International Journal of Oral and Dental Health
Assessment of Dentofacial Effects of Lower Incisor Versus 4 Premolar Extractions
Burçak Kaya1*, Ömür Polat-Özsoy1, Seda Erken2 and Faik Serhat Özsoy3
1Department of Orthodontics, Faculty of Dentistry, Baskent University, Ankara, Turkey
2Private Practice, Sakarya, Turkey
3Private Practice, Ankara, Turkey
*Corresponding author: Dr. Burcak Kaya, Associate Professor, Department of Orthodontics, Faculty of Dentistry, Baskent University, 1. Cad No: 107, 06490 Bahcelievler-Ankara, Turkey, Tel: +90 312 215 13 36, Fax: +90 312 215 29 62, E-mail: burcak_kaya@hotmail.com
Int J Oral Dent Health, IJODH-1-021, (Volume 1, Issue 4), Original Research; ISSN: 2469-5734
Received: October 20, 2015 | Accepted: November 16, 2015 | Published: November 25, 2015
Citation: Kaya B, Polat-Özsoy Ö, Erken S, Özsoy FS (2015) Assessment of Dentofacial Effects of Lower Incisor Versus 4 Premolar Extractions. Int J Oral Dent Health 1:021. 10.23937/2469-5734/1510021
Copyright: © 2015 Kaya B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objectives: To examine the dentofacial effects of orthodontic treatment with 1 lower incisor extraction in comparison with 4 premolar extractions.
Materials and Methods: Among 32 patients showing Class I malocclusion, 16 patients with a mean age of 22.0 ± 4.6 years and treated with 1 lower incisor extraction were included in the first group. 16 patients with a mean age of 18.4 ± 3.4 years and treated with 4 first premolar extractions were included in the second group. The pretreatment and post treatment lateral cephalograms were analyzed.
Results: SNGoGn angle increased in the first group, decreased in the second group and significant difference (p ≤ 0.05) was found between the groups. L1-NB distance (p ≤ 0.01), L1/NB (p ≤ 0.01) angle and L1/MP (p ≤ 0.05) angle showed significant decreases in the second group. The differences between the groups were significant for all parameters related with lower incisors. Upper and lower lips retruded in both groups.
Conclusion: Lower incisor extraction can be an alternative to 4 premolar extractions when little dental arch changes and localized treatment effects are desired.
Introduction
Tooth extraction is often preferred to obtain a satisfying functional and esthetic result in orthodontic treatment and its effects on dentofacial structures has been searched for years [1-4]. Until the late 50's the term extraction almost meant the removal of all four first premolars. Later, alternative extraction sequences such as upper and lower second premolars or second premolars from one arch and first premolars from the other were accepted [5]. However, the concern about the esthetic outcomes of premolar extractions remains fashionable, for both the professionals and the community [1,3,4,6-14].
Lower incisor extraction is a treatment option which gives clinician the direct intervention opportunity to the problematic area in patients with mandibular anterior crowding. However, it is not popular in the orthodontic practice despite the evident advantages [15,16]. Oppositions to this alternative treatment method with a different extraction option are based on clinical observations instead of scientific evidence [15-21].
There are a good number of researches examining the effects of orthodontic treatment involving premolar extractions with different extraction sequences [1-14]. However, there isn't sufficient number of researches examining the effects of lower incisor extraction. Thus, the aim of this study is to investigate the skeletal, dental and soft tissue changes that occur due to orthodontic treatment with 1 lower incisor extraction and compare it with 4 first premolar extractions.
Materials and Methods
This study was organized retrospectively as a parallel group design with 1:1 ratio between the groups. A power analysis was performed to calculate the sample size required for the study. The power analysis revealed that a total sample size of 30 (15 per group) was needed to detect clinically meaningful differences between the groups with a power of 80% at 0.05 significance level. Sample size estimation was performed by using NCSS (Number Cruncher Statistical Systems. Kaysville, Utah, USA. Version 2001) and PASS (Power Analysis and Sample Size, Kaysville, Utah, USA. Version 2000) software. Hence, the sample of this retrospective study consisted of 32 patients (18 females, 14 males) in permanent dentition stage, who received orthodontic treatment in Baskent University faculty of dentistry department of orthodontics with 0.018 × 0.022 inch slot edge-wise appliances. The inclusion criteria are shown below:
1) Presence and eruption of all permanent teeth,
2) No existence of supernumerary teeth,
3) Presence of Angle Class I malocclusion with moderate crowding,
4) Existence of Bolton excess in the lower anterior teeth,
5) Disuse of any intraoral or extra oral anchorage reinforcement mechanics, except for vertical intermaxillary elastics at finishing stage.
16 patients (9 females, 7 males) with a mean age of 20.0 ± 4.6 years and treated with 1 mandibular incisor extraction were selected randomly and included in the first group. 16 patients (9 females, 7 males) with a mean age of 19.4 ± 3.4 years which were selected randomly within a group matched for age, gender, dentoskeletal characteristics and treated with 4 first premolar extractions requiring moderate anchorage mechanics were included in the second group. The study was approved by Baskent University research and review board. All patients and parents were informed that the material obtained would be used for research studies and signed a consent form.
Cephalometric analysis
The lateral cephalometric radiographs of each patient were taken at the beginning and end of orthodontic treatment with a Planmeca cephalometer (PM 2002 EC; Proline, Helsinki, Finland). All the pretreatment (T0) and post treatment (T1) digital lateral cephalometric radiographs obtained from these patients were analyzed by the same examiner (BK) using VistaDent OC cephalometric software (VistaDent OC 1.1; GAC International Inc, Bohemia, New York, USA). A total of 20 parameters (8 skeletal, 10 dental, 2 soft tissue) were measured and evaluated (Figure 1).
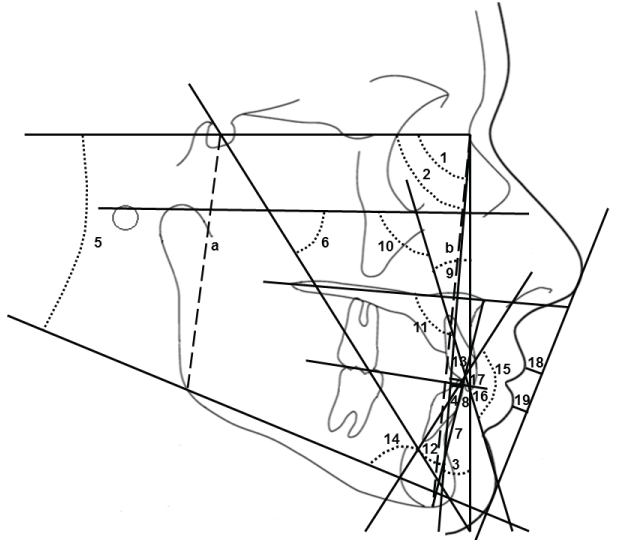
.
Figure 1: 1: SNA°, 2: SNB°, 3: ANB°, 4: Witts mm, 5: SNGoGn°, 6: Yaxis°, 7: ANSMe mm, 8: U1NA mm, 9: U1NA°, 10: U1FH°, 11: 1PP°, 12: L1NB°, 13: L1NB mm, 14:IMPA°, 15: Interincisal°, 16: Overjet, 17: Overbite, 18: ULipE mm, 19: LLipE mm, a/b: Jarabak% (Ratio).
View Figure 1
Statistical analysis
Data analysis was performed by using SPSS for Windows, version 11.5 (SPSS Inc., Chicago, IL, United States). The normality of distribution of the continuous variables was determined by using Shapiro Wilk test. Descriptive statistics were shown as mean ± standard deviation for continuous variables. The mean differences between pre-treatment and post-treatment measurements within the groups were analyzed by Bonferroni Adjusted Paired Samples t-test for normally distributed variables and by Bonferroni Adjusted Wilcoxon's signed test for not normally distributed variables. A p value less than 0.025 was considered statistically significant. The mean treatment changes obtained in the groups were compared by student's t-test for normally distributed variables and by Mann Whitney U-test for not normally distributed variables. A p-value less than 0.05 was considered statistically significant.
Method error
3 weeks after the first measurements, 22 lateral cephalometric films from 11 randomly selected patients were repeated by the same examiner (BK). Intra-class correlation coefficients (r) were calculated on pre-treatment and post-treatment cephalometric films for evaluation of reliability. 95 % confidence intervals were considered statistically reliable and the intra-class correlation coefficients (r) calculated for each variable ranged between these limits.
Results
The study groups consisted of very similar patients, since none of the parameters showed significant difference between the groups at T0 (Table 1, Table 2, Table 3 and Table 4). Orthodontic treatment was completed with a mean of 18.3 ± 4.2 months in the first group and with a mean of 25.0 ± 5.6 months in the second group. The difference between the groups was significant (p ≤ 0.01) for treatment time (Table 1).
![]()
Table 1: Demographic assessment of the sample.
View Table 1
At the end of treatment, significant sagittal skeletal changes were not observed in either group. ANS-Me distance increased significantly in both groups but the increase was much prominent in the first group. SNGoGn angle showed a slight increase in the first group, a slight decrease in the second group and significant difference was found between the groups. Jarabak ratio didn't change significantly in the first group, increased significantly in the second group and showed a significant difference between the groups (Table 3).
![]()
Table 2: Dental cast comparisons between the groups.
View Table 2
![]()
Table 3: Skeletal cephalometric comparisons within and between the groups.
View Table 3
No significant changes were observed at the upper incisors in either group. L1-NB distance, L1/NB angle and L1/MP angle showed non-significant increases in the first group and significant decreases in the second group. For all the parameters related with lower incisors, the differences between the groups were significant (Table 4).
![]()
Table 4: Dental and soft tissue cephalometric comparisons within and between the groups.
View Table 4
Interincisal angle showed a non-significant decrease in the first group and a non-significant increase in the second group, but no significant differences were found between the groups. Overjet and overbite remained statistically unchanged in either group with no significant differences between the groups (Table 4).
Upper and lower lips significantly retruded in both groups, with a much prominent retrusion in the second group. No significant differences were found between the groups for the measurements related with upper and lower lips (Table 4).
Discussion
Today, lower incisor extraction is still not a common treatment option in the orthodontic field. It is supposed that undesirable side-effects occur as a result of lower incisor extraction such as increases in overjet and overbite, unsatisfactory posterior occlusion, recurrence of crowding, space reopening and loss of the interdental gingival papillae in the mandibular anterior region [15-24]. However these comments have generally been supported by clinical case reports of few patients [19,21,24-30]. On the other hand, in some studies greater numbers of patients treated with lower incisor extraction were analyzed, but the patient samples were not homogenous concerning malocclusion characteristics [15,17,20,23]. However, in our study both groups were homogenous since all patients had started orthodontic treatment with Angle Class I malocclusion in addition to similar age and gender distribution.
In this study it was intended to evaluate the overall dentofacial outcome of orthodontic treatment with 1 lower incisor extraction and to compare it with the most common mechanics preferred in anterior crowding cases. Therefore, 4 first premolar extraction sequence was used for the comparisons. In addition, moderate anchorage requirement was defined as the prerequisite, since the premolar extraction spaces would be used for alignment of the anterior segment rather than maximum retraction. Hence, the treatment method applied in the second group of the study was chosen with an attempt to substitute 1 lower incisor extraction with dentofacial effects in patients with similar characteristics.
No significant sagittal skeletal change was observed in either groups and no difference was found between the groups. This is clearly due to avoiding heavy orthopedic forces and marked retraction of the upper anterior teeth in both groups.
The vertical changes were evidently different between the groups. The prominent increase in the lower anterior facial height and SNGoGn angle accompanied by the decrease of Jarabak ratio are the signs of posterior rotation in the first group. The differences observed between the groups in vertical skeletal parameters can be explained with the anterior rotation effect of premolar extractions. It is known that extraction of posterior teeth from each quadrant which results with mesialization of the teeth distal to the extraction sites causes mandibular anterior rotation or at least control of the lower anterior vertical dimension of the face. On the contrary, treatments without extraction usually result with increase in the lower anterior facial height and posterior rotation [31]. In the first group of our study 1 lower incisor extraction helped gaining space in the mandibular anterior segment, but didn't have any vertical control effect on the dentofacial structures.
The small movements observed at the upper incisors can be explained with the extraction protocol. In the first group, the upper incisors slightly proclined as there were mild-to-moderate arch length discrepancy and no tooth extractions in the upper arch. In the second group, non-significant retroclination was observed at the upper incisors due to bilateral upper first premolar extractions and the use of extraction spaces only for alignment rather than retraction by using moderate anchorage mechanics.
The non-significant proclination observed at the lower incisors in the first group can be explained with inadequacy of the extraction space of lower incisor teeth for eliminating the arch length discrepancy. Hence, the lower anterior teeth were forced to procline for increasing the arch length to align. This finding is similar with the study of Riedel et al. [20] which mandibular incisors proclined 3.5° and moved 0.56 mm anteriorly. In contrast, Faerovig and Zachrisson [16] obtained 5.9° mandibular incisor retroclination and 1.7 mm lingual movement. The mandibular incisor proclination observed in our study was 0.41° which is minor. The difference observed between the direction and amount of incisor teeth movements in these 3 studies was probably due to the difference between the malocclusions patient samples presented. The patients in the study of Riedel et al. [20] had apparent mandibular crowding whereas the ones in the study of Faerovig and Zachrisson [16] presented with Class III malocclusion with insufficient overjet. Therefore, in some patients the extraction space of the lower incisor was used for mandibular alignment and in the others it was used for retracting the remaining mandibular anterior teeth.
On the other hand, significant retroclination was observed at the lower incisors due to bilateral lower first premolar extractions in the second group of the present study. The prominent retroclination observed at the lower incisors despite using moderate anchorage mechanics can be explained with the dense structure of the mandibular bone and its resistance to the mesial movement of mandibular posterior teeth. This resistance may probably be the cause of premolar extraction spaces to be closed mostly by lingual movements of the lower anterior teeth beyond expected limits. There were significant differences between the groups for all parameters related with lower incisors which shows that the decision of whether to extract 1 lower incisor or 4 first premolars substantially effects the final position of the lower incisors.
Non-significant changes in interincisal angle caused slightly proclined anterior teeth in the first group and somewhat upright teeth in the second group. However, these small movements didn't cause a significant difference between the groups. Similarly, overjet and overbite showed non-significant increases in both groups, where no significant differences were found between the groups. Nevertheless, the changes that occurred in overjet and overbite must be evaluated in conjunction with the occlusal requirements of the patients in accordance with their maloccusions. In the study of Riedel et al. [20] the patients had increased overjet and overbite, so the aim was to reduce them. On the contrary, the patients in the study of Faeovig and Zachrisson [16] had reduced overjet and overbite, so the aim was just the opposite. In our study, the patients in both groups had overjet (4.1/2.3 mm) and overbite (2.7/0.7 mm) close to normal limits, which may be the reason of non-significant changes.
Upper and lower lips showed no significant movement in the first group and significant retrusion in the second group. This response of the soft tissues is the result of minor proclination of incisors observed in the first group and marked retrusion of incisors observed in the second group. Nevertheless, the changes that occurred in the upper and lower lips showed statistically no significant differences between the groups that can affect the clinician's decision whether to extract 1 lower incisor or 4 premolars.
The average treatment time was 18.3 months in the first group, 25.0 months in the second group and the difference between the groups was significant. The treatment times in this study were comparable with other studies in which similar treatment protocols were used [4,9,12,16]. Shorter treatment time is definitely one of the biggest advantages of any orthodontic protocol and can certainly change the clinician's choice of treatment method. On the other hand, it must be noted that problems such as lingual tilting of the lower canine crowns and narrowing of the intercanine width may increase the treatment time, hence the axial inclinations of the mandibular teeth must be displayed carefully throughout the treatment period [16].
It was emphasized that lower incisor extraction should be planned carefully with rational case selection for achieving satisfactory results by using simple treatment mechanics [19]. Some studies have suggested that in patients with severely crowded mandibular arches, removal of one or two mandibular incisors is the most reasonable choice [21,32]. It helps maintaining the arch form by preventing intercanine width increase and may increase stability of the mandibular anterior region without lifetime retention. Hence, marked lower anterior crowding or protrusion can be evaluated as indication for mandibular incisor extraction, especially when accompanied by loss of periodontal tissues at the labial surface of lower incisors [20,31]. Some authors stressed that narrow maxillary lateral incisors and some others stated that cases with Class III tendency are good candidates for lower incisor extraction, since collapse of the lower arch is required in such occasions [17,19,22,23,25,28,30]. Uribe et al. [33] emphasized that patients whose interproximal contact location is at the incisal interproximal third are at greater risk for developing an open gingival embrasure. Therefore, a realistic diagnostic set-up can be helpful in determining whether the occlusal result obtained with mandibular incisor extaction would be satisfactory and compatible with patients' requirements [19].
Conclusions
1. Skeletal effects of lower incisor extraction are similar to 4 premolar extractions, except for lack of control over the vertical facial dimension.
2. Greater lower incisor retroclination and retrusion occurs in patients treated with 4 premolar extractions compared to those treated with 1 lower incisor extraction.
3. Similar results are obtained in the facial soft tissues with both techniques.
4. Mandibular lower incisor extraction can be a conservative and practical alternative to 4 premolar extractions in cases demanding localized treatment effects and little changes in the dental arches, especially in the treatment of adult patients.
Acknowledgment
We would like to thank our biostatistician Dr. Salih Ergöcen for his contributions.
References
-
Zierhut EC, Joondeph DR, Artun J, Little RM (2000) Long-term profile changes associated with successfully treated extraction and nonextraction Class II Division 1 malocclusions. Angle Orthod 70: 208-219.
-
Bowman SJ (1999) More than lip service: facial esthetics in orthodontics. J Am Dent Assoc 130: 1173-1181.
-
Bowman SJ, Johnston LE Jr (2000) The esthetic impact of extraction and nonextraction treatments on Caucasian patients. Angle Orthod 70: 3-10.
-
Wholley CJ, Woods MG (2003) The effects of commonly prescribed premolar extraction sequences on the curvature of the upper and lower lips. Angle Orthod 73: 386-395.
-
Nance HN (1949) The removal of second premolars in orthodontic treatment. Am J Orthod 35: 685-696.
-
Bravo LA (1994) Soft tissue facial profile changes after orthodontic treatment with four premolars extracted. Angle Orthod 64: 31-42.
-
Caplan MJ, Shivapuja PK (1997) The effect of premolar extractions on the soft-tissue profile in adult African American females. Angle Orthod 67: 129-136.
-
Bishara SE, Cummins DM, Zaher AR (1997) Treatment and posttreatment changes in patients with Class II, Division 1 malocclusion after extraction and nonextraction treatment. Am J Orthod Dentofacial Orthop 111: 18-27.
-
Basciftci FA, Usumez S (2003) Effects of extraction and nonextraction treatment on class I and class II subjects. Angle Orthod 73: 36-42.
-
Stephens CK, Boley JC, Behrents RG, Alexander RG, Buschang PH (2005) Long-term profile changes in extraction and nonextraction patients. Am J Orthod Dentofacial Orthop 128: 450-457.
-
Scott Conley R, Jernigan C (2006) Soft tissue changes after upper premolar extraction in Class II camouflage therapy. Angle Orthod 76: 59-65.
-
Al-Nimri KS (2006) Vertical changes in class II division 1 malocclusion after premolar extractions. Angle Orthod 76: 52-58.
-
Hodges A, Rossouw PE, Campbell PM, Boley JC, Alexander RA, et al. (2009) Prediction of lip response to four first premolar extractions in white female adolescents and adults. Angle Orthod 79: 413-421.
-
Leonardi R, Annunziata A, Licciardello V, Barbato E (2010) Soft tissue changes following the extraction of premolars in nongrowing patients with bimaxillary protrusion. A systematic review. Angle Orthod 80: 211-216.
-
Dacre JT (1985) The long term effects of one lower incisor extraction. Eur J Orthod 7: 136-144.
-
Faerovig E, Zachrisson BU (1999) Effects of mandibular incisor extraction on anterior occlusion in adults with Class III malocclusion and reduced overbite. Am J Orthod Dentofacial Orthop 115: 113-124.
-
Richardson ME (1963) Extraction of lower incisors in orthodontic treatment planning. Dent Pract 14: 151-156.
-
Salzman J (1963) EH Angle on extraction in orthodontics. Am J Orthod 49: 464-466.
-
Kokich VG, Shapiro PA (1984) Lower incisor extraction in orthodontic treatment. Four clinical reports. Angle Orthod 54: 139-153.
-
Riedel RA, Little RM, Bui TD (1992) Mandibular incisor extraction--postretention evaluation of stability and relapse. Angle Orthod 62: 103-116.
-
Valinoti JR (1994) Mandibular incisor extraction therapy. Am J Orthod Dentofacial Orthop 105: 107-116.
-
Tuverson DL (1980) Anterior interocclusal relations. Am J Orthod 78: 361-393.
-
Canut JA (1996) Mandibular incisor extraction: indications and long-term evaluation. Eur J Orthod 18: 485-489.
-
Klein DJ (1997) The mandibular central incisor, an extraction option. Am J Orthod Dentofacial Orthop 111: 253-259.
-
Bolton WA (1958) Disharmony of tooth size and its relation to the analysis and treatment of malocclusion. Angle Orthod 28: 113-130.
-
Buchner HJ (1964) Treatment of cases with three lower incisors. Angle Orthod 34: 108-114.
-
DeAngelis V (1973) Selection of teeth for extraction as an adjunct to orthodontic treatment. J Am Dent Assoc 87: 610-615.
-
Bahreman AA (1977) Lower incisor extraction in orthodontic treatment. Am J Orthod 72: 560-567.
-
Sheridan JJ, Hastings J (1992) Air-rotor stripping and lower incisor extraction treatment. J Clin Orthod 26: 18-22.
-
Owen AH (1993) Single lower incisor extractions. J Clin Orthod 27: 153-160.
-
Chua A, Lim JYS, Lubit EC (1993) The effect of extraction versus nonextraction orthodontic treatment on the growth of the lower anterior face height. Am J Orthod Dentofacial Orthop 104: 361-368.
-
Joondeph DR, Riedel RA. Retention and relapse (1994) In: Graber TM, Vanarsdall RL Jr, (eds) Orthodontics: current principles and techniques, 2nd (edn). St. Louis: Mosby-Year Book, p. 908-950.
-
Uribe F, Holliday B, Nanda R (2011) Incidence of open gingival embrasures after mandibular incisor extractions: a clinical photographic evaluation. Am J Orthod Dentofacial Orthop 139: 49-54.





