatory cell abnormalities, increased cytokine and antibody production are observed.
View Figure 2
Due to the rapid spread of SARS-CoV2 infection globally, causing death in elderly persons and the persons with chronic illness, and the lack of definitive treatment approaches for the virus, different therapeutic approaches have been developed. The success in the treatment strategy is also important for reducing the size of the pandemic and preventing the disease. Accordingly, the need for a vaccine or a more specific therapeutic intervention arose in the short term [26]. The COVID-19 therapy applications consist of two groups; conventional and non-conventional therapies. It has been determined that certain antimalarial, antiviral and immunosuppressant/arthritic drugs from conventional therapy that have been used in clinical studies until recently reduce the symptoms of COVID-19. Non-conventional therapy is also based on immunotherapy. In addition to them, mesenchymal stem cells are used as a cellular therapy. Overall COVID-19 therapies are discussed in this section.
Emetine: Emetine, an alkaloid isolated from the flowering plant carapichea ipecacuanha, is also used to struggle with protozoan infections for treatment of ameobiasis. It also has anti-malarial effect by binding to the ribosomal E site of Plasmodium falciparum [27]. Emetine, which has also anti-viral activity against a wide variety of viruses including Zika virus, Ebolavirus, Cytomegalovirus, HIV-1, herpes simplex virus-2 and influenza, has recently been reported to inhibit the replication of SARS-CoV-2 at a concentration of 0.5 μM. It was also found that Emetine inhibits hCoV-OC43, hCoV-NL43, SARS-CoV, MERS-CoV, and MHV-A59 [27]. In clinical studies, it was determined that it showed inhibitory function against SARS-CoV-2 viral replication, and thus it has been used in clinic [27].
Azithromycin: Azithromycin is an antibiotic that belongs to the macrolide family and is commonly used for bacterial diseases as an anti-inflammatory drug. In addition to this, Azithromycin has an antiviral and immunomodulatory function. Azithromycin has been shown to have in vitro activity against Zika and Ebola viruses. It also reduces viremia in bronchial epithelial cells by inducing interferon type I and type III in patients with chronic obstructive pulmonary disease. Data have been obtained that the inclusion of azithromycin in combination with various treatment regimens can alter the course of viral infection and potentially affect clinical outcomes. A 100% reduction in viral load was observed in six patients treated in combination with azithromycin and hydroxychloroquine, but in another study treated with hydroxychloroquine alone, there is no effect in 57.1% of patients [28]. The main inhibitory mechanism of Azithromycin on COVID-19 treatment is related to the ability to inhibit SARS-CoV-2 binding by alteration of ACE2 glycosylation, destruction of membrane fusion, endocytosis, and lysosomal protease activation processes and also, immunomodulatory function including the reduction of the pro-inflammatory cytokines and chemokines (IL-1β, IL-6, IL-8, IL-12, IFN-γ, IP-10, TNF-α, and GM-CSF) production [29].
Chloroquine and Hydroxy-chloroquine The positive results obtained from the preliminary studies for the treatment of SARS-CoV-2 infection have brought chloroquine and hydroxy-chloroquine into the focus of attention. Chloroquine and hydroxychloroquine have been used on malaria therapy [30] and the studies showed the anti-viral function of these drugs in addition to the anti-malarial effect. Especially, certain in vitro studies have demonstrated that chloroquine and hydroxychloroquine have anti-viral activity against to Coronavirus types including SARS-CoV, MERS-CoV and SARS-CoV-2. The anti-viral mechanism of these drugs are based on the importance of the endo-lysosomal network which is required for the entry of coronavirus (CoV) into host cells. These drugs were found to block the entry of the virus to the host cells by inhibition of the acidification of endosomes and suppression of the immunomodulatory function. Their immunomodulatory activity is promoted by the production of immunosuppressive factors including IL-6 and TNFα [27]. Also, these agents can inhibit viral penetration into cells by disrupting the terminal glycosylation of the ACE2 receptor [31]. The therapeutic effects of chloroquine and hydroxychloroquine drugs on SARS-CoV-2 are shown in in vitro studies. Data are provided that chloroquine affects SARS-CoV replication in cell culture and that chloroquine is effective in preventing SARS-CoV infection in cell culture if added to cells 24 hours before infection. It has also been reported that it is significantly effective and has an antiviral effect after it is added to the culture 3-5 hours after infection [33]. However, animal studies showed the adverse effect including heart rhythm without any beneficial effect. Besides, some clinical trials demonstrated the benefit of these drugs on SARS-CoV-2 treatment with decrease in the severity of pneumonia and shortening the disease outcome without the side effects although some studies showed the opposite findings. Nevertheless, especially chloroquine is recommended to use for the COVID-19 treatment in some countries including China [31].
Favipiravir: Favipiravirin which is a pyrazinecarboxamide derivative and ribonucleotide analog, has been shown to selectively inhibit the RNA-dependent RNA polymerase (RdRP) of RNA viruses to prevent the formation of live viruses. Therefore, it causes the antiviral activity against RNA-carrying viruses. Favipiravir has been approved and used for the treatment of new influenza viruses in Japan and China and also, is found to be effective against Ebola and viral hemorrhagic fever RNA viruses [34]. The clinical studies of Favipiravir showed the fast clinical improvement [34,35], rapid viral clearance [35] and less requirement for oxygen and non-invasive mechanical ventilation [34]. Besides, this drug has been found to be ineffective at lower doses of 100 μM in clinical studies [28]. Therefore, Favipiravir is approved and used in some countries including India for COVID-19 therapy.
Remdesivir: Remdesivir was originally developed to treat Ebola infection and other associated viruses by inhibiting viral replication. The drug, an adenosine analog, is a ribonucleic acid (RNA)-dependent RNA polymerase inhibitor with broad-spectrum antiviral activity. It inhibits viral replication by competing with natural nucleosides during replication for a nucleoside analog, the RdRp active site. The drug has been extensively studied against SARS-CoV-2 in the United States and Europe, and its efficacy against severely infected patients has been evaluated as uncertain. However, emergency use of experimental Remdesivir has been approved by the US Food and Drug Administration (FDA) to treat hospitalized SARS-CoV-2 patients [32]. The drug was reported to have anti-viral activity by inhibition of SARS-CoV-2 replication, reduction of viral load. Besides, it also reduces the pathological symptoms and improves pulmonary lesions in SARS-CoV-2-infected animals [36]. The analysis performed on 12,000 patients in 500 hospital sites in over 30 countries showed that remdesivir had no statistically significant effect on the mortality rate [37] and also another study showed that there are no significant promising results in the COVID-19 patients. Furthermore, adverse drug reactions were reported with remdesivir administration in many hospitalized patients with COVID-19. These findings have caused concerns about the safety and efficacy of remdesivir in COVID-19 treatment [38].
Umifenovir (Arbidol): Arbidol (ARB), also known as Umifenovir, a small indole-derivative molecule and also, is a Russian-made drug used for some enveloped and non-enveloped viruses [39]. Arbidol has been used against influenza A and B viruses and the hepatitis C virus (HCV) more recently [40]. ARB has been reported to block viral entry into the host cells, inhibit synthesis of viral RNA, and stimulate immunemodulatory factors including serum interferon and activation of phagocytes [39]. It has also been shown that ARB has a broad-spectrum effect on viruses by acting on both cell adhesion and replication; therefore it is applied for post-exposure prophylaxis and treatment. It takes its place as one of the agents accepted as one of the effective antiviral drugs in the treatment of COVID-19 patients [40]. Meta-analysis results performed with 12 studies with 1052 patients mainly showed the relation to related to higher negative rate of PCR on day 14 in COVID-19, limited efficiancy in COVID-19, inabilit on COVID-19 patient outcomes [39].
C- D Vitamin: Vitamin C is an essential vitamin known for its antioxidant properties, which are very important for strengthening the immune system. The findings have been obtained that high doses of intravenous vitamin C may effectively prevent the cytokine storm, especially due to COVID-19. This approach is widely involved in the treatment of COVID-19 disease in China. Combination of Vitamin C with corticosteroids and thiamine is associated with a reduced risk of various progressive organ dysfunctions, including acute kidney injury, and reduced mortality in severe sepsis and septic shock patients. At the same time, its contribution to the treatment seems to be contradictory due to studies reporting that vitamin C does not provide a significant clinical benefit [41]. Vitamin D, which has been shown to have potential benefits in viral infections along with vitamin C, is one of the vitamins whose role has been investigated in the treatment of COVID-19. In a small pilot study, it was reported the low level of serum vitamin C and vitamin D in the majority of COVID-19 patients [42]. Vitamin D therapy has been identified as a potential strategy to prevent or treat COVID-19. Vitamin D therapy has also been shown to reduce other viral respiratory infections, especially in people with vitamin D deficiency [43,44]. Meta analysis on the effect of vitamin C and D supplementation showed the reduction of severity of COVID-19 with vitamin C and D supplementation [45].
Plasma obtained from people who have recovered from the illness have high level of the antibody produced against to the infectious agent. These antibodies are used as a cure for disease treatment and the vulnerable people can be immunized with this passive antibody therapy [46]. Due to the limited therapeutic alternatives for COVID-19 treatment, the clinicians and researchers focus on the administration of convalescent plasma (CP) [47]. The plasma obtained from COVID-19 patients recovering after SARS-CoV-2 infection including neutralizing antibodies against infectious agents are given externally to the patients. Therefore, it has been proven to be one of the safe, effective and reliable treatment options for viral infections. Although it is presented as an important treatment method to prevent the disease in individuals exposed to an infective agent or at risk of infection, CP treatment has several limitations. In general, CP transfusion is well tolerated by all patients and although it is associated with some side effects, its clinical consequences in severe cases of COVID-19 indicate that it can be potentially beneficial. However, it has been reported that it can cause mild fever to allergic reactions, life-threatening bronchospasm, and transfusion-related acute lung injury. Although very rare, CP administration carries the risk of transmission of various viral pathogens [48]. Another important limitations are inadequate level of neutralizing antibody obtained from some patients during convalescence and short-life of the antibodies. About 30% of patients recovering from SARS-CoV-2 show very low antibody titers and these antibodies only persist for a short period of time, such as weeks or months. Also, another major limitation of CP therapy is the requirement for large infusion volumes [48]. Clinical trials on CP administration showed that CP may be a safe therapy for COVID-19 and may be improved according to its limitations [46,49,50].
Apart from these treatment approaches, it has been reported that mesenchymal stem cells (MSCs) as cellular therapeutics also show antimicrobial effects against COVID-19 through direct or indirect mechanisms. MSCs can exert direct anti-viral effects through the secretion of antibacterial peptides and proteins (AMPs), induction of molecule activity such as indoleamine 2,3-dioxygenase (IDO), IL-17. They can show their indirect effects by regulating the host immune response against pathogens or by increasing the activity of phagocytes. Thus, unlike somatic cells that produce interferon during any virus invasion and subsequently activate hundreds of genes that resist virus infection, MSCs can continuously activate numerous anti-virus genes independent of interferon, such as the IFITM gene, which can encode protein structures that prevent viruses from invading cells [51,52].
AMPs or host defense peptides and proteins with a wide range of activities that can perform various functions such as antimicrobial and immunomodulatory effects constitute the group of endogenous molecules produced as the first immune response by multicellular organisms. These molecules exhibit selective activity against a wide variety of organisms, including bacteria, yeasts, fungi, viruses and even cancer cells. In many studies, MSCs have been reported to express four constitutive AMPs: Cathelicidin LL-37, human β-defensin-2 (hBD-2), hepcidin, and lipocalin-2 (Lcn2), which can be further modulated during infection and inflammation [52]. In the light of this information, the potential place of MSCs in the treatment of COVID-19 will be emphasized by referring to the summary of clinical studies conducted in the next sections of the article.
Mesenchymal stem cells (MSCs), also known as mesenchymal stromal cells, are multipotent stem cells that are capable of in vitro differentiation into various types of specific tissues under convenient circumstances [53,54]. MSCs, which can be obtained from a variety of tissues such as bone marrow [55], umbilical cord [56], cord blood [57], adipose tissue [58], have a capacity to differentiate into specific tissues such as hepatocytes, cardiomyocytes, neurons, or astrocytes [12,59]. The most commonly used type of MSCs for treatment of lung diseases are derived from bone marrow, adipose tissue, umbilical cord blood, and endothelial progenitor cells [12]. According to International Society for Cell Therapy, MSCs are described with three major characteristic properties; adherence capacity, maintenance of differentiation capacity throughout in vitro process, and positive expressions of certain cell surface markers such as CD73, CD90, CD105, and negative expressions of CD14, CD34, CD45 [60,61]. Moreover, it was showed that differentiation capacity and functionality of the MSCs vary depending on different properties such as tissue source, isolation and cell culture techniques [2,62].
MSCs usage can be defined as ''common'' therapeutic approach in clinical applications for various diseases. Approximately, 1330 clinical trials are available primarily in the fields such as musculoskeletal diseases, central nervous system, immune system, wounds and injuries and only 408 of them were completed (ClinicalTrials.gov). According to the recent in vivo and in vitro studies, potential risk of MSC transplantation is another important phenomenon that should not be considered lightly, despite the advantages of MSC in terms of tissue repair, their differentiation potential, extracellular vesicle (EV) release, and high paracrine capacity [63].
It was reported that MSCs ceased the progression of fibrosis, depending on their immunomodulatory functions that overcome the limitations especially in liver transplantation [64]. Additionally, MSCs have also been used in other organ transplants that associated with cancer as well as renal insufficiency, acute respiratory disease syndrome (ARDS), graft versus host disease (GvHD), and multiple sclerosis (MS) [65]. The MSCs are potentially used as a promising cellular therapy for COVID-19 patients due to their high proliferative and regenerative capability, immunomodulation ability in addition to antiapoptosis, angiogenesis, anti-scarring, and chemo-attraction functions. Immunomodulatory activity from their functions is primarily responsible mechanism for lung repair and regeneration (Figure 3) [12].
 Figure 3: MSCs can be used in different combinations in the treatment of COVID-19 and can modulate immune cells from pro-inflammatory to anti-inflammatory phenotypes, suppress cytokine storm and induce lung regeneration.
View Figure 3
Figure 3: MSCs can be used in different combinations in the treatment of COVID-19 and can modulate immune cells from pro-inflammatory to anti-inflammatory phenotypes, suppress cytokine storm and induce lung regeneration.
View Figure 3
Modulation of immune system by MSCs depends on various factors including exosomes [66]. It is known that MSCs induce therapeutic characteristics of the cells by release of bioactive molecules, named as secretomes, through a paracrine pathway. MSC secretomes are composed of soluble proteins. Exosomes involve miRNA, tRNA, non-coding RNA, lipids, growth factors and many other bioactive molecules. For an instance, existence of lipids contributes the infusion of exosomes with plasma membrane of adjacent cells [67]. besides regulation of more than 60% mRNA is conducted by miRNAs, which regulates inflammatory pathways. It has been reported that transfer of specific miRNA through MSC extracellular vesicles (EVs) has resulted in reduction of pulmonary injury [68].
Exosomes are also the agents which are able to decrease cytokine storm and reverse the inhibition of COVID-19 related host antiviral defenses. Usage of EVs that secreted by BM-MSCs for the treatment of a rat model with ARDS brought the result that EVs were effective on suppression of the inflammation [69]. MSCs are also capable of regulation of both innate and adaptive immune system by affecting immune system factors including macrophages, neutrophils, natural killer cells (NK), dendritic cells (DC), T cells and B cells [70]. It was reported that MSC implemented tissues showed anti-inflammatory effects due to the paracrine secretion. MSCs are also responsible for activation of local cells, depending on their self-renewal mechanism which promotes the regeneration on damaged tissues [71]. The combination of CD4+ and CD8+ T lymphocytes for transmission of the immune response after antigen presenting are processed was defined as adaptive immune memory [72]. MSCs are able to modulate excessive immune response by preventing proliferation of these antigen-specific T cells, and by inhibiting cytotoxicity. It has been stated that MSCs can cause not only apoptosis of T cells by secreting several mediators such as B7-H4, HLA-G, PGE2, IDO, NO and HO-1, but also via Fas/Fas ligand pathway. There exists also fail-safe mechanism which controls excessive inhibition of T cells and prevents the vulnerability against pathogenic agents [73]. MSCs also regulate the activation of B cells by a mechanism based on both cellular contact and excreted factors [74]. Particularly, the EVs synthesized by MSCs play an important role in modification of the immune cells including NK, DC, T and B lymphocytes [75]. EVs including both exosomes and microvesicles, do not generate immune response risk due to the fact that EVs provide negative expression with HLA-I and HLA-II [69].
Excessive activation of T lymphocytes and NK cells lead to raise the secretion of cytokines and chemokines called cytokine storm, which bring unbounded inflammatory responses [76]. During this process, monocytes, macrophages and neutrophils become activated, then proinflammatory cytokines are released. CD4+ T cells support the inflammatory response by differentiating into Th1 cells. Additionally, cytotoxic CD8+ T cells play an important role in the activation of Th17 cells which are able to induce excessive inflammatory responses such as IL-6 increase [77]. ARDS is defined as the leading cause of death in patients with severe COVID-19 pneumonia which is associated with IL-8, IL-1β, granulocyte macrophage colony-stimulating factor, CCL2, CCL-5, IFNγ-induced protein release [78]. Based on their regenerative potential, antimicrobial characteristic, immunomodulator and anti-inflammatory function, MSCs have a critical status for treatment of autoimmune diseases, particularly COVID-19 [79].
ARDS is resulted by the uncontrolled inflammatory response stimulated by the secretion of a large number of pro-inflammatory cytokines such as interleukin (IL)-1β, IL-2, IL-6, IL-7, IL-12, IL-18, IL-33, interferon (IFN)-α, IFN-γ, tumor necrosis factor-α (TNFα), granulocyte colony-stimulating factor (GSCF), interferon-γ inducible protein 10 (IP10), monocyte chemoattractant protein 1 (MCP1), macrophage inflammatory protein 1-α (MIP1A), and transforming growth factor-beta (TGF-β) such as chemokines during COVID-19. This extreme and uncontrolled secretion is also known as cytokine storm [80]. MSCs were reported to regulate the inhibition of cytokine storm, which is a major problem for COVID-19 patients, via intercellular interactions and excretion of biochemical factors such as growth factor beta 1 (TGF-β), prostaglandin E2 (PGE2) and HLA-G [77]. In addition to HLA-G interaction, they suppress the proliferation of T cells through expression of HLA-G that inhibits functions of T cells induced by interferon-γ (IFN-γ) [81]. Therefore, MSCs can only modulate the cytokine storm, but also they provide the immunosuppression through the inhibition of T cells by secretion of cytokines and growth factors and direct cell to cell contact effect. The stimulation IDO activity in MSC with exposure of MSCs to IFN-γ results in suppression of inflammatory response and apoptosis of pro-inflammatory T-cells [12].
PGE2 especially, changes macrophage polarization from M1 to M2, IL-10 decreases neutrophil receiving to lungs, and IDO increases pulmonary antimicrobial activity. During COVID-19, an increased ratio of T helper 17 (TH17)/Regulatory T (Treg) cells is associated with poor prognosis in ARDS patients, and it is also used as a risk indicator for determining 28-day mortality. Mouse BM-MSCs and rat lung-derived MSCs have been reported that they reduce the Th17/Treg ratio and provide a balance between the inflammatory cytokines by the regulation of the polarization of T cells into Th17 and Treg. Briefly, it was reported that MSCs can decrease Th17-related cytokines IL-17 and IL-22, and increase Treg-related IL-10 expression in both lung and plasma in addition to the inhibition of the differentiation of Th17 cells from naive CD4+ T cells via the programmed death-1 (PD-1) pathway [82].
On the other hand, MSCs inhibit the propagation and differentiation of B cells and induce IL-10 expression [69]. The fact that macrophages and monocytes are reprogrammed by human umbilical cord-derived MSCs (hUC-MSCs) via cytoplasmic organelles which are significant lung inflammatory inhibitors has been defined in certain resources [83].
Another therapeutic activity of MSCs is based on their anti-fibrotic function. Pulmonary fibrosis, which occurs with lung disease caused by viral and bacterial infections, adverse reactions of chemotherapy drugs and environmental factors, is a hallmark for ARDS. In vivo studies showed that MSC administration inhibited the fibrosis by reduction of fibroblast growth factors and ameliorate ARDS with the mechanisms that vary depending on MSC sources [82]. Application of MSC therapy is most commonly operated by intravenous (IV) infusion method. The studies showed that IV infusion enhances immune system against COVID-19. Accumulation of MSCs in lungs and correspondingly, preservation of pulmonary epithelial cells provided the formation of local regenerative cells [84]. In addition, it was indicated that intravenous MSC applications cause the induction of monocytes which are able to suppress autoimmune responses, regardless of regulatory T cell function [6]. In general, the efficacy of MSC therapy for respiratory health is related to the inhibition of inflammatory processes by transformation of M1 macrophages to M2 ones. Macrophages during prostaglandin E2 secretion increase IL-10 production which is reduced in acute lung injury. In that case, phenomenon like inhibition of T cell proliferation and activation, protease activity required by SARS-CoV-2 transmission (anti-proteolytic effect), siRNA mechanism for expression based determination occur [79]. Despite of the potential risks in clinical applications of MSCs therapy such as cellular immunogenicity, formation ectopic tissue, and in vitro transformation of the cells, studies proved that MSC therapy for autoimmune disorders provides promising and safe use as a therapeutic approach [85].
Mesenchymal stem cells can be obtained from various tissues according to clinical purposes. Certain resources have stated that umbilical cord (UC) and Wharton's Jelly (WJ) are the most effective MSC sources. UC, as a newborn tissue, contains fetus arterial blood, and WJ provides the structural support for umbilical arterials. The reason that UC-MSC and WJ-MSC are considered as postnatal tissue without function and becomes an advantage in terms of ease of accessibility and research potential. It was reported that EV enriched WJ contains excessive amount of MSC rather than other tissues [86]. EVs play an important role via regulation of cytokine storm which is an acquired outcome of clinical treatment for SARS-CoV-2 [87]. Due to noncurrent studies, MSCs are also received commonly from bone marrows (BM-MSC) [88]. The studies showed that the outcome that BM-MSCs accumulate in the injured liver, reduce proinflammatory cytokine production, alleviate liver injury, and suppress the in vitro cytotoxicity of NK cells [89]. Subdermal adipose tissue, one of the significant MSC sources, is utilized commonly based on easier isolation of stem cells by enzymatic digestion of lipids. It has been indicated that more MSCs can be obtained from adipose stem cells (ACSs) rather than BM-MSCs [90]. Additionally, amniotic membrane-derived MSCs (AMe-MSCs) and amniotic fluid-derived MSCs (AF-MSCs) are proved to be significant sources of MSCs. AF-MSCs, fetal-originated progenitor stem cells, have higher proliferation capacity than BM-MSC and also they induce vasculogenesis, angiogenesis and osteogenesis [91].
MSCs from different sources showed different proliferation capacity, differentiation potential, levels of paracrine factors and immunomodulatory properties [92]. The studies reported that injection of WJ-MSCs through intravenous infusion to 5 patients with severe COVID-19 has revealed that inflammation was restrained, supported with evaluation of cytokines and monitoring flow cytometry of CD4+ and CD8+ markers [93]. Another study revealed that patient injected with UC-MSCs showed enhanced and supported immune system compared to not injected group [94]. MSCs from different sources have comparable therapeutic effect and mechanisms during COVID-19 treatment.
Clinical and preclinical research has focused on the potential role of MSC in reducing mortality, inflammation, and lung injury in ARDS. The safety and efficacy of MSCs in ARDS has been established in numerous clinical trials. Due to ARDS's poor immunity, polytropic effects, and propensity to migrate to sites of damage, MSC therapy appears to be beneficial in ARDS. MSCs are capable of reducing C-reactive protein (CRP) levels modulate the overactivation of cytokine-secreting cells in COVID-19 patients. MSCs increase the host's resistance to sepsis and ARDS due to increased host cell phagocytosis, increased bacterial clearance and antibacterial peptide production, while reducing the host's damage from inflammation. MSCs also express several interferon-induced genes (ISGs) known to exhibit anti-viral activities. MSCs contribute to lung tissue regeneration in Acute Lung Injury (ALI) and ARDS diseases through the secretion of cytoprotective agents [77]. After intravenous injection, a portion of the MSC population is retained in the lung, and this is often known as a limitation on systemic infusion. Here, however, these MSCs can improve the pulmonary microenvironment, protect alveolar epithelial cells, arrest pulmonary fibrosis, and ameliorate lung dysfunction and COVID-19 pneumonia [6,77]. MSCs have immunomodulatory effects, regenerative properties and ability of the control oxidative damage. Therefore, they have become an exciting candidate for COVID-19-induced ARDS due to their endothelial and epithelial protection and antibacterial effects [77].
The number of patients suffering from COVID-19 is increasing day by day. In addition, the number of intensive care units required for the treatment of these patients is increased. ARDS, a highly complex disease process involving multiple organs, represents the most severe clinical state of COVID-19 infection and is the leading cause of death in intensive care units. Therefore, it is necessary to find an effective treatment for patients suffering from COVID-19 [95]. Although many countries such as the USA, China, Italy, England, France, Spain, Germany, Turkey, Iran, Brazil and Jordan have recommended the use of stem cells for COVID-19 patients, stem cell-based studies are only limited [96]. A total of 70 clinical treatments planned to use MSC for the treatment of COVID-19 have been reported on clinicaltrials.gov and chictr.org.cn (Summarized in Table 1) [69]. It has been determined that clinical studies have used allogeneically obtained MSCs at a rate of over 70%. In MSCs, it can be seen that the umbilical cord was used mostly [97].
Table 1: The clinical trials of MSCs on COVID-19. View Table 1
A primary report of a clinical trial aimed ot evaluate the safety, feasibility and tolerability of high-dose prenatal MSCs administered as three infusions as a potential treatment for critically ill COVID-19 patients with ARDS and showed that the patients with high rate of recovery had a rapid dramatic response 48-96 hours after their first MSC infusion and surviving cases were well during the 60-day follow-up evaluation. The only adverse event was transient tremor, which occurred once in two cases. It was claimed that this chill was not related with fever and was not caused by COVID-19 infection because it suddenly disappeared in less than an hour with effective care [98].
The condition of patients in a cohort of 7 COVID-19 patients treated with human MSCs was reported as well. As a result of intravenous administration of 1 × 106 MSCs per kilogram for 14 days, no side effects were observed in the patients. A rapid improvement in the respiratory functions and disease symptoms was observed [95,96,99]. In addition, the study carried out with quite low number of the patients showed the decrease in the inflammatory system activation such as cytokine-secreting immune system cells in peripheral blood, after the MSC treatment [95].
Recently, a study reported the clinical outcome of a 65-year-old COVID-19 female patient with severe pneumonia, respiratory and multi-organ failure, who was treated three times with allogeneic human umbilical cord blood-derived mesenchymal stem cells (UCB-MSCs) [69,77]. A 65-year-old female patient who had increased neutrophils, decreased lymphocyte count, and was confirmed to be positive for SARS-CoV-2 was treated with IV injection of the antiviral drugs lopinavir/ritonavir, IFN-α and moxifloxacin, methylprednisolone and immunoglobulin. However, the patient developed spastic cough, severe diarrhea and electrolyte disturbance, and was later diagnosed as critical and shifted elsewhere. The patient was taken to the intensive care unit and invasive tracheal cannula was applied to reduce respiratory distress. In addition, a noninvasive mechanical ventilator was used to combat hypoxia and respiratory muscle fatigue of the patient [96]. 5 × 107 cells/dose was administered 3 times intravenously every 3 days. After the second dose, clinical improvement was observed in the patient [69,77]. After the second dose, the patient was weaned from the ventilator and high tolerance and return of the measured parameters to normal levels were observed. Two days after the third injection, the patient was transferred from the intensive care unit and her test was confirmed to be negative for SARS-CoV-2 [77]. Within a week, the pneumonia was greatly relieved [96]. It was also reported that the inflammatory cell counts return to normal levels [69]. Further clinical studies showed the normal levels of laboratory indexes such as creatinine level, albumin, alanine aminotransferase, CRP, procalcitonin, D-dimer in addition to the better profile on the computed tomography (CT) images of lungs [96]. Although this study was reported on one case and extensive trials are needed, MSCs were reported to be useful in the treatment of COVID-19 infection [77].
In another patient whose vital activities deteriorated due to COVID-19, 1 × 105 UC-MSCs per kilogram were administered intravenously every 3 days. It has been reported that the patient's vital functions improved significantly after the first injection. Later, the patient was weaned from the ventilator while the patient's white blood cell and neutrophil and lymphocyte count returned to the normal level. Most importantly, CD3+ T cell, CD4+ T cell and CD8+ T cell numbers were significantly increased. In addition, the qualitative results obtained from CT images after the second and third UC-MSC injections showed that the pneumonia was greatly relieved, and the patient was discharged from the intensive care unit 2 days after the third injection [6].
Furthermore, from January 3, 2020 to April 4, 2020, UC-MSCs were used to treat severe COVID-19 pneumonia at Taikangtongji Hospital in Wuhan, China. 1 × 106 UC-MSCs per kilogramwere intravenously administered to SARS-CoV-2 patients. After a mean of 10 days following the first infusion of UC-MSCs, 96.8% of patients had SARS-CoV-2 negative profile. The laboratory parameters support the existence of an improvement after UC-MSC treatment [101].
In a double-blind, multi-center, randomized trial carried out in 40 ARDS patients with moderate to severe ARDS received a single intravenous dosage of 10 × 106 BM-MSCs/kg. Angiopoietin 2, a well-known mediator and biomarker of pulmonary and systemic vascular damage, was chosen to measure pulmonary function improvement, and there was a substantial connection between this biomarker and cell viability, as well as viability and improvement in oxygenation index. The researchers indicated that the MSC group's therapy was beneficial in recovering patients, with no MSC-related hemodynamic or respiratory side effects. The researchers found that a single intravenous dosage of BM-MSCs was safe in patients with moderate to severe ARDS, but that further studies were required to determine the efficiency of MSC administration [102].
Case reports of mesenchymal stem cell treatment in COVID-19 have provided the scientific evidence and set light on clinical research hypotheses. A severe COVID-19 patient with brain and multi-organ failure was recently treated with WJ-MSCs. WJ-MSCs were intravenously transplanted into the patient four times when the patient showed no improvement with conventional therapy. Relief of cytokine storm, recovery of other organ systems such as brain, recovery of respiratory function, recovery due to mesenchymal stem cell treatment were observed in the patients without any side effects [102].
Two phase 1/2 trials which used UC-MSCs (NCT04339660) and allogeneic human dental pulp MSCs (NCT04336254) were designed as randomized triple blinding. In both trials, the mesenchymal stem cell therapy is used as an incorporated therapy to the conventional treatment in a placebo-controlled method. The NCT04339660 trial is intended to demonstrate the efficacy of lung recovery using the indicators of inflammation and cytokine responses. Similarly, the NCT04336254 trial's major purpose is to identify the period to clinical improvement, and the adverse effects follow-up is mentioned in secondary outcome measures instead of primary ones [102].
The use of MSCs for the treatment of COVID-19 combined with a combinational therapy may result in a quick reduction in symptoms and rapid healing of tissues. MSCs are known to be effective in the treatment of the disease. Drug or convalescent plasma administration prior to MSC administration may result in better efficacy of MSCs. In some clinical studies, it has been observed that mesenchymal stem cell therapy can be used in the treatment of ARDS due to COVID-19 [103-105].
In an experiment related to these studies, UC-MSCs were used for the treatment with CP. which has attracted numerous attention since it was previously used to treat infectious diseases. In the preliminary study of Zhang's group, patients with severe COVID-19 were given intravenous CP infusion, and the 4 patients in the study recovered quickly, were safe and had no adverse effects. Neutralizing antibodies carried in convalescent plasma can reduce viral loads, thereby reducing inflammation and improving survival. During this experiment, two cytokine storms due to ARDS were observed andthe lymphocyte value did not return to its normal value while a decrease was observed in the neutrophil value. This situation was thought to be due to the damage caused by SARS-CoV-2 to the immune system. Convalescent plasma has been quite successful in neutralizing antibodies in ARDS. After the intravenous supplementation of three doses of UC-MSC, they showed the regulation of the immune response and inhibition the occurrence of cytokine storms, and recovery of lung tissue. These findings observed from one case might demonstrated the synergistic therapeutic effect of intravenous infusion of plasma and mesenchymal stem cells with complementary characteristics on COVID-19 pneumonia patients [103]. In another clinical study was based on the combinational treatment with UC-MSC and tocilizumab drug which is an IL-6 receptor antagonist authorized by the US Food and Drug Administration. Some drugs and cell-based therapy have been tested as alternatives to reduce symptoms of the disease, length of hospital stay, and mortality. Tocilizumab is widely used to treat cytokine release syndrome (CRS) caused by chimeric antigen receptor T-cell treatment. Pro-inflammatory IL-6 emerges as one of the critical cytokines leading to the inflammatory storm and causes increased alveolar gas exchange dysfunction. The improvements in the symptoms and CT opacities were observed after two doses of tocilizumab injection. It was concluded that after giving three doses of UC-MSC supplement, there is a significant increase in T lymphocyte values, and it was thought that this could contribute to lung repair. It has been stated that the treatment of UC-MSC with tocilizumab or a similar drug may be a promising therapeutical approach, but further studies are required [104].
Another clinical trial demonstrated the contribution of UC-MSC admisintration to the mix treatment way. In this study, MSCs were used by slow dilution in Plasma-Lyte A supplemented with human serum albumin and heparin (vehicle solution). While there were no deaths observed in the treatment group, the deaths related with ARDS were observed in the control group. It was reported that the treatment with MSCs gave faster results for improvement. As a consequence of this study, it was hypothesized that UC-MSCs might benefit severe COVID-19 patients by regulating immune responses and altering the immunopathogenic cytokine storm [105].
MSCs exert several therapeutical mechanisms for cellular therapy against COVID-19 including regulation of immune and inflammatory cells, modulation of cytokine storm, the release of exosomes with benefits and regulation of pulmonary fibrosis. Although the number of clinical studies showing the efficiency and safety is limited, preclinical and clinical studies showed that these functions of MSCs provide the improvement in SARS-CoV-2 patients and reduction of the disease symptoms, especially with ARDS. However, further clinical studies which will support the efficacy and safety of MSC applications are required in Covid-19 patients.
The authors report no conflicts of interest.
The authors contributed equally to the preparation of the manuscript.