International Journal of Clinical Cardiology
Dilated Cardiomyopathy due to Vitamin D Deficiency
Nalan Karabayir1,2*, Kelesoglu E2, Helen Bornau3, Kazim Oztarhan3, Aktas D4 and Erdem A4
1Faculty of Medicine, Istanbul Medipol University, Istanbul, Turkey
2Pediatrics Department, Istanbul Medipol University, Turkey
3Pediatric Cardiology, Kanuni Sultan Suleyman Training and Education Hospital, Turkey
4Pediatric Cardiology Department, Istanbul Medipol University, Turkey
*Corresponding author: Nalan Karabayir, MD, Pediatrics Department, Istanbul Medipol University, Kartaltepe mah. Aksoy sok 6/11, Bakirkoy, Istanbul, Turkey, Tel: 905064887276, E-mail: nalankarabayir@hotmail.com
Int J Clin Cardiol, IJCC-3-084, (Volume 3, Issue 2), Case Series; ISSN: 2378-2951
Received: May 30, 2016 | Accepted: August 04, 2016 | Published: August 06, 2016
Citation: Karabayir N, Kelesoglu E, Bornau H, Oztarhan K, Aktas D, et al. (2016) Dilated Cardiomyopathy due to Vitamin D Deficiency. Int J Clin Cardiol 3:084. 10.23937/2378-2951/1410084
Copyright: © 2016 Karabayir N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Dilated cardiomyopathy, which mostly has an idiopathic etiology or is caused by genetic inheritance or infection, may cause irreversible congestive heart failure. Hypocalcemia is a rare etiology of reversible dilated cardiomyopathy. Cardiogenic shock related to hypocalcemic cardiomyopathy is a rare event. Here we report two cases with congestive heart failure who was diagnosed as having dilated cardiomyopathy secondary to hypocalcemia. After calcium and vitamin D replacement therapy, the patients showed improvement in left ventricular function. Hypocalcemia should be included in the differential diagnosis of dilated cardiomyopathy.
Keywords
Cardiogenic shock, Dilated cardiomyopathy, Hypocalcemia, Vitamin D deficiency
Introduction
Dilated cardiomyopathy (DCM), which mostly has an idiopathic etiology, or is caused by genetic inheritance or infection, can cause irreversible congestive heart failure. Although hypocalcemia secondary to vitamin deficiency is an important cause of DCM in infants, cardiogenic shock as a presenting feature without clinical or radiological features of rickets is very rarely reported in the literature [1-4].
Here, we report two cases of DCM secondary to hypocalcemia that originated from a nutritional vitamin D deficiency induced rickets both were exclusively breastfed by mothers who had vitamin D deficiency.
Case 1
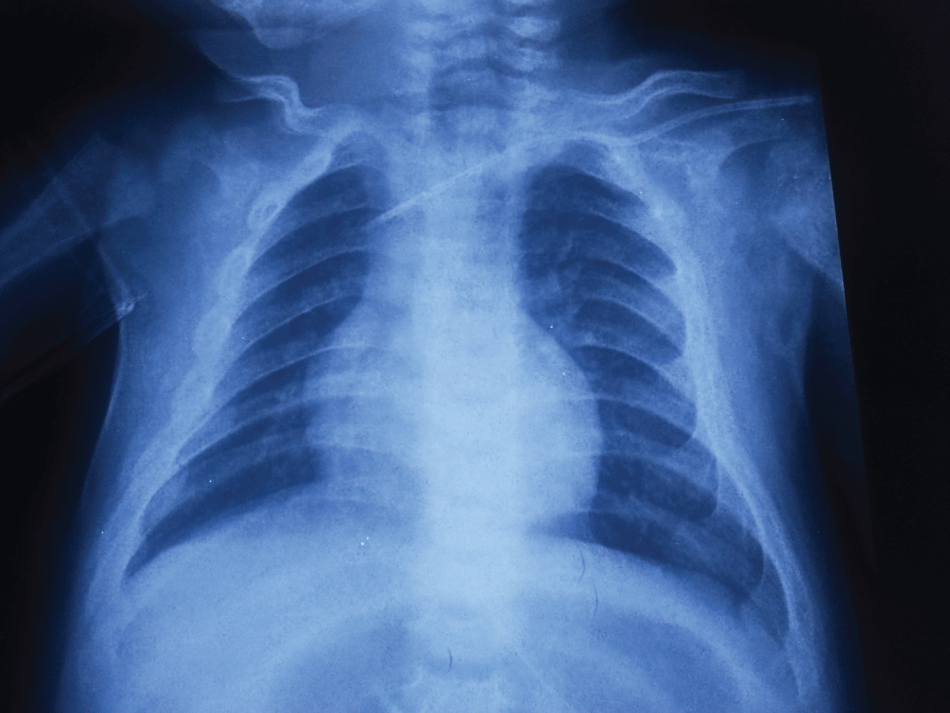
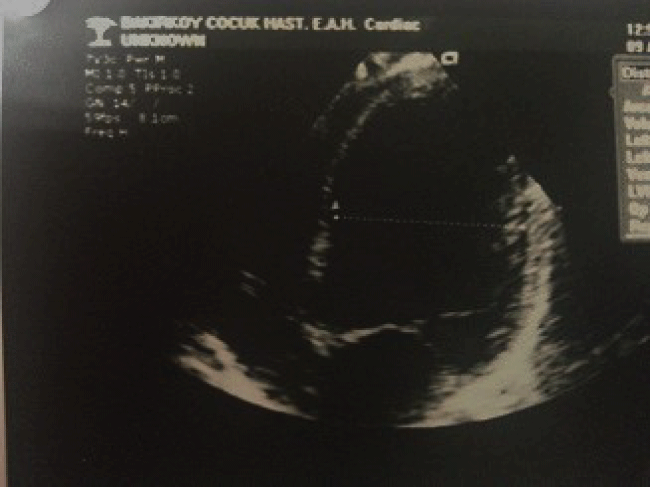
Five month-old boy who had cyanosis and respiratory difficulty was admitted to our emergency department. He was born at 38 weeks of gestational age with a birth weight of 3,850 kg and he had been exclusively breastfed. There were no medical or familial histories. He was not taking any medications or vitamin supplements. Family history was unremarkable. Immunizations were appropriate for age. On physical examination, his heart rate was 204, BP: 80/40 mmhg and capillary refill time > 2 sn were detected. The patients was intubated and transferred to PICU. There were moist ralles on both middle lung fields and chest wall retraction without cardiac murmurs. A chest X-ray showed an apparent cardiomegaly (Figure 1). An echocardiogram revealed a dilated, poorly functioning left ventricle; moderate mitral regurgitation; a shortening fraction of 16%; and an ejection fraction of 32% (Figure 2). The origin of the left coronary artery was well visualized and it appeared to be of normal size. Serum chemistries were significant for calcium of 4.1 mg/dl (normal, 7.5-10.0 mg/dl) and an ionized calcium of 0.46 mmol/L (normal, 1.0-1.3 mmol/L). Phosphorus was 5.5 mg/dl (normal, 3.2-6.3 mg/dl), albumin 3.7 mg/dl (normal, 2.8-5.0 mg/dl), and alkaline phosphatase 1907 U/L (normal, 150- 420 U/L). The patient was placed on milrinone, digoxin, furosemide, and captopril for congestive heart failure. Calcium gluconate (500 mg/ kg/day continuous IV) and vitamin D (2000IU/d) were started to correct the hypocalcemia. Hormone studies were revealed elevated parathyroid hormone (PTH) (686 pg/mL; normal 12-72 pg/mL) and decreased 25-hydroxy vitamin D (25OH2 D)( < 4 ng/mL; normal > 20 ng/mL). There were no metabolic disorders by amino acid and organic acid tests. FISH studies were negative for 22q11 deletion syndrome . A left wrist X-ray revealed mild fraying signs. His mother had a vitamin D deficiency as indicated by a decreased level of 25-hydroxy vitamin D (6.72 ng/mL). On the 5th day of the hospitalization, calcium, phosphor, and troponin T levels were 9.7 mg/dl, 5.4 mg/dl, and 0.1 (N: < 0.2 ng/ml), respectively and the patient was extubated. Ejection fraction of 51% and left ventricular dysfunction was obtained on echocardiographic examination at the same time. Anticongestive therapy and calcium replacement were continued. At a month control cardiac functions were totally normal.
Case 2
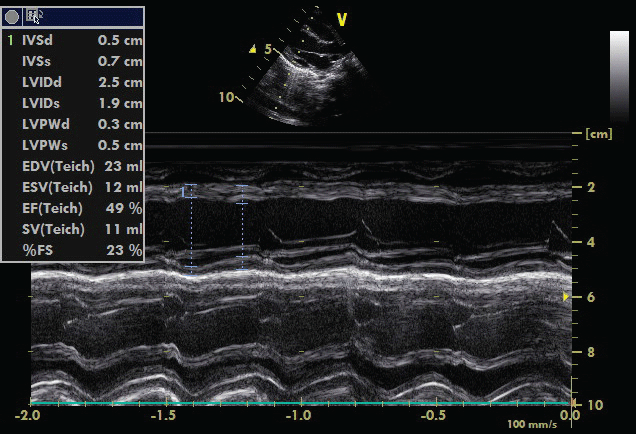
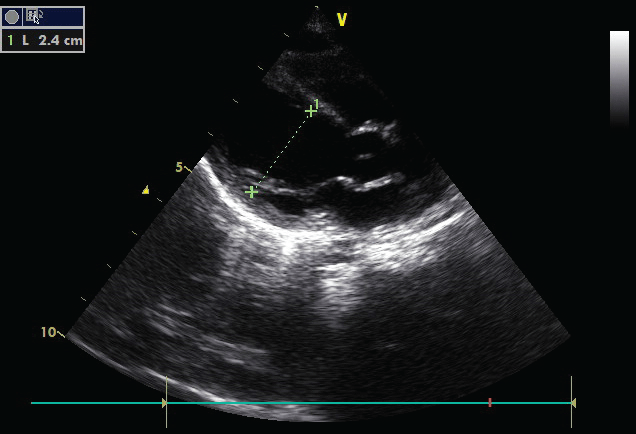
A 48-days-old male patient was referred to our clinic due to hypocalcaemia detected in another center where he had presented with complaints of cyanosis and respiratory distress. History revealed that he was the 1st child of nonconsanguineous parents, born via caesarean section at 2,390 g in week 35 of the pregnancy, has been breast-fed supplemented by formula, and receiving vitamin-D, 3 drops/day, since he was 15-days-old. Family history and physical exam were both unremarkable with the exception of tachypnea and paleness. Laboratory tests revealed: Hb: 9.1 g/dL, MCV: 96.5 fL, MCHC: 32.6 g/dL, RDW: 17.2%, WBC: 7.12 × 103/μL, HCT: 27.9%, PLT: 407 × 103/μL, ALB: 3.75 g/dL, ALP: 438 U/L, Ca: 5.82 mg/dL (9-11), P: 10.4 mg/dL (3.5-6.6), PTH: 93.92 pg/mL (15-65), 25OHD: 3.53 ng/mL and ionized Ca: 3.16 mg/dL. Therapy was initiated with Ca 50 mg/kg/day IV and vitamin-D 2,000 IU/day po. Electrocardiological assessment revealed a QTc interval of 380 ms with no pathology. Upon detection of a spheric left ventricle and EF 38% in echocardiography (Figure 3), furosemide and captopril treatments were initiated. The mother's biochemical tests obtained Ca: 9.3 mg/dL, P: 3.57 mg/dL, 25OHD: 3.0 ng/mL and PTH: 61.1 pg/mL. In addition, the patient's anemia work up revealed iron: 129 μg/dL (50-150), iron binding capacity: 239 μg/dL, and vitamin-B12: 255 pg/mL (211-946). Therefore, vitamin B12 was added to treatment at 50 μg/kg parenterally. Echocardiographic exam conducted 3 days after the initiation of therapy showed an EF of 65% (Figure 4), and a Ca value of 7.2 mg/dL, which allowed for oral calcium supplementation. After a further 1-week follow up, the Ca level was 8.78 mg/dL. The patient was discharged on current treatment and advised to return for follow up.
Discussion
Dilated cardiomyopathy in children have been well studied. The most common cause of DCM is an idiopathic etiology (> 60%), followed by familial cardiomyopathy and acute myocarditis. Other causes of DCM include viral infections, endocrine disorders and metabolic diseases. Cardio toxic drugs and systemic diseases can also cause DCM [5,6]. Calcium ions have a key role in the excitation of the cardiac muscle fibers, and reduction in serum calcium level may affect ventricular contraction [7,8]. Hypocalcemia causes decreased myocardial contractility, leading to congestive heart failure, hypotension, and angina [9]. Rickets is a metabolic disorder of the bone that develops due to in sufficient mineralization of the bone tissue and present strikingly in the skeletal system [10]. Hypocalcemia is present in the majority of patients with vitamin D deficiency rickets and may cause convulsions [4]. Consequently, it has been considered that the leading cause cardiomyopathy in patients with rickets was longstanding hypocalcemia, but the exact mechanism of cardiomyopathy has not been understood [4].
Many reports of with hypocalcemia-associated reversible heart failure and dilated cardiomyopathy have appeared in international publications. Yilmaz et al. showed that eight patients who developed dilated cardiomyopathy and congestive heart failure because of marked rickets-associated hypocalcaemia were described between 1999 and 2012 in our country [9]. Brown et al. reported four patients with signs of dilated cardiomyopathy related to rickets and congestive heart failure at the ages of 4-10 months [10]. At admission, extremely low calcium and vitamin D levels were revealed in our patients. After calcium and vitamin D replacement, abnormal findings of calcium and vitamin D were corrected rapidly with the normalization of parathyroid hormone and left ventricular function improved.
Rachitic hypocalcemic cardiomyopathy is a serious life threatening complication of infantile vitamin D deficiency rickets which is a growing community health problem, among breastfed infants born to vitamin D deficient mothers. In a study reported that maternal D vitamin status had a crucial effect on rickets development in babies [11]. Mother of our patients had very low vitamin D levels.
Although hypocalcemia secondary to vitamin D deficiency is an important cause of DCM in infants, cardiogenic shock as a presenting feature without clinical or radiological features of rickets is very rarely reported in the literature [12,13]. Kumar et al. noted that dilated cardiomyopathy and cardiogenic shock developed in a 2 month-old patient with severe hypocalcaemia as a result of vitamin D deficiency. Rickets caused a clinical picture characterised by a decline in cardiac function with progression to cardiogenic shock [1]. Our first patient had clinical, biochemical and radiological signs of rickets in conjunction with signs of cardiogenic shock secondary to severe DCM. Also, our second patient aged 48 days old is one of the youngest patients in the literature.
Paediatricians should recognize risk factors for rickets and prescribe appropriate vitamin supplementation in infants at risk. Plans for prevention by antenatal supplementation of vitamin D to pregnant mothers with 1000 -2000 IU of vitamin D3 is vital. Also, pediatric cardiologists should include hypocalcemia in the differential diagnosis of children with DCM.
References
-
Kumar M, Saikia D, Kumar V, Tomar R (2011) Vitamin D deficiency presenting with cardiogenic shock in an infant. Annal Pediatr Cardiol 4: 207-209.
-
Price DI, Stanford LC Jr, Braden DS, Ebeid MR, Smith JC (2003) Hypocalcemic rickets: An unusual cause of dilated cardiomyopathy. Pediatr Cardiol 24: 510-512.
-
Brown J, Nunez S, Russell M, Spurney C (2009) Hypocalcemic rickets and dialted cardiomyopathy: Case reports and review of literatüre. Pediatr Cardiol 30: 818-823.
-
Olgun H, Ceviz N, Ozkan B (2003) A case of dilated cardiomyopathy due to nutritional vitamin D deficiency rickets. Turk J Pediatr 45: 152-154.
-
Towbin JA, Lowe AM, Colan SD, Sleeper LA, Orav EJ, et al. (2006) Incidence, causes, and outcomes of dilated cardiomyopathy in children. JAMA 296: 1867-1876.
-
Daubeney PE, Nugent AW, Chondros P, Carlin JB, Colan SD, et al. (2006) Clinical features and outcomes of childhood dilated cardiomyopathy: Results from a national population-based study. Circulation 114: 2671-2678.
-
Tomar M, Radhakrishnan S, Shrivastava S (2010) Myocardial dysfunction due to hypocalcemia. Indian Pediatr 47: 781-783.
-
Uysal S, Kalayci AG, Baysal K (1999) Cardiac functions in children with vitamin D deficiency rickets. Pediatr Cardiol 20: 283-286.
-
NY, Laloglu F, Ceviz N, Yilmaz O, Olgun H, et al. (2015) Dilated cardiomyopathy secondary to rickets-related hypocalcemia: eight case reports and a review of the literatüre. Cardiology Young 25: 261-266.
-
Brown J, Nunez S, Russell M, Spurney C (2009) Hypocalcemic rickets and dilated cardiomyopathy: case reports and review of literature. Pediatr Cardiol 30: 818-823.
-
Andiran N, Yordam N, Ozön A (2002) Risk factors for vitamin D deficiency in breast-fed newborns and their mothers. Nutrition 18: 47-50.
-
Heird WC (2004) Vitamin deficiencies and excesses. In: Behrman RE, Kliegman RM, Jenson HB, Nelson Textbook of Pediatrics. (17th edn) WB Saunders, Philadelphia 177-190.
-
Gupta P, Tomar M, Radhakrishnan, Savitri Shrivastava (2011) Hypocalcemic cardiomyopathy presenting as cardiogenic shock. Annal Pediatr Cardiol 4: 152-155.