International Journal of Clinical Cardiology
Diagnosis of Stress-Induced Cardiomyopathy in a Patient with an Abnormal Myocardial SPECT Imaging
Teo Tee Yin Tracy1*, McNeely Parren1, Demetroulis Elaine2, Staffey Kimberly2 and Graham Michael1
1Department of Radiology, University of Iowa Hospital & Clinics (UIHC), Iowa City, USA
2Division of Cardiovascular Medicine, University of Iowa Hospital & Clinics (UIHC), Iowa City, USA
*Corresponding author: Teo Tee Yin Tracy, D.O, MBA, Chief resident of Nuclear Medicine, Nuclear Medicine Residency, Department of Radiology, Division of Nuclear Medicine (3804 JPP), University of Iowa Hospital & Clinics (UIHC), 200 Hawkins drive, Iowa City, IA, 52241, USA, Tel: 319-356 3380, Fax: 319-356 2220, E-mail: teeyin-teo@uiowa.edu
Int J Clin Cardiol, IJCC-2-063, (Volume 2, Issue 6), Case Report; ISSN: 2378-2951
Received: March 10, 2015 | Accepted: November 26, 2015 | Published: November 30, 2015
Citation: Tracy TTY, Parren M, Elaine D, Kimberly S, Michael G (2015) Diagnosis of Stress-Induced Cardiomyopathy in a Patient with an Abnormal Myocardial SPECT Imaging. Int J Clin Cardiol 2:063. 10.23937/2378-2951/1410063
Copyright: © 2015 Tracy TTY, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We present a case of stress-induced cardiomyopathy in a 66 year old male precipitated by electroconvulsive (ECT) for catatonia related to severe recurrent depression. Patient suffered from decades of bipolar syndrome with severe depression that is refractory from medication therapies. As the frequency of the recent admissions increases, the patient's guardian consented to ECT to treat his depression. During the ECT procedure, he developed non-sustained ventricular tachycardia (NSVT). The onset of the clinical symptoms coincide with a stressful event and findings of the single-photon emission computed tomography (SPECT) stress myocardial perfusion imaging (MPI) with Tc-99m tetrofosmin are compatible with stress-induced cardiomyopathy after an unsuccessful attempt to treat depression with ECT.
Keywords
Classic Takotsubo cardiomyopathy, Myocardial perfusion SPECT, Akinetic apex wall motions
Takotsubo cardiomyopathy was first described in Japan with an incidence of 0.02 and predilection for females [1]. In North America, Takotsubo cardiomyopathy is more commonly known as stress-induced cardiomyopathy or transient apical ballooning syndrome. Stress-induced cardiomyopathy is a reversible cardiomyopathy, typically involving the left ventricular apex and its adjacent areas after an insult of sudden emotional or physical stressors (Figure 1). The pathophysiology of the non-ischemic cardiomyopathy suggests that a sudden stressor temporarily weakens the myocytes contractility (Figure 2 and Figure 3) (AV101) [2,3]. The removal of the offending stressor, the transient vasospasm presumably will be resolved.
.
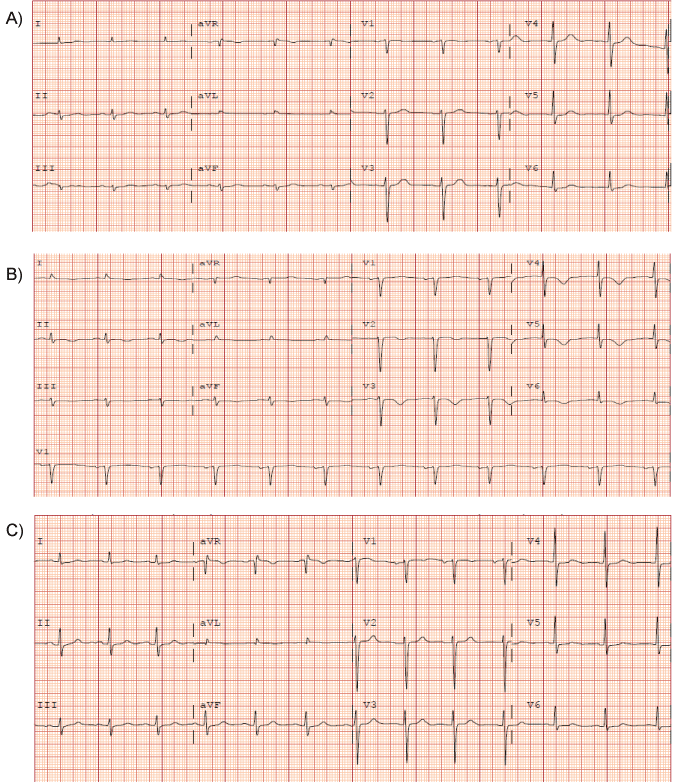
Figure 1A: Baseline ECG showed normal sinus rhythm, normal axis and normal R wave progression.
1B: ECG following ECT and NSVT event showed sinus bradycardia, and T wave inversions in the precordial leads.
1C: Follow-up ECG approximately 6 weeks after the event showed normal sinus rhythm with resolution of T-wave inversions (returned to baseline).
View Figure 1
.
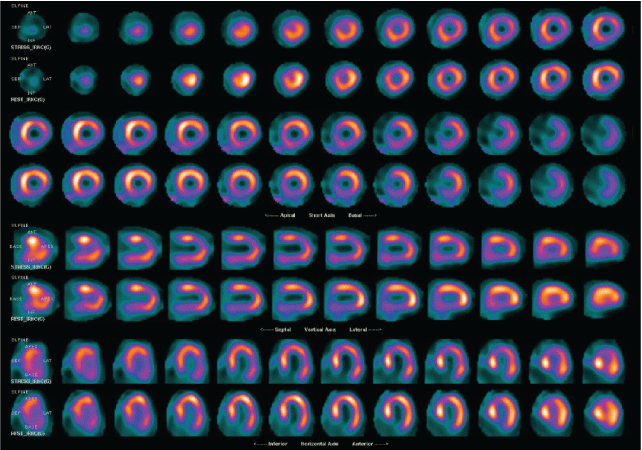
Figure 2: Myocardial perfusion SPECT images. Gated myocardial perfusion SPECT images are also supplemented.
View Figure 2
The most common ECG changes seen are diffuse T-wave inversions with prolonged QTc. Serum troponin T typically is only mildly elevated. The hallmark findings are apical ballooning of the left ventricle with reduced ejection fraction typically seen on transthoracic echocardiogram or invasive ventriculography [4,5]. Stress-induced cardiomyopathy is a diagnosis of exclusion and often requires anatomic evaluation of the coronary arteries to exclude obstructive disease. Left ventricle systolic function and wall motion abnormalities typically normalize in 4-6 weeks following the event [6,7].

.
Figure 3: Cardiac catheterization.
3A: RAO caudal view showing patent left main (LM), left anterior descending (LAD), and left circumflex (LCX) arteries.
3B: RAO cranial view showing patent LAD.
3C: LAO view showing patent RCA.
View Figure 3
Supplementary file
References
-
Notaristefano A, Niccoli Asabella A, Di Palo A, Ferrari C, Rubini G (2012) Morpho-functional imaging of a rare case of tako-tsubo syndrome in a young pregnant woman. Recenti Prog Med 103: 549-551.
-
Rau CM, Kauffmann M, Rau CL, Cereceda M, Castro G, et al. (2011) Tako-Tsubo syndrome: report of one case. Rev Med Chil 139: 348-352.
-
Hurst RT, Prasad A, Askew JW 3rd, Sengupta PP, Tajik AJ (2010) Takotsubo cardiomyopathy: a unique cardiomyopathy with variable ventricular morphology. JACC Cardiovasc Imaging 3: 641-649.
-
Sciagra R, Parodi G, Del Pace S, Genovese S, Zampini L, et al. (2010) Abnormal response to mental stress in patients with Takotsubo cardiomyopathy detected by gated single phonto emission computed tomography. Eur J Nucl Med Mol Imaging 37: 765-772.
-
Burgdorf C, Von Hof K, Schunkert H, Kurowski V (2001) Regional alterations in myocardial sympathetic innervations in patients with transient left ventricular apical ballooning (Tako-Tsubo cardiomyopathy). J Nucl Cardiol 15: 65-72.
-
Cimarelli S, Sauer F, Morel O, Ohlmann P, Constantinesco A, et al. (2010) Transient left ventricular dysfunction syndrome: patho-physiological bases through nuclear medicine imaging. Int J Cardiol 144: 212-218.
-
Mena LM, Martin F, Melero A, Ramos A, Jimenez IR (2011) Takotsubo syndrome. Usefulness of nuclear medicine studies. Rev Esp Med Nucl 30: 104-106.





