International Journal of Clinical Cardiology
Early Recurrence of Myocardial Infarction in a Young Female caused by Left Main Coronary Artery Thrombosis
Silvio Nocco*, Laura Concas, Daniele Congiu and Rinaldo Aste
Department of Cardiology, Sirai Hospital, Carbonia, Italy
*Corresponding author: Silvio Nocco, Department of Cardiology, Sirai Hospital, Via Ospedale, 09013, Carbonia, Italy, Tel: (0039) 070/6683382, E-mail: silvionocco@tiscali.it
Int J Clin Cardiol, IJCC-2-062, (Volume 2, Issue 6), Case Report; ISSN: 2378-2951
Received: August 14, 2015 | Accepted: November 26, 2015 | Published: November 30, 2015
Citation: Nocco S, Concas L, Congiu D, Aste R (2015) Early Recurrence of Myocardial Infarction in a Young Female caused by Left Main Coronary Artery Thrombosis. Int J Clin Cardiol 2:062. 10.23937/2378-2951/1410062
Copyright: © 2015 Nocco S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A young female, cardiovascular risk factors free, was admitted to the coronary care unit for a sub-acute myocardial infarction caused by a critical ostial stenosis of the left anterior descending artery, treated with coronary angioplasty and insertion of two drug-eluting stents. Despite the administration of aggressive treatment, just 5 days after discharge, the patient was readmitted for early recurrence of myocardial infarction caused by left main coronary artery thrombosis treated with emergency angioplasty and insertion of three drug-eluting stents.
Keywords
Acute coronary syndrome, Young, Risk factors, Atherosclerosis, Therapy
Introduction
Acute myocardial infarction (MI) in young adults is rare; it can be broadly divided into two groups: those with angiographically normal coronary arteries and those with coronary artery disease of varying aetiology [1]. Fortunately, its incidence is uncommon in patients younger than 45 years. Indeed, just 3% of patients with coronary heart disease are aged less than 40 years [2]. Various pathophysiological mechanisms, including familial hypercholesterolaemia [3], hyperhomocysteinaemia [4], smoking, hypertension, insulin resistance diabetes and obesity, may be involved in the accelerated atherosclerosis. On the other hand, hypercoagulable states, antiphospholipid syndrome, coronary artery spasm, coronary embolisation and myocardial bridging are involved in myocardial infarction involving angiographically "normal" coronary arteries [2].
Case Report
A 39-year-old female, not presenting any cardiovascular risk factors, was admitted to the coronary care unit of the Hospital Sirai Department of Cardiology (Carbonia, Italy) for a sub-acute myocardial infarction complicated by post infarct angina. The only therapy the patient was taking was oral contraceptives.
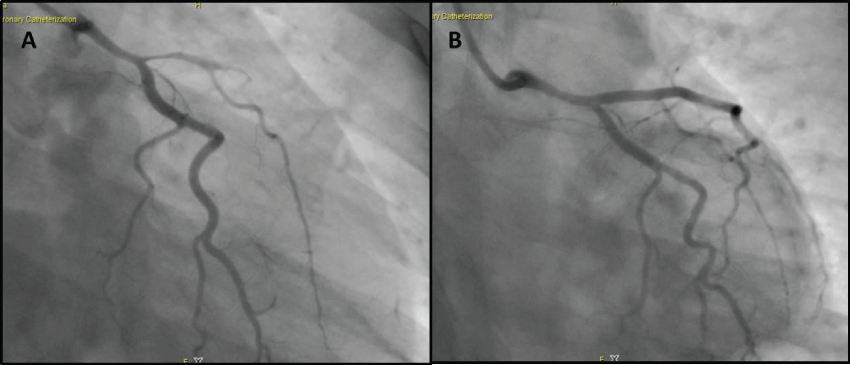
The patient's electrocardiogram (ECG) taken upon admission showed Q waves in DI, aVL and from V2 to V4, ST depression and T-wave inversion in the inferior lead. Echocardiography demonstrated akinesia of the apical segments, the mid-basal segment of anterior interventricular septum (IVS) and the anterior wall and of the middle segment of the inferior IVS. The left ventricular ejection fraction (LVEF) was equal to 32% and mild diastolic dysfunction was found. The patient received emergency coronary angiography, showed single-vessel disease with critical ostial stenosis of the left anterior descending artery (LVDA) and thrombotic occlusion of the middle portion (Figure 1, panel A). After administration of a standard dose of unfractionated heparin, this was treated with coronary angioplasty and insertion of two drug-eluting stents, with a good angiographic result (Figure 1, panel B).
.
Figure 1: First coronary angiography: anteroposterior view revealed single-vessel disease with critical stenosis of the ostial left anterior descending artery and thrombotic occlusion of the middle portion (panel A), view after insertion of two drug-eluting stents (panel B).
View Figure 1
Given the young age and the absence of traditional cardiovascular risk factors, the patient was subjected to further investigation. Laboratory tests were unable to detect any defective alterations in coagulation, thrombophilia or autoimmunity. The echo-Doppler of the carotid arteries and CT scan of the aorta were normal.
The patient's clinical course was characterised by both clinical and haemodynamic stability. After five days she was discharged on aspirin 100 mg/day, ticagrelor180 mg/day, atorvastatin 80 mg/day, bisoprolol 2, 5 mg/die, polyunsaturated fatty acids 1000 mg/day, ivabradine 10 mg/day and omeprazole 20 mg/day. The patient's contraceptive oestrogen-progestin therapy was discontinued. The echocardiogram performed prior to discharge showed improved systolic function (LVEF 43%) with residual akinesia of the apical segments and the middle segment of the anterior wall.
Just 5 days after discharge, the patient was readmitted for the onset of chest pain with evidence of anterior ST-segment elevation on the ECG, complicated by cardiogenic shock. An emergency echocardiogram showed akinesia of the apex and the middle segments of the anterior wall and IVS, and hypokinesia of the inferior-lateral and anterior-lateral middle segment with a LVEF of 35%.
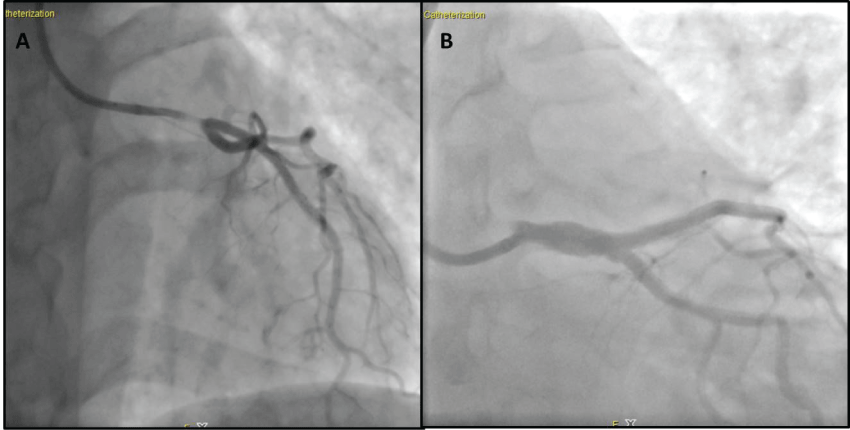
During coronary angiography, performed with the aid of an intraortic balloon pump, sub occlusive thrombotic stenosis of the body and distal region of the left main coronary artery was evident, engaging the ostium of the LVDA and the circumflex coronary artery (Cx) (Figure 2, panel A). This was treated with coronary angioplasty, complicated by dissection of the Cx ostium, and insertion of three drug-eluting stents on the left main, the ostium of the LVDA and the Cx (Figure 2, panel B) (Table 1).
.
Figure 2: Second coronary angiography: left anterior oblique view showed sub occlusive thrombotic stenosis of the body and the distal left main coronary artery, engaging the ostium of the LVDA and the circumflex coronary artery (panel A), caudal left anterior oblique view after insertion of three drug-eluting stents on the left main, the ostium of the LVDA and the Cx (panel B).
View Figure 2
![]()
Table 1: Clinical Manifestation.
View Table 1
The patient's clinical course was once again characterised by clinical and haemodynamic stability. During hospitalisation, the patient's therapy with ticagrelor was replaced with prasugrel, and off-label therapy with low-molecular-weight heparin (LMWH) was initiated.
The echocardiogram performed prior to discharge (following 20 days hospitalisation) showed an improvement in systolic function (LVEF 43%) with residual akinesia of the apical segments and the middle segment of the anterior wall. A moderate reduction of diastolic function was also highlighted. The submaximal exercise test performed prior to discharge showed no arrhythmias and no repolarisation abnormalities during stress. Control coronary angiography showed patency of vessels treated and TIMI 3 flow score [5].
The patient was discharged on therapy with aspirin, prasugrel, bisoprolol, atorvastatin, bisoprolol, polyunsaturated fatty acids, ivabradine, omeprazole, and LMWH (LMWH was administered for one month). After six months of follow up, the patient was asymptomatic, haemodynamically stable and in NYHA class I. Echocardiographic and ECG findings were unchanged.
Discussion
In the present case study, no alterationsin coagulation or autoimmunity was identified. Coronary angiography revealed premature coronary atherosclerosis despite the fact that the patienthad not any of the traditional cardiovascular risk factors. The association between myocardial infarction and the use of oral contraceptives is controversial [6], this may be an independent predictor of a high-grade thrombus burden [7]. Despite the application of aggressive risk factor management, the discontinuation of oral contraceptives and the dual antiplatelet therapy, our patient had an early recurrence of an acute coronary event.
The numerous cases of myocardial infarction in young adults described are related to autoimmune diseases [8], nephrotic syndrome [9], antiphospholipid syndrome [10], spontaneous coronary artery dissection [11], antithrombin III deficiency [12], cigarette smoking [13], and familial hyperlipidemia [14].
It was not possible to identify the factors that were responsible for the coronary events and early atherosclerosis in this patient. Thus, an as yet unidentified mechanism is likely to be at the base of this and other similar cases. Future studies focussed on subjects completely free of cardiovascular risk factors would be helpful to identify the underlying causes leading to infarction and thus the best treatment strategies.
Finally, some doubt remains about which antiplatelet and anticoagulant treatment (double anti-aggregation only or anticoagulant therapy) should be prescribed for early recurrence of acute coronary syndrome, and for how long this should be continued.
Conflicts of Interest and Funding
There are no conflicts of interest to declare and no grants or funding was received by any of the authors for this study.
The patient is aware of this publication and has signed a written consent form.
References
-
Osula S, Bell GM, Hornung RS (2002) Acute myocardial infarction in young adults: causes and management. Postgrad Med J 78: 27-30.
-
Jalowiec DA, Hill JA (1989) Myocardial infarction in the young and in women. Cardiovasc Clin 20: 197-206.
-
Vuorio AF, Kontula K, Turtola H, Sajantila A (1999) Post mortem molecularly defined familial hypercholesterolemia and sudden cardiac death of young men. Forensic Sci Int 106: 87-92.
-
Booth GL, Wang EE (2000) Preventive health care, 2000 update: screening and management of hyperhomocysteinemia for the prevention of coronary artery disease events. The Canadian Task Force on Preventive Health Care. CMAJ 163: 21-29.
-
De Boer MJ, Reiber JHC, Suryapranata H, van den Brand MJBM, Hoorntje JCA, et al. (1995) Angiographic findings and catheterisation laboratory events in patients with primary coronary angioplasty or streptokinase therapy for acute myocardial infarction. Eur Heart J 16: 1347-1355.
-
Roach RE, Helmerhorst FM, Lijfering WM, Stijnen T, Algra A, et al. (2015) Combined oral contraceptives: the risk of myocardial infarction and ischemic stroke. Cochrane Database Syst Rev.
-
Karabay CY, Kokabay G, Oduncu V, Kalayci A, Guler A, et al. (2013) Drospirenone-containing oral contraceptives and risk of adverse outcomes after myocardial infarction. Catheter Cardiovasc Interv 82: 387-393.
-
Korkmaz C, Cansu DU, Kasifoglu T (2007) Myocardial infarction in young patients (< or = 35 years of age) with systemic lupus erythematosus: a case report and clinical analysis of the literature. Lupus 16: 289-297.
-
Zaffanello Marco, Massimo Franchini (2007) Thromboembolism in childhood nephrotic syndrome: a rare but serious complication. Hematology 12: 69-73.
-
Davies JO, Hunt BJ (2007) Myocardial infarction in young patients without coronary atherosclerosis: assume primary antiphospholipid syndrome until proved otherwise. Int J Clin Pract 61: 379-384.
-
Khan, Nazim Uddin Azam (2015) Spontaneous coronary artery dissection. Acute cardiac care.
-
Fennich Nada, Akhbour Salwa, Bouzamour Nadia, Oukerraj Latifa, Zarzur Jamila, et al. (2013) Acute coronary syndrome in a young woman with antithrombin III deficiency. Journal of Cardiology Cases 7: e101-e103.
-
Lin Yen-Chen, Lung-An HSU, Yu-Shien KO, Chi-Tai KUO, Wei-Jan Chen, et al. (2010) Impact of conventional cardiovascular risk factors on acute myocardial infarction in young adult Taiwanese. Acta Cardiol Sin 26: 228-234.
-
Muthupalaniappen L, Menon RK, Das S (2012) Acute myocardial infarction in an adolescent. Saudi Med J 33: 197-200.





