International Journal of Clinical Cardiology
Brugada Syndrome; Cause of Syncope during Transcutaneous Electrical Nerve Stimulation Therapy
Abdulmelik Yildiz1, Mustafa Budancamanak2 and Cennet Yildiz3*
1Ekotom Medical Center, Cardiology, Istanbul, Turkey
2Ekotom Medical Center, Physical Therapy and Rehabilitation, Istanbul, Turkey
3Tekden Hospital, Cardiology, Istanbul, Turkey
*Corresponding author: Cennet Yildiz, Tekden Hospital, Cardiology, Istanbul, Turkey, Tel: +902125176714, Fax: +902125505757, E-mail: firdevsi@yahoo.com
Int J Clin Cardiol, IJCC-2-060, (Volume 2, Issue 6), Case Report; ISSN: 2378-2951
Received: June 23, 2015 | Accepted: November 17, 2015 | Published: November 20, 2015
Citation: Yildiz A, Budancamanak M, Yildiz C (2015) Brugada Syndrome; Cause of Syncope during Transcutaneous Electrical Nerve Stimulation Therapy. Int J Clin Cardiol 2:060. 10.23937/2378-2951/1410060
Copyright: © 2015 Yildiz A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Brugada syndrome is an genetic disorder characterized by sudden cardiac death and associated with mutations of SCN5A gene, which encodes cardiac sodium channel [1]. Fever can precipitate Brugada-like electrocardiographic (ECG) changes [2]. Syncope and sudden death usually ocur at rest or during periods of bradicardia. TENS is the application of low-level electrical current through special electrodes placed on the skin for analgesia.
Keywords
Transcutaneous Electrical Nerve Stimulation, Brugada syndrome, Syncope
Case Report
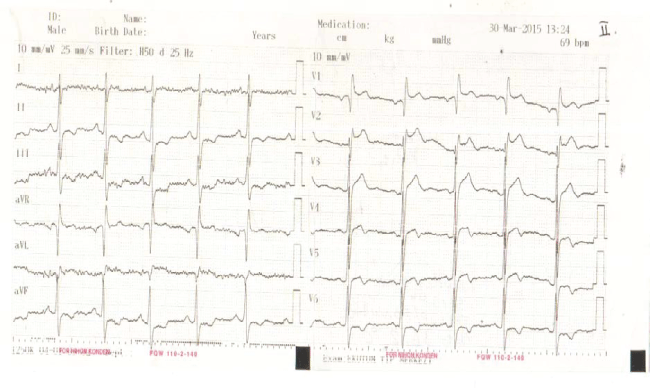
38 year old male patient with preauricular abcess developed presyncope during high-grade fever and diagnosed as having Brugada syndrome with type 1 ECG pattern. The diagnosis of Brugada syndrome was made in educational and research hospital. His Electroencephalography (EEG) was normal. Coronary angiography showed myocardial bridging of the left anteriyor descending coronary artery after second diagonal branch and no hemodynamically significant coronary artery disease. Technesium (TC99 MIBI) Myocardial Perfusion SPECT and Cardiac Magnetic Resonance imaging results were normal. Ajmaline test confirmed the diagnosis, and ventricular fibrillation (VF) induced during electrophysiological study (EPS). There was no family history of sudden death. The patient diagnosed with left shoulder adhesive capsulitis and TENS was applied for 20 min a constant frequency of 80 HZ for pain relief (Figure 1).
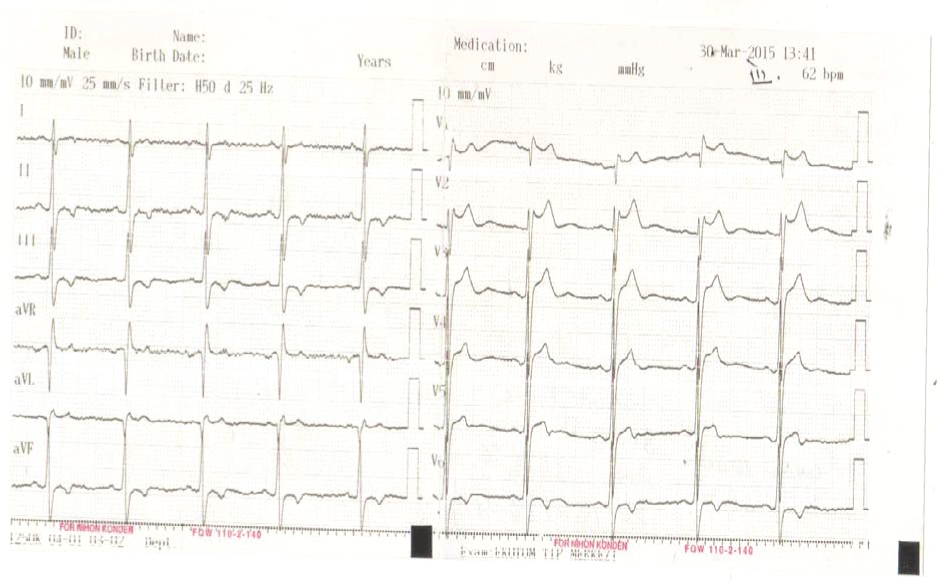
During therapy the patient experienced syncope. He was treated emergently in physical therapy service and we were unable to obtain an ECG trace in physical therapy service during firs session. ECG recordings of the patient were taken at 1, 5, 10 and 15 minutes during second session. ECG recordings showed bradycardia and dynamic ECG changes between type 2 and type 3 pattern (Figure 2). After ten minutes the patient developed presyncope. His blood pressure was 120/80 mmHg. ECG revealed bradycardia and marked QT prolonongation (QTc 425 ms). TENS treatment was stopped and subsequent sessions have been cancelled (Figure 3).
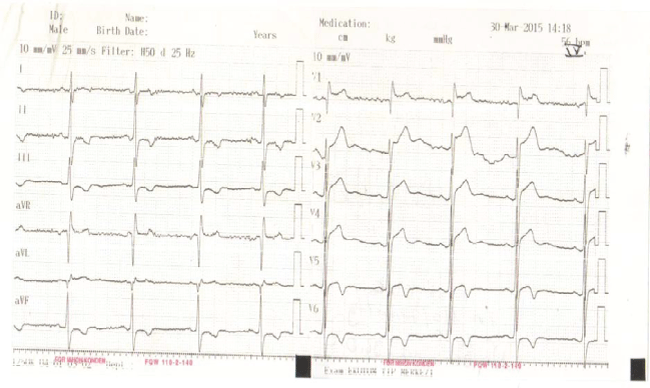
.
Figure 3: ECG showing sinus bradycardia (heart rate 56/min) and ST-T wave changes immediately after TENS therapy.
View Figure 3
Discussion
Brugada syndrome, an entity described in 1992, is characterized by episodes of ventricular tacyarrhythmias or unexpected sudden cardiac death in patients with a structurally normal heart, and a characteristic ECG consisting of a right bundle-branch block (RBBB) pattern and ST segment elevation in the precordial V1 through V3 leads [3]. Ventricular arrhythmias more often occur during rest or sleep when the vagal tone is predominant. Increased vagal tone mediated by acetylcholine decreases the calcium currents, which could lead to arrhythmogenesis via phase 2 reentry [4]. TENS is a non-invasive analgesic techique that is used for pain relief. During TENS low-level electrical currents delivered across the intact surface of the skin via electrodes. According to the "Gate Control Theory" of pain, TENS treatment is thought to activate the body's pain inhibitory system. Closure of this gate helps to block incoming pain transmission from periphery and spinal cord. It also stimulates the release of endogenous opioids. This low-level electrical currents affect sodium and potassium channels in conduction system and generation of action potential in muscles, nerves and heart [5-7].
However, virtually no information is available about the effects of TENS treatment on sodium and calcium channels in Brugada syndrome. TENS treatment leads to an increase in parasympathetic activity, resulting in bradycardia. It is known that local increase in body temperature and release of endogenous endorphins during therapy may cause sleepiness [4]. Increased vagal activity has been associated with the development of cardaic arrhythmias in Brugada syndrome. Fever-induced Brugada syndrome is a well-known entity.
In the presented case, there was no conclusive evidence for VF as a potential cause of syncope. Dynamic ECG changes between type 2 and type 3 pattern with bradycardia during second session, a prolonged QTc interval without hypotension could however be interpreted as supporting evidence for VF.
Polymorphic ventricular tachycardia and ventricular fibrillation are the most common arrhythmias in rare cases, syncope in Brugada syndrome may be due to vasovagaal mechanism [8]. This seems unlikely in our patient as his symptoms were unrelated to postural challenge. The effect of TENS on neuron action potential is well-known, but its effect on cardiac myocytes is uncertain. In our case report we would like to draw atttention to the possibility of cardiac arrhythmia during TENS therapy in patients with Brugada syndrome.
References
-
Antzelevitch C (2006) Brugada syndrome. Pacing Clin Electrophysiol 29: 1130-1159.
-
Brugada R, Brugada J, Antzelevitch C, Kirsch GE, Potenza D, et al. (2000) Sodium channel blockers identify risk for sudden death in patients with ST-segment elevation and right bundle branch block but structurally normal hearts. Circulation 101: 510-515.
-
Brugada P, Brugada J (1992) Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome: a multicenter report. J Am Coll Cardiol 20: 1391-1396.
-
Litovsky SH, Antzelevitch C (1990) Differences in the electrophysiological response of canine ventricular subendocardium and subepicardium to acetylcholine and isoproterenol. A direct effect of acetylcholine in ventricular myocardium. Circ Res 67: 615-627.
-
Walter R, Frontera (2010) DeLisa's phsical medicine and rehabilitation: Principles and practice, two volume set (rehabilitation medicine (Delisa)) Hardcover.
-
Eijkelkamp N, Linley JE, Baker MD, Minett MS, Cregg R, et al. (2012) Neurological perspectives on voltage-gated sodium channels. Brain 135: 2585-2612.
-
Bian D, Chen YG, Sui YJ, Tian H, Liu YL, et al. (2015) Effect of electroacupuncture stimulation of "Neiguan" (PC 6) on expression of alpha- and beta-subunit proteins of voltage-gated sodium channels in rats with myocardial ischemia. Zhen Ci Yan Jiu 40: 45-49.
-
Patruno N, Pontillo D (2006) Brugada syndrome and vasovagal syncope. Pacing Clin Electrophysiol 29: 215.