International Journal of Pediatric Research
A Valuable Tool to Determine Supraventricular Tachycardia in Children: Trans-Esophageal Electrophysiological Study
Şeyma Kayali*, İlker Ertuğrul, Vehbi Doğan, Senem Özgür, Utku Arman Örün and Selmin Karademir
Pediatric Cardiology, Dr. Sami Ulus Maternity and Children Research and Training Hospital, Turkey
*Corresponding author: Şeyma Kayali, Pediatric Cardiology, Dr. Sami Ulus Maternity and Children Research and Training Hospital, Babur Street, No: 44 (06080) Altındağ/Ankara, Turkey, Tel: +90 312 305 62 97, E-mail: ak-seyma@hotmail.com
Int J Pediatr Res, IJPR-2-023, (Volume 2, Issue 2), Original Article; ISSN: 2469-5769
Received: May 23, 2016 | Accepted: August 20, 2016 | Published: August 22, 2016
Citation: Kayali Ş, Ertuğrul I, Doğan V, Özgür S, Örün UA, et al. (2016) A Valuable Tool to Determine Supraventricular Tachycardia in Children: Trans-Esophageal Electrophysiological Study. Int J Pediatr Res 2:023. 10.23937/2469-5769/1510023
Copyright: © 2016 Kayali Ş, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: The aim of this study was to determine the accuracy of trans-esophageal electrophysiological study (TEEPS) in the diagnosis and differentiation of mechanisms of supraventricular tachycardia in pediatric patients.
Methods: A total of 132 patients who underwent TEEPS at our institution were included. Demographic features and symptoms of patients were evaluated and the patients were divided into three groups to compare the inducibility of tachycardia: Symptom group was consisting of 91 patients who had symptoms of arrhythmias, Wolf Parkinson White group was consisting of 18 patients who had Wolf Parkinson White pattern on surface electrocardiogram, and Tachycardia group was consisting of 23 patients who had previously detected or ongoing tachycardia on electrocardiographic monitoring.
Results: Forty nine male (37.1%), and 83 female (62.9%) patients with an average age of 12.3 ± 3.1 years (range: 4.7-18) attended this study. Tachycardia was induced in a total of 40 procedures (40/132, 30.3%): 13/91 (14.3%) in Symptom group, 7/18 (38.9%) in WPW group and 20/23 (86.9%) in Tachycardia group.
Conclusion: TEEPS is a safe and valuable diagnostic method to evaluate the patients with symptoms possibly related with arrhythmia or in the management of patients who have any arrhythmias.
Keywords
Arrhythmia, Children, Electrophysiological study
Introduction
Trans-esophageal electrophysiological study (TEEPS) is a semi-invasive method for diagnosis and management of children with supraventricular tachycardia (SVT). TEEPS is also useful to evaluate the patients with symptoms suggestive of SVT without electrocardiographic documentation, to assess the mechanisms responsible for re-entry tachycardia, risk stratification for sudden cardiac death (SCD) of Wolf Parkinson White (WPW) syndrome, to terminate re-entry SVT in children and for follow up after radiofrequency ablation (RFA) [1]. In the present study we will report our results of TEEPs performed with these indications.
Material and Methods
The study group was consisted of 132 patients (49 male, 83 female) who underwent TEEPS from January 2010 to February 2015 at Dr. Sami Ulus Maternity and Child Health Training and Research Hospital, Pediatric Cardiology Department. TEEPS was performed with following indications: evaluation of symptoms that may be sign of arrhythmias, evaluation and risk assessment of WPW patients and determination of the mechanism of previously detected or ongoing tachycardia. According to the indications, the study population was divided into three groups. Symptom group had been constituted from 91 (68.9%) patients who had symptoms that may be signs of arrhythmia such as palpitation, syncope or chest pain with palpitation and without an electrocardiographic evidence of tachycardia. WPW group was consisted of 18 (13.6%) WPW patients who had no previously documented tachycardia attack. Tachycardia group was consisted of 23 (17.4%) patients who had previously detected or ongoing tachycardia in ECG or Holter monitoring. Forty patients had some abnormalities in transthoracic echo-cardiographic evaluation including mitral valve prolapses (n:23 patients), atrial septal defect (n:6 patients), mild and moderate mitral or aortic valve insufficiency (n:11 patients), transposition of great arteries (n:1 patient) and dilated cardiomyopathy (n:1 patient), respectively. A standard electrocardiogram was obtained in all patients. Electrocardiogram was normal in 97 (73.5%) patients at the time of admission. Dysrhythmia was detected with current standard 12-lead ECG in only 19 patients. Holter monitoring was performed in 99 patients - 1 had SVT, 8 had frequent supraventricular ectopic beats, 5 had rare ventricular ectopic beats, and 1 had non-sustained ventricular tachycardia attack. Exercise testing was performed in 16 patients and all were normal. In 2 patients with premature extra-systoles, extra-systole disappeared during exercise testing (Table 1and Table 2).
![]()
Table 1: Clinical characteristics of the patients.
View Table 1
![]()
Table 2: Distribution of tachyarrhythmia according to groups.
View Table 2
Trans-esophageal electrophysiological study
TEEPS was performed in all patients as previously described by Benson, et al. [1]. The procedure was achieved in the fasting state (at least four hours), in angiography laboratory after explaining the patients and/or parents possible discomfort induced by TEEPS and a written informed consent form was obtained from all parents. Midazolam was administered through venous line (0.05-0.1 mg/kg) to only patients who did not tolerate the procedure. In our study, only 18 (13.6%) patients required sedation with midazolam. A 6 Fr quadripolar electrode (Fiab, Esokid 4, Italy) with electrode spaced at 10 mm was positioned through the nares in the esophagus with the aid of esophageal electrocardiogram at the appropriate depth where optimum atrial signals were obtained. Before insertion, the tip of the catheter was coated with 1% lidocaine in all patients.
Atrial stimulation was done with a programmable stimulator (Fiab Programmable Cardiac Stimulator 8817 with a pulse width and amplitude capacity between 10-20 msec and 15-20 mA consecutively). A standard ECG machine was used for recording. Single and pair extra-stimuli at progressively higher rates were performed until the atrioventricular (AV) effective refractory period was reached. Incremental pacing to the point of second-degree AV block and burst pacing at cycle lengths similar to those producing second-degree AV block were performed. When sustained tachycardia was not induced under basal conditions, we repeated the pacing protocol after isoproterenol (0.05-0.1 μg/kg/min) infusion. We terminated the induced tachycardia by atrial overdrive pacing. The endpoint of the procedure was either an induction of tachycardia or completion of the protocol.
Tachycardia mechanisms
Atrioventricular nodal re-entrant tachycardia (AVNRT) was presumed to be present under the condition of regular tachycardia, no evidence of AV dissociation or 2:1 AV block, and a ventriculoatrial (VA) interval of ≤ 70 ms. Atrioventricular reentrant tachycardia (AVRT) was presumed to be present under the condition of regular tachycardia, no evidence of AV dissociation, and a VA interval ≥ 70 msec [1].
Results
TEEPS could be successfully performed and well tolerated in all patients without any complications related to the procedure. Average age of the patients at time of trans-esophageal study was 12.3 ± 3.1 years (range: 4.7-18 years). There were 83 females (62.9%) and 49 males (37.1%). Tachycardia was induced in a total of 40 procedures (40/132, 30.3%):13/91 (14.3%) in Symptom group, 7/18 (38.9%) in WPW group, 20/23 (86.9%) in Tachycardia group (Figure 1).
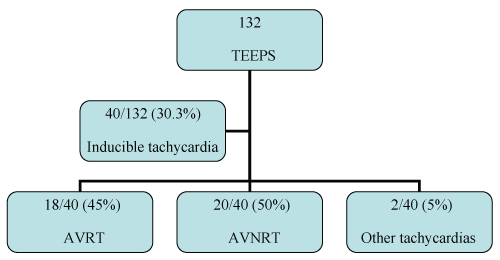
.
Figure 1: Mechanism of tachycardia induced by TEEPS.
AVNRT: Atrioventricular Nodal Reentrant Tachycardia, AVRT: Atrioventricular Reentrant Tachycardia, TEEPS: Transesophageal Electrophysiologic Study
View Figure 1
Symptom group was consisting of patients with palpitation (n: 61, 46.2%), chest pain plus palpitation (n: 22, 16.7%), and syncope plus palpitation (n: 8, 6.1%). In Symptom group, inducible tachycardia was diagnosed as AVRT in 3/13 (23%), AVNRT in 10/13 (77%) patients. Tachycardia was induced in 19.7% and 4.3% of the patients presenting with palpitation and chest pain plus palpitation, respectively; while tachycardia was not induced in the patients with palpitation and syncope.
In WPW group, 4 patients had palpitation, 1 had palpitation plus chest pain and 1 had palpitation plus syncope while 12 had no symptoms. Inducible tachycardia had been found in 7 (38.9%) patients, 6 of inducible tachycardia patients were having AVRT and in one patient atrial fibrillation was induced. All patients with inducible tachycardia had VA interval longer than 70 msec and 2 of these patients had accessory pathway effective refractory period (APERP) shorter than 250 msec.
In Tachycardia group, tachycardia was induced in 86.9% of the patients. Inducible tachycardia was diagnosed as AVRT in 9/20 (45%), AVNRT in 10/20 (50%) patients and atrial flutter in 1/20 (5%). The sensitivity and specificity of our study were 86.9% and 81.6%, respectively similar to previous studies in literature [2,3].
Because of the lack of possibility to perform intracardiac electrophysiological studies (IEPS) in our clinic, all patients with inducible tachycardia were referred to other clinics. We reached 21 patients from the records in our hospital data. Four of 21 patients did not admit to any other clinics. IEPS was performed in 13 patients having inducible tachycardia in another clinic. Tachycardia was induced in all 13 patients by IEPS, too. Mechanisms of tachycardia were all the same. Ablation was performed in 10 of 13 patients.
Discussion
SVT is a common rhythm anomaly during childhood and reentry that originates from accessory pathway is usually the responsible mechanism [4]. Since the duration of a single SVT attack is commonly quite short and infrequent, the possibility of recording a SVT attack on a standard ECG recording is very low. Therefore, repeated and extensive investigations may be required for a long period in patients without precise diagnosis. By using TEEPS, etiology can be clarified precisely in a short time.
The information gathered from the present and previously published studies shows that TEEPS is a useful and semi-invasive method of diagnosing and treating arrhythmias in pediatric patients [3,5]. It is currently used to assess the function of the sinus and AV nodes. In the present study we performed TEEPS to evaluate the children with arrhythmia symptoms, to determine the risk in children with WPW and to understand potential mechanisms of tachycardia in patients with documented SVT.
A study by Perrot, et al. reported that TEEPS is a fast method for proving the nature of paroxysmal tachycardia in children and teenagers presenting with normal ECG and for demonstrating WPW syndrome not visible on standard ECG. The negative predictive value of TEEPS for the diagnosis of SVT was 100% [6]. Similarly, another study which evaluated palpitation/tachycardia and catheter ablation control reported that the sensitivity and specificity of the TEEPS was 74% and 90%, respectively [7]. The sensitivity and specificity of our study were 86.9% and 81.6%, respectively. We found the SVT inducibility rate as 30.3% in this study group. But tachycardia was induced by TEEPS in 20 of 23 patients with documented electrocardiography (sensitivity 86.9%). This result is similar with the study which reported the sensitivity as 92.9% in patients with documented electrocardiogram [3]. Although, in the present study, tachycardia inducibility rate is low by TEEPS in Symptom group, it is important to note that, especially in adolescent patients, such complaints are likely to be psychological. But before associating palpitations and other symptoms with psychiatric problems, arrhythmia work-up should be performed. Although noninvasive methods (rhythmHolter, event recording, ECG) can be used for this purpose, these methods have disadvantages like low possibility to document SVT attack as mentioned before. We think that TEEPS could also be performed for immediate diagnosis and relieving parent anxiety.
Initial presentation in patients with WPW syndrome whether symptomatic or not may be sudden cardiac death [2,8]. High ventricular rate during atrial fibrillation is generally the underlying etiology. So, identifying WPW patients with increased risk of developing ventricular fibrillation is very important. APERP length is the most important indicator of ventricular fibrillation development during atrial fibrillation [9]. Long refractory period of the accessory pathway lowers the risk of developing ventricular fibrillation. APERP is shorter in children than in adults, so the probability of initially presenting with ventricular fibrillation or sudden death is higher in children with WPW syndrome [10]. The gold standard for the determination of APERP is electrophysiological studies.
In our study, we applied TEEPS for risk assessment of WPW in 18 patients. AVRT was induced in 6 patients, and atrial fibrillation was induced in one patient. We could not induce tachycardia in 11 patients. The APERP was found to be shorter than 250 msec in two patients.
TEEPS seems to be very effective in the differential diagnosis of SVTs. Differential diagnosis between AVRTs and AVNRTs depends on the VA interval being < 70 msec or > 70 msec [1]. Studies which compare SVT mechanisms by TEEPS and intracardiac electrophysiological studies revealed high compatibility rates between two methods [3,11]. In our study, SVT mechanisms were all same in 13 patients who had IEPS in another clinic.
Though, TEEPS seems to be safe and relatively easy, rarely serious arrhythmias like ventricular tachycardia and fibrillation could be induced during the procedure. In addition to this, mild esophageal ulcerations could be seen on follow up after the procedure [12]. In our study group, the investigation was well tolerated and could be completed in all patients without any complications related to the procedure.
In conclusion, we think that TEEPS should be preferred in patients whose complaints cannot be explained by non-invasive procedures like ECG and Holter monitoring. TEEPS is a semi-invasive, safe, effective and valuable initial evaluation method for children with tachycardia symptoms that also provides differential diagnosis of SVTs and determines SCD risk in pediatric patients with WPW.
Author's Contribution
SK (first author): study's conception and design, development of the study and manuscript preparation; IK: study's conception and design, and manuscript preparation; VD: study's conception and design, and analysis of results; SO: study's design and manuscript preparation; UAO: study's design and manuscript preparation; SK: study's design and manuscript preparation.
References
-
Benson DW Jr, Sanford M, Dunnigan A, Bendit DG (1984) Transesophageal atrial pacing threshold: Role of interelectrode spacing, pulse duration and catheter insertion depth. Am J Cardiol 53: 63-67.
-
Erdogan I, Ozer S, Karagoz T, Sahin M, Celiker A (2009) Clinical importance of transesophageal electrophysiologic study in the management of supraventricular tachycardia in children. Turk J Pediatr 51: 578-581.
-
Akin A, Ozer S, Karagoz T, Aykan HH, Gulgun M, et al. (2014) Sensitivity of transesophageal electrophysiologic study in children with supraventricular tachycardia on electrocardiography. Pacing Clin Electrophysiol 37: 1002-1008.
-
Brembilla-Perrot B, Marcon F, Bosser G, Lucron H (2000) Junctional tachycardia in adolescents: nodal reentry is the most frequent cause. Ann Cardiol Angeiol (Paris) 49: 8-12.
-
Blafox AD, Warsy I, D'Souza M, Kanter R (2011) Transesophageal electrophysiological evaluation of children with a history of supraventricular tachycardia in infancy. Pediatr Cardiol 32: 1110-1114.
-
Brembilla-Perrot B, Groben L, Chometon F, Lethor JP, Admant P, et al. (2009) Rapid and low-cost method to nature of no documented tachycardia in children and teenagers without pre-excitation syndrome. Europace 11: 1083-1089.
-
Kesek M, Sheikh H, Bastani H, Blostrom P, Lundqvist CB (2000) The sensitivity of transesophageal pacing for screening in atrial tachycardias. Int J Cardiol 72: 239-242.
-
Yildirim I, Ozer S, Karagoz T, Sahin M, Ozkutlu S, et al. (2015) Clinical and electrophysiological evaluation of pediatric Wolff-Parkinson-White patients. Anatol J Cardiol 15: 485-490.
-
Ro PS, Rhodes LA (2001) Atrioventricular node reentry tachycardia in pediatric patients. Prog Pediatr Cardiol 13: 3-10.
-
Bromberg BI, Lindsay BD, Cain ME, Cox JL (1996) Impact of clinical history and electrophysiologic characterization of accessory pathways on management strategies to reduce sudden death among children with Wolff- Parkinson-White syndrome. J Am Coll Cardiol 27: 690-695.
-
Aykan HH, Ozer S, Karagoz T, Akin A, Gulgun M, et al. (2015) Comparison of Transesophageal and Intracardiac Electrophysiologic Studies for the Diagnosis of Childhood Supraventricular Tachycardias. Pediatr Cardiol 36: 1429-1435.
-
Torok TS, Mikhaylov E, Witsenburg M (2009) Transesophageal electropysiologic study for children: can we swallow the limitations? Europace 11: 987-988.





