International Archives of Urology and Complications
Female Pelvic Organ Prolapse (POP) Surgery. Results at 24-Month Follow-Up
Rosita Aniuliene1*, Povilas Aniulis2, Lina Slabsyte3 and Titas Telksnys2
1Department of Obstetrics & Gynecology, Lithuanian University of Health Sciences (LUHS), Lithuania
2Deptartment of Urology, Lithuanian University of Health Sciences (LUHS) Hospital, Lithuania
3Department of Internal Medicine, Lithuanian University of Health Sciences (LUHS) Hospital, Lithuania
*Corresponding author: Rosita Aniuliene, Department of Obstetrics & Gynecology, LUHS University Hospital, EIVENIU 2, Kaunas, LT-50009, Lithuania, Tel. +37068778631, E-mail: rosita.aniuliene@kaunoklinikos.lt
Int Arch Urol Complic, IAUC-1-007, (Volume 1, Issue 2), Research Article; ISSN: 2469-5742
Received: May 03, 2015 | Accepted: July 06, 2015 | Published: July 09, 2015
Citation: Aniuliene R, Aniulis P, Slabsyte L, Telksnys T (2015) Female Pelvic Organ Prolapse (POP) Surgery. Results at 24-Month Follow-Up. Int Arch Urol Complic 1:007. 10.23937/2469-5742/1510007
Copyright: © 2015 Aniuliene R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: PROLIFT (anterior, posterior, total) is a type of the surgical procedure during which synthetic implants are used. PROLIFT procedure involves the use of porous, non-absorbable polypropylene mesh and fixation of the uterine fascia and its ligaments. The aim of this study: to evaluate the efficacy, outcomes and complications of the PROLIFT procedure and evaluate the changes in the patients sexual function (before and after surgery).
Material and methods: A prospective study based on observation of clinical outcomes of the PROLIFT procedure performed by one surgeon during the period of 4 years (01/05/2008 -01/05/2012). Patients were observed and examined after 3, 6, 12 and 24 months. Our studied women responded to the FSFI questionnaire and special 4 questions before and after surgery about quality of their sexual life.
Results: Analysis of 51 PROLIFT procedures was performed. Mean age of women - 52.19 years. All women reported having active sexual life. 70.6% of women were menopausal. The mean number of births - 2.21. The following factors for POP were distinguished: birth weight over 4kg in 37 cases (72.5%), BMI above 30kg/m2 (37.3%) in 19 women, and manual work was reported by 8 women (15.7%). Three types of the PROLIFT procedures were carried out: anterior - for 45 women (88.2%), posterior - 5 women (9.8%) and total - 1 woman (2%). PROLIFT procedure was combined with colpoperineoplasty in 45 cases (88.2%), with amputation of the uterine cervix in 5 cases (9.8%), and in 1 case (2%) with TVT operation. Spinal anesthesia was administered in 43 cases (84.3%), general anesthesia - in 6 cases, (11.8%) and in 2 cases (3.9%) - intravenous anesthesia. Mean PROLIFT procedure time - 43.2 minutes. Mean hospital stay - 2.7 days. Mean amount of blood loss during procedure - 131ml. Efficacy of the procedure was evaluated after 24 months and showed a 98.0% success rate. There was 1 case of recurrence (2%), thus the procedure was repeated.
Conclusions: PROLIFT procedure as minimally invasive surgical treatment for POP is shown to be effective in 98.0 % of cases after 24 months. With aging and pelvic organ prolapse stage, a number of early complications increases. Women have significantly better sexual life after PROLIFT procedure.
Keywords
Pelvic organ prolapse (POP), PROLIFT operation, Cystocele, Rectocele, Enterocele
Introduction
Women pelvic organ prolapse (POP) is a common pathology in urogynaecology. Given the fact that women's lifespan is increasing and society is aging, this disorder is becoming more relevant, moreover, it is embarrassing for the women involved.
Literature points out that pelvic organ prolapse is common in middle age women and occurs in 50% of parous women [1-3], however, not all women require surgical intervention. Approximately, from 11 to 20% of all women may have the risk of surgical treatment for POP [3-6]. There is no data and register on prevalence of pelvic organ prolapse in Lithuania.
POP has been classified depending on which presumed organ protrudes into vaginal opening or vagina. When the bladder protrudes it is called vesicocele or cystocele, when the bladder/urethra- vesico/cystourethrocele, when the uterus - uterine prolapse, when the intestines protrude in the presence of hysterectomy - enterocele, when part of the rectum - rectocele [7].
Since 1996 The International Continence Society has defined the system of Pelvic Organ Prolapse Quantification (POP-Q). This system has become predominant, though some European countries use Baden-Walker classification [8,9].
Pelvic organ prolapse may result from injuries of the levator ani, vaginal wall, disorders of smooth muscle functions and changes of the connective tissue [10]. The risk factors for these pathologies are as follows: vaginal childbirth, age, menopause, a reduced level of estrogens, chronically increased intra-abdominal pressure, chronic obstructive pulmonary disease, constipation, obesity, pelvic floor trauma, genetic factors, race, injuries of the connective tissue, hysterectomy, spinal hernia [3,11,12].
Pelvic organ prolapse is characterized by different symptoms involving anatomical or functional systems. The symptoms of this condition are as follows: felt or seen protrusion into the wall of the vagina or perineum, pressure or feeling of heaviness in the pelvis or vagina. The symptoms of urinary disorders - incontinence, the symptoms of overactive bladder, the feeling that the bladder is not completely empty, change in position or a need to digitally reduce vaginal bulge to initiate or complete urination. Bowel symptoms are the following: incontinence of gas, fluids or watery stools, incomplete emptying, difficulty in opening the bowels or urge to have bowel movements. The symptoms of sexual function include dyspareunia, reduced lubrication, lack of sensation with intercourse, lack of friction. Pain felt in the vagina, the bladder, the rectum, pelvic area and lower back- loin [13].
Women who are asymptomatic with POP or have minimal symptoms do not require treatment. Women having stages III - IV POP or severe symptoms need surgical or conservative treatment. Conservative treatment comprises pessary use [14] and strengthening pelvic muscles by Kegel exercises [15,16]. Various surgical techniques are used for POP management: classical colpoperineoplasty, vaginal hysterectomy, colpopexy, promontorium fixation [3,17,18]. However, clinical outcomes of surgery are not always satisfactory, and study data show that up to 30% of women need repeated surgical intervention over the 5 years following the previous operation [3,19,20]. Recurrence of pelvic organ prolapse and a number of repeated surgeries declined since original minimally invasive procedures - synthetic prolene meshes - have been introduced. The efficacy of this surgical procedure corresponds the outcomes of laparotomy, laparoscopic colpopexy and promontorium fixation, i.e. the Level 1A recommendation, when POP is treated surgically [17,21].
PROLIFT (anterior, posterior, total) is a type of the surgical procedure during which synthetic implants are used. PROLIFT procedure involves the use of porous, non-absorbable polypropylene mesh and fixation of the uterine fascia and its ligaments. According to studies, the efficacy of Prolift surgical procedure ranges from 87% to 97% [22-29]. Complications of PROLIFT procedure may be early occurring perioperatively, and late postoperative complications, which further is classified into early postoperative and late postoperative. Most common perioperative complications are injury of the bladder, which occurs from 0.9% to 2.6% [22,26,28-32]. The other perioperative complication is damage of the main surrounding nerves and blood vessels [33]. Early postoperative complications may include pyrexia, urinary infection, urinary retention, abscess, large hematoma. Late postoperative complications comprise mesh protrusion, recurrence, granuloma, the shrinking of the mesh, vaginal erosion, adhesions, chronic pain of pelvis and buttocks, sexual dysfunction [22,29-31]. The rate of recurrence of pelvic organ prolapse ranges from 4.7% to 10 % of all operated women [22,31,32].
The aim of this study is to evaluate the efficacy, outcomes, and complications of PROLIFT surgical treatment and estimate it impact on the patient's sexual function.
Material and Methods
It is a prospective study based on observation of clinical outcomes of PROLIFT procedure performed by one surgeon during the period of 4 years (01/05/2008 -01/05/2012) in tertiary level hospital, department of Gynecology. Patients were observed and examined after 3, 6, 12 and 24 months. The surgical technique was followed product guidance.
The number of patients to be studied was established using PASS (Power Analysis and Sample Size programme). The statistical power of the research was found to be 0.8.
The stage of the prolapse was assessed in the lithotomic position while the patient performed a Valsalva maneuver. During physical examination, the prolapse was classified using the Baden and Walker classification. According to this classification, stage I was defined when the leading edge descends to the first third of the vagina, stage 2 to the mid vagina, stage 3 at the hymen level and stage 4 outside the hymen.
A concomitant procedure was performed if necessary, including posterior vaginal repair with perineorraphy or TVT as SUI procedure, or amputation of uterine cervix.
Inclusion criteria: stage III and stage IV prolapse, a patient has sexual intercourse on regular basis and agree to buy single use GYNECARE PROLIFT® kit by themselves (there is no compensation from the patient fund) and signed informed consent form confirming their willingness to participate in the study.
Exclusion criteria: clinical depression or other major psychiatric disease, patients who filled questionnaire incompletely.
Prior and after procedure, patients were asked Female Sexual Function Index (FSFI) and non-validated special author's questions about quality of their sexual life.
1. How does POP affect your life?
2. How often per month do you have sexual intercourse?
3. Do you always experience orgasm? (If not always - please state how often in per cent).
After surgery, the following questions were asked:
1. Are you satisfied with the results?
2. If not, tell the reasons.
3. How often per month do you have sexual intercourse?
4. Do you always experience orgasm? (If not -state how often in per cent).
The FSFI is a 19-item survey that assesses six domains of female sexual dysfunction (FSD) developed by Rosen in 2000. Scores range of the FSFI from 2 to 36.0; a total score of 26.55 or less is suggestive of FSD and individual domain scores of less than 3.6 are considered dysfunction. This questionnaire assesses: arousal, desire, orgasmic disorder and sexual dysfunction associated with pain over the preceding month of a patient's life.
After surgery, history and physical examination with speculum exam and vaginal palpation were repeated at 3, 6, 12, 24 months for all patients.
Recurrent prolapse was defined as any descent of stage 3 or 4 (cystocele, vault or uterine prolapse, enterocele or rectocele) even if the patient had no symptoms. Failure was defined as recurrent prolapse or any symptomatic prolapse.
Statistical analysis was performed using SPSS 19.00 for Windows. Calculation was performed with the use of Student's test and chi-square test, Pearson's correlation coefficient and p<0.05 was considered as statistically significant.
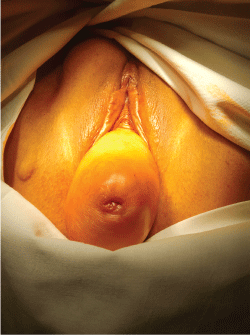
The study was approved by the Ethic Committee of the Lithuanian University of Health Sciences. Permission number: BEC-MF-306. Informed consent from the patient J.M. was obtained for agreement to publish the photo pictures Number 5 and 6 of this manuscript.
No financial assistance was received from any company for the execution of this study.
Results
Analysis of 51 PROLIFT surgical procedures was performed over the investigated period. All the patients had a prolapse with at least a stage 3 or 4 component.
Mean age of women undergoing the procedure - 52.19 years, the youngest woman was 30 years old, and the oldest - 68. All women are married and reported having active sexual life. Of our studied women, 36 (70.6%) were menopausal. Mean number of births - 2.21 (range from 1 to 4). Three women gave birth to twins (5.9%) (Table 1).
![]()
Table 1: Data of patients and PROLIFT procedure
View Table 1
The following risk factors for pelvic organ prolapse were analysed: birth weight over 4kg in 37 cases (72.5%), BMI above 30kg/m2 (37.3%) in 19 women, and manual work was reported by 8 women (15.7%). Out of 51 women, 2 had bronchial asthma (3.9%) that could predispose POP, since bronchial asthma is a disease, which increases intra-abdominal pressure.
Distribution of surgeries recorded in anamnesis was : laparoscopically assisted vaginal hysterectomy (LAVH) - 1 case (2%), TVT - 1 case (2%), subtotal hysterectomy-2 cases (3.9%), Dollar-Gilliam operation - 1 case (2%), colpoperineoplasty- 1 case (2%), vaginal hysterectomy - 3 cases (5.9%), Manchester operation - 2 cases (3.9%),Mayo hysterectomy - 1 case (2%).
Pelvic organ prolapse stage III was in 37 cases (72.5%) and stage IV - in 14 cases (27.5%). Three types of PROLIFT procedure were carried out: anterior - for 45 women (88.2%), posterior - 5 women (9.8%) and total - for 1 woman (2%).
In all cases PROLIFT procedure was combined with other surgical treatment: with vaginal repair and perineorraphy in 45 cases (88.2%), with amputation of the uterine cervix in 5 cases (9.8%), and with TVT in 1 case (2%).
Most commonly, spinal anesthesia was administered in 43 cases (84.3%), general anesthesia - in 6 cases, (11.8%) and in 2 cases (3.9%) - intravenous anesthesia.
Mean PROLIFT procedure time- 43.2 minutes. Mean hospital stay - 2.7 days. Mean amount of blood loss - 131ml. Efficacy of the procedure was evaluated after 24 months and showed a 98.0% success rate. There were 1 case of recurrence (2%), thus the procedure was repeated.
Two early complications were distinguished. Hemorrhage was evaluated when amount of blood lost was above 500 ml in 2 cases (3.9%) and pyrexia - in 3 cases (5.9%).
Late post-operative complications were also evaluated and were as follows: vulvar hematoma in 1 case (2%), parametrial hematoma - in 1 case (2%), retention of urine - in 2 cases (3.9%), prolene protrusion - in 4 cases (7.8%), dyspareunia - in 2 cases (2%) and pelvialgia occurred in 2 cases (2%). There are no severe cases when eroding a large area of mesh, it just a single suture seen in all prolene protrusion cases.
Statistically significant direct relationship between age and early complications was determined (r=0.974, p<0.05), and similar relationship between POP stage and early complications was found (r=0.964, p<0.05) suggesting that a number of early complications increased with age and pelvic organ prolapse stage. There are no statistically significant relationship between age, POP stage and late complications.
Analysis of type of early complications and POP stage did not reveal statistically significant difference (χ2=3.771; lls=5; p=0.583).
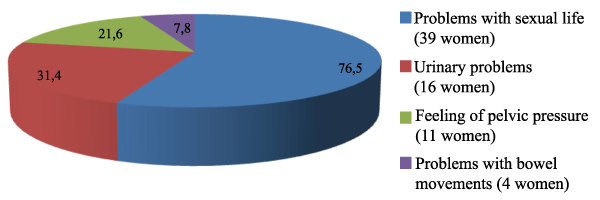
Our studied women responded to the FSFI questionnaire and 4 special questions before and after procedure. The aim of questionnaire presented before surgery was to find out the reasons of choosing surgical treatment and symptoms of complaints. Of 51 women, 39 (76.5%) responded that POP interfered with sexual life, 16 (31.4%) reported urinary problems, 11 women (21.6%) had a feeling of pelvic pressure, and 4 women (7.8%) indicated problems with bowel movements (Figure 1). Evaluation of sexual activity before surgery was based on the number of intercourse per month and number of experienced orgasm during intercourse.
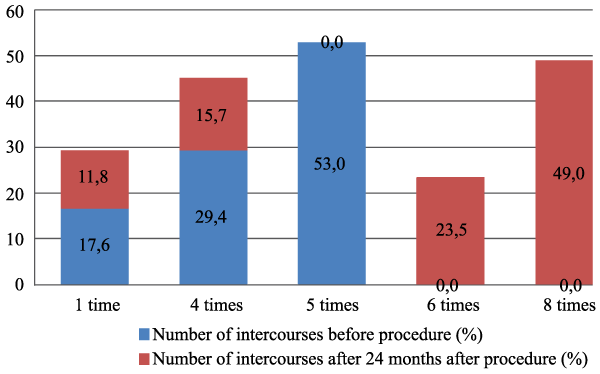
After surgery, 43 women (84.3%) reported being satisfied with the results of operation and 8 women (15.7%) responded that they were not satisfied. Of 8 unsatisfied women, four pointed out that they felt protrusion of the mesh, two - experienced chronic pain of lower abdomen, and two women reported having dyspareunia. In order to evaluate the impact of the PROLIFT procedure on women's sexual activity, the women were asked to answer to the same questions after 24 months following surgery. A comparison of women sexual activity before and after surgery is presented in figure 2 and 3. FSFI scores before and after procedures are shown in table 2.
.
Figure 2:P=0.000
Comparison of number of intercourses per month before and after procedure
View Figure 2
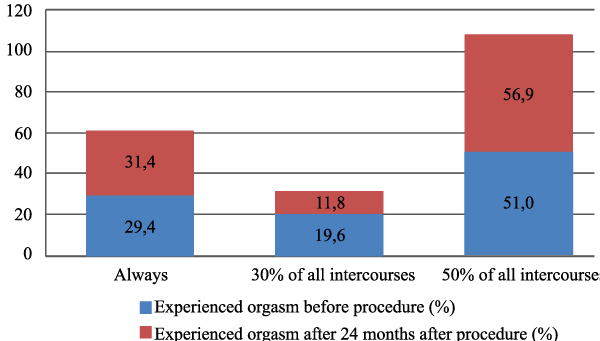
.
Figure 3: P=0.384
Number of orgasms felt during intercourse before and after procedure
View Figure 3
![]()
Table 2: Pre- and Postoperative FSFI Scores.
View Table 2
Statistically significant difference between a number of intercourse per month before and after surgery was determined (χ2=76.185; lls=6; p=0.000). It showed that women after PROLIFT procedure had a more active sexual life, and a higher number of intercourses per month compared with their sexual life before procedure. Frequency of orgasm was not influenced by surgical treatment (p=0.384).
Discussion
According to literature, the main possible risk factors for pelvic organ prolapse are vaginal childbirth, number of childbirths, age, increased intra-abdominal pressure, obesity [3,11,12]. This study revealed that 37 women (72.5%) delivered newborns with birth weight over 4kg. BMI over 30kg/m2 was determined in 19 women (37.3%). Difficult manual work was reported by 8 women (15.7%), 2 women (3.9%) had bronchial asthma that could predispose POP, since this disease increases intra-abdominal pressure. Age is also a risk factor contributing to this pathology. Studies have revealed a relationship between age and pelvic organ prolapse: with aging the risk factor for POP is increasing [11]. Mean age of our studied women was 52.19 years. According to other authors, mean age of women studied was higher. Withagen M et al. [23] in their prospective cohort study presented mean age of 66 years [34]. In the other prospective multicenter study Murphy M et al. [24] investigated women whose mean age was 65 years [24].
According to literature, women usually present with the main complaints such as felt protrusion, dysfunction of urination, bowel movements and sexual function, pain [13]. Our study showed that 39 women (76.5%) responded that POP interfered with sexual life, 16 women (31.4%) reported difficulty urinating, 11 women (21.6%) felt tension in the lower abdomen and 4 women (7.8%) indicated that POP caused problems with bowel movements. According to the study carried out by Roberts CH et al. [27] in London, 100% of patients experienced the symptoms of protrusion, urinary problems were reported by 75% of patients, and dysfunction of bowel movements - by 17.5% of studied [27]. It is worth to mention that POP causes great discomfort for women.
Scientific literature worldwide presents a large number of studies that report a reduced PROLIFT procedure time. According to our study, mean time of the procedure was 43.2 minutes. The data obtained were compared to data from other authors, similarity with Flame et al. [35] was observed; according to their study, the procedure time was 38 min. However, it is twice shorter if compared with the study performed by Fatton B et al. [31] in France, and compared with Van Raalte et al. [1] data - 89.8 min and 102.8 min, respectively [22,31,35].
Short hospital stay is characteristic of PROLIFT surgical procedure. There are studies that reported mean postoperative hospital stay, which did not exceed 24 hours. For instance, the study carried out by Folke Flam in Sweden determined that most patients (64%) participating in the study were released on the same day after surgery, and hospital stay lasting up to 24 hours was observed only in 36% of patients [35]. Mean hospital stay in our study was 2.7 days compared with Fatton B et al. [31] results presenting 3.6 days and Withagen M et al. [34] hospital stay - 4 days [31,34].
Local anesthesia, less commonly spinal and general, was used in many studies during PROLIFT procedure. In the study carried out by Folke Flam in Sweden, in 100% of cases local anesthesia was administered [35]. In the other multicenter prospective study by Altman et al. spinal anesthesia was used in 65.32% of cases [30]. In our study, more commonly, spinal anesthesia was administered (84.3%).
In literature complications are commonly classified into early and post-operative complications. According to our study, early complications were amount of blood lost above 500ml in 3.9% of cases and pyrexia - in 5.9% of cases. Other authors present a low mean amount of blood lost during PROLIFT procedure, and higher level of lost blood has not been reported. In our study mean amount of blood lost during surgery was 131ml. A comparison of results in our study and in the study carried out by Roberts et al. [27] in London revealed a similar amount of lost blood, 143ml. Other studies have shown even lower amount of blood lost; Withagen M et al. [23] report a loss of 100ml of blood and more than 500ml of blood lost in only 1.7% of studied [23,27].
In our study late complications were as follows: vulvar hematoma in 1 case (2%), parametrial hematoma - in 1 case (2%), retention of urine - in 2 cases (3.9%), prolene protrusion - in 4 cases (7.8%), dyspareunia - in 2cases (3.9%) and pelvialgia occurred in 2 cases (3.9%). A comparison of clinical outcomes of post-operative complications in our study and the results obtained by multicenter retrospective study carried out by Fatton B et al. [31] in France . They determined that dyspareunia occurred in 4.1% and prolene protrusion in 4.7% of cases, and retention of urine occurred more frequently, in 11.8% of patients, compared with 3.9% of women in our study [31]. According to Jakimuk et al. [36] data, retention of urine occurred in 2.5% of patients, however, pelvialgia, which in scientific sources is reported rarely, affected 2.5% of women [36].
Some differences in the outcomes and complications rate between our results and the other published studies might be related to some limitations in our study. All operations were performed by one surgeon, so, experience increased during the long inclusion into the study period.
Evaluation of women's sexual life before and after surgery in our study determined statistically significant difference between data of number of intercourse per month before and after surgery. When comparing the data with Withagen M et al. [34] study, the participants had to answer the question how often they had intercourse; before surgery 39% of respondents reported not having intercourse, and after surgery - 30%. Dyspareunia before and after surgery was pointed out by 55% of women, and severe dyspareunia was reported by 10% of women before surgery and 2% - after surgery [37]. According to our data, dyspareunia after surgery was pointed out by 3,9% of women. The results of the FSFI indicated that satisfaction was improved (Table 2). In sexually active women preserving sexual capacity of the vagina is an important aspect of surgery. In our study group, results from the FSFI questionnaire received before surgery showed clinically significant sexual dysfunction, which indicated that pelvic organ prolapse is negative impact in their sexual function. Statistical analysis of the FSFI questionnaire revealed statistically significant changes in arousal and satisfaction domains and in the full score before and after surgery. Other domains slightly improved, but didn't reach statistically significant difference.
Our study showed that the PROLIFT was effective in 98.0% of cases, and due to recurrence, repeated surgery was needed in 2% of the studied (Figure 4,5). A comparison of our data and other studies also revealed a low rate of recurrence. Van Raalte et al. [22] in the USA report 9.43% of recurrences [22]. Neuman M et al. [28] present a 0.7% rate of unsuccessful procedures [28]. Evaluation of women's reports after surgery in our study revealed that a positive effect was pointed out by 43 women (84.3%) and 8 women (15.7%) reported being not satisfied. Seeger D et al. [38] in prospective study in Germany reported that 89.2% of patients did not experience POP symptoms [38].
Currently, to treat POP, less traumatic surgeries such as abdominal, laparoscopic sacrocolpopexy and using fixation to promontorium are performed. Other authors have shown that the efficacy of sacrocolpopexy ranges from 83% to 100% [39-43]. According to other data, the efficacy of using fixation to promontorium is from 88.5% to 92.4% [44-46]. These data are very similar to the outcomes of effectiveness determined in our study, therefore, we may state that efficacy of PROLIFT procedure corresponds to the results obtained after laparotomy, laparoscopic colpopexy and using fixation to promontorium suggesting that PROLIFT is level 1A recommendation in POP treatment.
Conclusions
PROLIFT procedure as minimally invasive surgical treatment for POP is shown to be effective in 98.0 % of cases after 24 months. With aging and pelvic organ prolapse stage, a number of early complications increases. Women have more active sexual life after PROLIFT procedure.
Acknowledgements
We wish to thank prof. Michael Halaska, the head of the Department of Gynecology of Prague Bulovka university hospital and Lithuanian Society of Urogynecology for the general support and reasonable advises.
References
-
Beck RP, McCormick S, Nordstrom L (1991) A 25-year experience with 519 anterior colporrhaphy procedures. Obstet Gynecol 78: 1011-1018.
-
Digesu GA, Chaliha C, Salvatore S, Hutchings A, Khullar V (2005) The relationship of vaginal prolapse severity to symptoms and quality of life. BJOG 112: 971-976.
-
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89: 501-506.
-
Smith FJ, Holman CD, Moorin RE, Tsokos N (2010) Lifetime risk of undergoing surgery for pelvic organ prolapse. Obstet Gynecol 116: 1096-1100.
-
de Boer TA, Slieker-Ten Hove MC, Burger CW, Kluivers KB, Vierhout ME (2011) The prevalence and factors associated with previous surgery for pelvic organ prolapse and/or urinary incontinence in a cross-sectional study in The Netherlands. Eur J Obstet Gynecol Reprod Biol 158: 343-349.
-
Fialkow MF, Newton KM, Lentz GM, Weiss NS (2008) Lifetime risk of surgical management for pelvic organ prolapse or urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 19: 437-440.
-
Committee on Practice Bulletins-Gynecology, American College of Obstetricians and Gynecologists1 (2007) ACOG Practice Bulletin No. 79: Pelvic organ prolapse. Obstet Gynecol 109: 461-473.
-
Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, et al. (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175: 10-17.
-
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, et al. (2002) The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-Committee of the International Continence Society. Neurol Urodyn 21: 167-178.
-
Kim S, Harvey MA, Johnston S (2005) A review of the epidemiology and pathophysiology of pelvic floor dysfunction: do racial differences matter? J Obstet Gynaecol Can 27: 251-259.
-
Swift S, Woodman P, O'Boyle A, Kahn M, Valley M, et al. (2005) Pelvic Organ Support Study (POSST): the distribution, clinical definition, and epidemiologic condition of pelvic organ support defects. Am J Obstet Gynecol 192: 795-806.
-
(2000) Risk factors for genital prolapse in non-hysterectomized women around menopause. Results from a large cross-sectional study in menopausal clinics in Italy. Progetto Menopausa Italia Study Group. Eur J Obstet Gynecol Reprod Biol 93: 135-140.
-
Barber MD (2005) Symptoms and outcome measures of pelvic organ prolapse. Clin Obstet Gynecol 48: 648-661.
-
Cundiff GW, Weidner AC, Visco AG, Bump RC, Addison WA (2000) A survey of pessary use by members of the American urogynecologic society. Obstet Gynecol 95: 931-935.
-
Bo K (2004) Pelvic floor muscle training is effective in treatment of female stress urinary incontinence, but how does it work? Int Urogynecol J Pelvic Floor Dysfunct 15: 76-84.
-
Thakar R, Stanton S (2002) Management of genital prolapse. BMJ 324: 1258-1262.
-
Maher C, Baessler K, Glazener CM, Adams EJ, Hagen S (2008) Surgical management of pelvic organ prolapse in women: a short version Cochrane review. Neurourol Urodyn 27: 3-12.
-
Gomelsky A, Penson DF, Dmochowski RR (2011) Pelvic organ prolapse (POP) surgery: the evidence for the repairs. BJU Int 107: 1704-1719.
-
Clark AL, Gregory T, Smith VJ, Edwards R (2003) Epidemiologic evaluation of reoperation for surgically treated pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol 189: 1261-1267.
-
Lawrence JM, Lukacz ES, Nager CW, Hsu JW, Luber KM (2008) Prevalence and co-occurrence of pelvic floor disorders in community-dwelling women. Obstet Gynecol 111: 678-685.
-
Jia X, Glazener C, Mowatt G, MacLennan G, Bain C, et al. (2008) Efficacy and safety of using mesh or grafts in surgery for anterior and/or posterior vaginal wall prolapse: systematic review and meta-analysis. BJOG 115: 1350-1361.
-
Van Raalte, Lucente, Murphy, Haff, McCardell (2007) Short-Term Results of the Prolift Procedure in 350 Patients Used in the Treatment of Pelvic Organ Prolapse. Int Urogynecol J 18: 49.
-
Withagen M, Milani F, Kluivers K, van den Akker S, Vierhout M (2007) Objective and Subjective Results on Tension Free Vaginal Mesh Procedure (Prolift®) for Pelvic Organ Prolapse. Post at the 37th Annual Meeting of the International Continence Society.
-
Murphy M, Raders JL, Haff R, Yeager M, Lucente VR (2006) Early U.S. Experience With Vaginal Extraperitoneal Colpopexy Using a Polypropylene Graft (Prolift(TM)) for the Treatment of Pelvic Organ Prolapse. Journal of Pelvic Medicine and Surgery 12: 104-105.
-
Paplomata E, Balaxis D, Pantelis T, Karagonis S, Madenis N, et al. (2007) Genital Floor Repair using Polypropylene Meshes: A Comparitive Study. Poster at the 37th Annual Meeting of the International Continence Society.
-
Manchana T, Han HC, Lee LC (2007) The use of Prolift in the surgical treatment of pelvic organ prolapse. Int Urogynecol J 18: 54-55.
-
Roberts CH, Nnochiri A, Rostom N,Barnick C (2007) Functional and anatomical outcome of prolapse repair surgery using Prolift mesh at 6 months. Int Urogynecol J18: 161.
-
Neuman M, Friedman M (2007) Advanced mesh implants for vaginal pelvic floor reconstruction: report of 100 prolift operations. Harefuah 146: 923-927, 999-1000.
-
Altman D, Väyrynen T, Engh ME, Axelsen S, Falconer C; Nordic Transvaginal Mesh Group (2008) Short-term outcome after transvaginal mesh repair of pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 19: 787-793.
-
Altman D, Falconer C (2007) Perioperative morbidity using transvaginal mesh in pelvic organ prolapse repair. Obstet Gynecol 109: 303-308.
-
Fatton B, Amblard J, Debodinance P, Cosson M, Jacquetin B (2007) Transvaginal repair of genital prolapse: preliminary results of a new tension-free vaginal mesh (Prolift technique)--a case series multicentric study. Int Urogynecol J Pelvic Floor Dysfunct 18: 743-752.
-
Meschia M, Spreafico L, Ambrogi V, Perrone A, Dematteis G, et al. (2007) A multicenter retrospective study on transvaginal mesh repair of genital prolapse with the PROLIFT system. Int Urogynecol J 18: 25-105.
-
Reisenauer C, Kirschniak A, Drews U, Wallwiener D (2007) Anatomical conditions for pelvic floor reconstruction with polypropylene implant and its application for the treatment of vaginal prolapse. Eur J Obstet Gynecol Reprod Biol 131: 214-225.
-
Withagen M, Milani F, Kluivers K, van den Akker S, Kluivers KB, ET AL. (2007) Total vaginal mesh in pelvic organ prolapse: results after six months. Int Urogynecol J 18: 158.
-
Flam F (2007) Sedation and local anaesthesia for vaginal pelvic floor repair of genital prolapse using mesh. Int Urogynecol J Pelvic Floor Dysfunct 18: 1471-1475.
-
Jakimiuk AJJ, Borucki WB, Beta JB, Maciejewski TM, Durczyñski AD (2007) Anatomical and functional assessment of vaginal prolapse treatment in women undergoing transvaginal synthetic mesh implantation (Gynecare Prolift®). Int Urogynecol J18: 168-169.
-
Van der Vaart CH, de Leeuw JR, Roovers JP, Heintz AP (2003) Measuring health-related quality of life in women with urogenital dysfunction: the urogenital distress inventory and incontinence impact questionnaire revisited. Neurol Urodyn 22: 97-104.
-
Seeger D, Schmidt A, Kimmig R (2006) Transobturator Polypropylene Mesh Interposition For Paravaginal Defect Repair In Women With Symptomatic Cystocele POP-Q Stage III / IV- A Prospective Trial. Int Urogynecol J 17: 268-269.
-
Gadonneix P, Ercoli A, Salet-Lizée D, Cotelle O, Bolner B, et al. (2004) Laparoscopic sacrocolpopexy with two separate meshes along the anterior and posterior vaginal walls for multicompartment pelvic organ prolapse. J Am Assoc Gynecol Laparosc 11: 29-35.
-
Agarwala N, Hasiak N, Shade M (2007) Laparoscopic sacral colpopexy with Gynemesh as graft material--experience and results. J Minim Invasive Gynecol 14: 577-583.
-
Rozet F, Mandron E, Arroyo C, Andrews H, Cathelineau X, et al. (2005) Laparoscopic sacral colpopexy approach for genito-urinary prolapse: experience with 363 cases. Eur Urol 47: 230-236.
-
Hsiao KC, Latchamsetty K, Govier FE, Kozlowski P, Kobashi KC (2007) Comparison of laparoscopic and abdominal sacrocolpopexy for the treatment of vaginal vault prolapse. J Endourol 21: 926-930.
-
Maher CF, Qatawneh AM, Dwyer PL, Carey MP, Cornish A, et al. (2004) Abdominal sacral colpopexy or vaginal sacrospinous colpopexy for vaginal vault prolapse: a prospective randomized study. Am J Obstet Gynecol 190: 20-26.
-
Bacle J, Papatsoris AG, Bigot P, Azzouzi AR, Brychaet PE, et al. (2011) Laparoscopic promontofixation for pelvic organ prolapse: a 10-year single center experience in a series of 501 patients. Int J Urol 18: 821-826.
-
Sabbagh R, Mandron E, Piussan J, Brychaert PE, Tu le M (2010) Long-term anatomical and functional results of laparoscopic promontofixation for pelvic organ prolapse. BJU Int 106: 861-866.
-
Rivoire C, Botchorishvili R, Canis M, Jardon K, Rabischong B, et al. (2007) Complete laparoscopic treatment of genital prolapse with meshes including vaginal promontofixation and anterior repair: a series of 138 patients. J Minim Invasive Gynecol 14: 712-718.