International Journal of Clinical Cardiology
Accuracy of Doppler Echocardiographic Estimates of Pulmonary Artery Pressures at the King Faisal Specialist Hospital and Research Center Riyadh
I.Y. Nizami* and Saeed Akram
Organ Transplant Center, King Faisal Specialist Hospital and Research Center, Riyadh 11211, Saudi Arabia
*Corresponding author: I.Y. Nizami, Organ Transplant Center, King Faisal Specialist Hospital and Research Center, Riyadh 11211, Saudi Arabia, Tel: 96614647272, Fax: 96614427499, E-mail: imranyaqoob@kfshrc.edu.sa
Int J Clin Cardiol, IJCC-2-066, (Volume 2, Issue 6), Research Article; ISSN: 2378-2951
Received: September 02, 2015 | Accepted: December 08, 2015 | Published: December 11, 2015
Citation: Nizami IY, Akram S (2015) Accuracy of Doppler Echocardiographic Estimates of Pulmonary Artery Pressures at the King Faisal Specialist Hospital and Research Center Riyadh. Int J Clin Cardiol 2:066. 10.23937/2378-2951/1410066
Copyright: © 2015 Nizami IY, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background and Objectives: The accuracy of Doppler echocardiography in estimating pulmonary arterial hypertension has been a center of debate with recent reports suggesting poor correlation between the Doppler echocardiographic estimation of pulmonary pressure with the one measured by right heart catheterization. Our aim is to study the correlation between the Doppler echocardiographic estimates of pulmonary artery pressures with the right heart catheterization measured pulmonary artery pressures at our center.
Design and Settings: This is a non-randomized, retrospective, observational study.
Methods: Retrospective analysis of 100 consecutive patients was done who have undergone the echocardiogram and right heart catheterization within 3 months of each other during the last five years at our hospital.
Results: here was a moderate correlation between PASP determined during RHC and estimated PASP using Doppler echocardiography (Pearson correlation r = 0.51, P < 0.0001). Using the predefined definition of an inaccurate Doppler echocardiographic estimation of PASP as ± 10 mmHg different from PASP measured during RHC, we found that Doppler echocardiography was inaccurate 49% (49/100) of the time. When inaccurate, Doppler Echocardiography overestimated PASP by as much as 38 mmHg and underestimated PASP by as much as 37 mmHg.
Conclusion: The Doppler echocardiographic estimates of PASP were found inaccurate at our center.
Keywords
Lung transplantation, Pulmonary Hypertension, Echocardiogram.
Abbreviations
PASP: Pulmonary Artery Systolic Pressur, LAS: Lung Allocation Score, DE: Doppler Echocardiography, RAP: Right Atrial Pressure
Introduction
Doppler echocardiography is widely used as the modality of choice for screening the patients suspected of suffering from pulmonary hypertension. It is also a standard test in evaluating potential lung transplant candidates. The accuracy of Doppler echocardiography in estimating pulmonary arterial hypertension has been a center of debate with recent reports suggesting poor correlation between the Doppler echocardiographic estimation of pulmonary pressure with the one measured by right heart catheterization [1-4]. The number of patients referred for both lung transplantation and pulmonary hypertension is steadily increasing at our institute. The management of pulmonary hypertension requires a serial measurement of cardiac hemodynamics. The patients referred for lung transplant also require an estimation of pulmonary arterial pressure to assign them an accurate lung allocation score (LAS). The LAS determines the priority of patients listed for lung transplantation. The right heart catheterization remains the gold standard for the measurement of pulmonary arterial pressures but is invasive and often requires longer waiting time.
Our aim is to study the correlation between the Doppler echocardiographic estimates of pulmonary artery pressures with the right heart catheterization measured pulmonary artery pressures at our center.
Methods
The Research Ethics Committee (REC) at The King Faisal Specialist Hospital and Research Center, Riyadh approved the study. Proposal number was 2121120.
The charts of all patients that have undergone the echocardiogram and right heart catheterization within 3 months of each other during the last five years at our hospital were reviewed. The estimation of pulmonary artery systolic pressure by echocardiogram was compared with the pulmonary artery systolic pressure measured directly by the right heart catheterization. A difference of > 10 mmHg was considered as poor correlation. A difference of < 10 mmHg was considered as good correlation between the two measurements and accurate for statistical considerations. The data collected included age, sex, diagnosis for which the right heart catheterization was being performed, date of echocardiogram, date of right heart catheterization, pulmonary artery systolic pressure by echocardiogram and right heart catheterization.
Right-Sided Heart Catheterization
All RHC measurements made during the study were performed by certified physicians experienced in cardiac catheterization.
Echocardiography
Two-dimensional transthoracic echocardiography and DE (Doppler Echocardiography) were performed using general electric, VIVID E9 machine. Serial number VE91055. Echocardiograms were performed in multiple views to obtain the optimal appearing tricuspid regurgitation (TR) jet. Patients were excluded from the study if tricuspid regurgitation was not present on DE or if the TR jet was insufficient to estimate the PASP. After acquiring the necessary images, the TR jet velocities were measured, and estimated PASPs were determined using the modified Bernoulli equation in conjunction with an echocardiographic estimation of RAP. All echocardiographic and DE studies were performed by an experienced and certified sonographer. Interpretations of echocardiographic and DE measurements were performed only by physicians experienced with and board certified in echocardiography.
Statistics
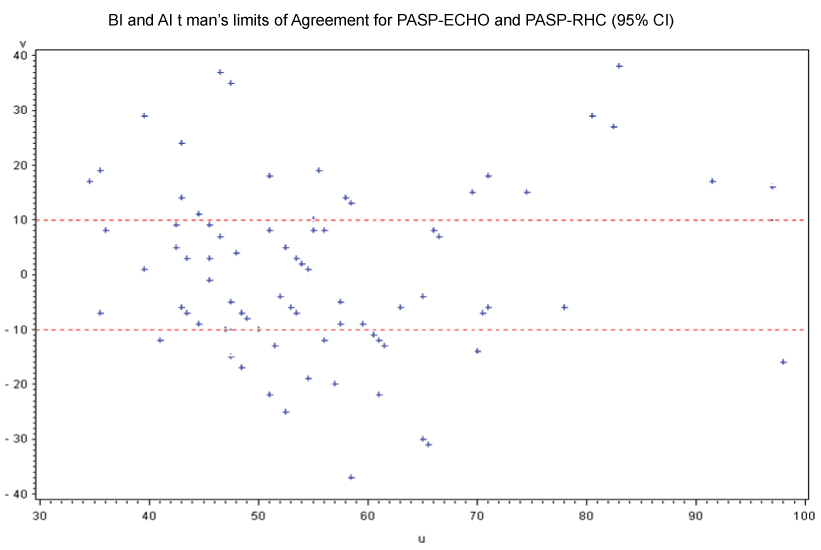
Bland-Altman analysis was used to evaluate the agreement between the Doppler echocardiographic (DE) estimates of pulmonary artery systolic pressure (PASP) and right heart catheterization measurement of PASP. DE estimates of PASP were considered accurate if the differences were within the 95% limits of agreement between the DE and RHC measurements were small and not considered clinically relevant. Alternatively, it was unacceptable to consider DE estimates of PASP as accurate compared with RHC measurement of PASP if the 95% limits of agreement were large and thought to be of clinical relevance. Accuracy was predefined as 95% limits of agreement within ± 10 mmHg for PASP estimates.
Results
Among 100 patients the mean age was 41 ± 13 SD, 81 were male and 19 were female. The indications for right heart catheterization included evaluation for lung transplant, evaluation of pulmonary hypertension, congestive heart failure and valvular heart disease. Wide ranges of pulmonary artery systolic pressure (PASP) were noted during Doppler echocardiographic (32 mmHg to 105 mmHg) and right heart catheterization (25 mmHg to 106 mmHg) measurement. There was a moderate correlation between PASP determined during RHC and estimated PASP using Doppler echocardiography (r = 0.51, P < .0001). Using the predefined definition of an inaccurate Doppler echocardiographic estimation of PASP as ± 10 mmHg different from PASP measured during RHC, we found that Doppler echocardiography was inaccurate 49% (49/100) of the time. When inaccurate, Doppler Echocardiography overestimated PASP by 38 mmHg and underestimated PASP by 37 mmHg (Table 1, Figure 1).
![]()
Table 1: Variable N = 100.
View Table 1
Discussion
The number of patients referred for lung transplant and for management of pulmonary hypertension in our center is increasing steadily. The patients referred for lung transplant are prioritized on the waiting list based on lung allocation score (LAS). Patients with higher LAS score are given priority over patients with lower LAS score. One of the components of LAS score is pulmonary arterial pressures. A wrong calculation of LAS score can lead to incorrect prioritization of the deceased donor lungs. Similarly, the number of patients referred for the diagnosis and management of pulmonary hypertension is increasing at our center. The pulmonary hypertension specific medications are not only expensive but also have potential of causing serious side effects.
There are several potential pitfalls to explain the inaccuracy of DE in estimation of PASP. Whereas PASP is measured directly during RHC, estimation of PASP using DE requires a two-step process, with each step having its own inherent imprecision [1]. The pressure gradient between the right ventricle (RV) and right atrium during systole must be determined, and this requires the patient to have tricuspid regurgitation. If tricuspid regurgitation is present, a TR Doppler signal suitable for performing a precise measurement of the peak TR velocity must also be present. Unfortunately, there is substantial variability in the quality of the TR jet in patients with PH, which contributes to imprecise determinations of the peak TR velocity. Also, the modified Bernoulli equation assumes a perfect, parallel alignment between the Doppler beam and the TR jet. Failure to correct for the angle between the Doppler beam and TR jet can result in an inaccurate determination of the peak TR velocity used to determine the pressure gradient. Even when the TR jet is of sufficient quality and the Doppler beam is aligned optimally, the presence of severe tricuspid regurgitation, a common finding in patients with PH, may result in an underestimation of this pressure gradient [1]. Determination of this pressure gradient between the RV and right atrium is followed by the addition of an echocardiographic estimate of RAP, using the parameters of IVC size and collapsibility as a surrogate for the directly measured RAP. However, a recent study has shown that RAP estimates using echocardiography was relatively imprecise. Because of the many steps involved in the noninvasive estimation of PASP, each with its own inherent limitations, it is not particularly surprising that we have found using DE estimates of PASP to be an unreliable method in patients with PH [1].
Despite the unreliability of DE to accurately determine PASP, echocardiography remains a critically important tool in patients with PH by providing an assessment of various indices of RV size and function, LV size and function and presence or absence of valvular heart disease. Thus DE remains a vital initial screening test in patients referred for lung transplant and for management of PH.
Our study has several limitations. It is retrospective in nature; the DE measurements of PASP and RHC are not done simultaneously. This, however, represents the real life situation as it takes us anywhere from few weeks to three months to organize a RHC after the DE. An ideal study would have been to perform both measurements simultaneously.
We also realize that the topic has been studied by several previous authors [1-7] but a significant controversy exists regarding the accuracy of DE in measurement of PASP. The same topic was a center of debate among the cardiologists and the lung transplant physicians at our center especially when a patient with mildly elevated PASP on DE was referred for a RHC. As mentioned earlier PASP is a component of LAS and therefore determines the urgency of lung transplant in patients waiting on the lung transplant waiting list. Both overestimation and underestimation of PASP will wrongly assign the LAS and therefore can result in an unfair allocation of the deceased donor lungs.
Conclusion
In conclusion, similar to previous reports we found that the estimation of PASP by DE was inaccurate at our center. DE remains a good screening test in patients referred for lung transplant and for PAH management, but for correct calculation of LAS score and accurate diagnosis of PH, right heart catheterization is mandatory.
References
-
Rich JD, Shah SJ, Swamy RS, Kamp A, Rich S (2011) Inaccuracy of Doppler echocardiographic estimates of pulmonary artery pressures in patients with pulmonary hypertension: implications for clinical practice. Chest 139: 988-993.
-
Harrison W Farber, Aime J foreman, Dave P Miller, Micheal D McGoon (2011) REVEAL registry: Correlation of Right Heart Catheterization and Echocardiography in Patients with Pulmonary Arterial Hypertension. Congest Heart fail 17: 56-64.
-
Micah R Fisher, Paul R Forfia, Elzbieta Chamera, Traci Houston-Harris, Hunter C Champion, et al. (2009) Accuracy of Doppler Echocardiography in the Hemodynamic Assessment of Pulmonary Hypertension. Am J Respir Crit Care Med 179: 615-621.
-
Attaran RR, Ramaraj R, Sorrell VL, Movahed MR (2009) Poor correlation of estimated pulmonary artery systolic pressure between echocardiography and right heart catheterization in patients awaiting cardiac transplantation: results from the clinical arena. Transplant Proc 41: 3827-3830.
-
Berger M, Haimowitz A, Van Tosh A, Berdoff RL, Goldberg E (1985) Quantitative assessment of pulmonary hypertension in patients with tricuspid regurgitation using continuous wave Doppler ultrasound. J Am Coll Cardiol 6: 359-365.
-
Currie PJ, Seward JB, Chan KL, Fyfe DA, Hagler DJ, et al. (1985) Continuous wave Doppler determination of right ventricular pressure: a simultaneous Doppler-catheterization study in 127 patients. J Am Coll Cardiol 6: 750-756.
-
Fisher MR, Criner GJ, Fishman AP, Hassoun PM, Minai OA, et al. (2007) Estimating pulmonary artery pressures by echocardiography in patients with emphysema. Eur Respir J 30: 914-921.