International Journal of Clinical Cardiology
Screening for Familial Hypercholesterolemia: West and North Zone in Manaus-Amazonas
Marco A Trujillo1*, Haydee M Carmona2 and Jorge T Mendoza3
1Internal Medicine, Serviços Municipais de Saúde, Brazil
2Cardiology Division, Regional Hospital, Instituto Mexicano Seguro Social IMSS, México
3Generalist Training in Genetics, ISSEMYM, Centro Medico Oncologico, México
*Corresponding author: Marco A Trujillo, Internal Medicine, SEMSA (Serviços Municipais de Saúde), DISA (Distrito Saúde-OESTE), Amazonas, Brazil, E-mail: citalini@hotmail.com
Int J Clin Cardiol, IJCC-4-091, (Volume 4, Issue 1), Clinical Prospective Article; ISSN: 2378-2951
Received: June 23, 2016 | Accepted: February 20, 2017 | Published: February 23, 2017
Citation: Trujillo MA, Carmona HM, Mendoza JT (2017) Screening for Familial Hypercholesterolemia: West and North Zone in Manaus-Amazonas. Int J Clin Cardiol 4:091. 10.23937/2378-2951/1410091
Copyright: © 2017 Trujillo MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: The Familial hypercholesterolemia (FH), is defined by LDL-c since 150 mg/ml (4.0 mmol/L) or more and Total Cholesterol 300 mg/ml or more, it is an inherited disease of two types, estimated frequency 1:400, for heterozygotes (He) and 1:1,000,000 homozygotes (Ho) we did the detection in general population, using the Dutch Lipid Register Network.
Methods: In the city Manaus, Amazonas, with the Dutch Lipid Register Network. Were analyzed 1294 lipid profiles, of the North and West zone of city, neither with DMII, between June 2014 and March 2015, from people aged range 18 to 77 years old. Whose clinical history of familial cardiovascular disease (CVD) was wondered.
Outcomes: Incidence of 1:45, without genetics study just applying the Dutch, Lipid Register Network, average Cholesterol total 297 mg/ml, (7.78 mmO/L), LDL-C.199 mg/ml (5.13 mmO/L), HDLc.58 mg/ml and Positive Familial History for CVD.
Conclusions: FH is important to improve the efforts in medical staff and prevent disease of heart attack in the stage early. Without cost just reviewed, laboratory studies of routine considered, of course, those results aren´t definitive or conclusive, later the genetic test can be done to confirm the FH.
Keywords
Familial hypercholesterolemia, Dyslipidemia, Atherosclerosis, LDL-C Dutch Lipid Register Network
Introduction
Familial Hypercholesterolemia is a disorder, characterized of high levels of LDL-C, since 155 mg (4.0 mmo/L)/ml serum plus total cholesterol of ≥ 300 mg/ml, which is transmitted from parents to children, i.e., hereditary Familial hypercholesterolemia is a genetic disorder caused by a defect on chromosome 19, is transmitted with an autosomal dominant trait that is only needed for a parent with the anomaly, if one is alone, heterozygous (He) with an estimated prevalence 1:400 in the general population and if both parents are homozygous (Ho) involvement is with an even lower prevalence (rare) of 1:1 million the condition begins at birth and can cause heart attacks at an early age [1-4]. A strong familial history for premature cardiovascular disease (CAD) contributes to a patients risk coronary heart disease, however only less that 10% can be attributed to FH [5,6]. The genetic basis of FH was first demonstrated as a important risk factor for CAD in 1961 [7] and later the lipoproteins were involved as a factor of development in atherosclerosis [8]. The responsible for transport of cholesterol, are LDL 80% and HDL (20%), approximately, cholesterol is brought to the liver [9], the mobility of cholesterol is carried by LDL-C, that is why what are considered atherogenic, because in them rests the highest percentage of cholesterol uptake which is a process performed through cellular receptors and finally captured by the cell through endocitosis. The most important part is LDL-C meet condition is your receptor has a responsible mutation for 80% or more of the abnormalities, the LDLR receptor (low-density lipoprotein cholesterol) is a glycoprotein of 839 amino acids and bonded to at least two proteins, apolipoprotein B100 (Apo B) and apolipoprotein E (Apo E) .The gene mutations causing LDLr and FH are often divided into 5 types, due to the functional part affected [2,10], and are:
• Mutation type 1 is the most common and it has null alleles, the messenger RNA (mRNA) is not functional [10].
• Mutation type 2 with complete or partial blockage in the process of transport. Here they have defective alleles for transportation [10].
• Mutation type 3 alleles have faulty, lacking the capacity to bind to LDL particles.
• Mutation type 4 alleles are faulty for entry of cholesterol into the cell.
• Mutation type 5 alleles are faulty at the recycling stage of the process.
Frequency
The countries which have implemented detection program for FH like the Netherlands (Holland), Spain, UK, USA. In the Caucasian population is approximately 1/500 (0.20%) [10], based on presenting the survivors of heart attacks in the US and being similar to that described in other countries: Norway, Hungary [11]. Sometimes the frequency, heterozygote is much higher than 1/500, to 1:250 (J Biomedical Science 2016), seems to be due to the proximity of inbreeding. Brazil 2015 public a study done in Sao Paulo, but in Caucasian and Lebanese population and Which could explain why some mutations caused FH patients [12]. The high frequency FH, as described in French Canadians [13], Finland [14] South African of Dutch origin Tunisia [7] Iceland [15] and Ashkenazi Jews of South Africa [16]. Moreover, where populations are genetically heterogeneous, as Spain, studies show no mutation at high prevalence among affected subjects of HF. As Canadians, Finns and Jews already mentioned [5,17-19].
Netherlands (Netherlands) has a system, possibly the best detection, study and treatment of familial hypercholesterolemia, (Lipid Clinic Network), currently a genetic study almost 50% of the population studied [5,19,20] program beginning in 1999. United Kingdom: it states that 10% of the patients with FH premature death can be avoided resulting in a cost reduction of 9 usd million/year with lipid lowering treatment to prevent coronary events, and treat family, to avoid FH-related events in early age. Spain: 4000 people that were detected approximately 20% corresponding to FH, and of these roughly 60% involved with clinical data in accordance with published Mata, et al. [18,19] in this country, despite the gratuity of statins, has a 25% were unaware that they had HF finally study the genetic mutation in the genes (PCSK 9) propotein convertase subtilisin Kexin type 9. From Apo B and LDL receptor gene (LDLR) the latter the being most common [14,21]. In the Dutch Clinic Lipid Network Database for diagnosis of FH is not strict criterion.
Familial Hypercholesterolemia: Detection
Detection of familial hypercholesterolemia (FH), was by Brown & Goldstein, Nobel Prize in Medicine (1985) [3,22]. The physical findings such as palpebral xanthomas, corneal arch. Unfortunately, the presence of sensitivity, of corneal arch may present in individuals without dyslipidemia, the positive index case is just 5-10% [23]. So the relevance of the genetic tests is also not sensitive, but yes highly specific. Unfortunately FH is not recognized as a formal pathology by the World Health Organization (WHO) with current classification of diseases [24]. The relation of genetics test with case-index is poor the UK is a good example of the low profitability of incidence FH case-index [23]. The publications show that FH patients without clinical coronary disease involvement and under treatment with statins reduce coronary risk in a very important way, around 80% with what your risk of coronary involvement is similar to that of the general population [25], which emphasizes the detection basic standards early detection [25-28].
The special value because of its high detection of the patients who could be positive for FH with the application of a very useful tool in clinical practice as has proven to be the use of the Dutch Lipid Network Database (DLND).
The high cholesterol levels do not lead to specific symptoms immediately, some types of hypercholesterolemia could has specific physical findings such the presence of xanthomas (cholesterol deposition in the skin or tendons), xanthelasma eyelids (deposits around the eyelids). Hypercholesterolemia leads to accelerated atherosclerosis in people younger than 40 years, Sometimes it is a symptom such as dizziness, lightheadedness, tinnitus, the common thing is often dizziness, this can be due to the high serum cholesterol level and the difficulty that causes for the control of the body to walk, to stand or movements such as getting up from bed, sitting, turning the head or orthostatic-like data, as changing the body position, it might be necessary to carry out indicated studies. By the primary care physician to evaluate the presence of alterations in serum levels of lipids, in this case cholesterol.
Material and Methods
FH clinical criterions
Prospective longitudinal study with cross section in the north, in the Balbina Mestrinho clinic and West area in the Damasceno Lindalva clinic, Annex 0-47, between periods March 2014 to July 2015 in the City Manaus, Amazonas. Patients were informed, and were solicited consent of study and use of data, were informed the authorities of local health the kind study and was authorized, the lipid profile performed done as part of his studies of screening for patients with, hypertension, metabolic syndrome or healthy patients. 1294 laboratory tests performed on adults of both sexes with age range of 16-94 years of age were reviewed, being 763 in the north area and 531 in western area. The Dutch Lipid Network Database, for who have > 4.0 mmol/L of LDL cholesterol was. Patients with DM, II, Arterial Hypertension, Renal, Thyroid, HIV/AIDS patients treated with antiretroviral drugs were excluded.
Inclusion criteria
1. Criteria Dutch Lipid-Clinic Network [29]
2. Sérum Cholesterol ≥ 300 mg/dl. (7.72 mmO/ L)
3. LDL-C ≥ 155 mg/dl (4.07mOs/L)
4. HDL-C Normal ≥ 45 mg/ml-in men and 40 mg/ml in women
5. Corneal Arch before 45 years of age
6. Presence of tendon xanthomas
7. Genetic Testing Cr 19p [29]
LDLR-C (mutation (PCSK 9) propotein convertase subtilisin Kexin type 9 Apo B) present in any of its five identified type [10,14,21]. Stata Statistical Program 2.0.Metodo.
Exclusion criteria
Chronic renal failure, nephrotic syndrome, intake of antiretroviral drugs [30].
Results
Men 13, Women 11 Age 48 (range 31-77 years), systemic arterial hypertension Comorbidities 5, Diabetes Mellitus II 3, for pooled 95%, Chi2 9. IC with p ≤ 0.016 Lipid Clinic Network (LCN) (Table 1). Certainty 6/23, 4/23 Probable, Possible 13/23. Average Total Cholesterol 297 mg/ml, (7.78 mmO/L), LDLC 199 mg/ml 5.23 mmO/L), HDLc 0.58 mg/ml (Figure 1). In the area North 13 with total cholesterol values greater than 300 mg/dl (range 302- 470), and LDL cholesterol values greater than 170. In the western area with values of total cholesterol ranges 290-360) 11, and 170 LDLC ≥ mg/dl, diagnosing Score, (Table 2). The gender frequency ratio male: female were of 1.3:1, more in men 1:56 frequency in our study.
.
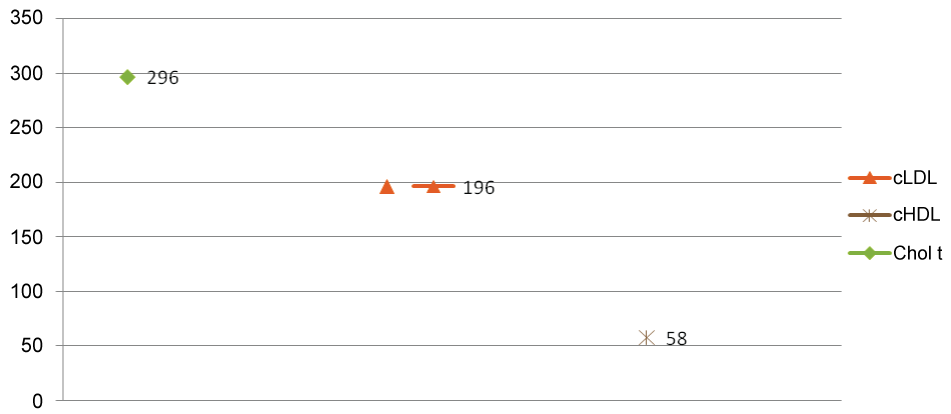
Figure 1: Average of lipid profile LDL-c (Cohort).
Averages of Cholt 297 mg/ml, (7.78 mmol/L); c LDL196 mg/ml, (5.15 mmol(L); c HDL 58 mg/ml, (1.52 mmol/L) SEMSA Manaus.
(Cholt = Cholesterol total; c-LDL = Cholesterol LDL; c-HDL= High Density Lipoprotein Cholesterol).
View Figure 1
![]()
Table 1: Plasma lipid and lipoprotein concentrations (Cohort).
View Table 1
![]()
Table 2: Diagnostic criteria for diagnosing heterozygous familial hypercholesterolemia.
View Table 2
Analysis
The results show a higher prevalence than expected i.e., 1:56 (reported or expected 1:400), data from genetic testing is not possible in Amazonas, and it lacks the means to that. Nevertheless, clinically in accordance with DLCN, the data show a considerable number of patients with probably FH. The 42% of positive with criteria for true diagnosis. Of course, the applicable genetic studies should be done, and I hope other groups will continue these trials. Therefore making workshops for primary care physicians and medical continuing education especially in the area of nutrition for dissemination in their coverage area.
Brazil has not program in this area for the Amazon region specific to detecting FH This use DLND program would first perform by stratify as first step the clinical suspicion based on evidence and then make the diagnosis of certainty, with genetic tests. The characteristics of Amerindian and its black population that are predominant in this region of Brazil with 2 million inhabitants in its capital, Manaus, are of public health interest to determine the prevalence of FH real and to know what the is the prevalence.
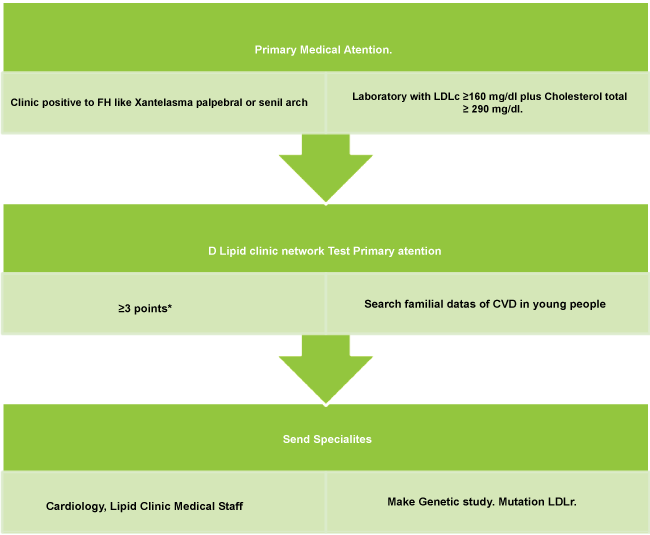
The primary health care level is ideal and important for primary detection of diseases and opportune treatment (Figure 2). In this cases of FH, the measures for primary care could be the recommended changes in their lifestyle, like eating less beef, chicken, pork and lamb. Replaced or modified foods high in saturate fat, dairy products by low-fat products. Eliminate Tran’s fats from food. To reduce the amount of cholesterol eliminating egg yolks and red meats. Do mild to moderate exercise with walking at least 30 minutes a day, another important advices: Pharmacotherapy Statins are very effective. These drugs help reduce the risk of heart attack or stroke in appropriate doses and time required, to monitor side effects possible. Ezetimiba [6,31] is another alternative for treating hypercholesterolemia, alone or combined Currently due to explosion of overweight and obesity not only in developed countries and developing have done a lot of studies such as the lipid profile, are infrequent however, its correct detection and interpretation at the primary level of care is still very poor. The limitations in this section are different according to published studies and may include detection PCP scarce, extension studies the patient and family are practically nil, reflected with little reference to lipid clinics. Most patients without adequate or suboptimal treatment with statins, uncontrolled studies of enzymes to look for the presence of myopathies, Therapy with combined Antilipemics are small number of did treatment and not always correct [32].
.
Figure 2: Basic way of screening of familial hypercholesterolemia.
*Dutch Lipid Network Database.
View Figure 2
The participation of specialist clinical lipid area is very limited, the existing number of professional and geographical distribution are serious limitations by not be uniforms his cover, related to the country’s reality. In countries with higher health, coverage has lipid specialist only 10-15% these patients are treated by physician in Lipids, as UK recognizes, In Brazil the frequency is not known. The detection of the disease and treatment when target organ damage, involves higher costs of treatment, rehabilitation and lost productivity days, the Unified Health System (SUS), (For its acronym in Portuguese) making efforts to bring primary care to underserved areas.
Is possible to get decrease the likelihood of any complications in the quality of life. Undoubtedly, it requires studies greater coverage and initially must determine who meet criteria for probability studies and certainty and according to Dutch Lipid Clinic Network.
Network database
The clinical data are essential and thus largely eliminate unnecessary costs, it is here, that we believe that our study is valuable and of interest in public health. A diagnosis to know to be treated and how, since the absence of diagnosis has immediate consequences on the quality and quantity of life, in addition to increasing health costs now so involved in public health is always desirable.
Because knowing that the number of patients have scores greater than 5 in the DLCN Score, allows us a selection of FH suspects (Table 2), the probability of a disease with easy to detect data and later to do molecular diagnosis, which are not possible to implement in all locality. The strength of this type of studies is the detection of cardiovascular risk factors that affect family death globally, since this disease, which is autosomal dominant, not only has monogenic traits, The ability and ability to detect as early as possible. The FH has implications not only medical, also social and obviously economic. With benefits in morbidity and mortality rates, lost productive years and, of course, a public health impact in summary form. Identification of FH is primarily byclinical diagnosis with subsequent confirmation by genetic testing where posible.
Conflicts of Interest
We haven't Disclosure of Potential Conflicts of Interest.
References
-
Ose L (2002) Muller-Harbitz disease-familial hypercholesterolemia. Tidsskr Nor Laegeforen 122: 924-925.
-
Defesche J (2001) World Health Organization report on familial hypercholesterolemia. Atherosclerosis 154: 242.
-
Brown MS, Goldstein JL (1986) A receptor-mediated pathway for cholesterol homeostasis. Science 232: 34-47.
-
Robert A Hegele (2009) Plasma Lipoproteins: genetic influences and clinical implications. Nature Reviews Genetics 10: 109-121.
-
Pedro Mata, Rodrigo Alonso, y Francisco Perez-Jimenez (2014) Detección de la hipercolesterolemia familiar: un modelo de medicina Preventiva. Rev Esp Cardiol.
-
Gagne C, Bays HE, Weiss SR, Mata P, Quinto K, et al. (2002) Efficacy and safety of ezetimibe added to ongoing statin therapy for treatment of patients with primary hypercholesterolemia. Am J Cardiol 90: 1084-1091.
-
Seftel HC, Baker SG, Sandler MP, Forman MB, Joffe BI, et al. (1980) A host of hypercholesterolaemic homozygotes in South Africa. Br Med J 281: 633-636.
-
Slimane MN, Pousse H, Maatoug F, Hammami M, Ben Farhat MH (1993) Phenotypic expression of familial hypercholesterolaemia in central and southern Tunisia. Atherosclerosis 104: 153-158.
-
Goldstein JL, Brown MS, Anderson RGW, Russell DW, Schneider WJ (1985) Receptor-mediatedendocytosis: Conceptsemergingfromthe LDL receptor system. Annu Rev Cell Biol 1: 1-39.
-
Atienza G (2006) Hipercolesterolemia familiar: evaluación del diagnóstico genético mediante micromatrices de ADN. Consultas Técnicas.
-
Kalina A, Csaszar A, Czeizel AE, Romics L, Szaboki F, et al. (2001) Frequency of the R3500Q mutation of the apolipoprotein B-100 gene in a sample screened clinically for familial hypercholesterolemia in Hungary. Atherosclerosis 154: 247-251.
-
Raul D Santos (2016) HomozygousFamilialHypercholesterolemia: phenotype rules! Atherosclerosis 248: 252-254.
-
Moorjani S, Roy M, Gagne C, Davignon J, Brun D, et al. (1989) Homozygous familial hypercholesterolemia among French Canadians in Quebec Province. Arteriosclerosis 9: 211-216.
-
Yajnavalka Banerjee, Khalid Al-Rasadi, Khalid Al-Waili, Hilal Ali Al-Sabti, Ali Al-Hinai, et al. (2014) Criteria for Diagnosis of Familial Hypercholesterolemia: A Comprehensive Analysis of the Different Guidelines, Appraising their Suitability in the Omani Arab Population. Oman Med J 29: 85-91.
-
Rubinsztein DC, van der Westhuyzen DR, Coetzee GA (1994) Monogenic primary hypercholesterolaemia in South Africa. S Afr Med J 84: 339-344.
-
Seftel HC, Baker SG, Jenkins T, Mendelsohn D (1989) Prevalence of familial hypercholesterolemia in Johannesburg Jews. Am J Med Genet 34: 545-547.
-
Mata P, Alonso R, Castillo S, Pocovi M, Spanish Group of Familial Hypercholesterolemia (2002) MEDPED and the Spanish Familial Hypercholesterolemia Foundation. Atheroscler Suppl 2: 9-11.
-
Alonso R, Mata N, Castillo S, Fuentes F, Saenz P, et al. (2008) Cardiovascular disease in familial hypercholesterolaemia: influence of low-density lipoprotein receptor mutation type and classic risk factors. Atherosclerosis 200: 315-321.
-
Simon Broome Register Group (1991) Risk of fatal coronary heart disease in familial hypercholesterolaemia. BMJ 303: 893-896.
-
Umans-Eckenhausen MA, Defesche JC, Sijbrands EJ, Scheerder RL, Kastelein JJ (2001) Review of first 5 years of screening for familial hyercholesterolemia in the Netherlands. Lancet 357: 165-168.
-
Cohen JC, Boerwinkle E, Mosley TH, Hobbs HH (2006) Sequence variations in PCSK9, low LDL, and protection against coronary heart disease. N Engl J Med 354: 1264-1272.
-
Brown MS, Goldstein JL (1984) How LDL Receptors Influence Cholesterol and Atherosclerosis. Sci Am 251: 58-66.
-
Emily S van Aalst-Cohen, Angelique CM Jansen, Michael WT Tanck, Joep C Defesche, Mieke D Trip, et al. (2006) Diagnosing familial hypercholesterolaemia: the relevance of genetic testing. Eur Heart J 27: 2240-2246.
-
Goldstein JL, Schrott HG, Hazzard WR, Bierman EL, Motulsky AG (1973) Hyperlipidemia in coronary heart disease II. Genetic analysis of lipid levels in 176 families and delineation of a new inherited disorder, combined hyperlipidemia. J Clin Invest 52: 1544-1568.
-
Hamrefors V, Orho-Melander M, Krauss RM, Hedblad B, Almgren P, et al. (2009) A gene score of nine LDL and HDL regulating genes is associated with fluvastatin induced cholesterol changes in women. J Lipid Res 51: 625-634.
-
Defesche JC (2010) Defining the challenges of FH screening for familial hypercholesterolaemia. J Clin Lipidol 4: 338-341.
-
Gotto AM Jr (2002) Management of dyslipidemia. Am J Med 112: 10S-18S.
-
Defesche J (2000) Familial Hypercholesterolemia. In: Betteridge J, Lipids and vascular disease. London: Martin Dunitz 6: 65-76.
-
Nordestgaard BG, Chapman MJ, Humphries SE, Ginsberg HN, Masana L, et al. (2013) Familial hypercholesterolaemia is underdiagnosed and undertreated in the general population: guidance for clinicians to prevent coronary heart disease. Eur Heart J 34: 3478a-3490a.
-
Stone NJ (1994) Secondary causes of hyperlipidemia. Med Clin North Am 78: 117-141.
-
Ballantyne CM, Abate N, Yuan Z, King TR, Palmisano J (2005) Dose-comparison study of the combination of ezetimibe and simvastatin (Vytorin) versus atorvastatin in patients with hypercholesterolemia: the Vytorin Versus Atorvastatin (VYVA) study. Am Heart J 149: 464-473.
-
Ziajka PE, Reis M, Kreul S, King H (2004) Initial low-density lipoprotein response to statin therapy predicts subsequent low-density lipoprotein response to the addition of ezetimibe. Am J Cardiol 93: 779-780.





