International Journal of Pediatric Research
Super Giant Coronary Aneurysm in an Algerian Boy with Kawasaki Disease
Houda Boudiaf1,2*, Manel Gherbi1,2 and Moussa Achir1,2
1Department of Pediatrics, Birtraria Hospital, Algeria
2University of Medical Sciences, Algeria
*Corresponding author: Houda Boudiaf, Department of Pediatrics, Birtraria Hospital, Pasteur Avenue 16606, Algiers, Algeria, E-mail: dr.houdaboudiaf@gmail.com
Int J Pediatr Res, IJPR-2-021, (Volume 2, Issue 2), Case Report; ISSN: 2469-5769
Received: April 12, 2016 | Accepted: July 19, 2016 | Published: July 22, 2016
Citation: Boudiaf H, Gherbi M, Achir M (2016) Super Giant Coronary Aneurysm in an Algerian Boy with Kawasaki Disease. Int J Pediatr Res 2:021. 10.23937/2469-5769/1510021
Copyright: © 2016 Boudiaf H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The patient is a 5-year-old male with findings suggestive of Kawasaki disease. He was treated with intravenous gamma globulin (IVG) and oral aspirin. Because the fever persisted, he received additional IVG and intravenous methylprednisolone. Echocardiography showed diffuse dilatation of the right coronary artery (RCA; 13 mm) and proximal dilatation of the left main coronary artery (LMCA; 8 mm). Despite treatment, the size of coronary had enlarged significantly (from 13 mm to 22 mm and from 8 mm to 25 mm, respectively). Angiography study performed and showed a bilateral supergiant aneurysm and an occlusion in the left anterior descending artery. Beta blocker was administered in conjunction with warfarin/aspirin anti-coagulation therapy. Twelve months after the first episode of the illness, the patient relapsed. Echocardiography showed changes in the size of the CAA (LMCA 29 mm; RCA 25 mm).
Keywords
Kawasaki disease, Coronary aneurysm, Super giant coronary aneurysm, Complications
Introduction
Kawasaki disease (KD) is now recognized as the leading cause of acquired heart disease among children in developed countries [1]. Today this illness has been described in almost every country such as Algeria [2]. The prevalence of coronary artery involvement is approximately 15-25%, and it decreases to 5% after the introduction of intravenous immunoglobulin (IVIG) treatment [3]. Giant coronary artery aneurysms (gCAA) are defined as being > 8 mm in diameter and occur at an incidence of approximately 0.25-2% in patients with KD. Large coronary aneurysms can be termed super giant when internal diameter was greater than 10mm [4].
KD patients with giant and super giant CAA show the greatest risk of stenosis and obstruction of the coronary artery, and even myocardial infarction during follow-up [5]. In this report, we present a rare patient with Kawasaki disease with multiple super giant CAA.
Case Report
A 5-year old boy was referred to our hospital with 8‐day duration of fever. He showed bilateral conjunctival injection, enlargement of the cervical lymph nodes, dry red lips, a strawberry tongue and a generalized maculopapular rash.
Initial laboratory results were as follows: haemoglobin, 9.6 g/dL; white blood cell (WBC) count, 13000/mm3 (polymorphonuclear leukocytes, 65.6%; lymphocytes, 27.9%; monocytes 6.5%), platelet count, 394 × 103/mm3 ; C-reactive protein (CRP ), 96 mg/L; sodium 135 mEq/L ; aspartate aminotransferase (AST), 16 U/L ; alanine aminotransferase (ALT), 10 U/L, total bilirubin 2 mg /L and albumin, 40 g/l.
Echocardiography was performed at the time of admission and showed diffuse dilatation of the right coronary artery (RCA) and proximal dilatation of the left main coronary artery (LMCA). RCA measured 13 mm at origin while LMCA measured 8 mm at origin. No impairment of the left ventricular function or of the pericardial effusion was found.
With a clinical diagnosis of KD, he was given intravenous gamma globulin (IVG) at 2 g/kg along with high aspirin doses. Because the fever persisted, he received additional IVIG (2 g/kg). The patient had recurrent fever 72-hours after completion of the initial treatment. On the seventh hospital day, he was given intravenous methylprednisolone (30 mg/kg/day) for three days, followed by one week of oral prednisolone (1 mg/kg/day) tapered over seven days. Fever gradually subsided. He was discharged with aspirin and subcutaneous enoxaparine.
Subsequent echocardiograms after 2, 6 and 12 months showed progressively enlarged aneurysms of both coronary arteries. The last echocardiography revealed a super giant fusiform aneurysm of RCA and a super giant aneurysm of the proximal left main coronary artery (RCA 22 mm, LMCA 25 mm). However, no electrocardiogram abnormalities were observed.
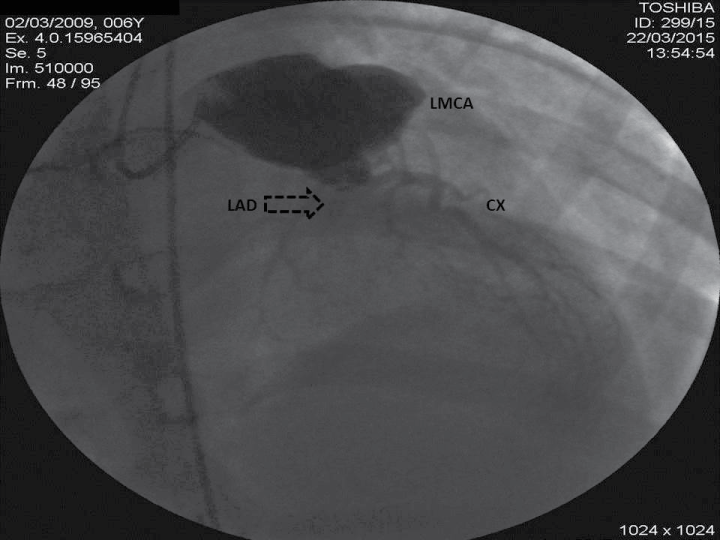
Coronary angiography was performed and showed a bilateral supergiant aneurysm and occlusion of the left anterior descending artery (Figure 1 and Figure 2). Oral carvedilol, warfarine and aspirin were started. Cardiac enzymes and stress test (treadmill test, tomographic myocardial perfusion imaging) remained normal.
.
Figure 1: Left arteriogram showing giant coronary artery aneurysm in LMCA and occlusion in the LAD.
LAD: left anterior descending artery; LMCA: left main coronary artery; Cx: circumflex artery
View Figure 1
.
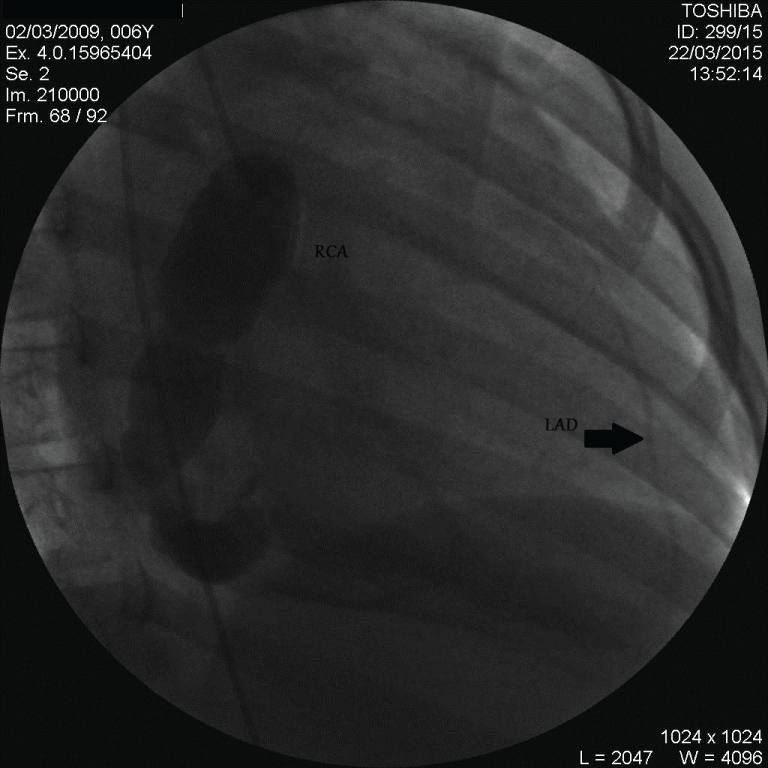
Figure 2: Right, arteriogram showing giant coronary artery aneurysm in RCA.
RCA: right coronary artery
View Figure 2
When the child was 6 years old, he presented clinical features compatible with a KD diagnosis, soon after primo infection with varicella zoster virus. Echocardiography showed changes in the size of the CAA (LMCA 29 mm; RCA 25 mm). At the last follow up visit, the patient was doing well without any symptoms.
Discussion
KD is the most prevalent vasculitis in the developed countries and can leave giant coronary artery aneurysms (gCAA) even with recommended treatment. Few cases with super giant coronary artery aneurysm have been reported in the literature [6,7]. Imai et al. consider it interesting to distinguish aneurysms which rapidly dilate and continue to increase over a diameter of 10 mm (these CAA can be termed "super-giant") [4]. Risk factors reported for developing giant aneurysms are age < 1 year and ≥ 5, male individuals, longer duration of fever and failure to respond initial IVG [8].
Approximately 15% to 20% of patients with KD are not responsive to initial IVIG treatment, and these patients are at a higher risk for CALs [9]. It is important to identify those patients because they might benefit from a more aggressive initial treatment. Various risk factors and scoring (Egami, Kobayashi, Sano) for IVIG-non-response have been described, including early treatment before day 5, male gender, laboratory parameters (e.g., increased CRP, low hemoglobin, low albumin, low sodium and platelet count and high alanine transaminase level) KD [10-13].
In our patient, besides risk factors of refractory KD (male gender, high CRP and low hemoglobin), none of the others usual indices were useful.
The optimal therapy for IVIG non-responders remains controversial as treatment strategies have varied between institutions. Management options include further dose(s) of IVIG, corticosteroids or new thérapies such as TNF-α blockade, cyclosporin A, anti-IL-1 cyclophosphamide, methotrexate and anti-CD20 therapy [14]. Limited studies exists regarding the use of these agents, but these medications could be considered in treating unresponsive KD.
In our patient, super gi¬ant CA aneurysms and stenosis developed despite IVG, steroid and anti-coagulant therapy, and this may be attributable to the major risk factors he had and probably to recurrence episode. This finding is plausible because repeated episodes of inflammation in KD are more likely to have greater effect on cardiac sequelae than would an isolated episode of disease [15].
Long-term management of patients with KD depends on the degree of coronary arterial involvement. Follow-up of a patient with coronary arterial aneurysms must be adapted to his clinical course and severity of the lesions.
Giant and super giant aneurysms are associated with higher morbidity and mortality, despite antiplatelet and anticoagulation therapy. Thrombosis of these aneurysms or stenosis due to luminal myofibroblastic proliferation can lead to myocardial infarction, ischemic heart disease, or sudden death. In this case, the coronary arteries were severely dilated, and stenosis had developed within a 12-months period after the onset of KD. The patient needed strict anti-coagulation to avoid thrombus formation. There are currently no evidence-based guidelines for optimal thromboprophylactic therapy for these children. However, the combination of warfarin and aspirin is known to have high cardiac event free incidence survival [16]. Low molecular weight heparin (LMWH) can be used instead of warfarin as warfarin is difficult to regulate and no difference was reported in the frequency of thrombotic CA occlusions with LMWH [17].
Hemodynamic stabilization by calcium channel blockers, and beta blockers to prevent further coronary dilation or rupture are mandatory in the management of this condition. In fact these therapeutics could be helpful in lowering blood pressure and heart rate, and could reduce sheer stress on the dilated coronary arterial wall.
The longitudinal changes of giant coronary aneurysms caused by KD and their long-term outcome are still unclear. The long-term results of KD patients with giant coronary aneurysms reported by Kato were that 46% of giant coronary aneurysms progressed to coronary artery stenosis or complete occlusion [18]. However, in a large recent study, cardiac event free and survival rate at 30 years after KD with giant aneurysms were found to be 36% and 90% respectively [19]. Progressive coronary dilatation at two or more months after diagnosis such as our patient, may be an indicator of the severity of vasculitis with worse late coronary outcomes.
Conclusion
This patient is remarkable because he presented a bilateral super giant CA despite early diagnosis and adequate treatment with IVG. More careful follow-up and intensive treatments are necessary for these particular patients.
Potential Conflict of Interest
No potential conflict of interest relevant to this article was reported.
Acknowledgment
We thank Dr. Younes Boudjemline (Director of the Cardiac Catheterization laboratory in Necker for Sick Children in Paris) and Nagib Dahdah (Pediatric Cardiologist at Sainte-Justine University Hospital Center) for the angiographic studies.
References
-
Uehara R, Belay ED (2012) Epidemiology of Kawasaki disease in Asia, Europe, and the United States. J Epidemiol 22: 79-85.
-
Boudiaf H, Achir M (2016) The Clinical Profile of Kawasaki Disease in Algerian Children: A Single Institution Experience. J Trop Pediatr 62: 139-143.
-
Newburger JW, Takahashi M, Gerber M, Gewitz MH, Tani LY, et al. (2004) Diagnosis, treatment and long-term complications of Kawasaki disease: a statement for health professionals from Committee on Rheumatic Fever, Endocarditis and Kawasaki disease, Council on Cardiovascular disease in Young, American Heart Association. Circulation 110: 2747.
-
Imai Y, Sunagawa K, Ayusawa M, Miyashita M, Abe O, et al. (2006) A fatal case of ruptured giant coronary artery aneurysm. Eur J Pediatr 165: 130-133.
-
Suda K, Iemura M, Nishiono H, Teramachi Y, Koteda Y, et al. (2011) Long-term prognosis of patients with Kawasaki disease complicated by giant coronary aneurysms: a single-institution experience. Circulation 123: 1836-1842.
-
Behjati-Ardakani M, Islami Z (2009) Super Giant Coronary Aneurysm in Kawasaki Disease. Iran J Pediatr 19: 317-321.
-
Lee J, Kim GB, Kwon BS, Bae EJ, Noh CI (2014) Two cases of super-giant coronary aneurysms after kawasaki disease. Korean Circ J 44: 54-58.
-
Sudo D, Monobe Y, Yashiro M, Sadakane A, Uehara R, et al. (2010) Case-control study of giant coronary aneurysms due to Kawasaki disease: the 19th nationwide survey. Pediatr Int 52: 790-794.
-
Tremoulet AH, Best BM, Song S, Wang S, Corinaldesi E, et al. (2008) Resistance to intravenous immunoglobulin in children with Kawasaki disease. J Pediatr 153: 117-121.
-
Uehara R, Belay ED, Maddox RA, Holman RC, Nakamura Y, et al. (2008) Analysis of potential risk factors associated with nonresponse to initial intravenous immunoglobulin treatment among Kawasaki disease patients in Japan. PediatrInfect Dis J 27: 155-160.
-
Egami K, Muta H, Ishii M, Suda K, Sugahara Y, et al. (2006) Prediction of resistance to intravenous immunoglobulin treatment in patients with Kawasaki disease. J Pediatr 149: 237-240.
-
Kobayashi T, Inoue Y, Takeuchi K, Okada Y, Tamura K, et al. (2006) Prediction of intravenous immunoglobulin unresponsiveness in patients with Kawasaki disease. Circulation 113: 2606-2612.
-
Sano T, Kurotobi S, Matsuzaki K, Yamamoto T, Maki I, et al. (2007) Prediction of non-responsiveness to standard high-dose gamma-globulin therapy in patients with acute Kawasaki disease before starting initial treatment. Eur J Pediatr 166: 131-137.
-
Saneeymehri S, Baker K, So TY (2015) Overview of Pharmacological Treatment Options for Pediatric Patients with Refractory Kawasaki Disease. J Pediatr Pharmacol Ther 20: 163-177.
-
Nakamura Y, Oki I, Tanihara S, Ojima T, Yanagawa H (1998) Cardiac sequelae in recurrent cases of Kawasaki disease: a comparison between the initial episode of the disease and a recurrence in the same patients. Pediatrics 102: E66.
-
Suda K, Kudo Y, Higaki T, Nomura Y, Miura M, et al. (2009) Multicenter and retrospective case study of warfarin and aspirin combination therapy in patients with giant coronary aneurysms caused by Kawasaki disease. Circ J 73: 1319-1323.
-
Manlhiot C, Brandao L, Somji Z, Chesney AL, Gurofsky R, et al. (2010) Long term anticoagulation in Kawasaki Disease: Initial Use of Low Molecular Weight Heparin is a Viable Option for Patients with Severe Coronary Artery Abnormalities. Pediatr Cardiol 31: 834-842.
-
Kato H, Sugimura T, Akagi T, Sato N, Hashino K, et al. (1996) Long-term consequences of Kawasaki disease. A 10- to 21-year follow-up study of 594 patients. Circulation 94: 1379-1385.
-
Tsuda E, Hamaoka K, Suzuki H, Sakazaki H, Murakami Y, et al. (2014) A survey of the 3-decade outcome for patients with giant aneurysms caused by Kawasaki disease. Am Heart J 167: 249-258.





