International Journal of Oral and Dental Health
CT Imaging in Congenitally Healed Microform of Primary Cleft Palate
Dorota Cudzilo1*, Teresa Matthews-Brzozowska1,2 and Monika Bekiesinska-Figatowska3
1Department of Maxillofacial Orthopaedics and Orthodontics, Institute of Mother and Child, Kasprzaka, Poland
2Department and Clinic of Maxillofacial Orthopaedics and Orthodontics, University of Medical Sciences, Bukowska, Poland
3Department of Diagnostic Imaging, Institute of Mother and Child, Kasprzaka, Poland
*Corresponding author: Dorota Cudziło, Department of Maxillofacial Orthopaedics and Orthodontics, Institute of Mother and Child, Kasprzaka 17a, 01-211 Warsaw, Poland, Tel: +48-22-32-77-128, E-mail: dcudzilo@gmail.com
Int J Oral Dent Health, IJODH-3-040, (Volume 3, Issue 1), Case Report; ISSN: 2469-5734
Received: August 26, 2016 | Accepted: March 14, 2017 | Published: March 17, 2017
Citation: Cudzilo D, Matthews-Brzozowska T, Bekiesinska-Figatowska M (2017) CT Imaging in Congenitally Healed Microform of Primary Cleft Palate. Int J Oral Dent Health 3:040. 10.23937/2469-5734/1510040
Copyright: © 2017 Cudzilo D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Diagnostic radiology is essential in the planning of multidisciplinary treatment for cleft defects. The aim of this study is to present the merits of performing computed tomography in the case of a patient with a suspected cleft defect on the left side and its spontaneous healing in intrauterine life. This paper describes the case of a patient with a visible scar suggesting a left-sided cleft lip. Anamnestic examination ruled out any surgical correction, although the scar was already evident at birth. Intraoral examinations revealed hypodontia of a lateral incisor on the right side and hyperdontia of the lateral incisors on the left side, which is a characteristic symptom of a cleft in the primary palate. The dental status was confirmed by means of an orthopantomogram, which did not show any fissure within the bone structures. Only dental CT imaging revealed an alveolar cleft on the left side. In particular cases of congenital craniofacial defects it is advisable to broaden the scope of diagnostic radiography to include three-dimensional imaging of the maxillary bone structure.
In world literature there are isolated clinical reports relating to a spontaneous healing of cleft defects in utero, none of which contained any information on imaging examinations that could document the actual picture of the craniofacial changes accompanying the facial scar.
Introduction
The surgical correction of a unilateral cleft lip and palate leaves a noticeable scar on the face between the upper lip and the nose. Another common symptom of a cleft is hypodontia-a decreased number of teeth, or hyperdontia-supernumerary teeth [1]. Diagnostic radiology is essential in the planning of multidisciplinary treatment for cleft defects, but in the case of microform clefts which require the treatment of occlusal disorders, standard radiographic examinations including orthopantomograms and lateral cephalometric radiographs are usually performed [2].
The aim of this study is to present the merits of performing computed tomography to indicate a suspected left cleft lip/palate defects and their spontaneous healing intrauterine life.
Case Report
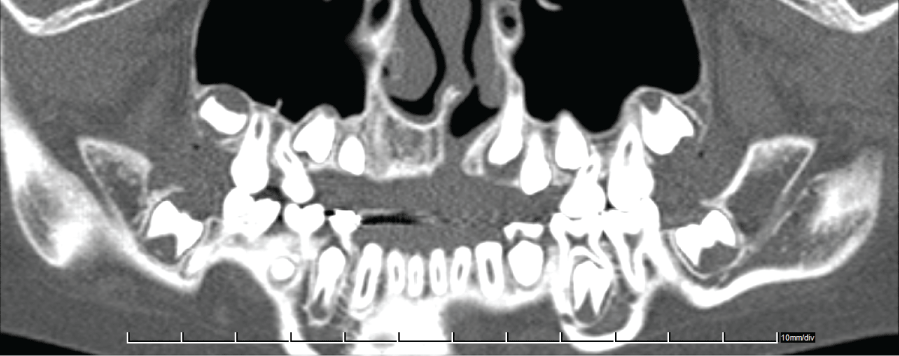
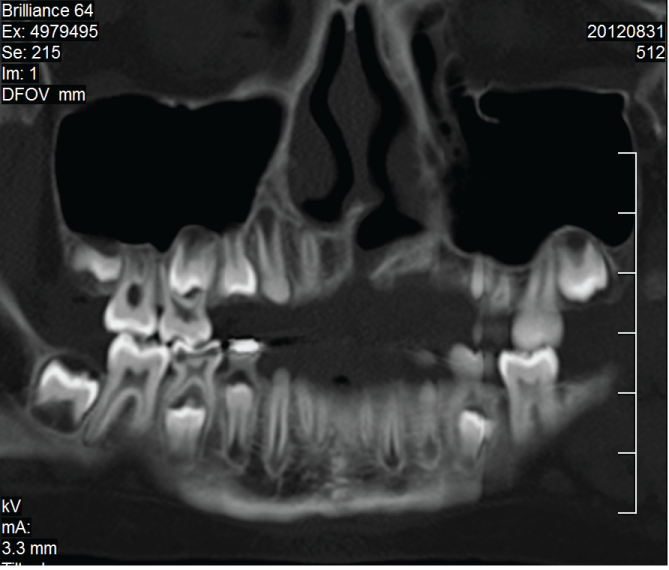
An 11-year-old patient presented to the Orthodontic Clinic with dental disorders. The patient's face had a post-operative appearance characteristic of a patient with a unilateral, cleft lip/palate, showing a vertical scar with a slight lowering of the line of the upper lip accompanied by an asymmetry of the nasal base on the left side. An anamnesis ascertained that the child had not undergone any facial surgery. Intraoral examination revealed correct occlusal relationships in the molars, hypodontia of tooth 12, and a supernumerary tooth 22. The dental status was confirmed by means of an orthopantomogram, which did not show any fissure within the bone structure. Because the lateral cephalometric radiograph did not unequivocally confirm or rule out disorders in the bone structure a CT with a 64-row scanner was performed, which revealed an alveolar cleft on the left side (Figure 1, Figure 2 and Figure 3).
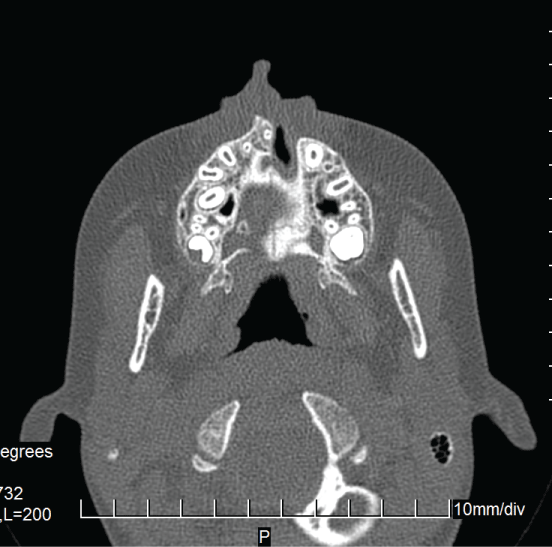
.
Figure 1: Native scan in an axial projection-crossectional image of the maxilla and partially the palate.
View Figure 1
Discussion
Embryonic craniofacial development takes place in stages. The process begins in the fourth week of gestation, when migrating neural crest cells combine with mesodermal cells to establish the facial primordial [3]. The primary palate is formed between days 28 to 38 postfertilization. It is created by fusion of the medial and lateral nasal processes and the maxillary prominence. The result is the formation of the upper lip and the area of the alveolar ridge containing the central and lateral incisors. The secondary palate closure takes place afterwards, between days 42 to 55, by fusion of the elevated palatal shelves. Interferences with the mentioned above fusions result in clefts, if occurred earlier in embryological life, will effect with cleft lip, if later - will affect the palate. If the interference appears early and is still present after primary palate development is completed, it will result with both, cleft lip and cleft palate. The pathomechanism of microform cleft lip is not clear. MCL can result from either partial failure in the mechanism of fusion of the frontonasal and maxillary processes before week seven of embryonic life or from spontaneous late foetal repair of an open cleft lip [4]. However, it seems to be confirmed, that microform cleft lip is part of the spectrum of CL/P and should be considered during clinical evaluations of families with clefts [5].
In the case of the patient described in this study, intraoral examination revealed features typical of patients with clefts who had undergone primary corrective surgery. In the interview, the parents stated that the child had not been operated on and the scar was already visible at birth [2]. Descriptions of similar cases can be found in only very few publications (based solely on photographs), as a microform cleft lip, or as a congenital healed cleft lip [6,7]. A diagnosis of a spontaneously healed cleft in utero can be made on the basis of the information obtained in a medical interview. Another indicator can be the shape of the vertical scar in the subnasal area. After corrective surgery for a cleft lip, the scar usually has a zigzag shape, depending on the incision lines and the adopted method of surgical correction [8]. In genetic studies conducted on materials obtained from patients from several countries who had been diagnosed with cleft lips or a microform clefts, numerous mutations were observed where the clinical pictures were similar; however, the occurrence of intrauterine clefts with spontaneous healings were not confirmed [5]. In the case described in this paper, we opted for a different way of proving the clinical and pathological picture. An experienced team of doctors at the Institute of Mother and Child in Warsaw, which currently treats the largest number of children with congenital clefts in Poland, could not unequivocally confirm a congenital healed cleft because such cases are extremely rare. It was therefore vital to extend the scope of diagnostic radiography in order to confirm or exclude the existence of a cleft and its spontaneous healing by including another imaging method that would complement orthopantomograms and lateral cephalometric radiographs. Two of such diagnostic methods are available in Poland as standards before orthodontic treatments are done. Both are ionizing radiation based, and they include: computed tomography (CT) and cone beam computed tomography (CBCT). The two techniques are equally good and reliable for assessing bone defects in the alveolar ridge and the palate, as well as monitoring bone grafts following surgical treatment of the defects [9]. CT images show a better signal-to-noise ratio, which means that three-dimensional reconstructions obtained by this method are more accurate than those obtained by CBCT [10]. On the other hand, it is generally believed that CBCT exposes patients to a lower dose of ionizing radiation. However, this is not entirely true as there are scanners on the market which emit smaller or larger doses depending on the field-of-view size and the type of x-ray beam (pulsed or continuous), whereas CT scanners (though not all of them) have a dose reduction function. Thus, the choice of a method largely depends on availability. In the case of our patient CT with Dental software was used, which made it possible to verify the previously taken radiographs by showing an alveolar cleft on the side of the scar.
The rarity of the problem which is 6:1,000,000 ratio [6], means that there are very few publications covering it [6,7,11] and none contained any information on imaging examinations that could document the actual picture of the craniofacial changes accompanying the facial scar. In this respect, this case report is the first in world literature.
Conclusions
The CT scan invariably confirmed the intrauterine pathology of cleft and its spontaneous repair. The presence of congenital scar and clinical history are sufficient to suggest the condition but there is need for confirmatory investigation which is what we did. Computed tomography is good in detecting occult pathology in the alveolus and the primary palate.
References
-
Rullo R, Festa VM, Rullo R, Addabbo F, Chiodini P, et al. (2015) Prevalence of dental anomalies in children with cleft lip and unilateral and bilateral cleft lip and palate. Eur J Paediatr Dent 16: 229-232.
-
Cudziło D (2014) Microform cleft lip or congenital healed cleft lip? Dev Period Med 18: 23-26.
-
Sathyaprasad S, Sharma SM, Shetty V (2014) BMP4 Gene and Pathophysiology of Cleft Lip and Palate. RRJDS.
-
Pace D, Attard-Montalto S, Grech V (2006) Bilateral microform cleft lip. MMJ 18: 36-37.
-
Suzuki S, Marazita ML, Cooper ME, Miwa N, Hing A, et al. (2009) Mutations in BMP4 Are Assotiated with Subepithelial, Microform, and Overt Cleft Lip. Am J Hum Genet 84: 406-411.
-
Castilla EE, Martínez-Frías ML (1995) Congenital healed cleft lip. Am J Med Genet 58: 106-112.
-
Grech V, Lia A, Mifsud A (2000) Congenital heart disease in a patient with microform cleft lip. Cleft Palate Craniofac J 37: 596-597.
-
Hultman CS, Friedstat JS (2014) The ACAPS and SESPRS surveys to identify the most influential innovators and innovations in plastic surgery: no line on the horizon. Ann Plast Surg 72: 202-207.
-
Albuquerque MA, Gaia BF, Paraíso Cavalcanti MG (2011) Comparison between multislice and cone-beam computerized tomography in the volumetric assessment of cleft palate. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 112: 249-257.
-
Rozylo-Kalinowska I, Bekiesinska-Figatowska M, Rozylo TK (2013) Imaging diagnostics of cleft lip and palate. Mag Stom 5: 14-20.
-
Hunnekens MC, Rook F (2010) A newborn with an unusual lip. Ned Tijdschr Geneeskd 154: 1304.